It has long been known from clinical follow-up studies that children with attention-deficit hyperactivity disorder (ADHD) often continue to have symptoms in adulthood (Reference Weiss and HechtmanWeiss & Hechtman, 1993), that symptoms of inattention are more likely to persist into adulthood than symptoms of hyperactivity or impulsivity (Reference Wilens, Faraone and BiedermanWilens et al, 2004) and that adults with a history of childhood ADHD have a comparatively high prevalence of other mental disorders that develop subsequent to ADHD and might be to some extent consequences of primary ADHD (Reference BiedermanBiederman, 2004); however, adult ADHD has only recently become the focus of widespread clinical attention (Reference Wilens, Faraone and BiedermanWilens et al, 2004). Not only is the study of adult ADHD comparatively new, it is also characterised by controversy due to lack of agreement on appropriate diagnostic criteria and the realisation that diagnosis is complicated by symptom overlap with a number of other disorders (Reference McGough and BarkleyMcGough & Barkley, 2004).
As adult ADHD was not included in any of the major psychiatric epidemiological surveys that have been carried out around the world since the landmark Epidemiologic Catchment Area study in the early 1980s (Reference Weissman, Bland and CaninoWeissman et al, 1996; World Health Organization (WHO) International Consortium in Psychiatric Epidemiology, 2000), attempts to estimate adult ADHD prevalence have been based either on extrapolations from childhood prevalence estimates using information from clinical studies regarding the proportion of childhood cases that persist into adulthood (Reference Barkley, Fischer and SmallishBarkley et al, 2002) or on direct estimates from small samples (Reference Faraone and BiedermanFaraone & Biederman, 2005). Most of the studies of either type have taken place in the USA, where estimates of adult ADHD prevalence are in the range 1–6%. A review by Faraone et al (Reference Faraone, Sergeant and Gillberg2003) based on 20 studies in the USA and 30 studies in other countries found that prevalence estimates of childhood and adolescent ADHD were as high in many non-US studies as in US studies. Studies of adult ADHD in non-US populations, though, are much rarer. The only general-population non-US study took place in a town in The Netherlands (Reference Kooij, Buitelaar and van den OordKooij et al, 2005), but absence of information on age of onset and pervasiveness of symptoms made it impossible to generate an unbiased prevalence estimate of adult ADHD in this population. In order to obtain more accurate estimates of prevalence and correlates of adult ADHD, a screen for this disorder was developed for use in the World Health Organization World Mental Health (WMH) surveys (Reference Demyttenaere, Bruffaerts and Posada-VillaDemyttenaere et al, 2004). We present here the results from the ten WMH surveys that included this screen.
METHOD
Samples
Adult ADHD was assessed in the following WMH countries: Belgium, Colombia, France, Germany, Italy, Lebanon, Mexico, The Netherlands, Spain and the USA. Three of these ten are classified by the World Bank as ‘less developed’ (Colombia, Lebanon and Mexico; World Bank, 2003). The other seven countries are classified as ‘developed’. All surveys were conducted face-to-face by trained lay interviewers in multi-stage household probability samples (Table 1). The weighted average response rate across all ten of these countries was 67.9%, with a range of 45.9–87.7%.
Table 1 Sample characteristics

| Country | Survey | Sample characteristics 1 | Field dates | Adult ADHD subsample size 2 n | Response rate 3 |
|---|---|---|---|---|---|
| Belgium | ESEMeD | Stratified multistage clustered probability sample of individuals residing in households from the national register of Belgium residents (NR) | 2001/2 | 486 | 50.6 |
| Colombia | NSMH | Stratified multistage clustered area probability sample of household residents in all urban areas of the country (approximately 73% of the total national population) | 2003 | 1731 | 87.7 |
| France | ESEMeD | Stratified multistage clustered sample of working telephone numbers merged with a reverse directory (for listed numbers); initial recruitment was by telephone, with supplemental in-person recruitment in households with listed numbers (NR) | 2001/2 | 727 | 45.9 |
| Germany | ESEMeD | Stratified multistage clustered probability sample of individuals from community resident registries (NR) | 2002/3 | 621 | 57.8 |
| Italy | ESEMeD | Stratified multistage clustered probability sample of individuals from municipality resident registries (NR) | 2001/2 | 853 | 71.3 |
| Lebanon | LEBANON | Stratified multistage clustered area probability sample of household residents (NR) | 2002/3 | 595 | 70.0 |
| Mexico | M–NCS | Stratified multistage clustered area probability sample of household residents in all urban areas of the country (approximately 75% of the total national population) | 2001/2 | 1736 | 76.6 |
| Netherlands | ESEMeD | Stratified multistage clustered probability sample of individuals residing in households that are listed in municipal postal registries (NR) | 2002/3 | 516 | 56.4 |
| Spain | ESEMeD | Stratified multistage clustered area probability sample of household residents (NR) | 2001/2 | 960 | 78.6 |
| USA | NCS–R | Stratified multistage clustered area probability sample of household residents (NR) | 2002/3 | 3197 | 70.9 |
ADHD, attention-deficit hyperactivity disorder; ESEMeD, European Study of the Epidemiology of Mental Disorders; LEBANON, Lebanese Evaluation of the Burden of Ailments and Needs of the Nation; M–NCS, Mexico National Comorbidity Survey; NCS–R, National Comorbidity Survey Replication; NR, nationally representative; NSMH, Colombian National Study of Mental Health
1. Most World Mental Health (WMH) surveys are based on stratified multistage clustered area probability household samples in which samples of areas equivalent to counties in the UK were selected in the first stage followed by one or more subsequent stages of geographic sampling (e.g. towns within counties, blocks within towns, households within blocks) to arrive at a sample of households, in each of which a listing of household members was created and one or two people were selected from this listing to be interviewed. No substitution was allowed when the originally sampled household resident could not be interviewed. These household samples were selected from census area data in all countries other than France (where telephone directories were used to select households) and The Netherlands (where postal registries were used to select households). Several WMH surveys (Belgium, Germany, Italy) used municipal resident registries to select respondents without listing households. Eight of the ten WMH surveys considered here are based on nationally representative household samples; the two others are based on nationally representative household samples in urban areas (Colombia, Mexico)
2. Attention-deficit hyperactivity disorder was assessed only among respondents in the age range 18–44 years in the Part II sample of each survey
3. Calculated as the proportion of the number of households in which an interview was completed to the number of households originally sampled, excluding from the denominator households known not to be eligible either because of being vacant at the time of initial contact or because the residents were unable to speak the designated languages of the survey
The WMH interview schedule was in two parts. All respondents completed part I, which contained core diagnostic assessments. All part I respondents who met criteria for any of these core disorders plus a probability subsample of other part I respondents were administered part II, which assessed disorders of secondary interest and a wide range of correlates. Adult ADHD was assessed in part II. As one requirement for a diagnosis of ADHD is onset of symptoms in childhood, the assessment was limited to respondents in the age range 18–44 years because of concerns about accuracy of retrospective recall among older respondents. A total of 11 422 respondents in this age range were screened across the ten surveys, with the size of within-country samples ranging from 3197 in the USA to 486 in Belgium.
The WMH interview schedule and all other study training materials and respondent visual aids were translated using standardised World Health Organization (WHO) translation and back-translation protocols (these materials are posted at http://www.hcp.med.harvard.edu/wmh). Consistent interviewer training and quality control procedures were used in all surveys. Procedures for informed consent, which was obtained in all countries before beginning interviews, were approved and monitored for compliance by the institutional review boards of the organisations coordinating the surveys in each country.
Adult ADHD
The retrospective assessment of childhood ADHD in the WMH surveys was based on the Diagnostic Interview Schedule for DSM–IV (DIS; Reference Robins, Cottler and BucholzRobins et al, 1995). Respondents classified retrospectively as having met full ADHD criteria in childhood were then asked a single question about whether they continued to have any current problems with attention or hyperactivity–impulsivity. A clinical reappraisal interview of these respondents was carried out in a probability subsample of 154 respondents in the WMH sample in the USA using the Adult ADHD Clinical Diagnostic Scale, version 1.2 (ACDS; Reference Adler and CohenAdler & Cohen, 2004; Reference Adler and CohenAdler & Spencer, 2004), a semi-structured interview which includes the ADHD Rating Scale (ADHD–RS; Reference DuPaul, Power and AnastopoulosDuPaul et al, 1998) for childhood ADHD and an adaptation of the ADHD–RS to assess current adult ADHD. The ACDS has been used in clinical trials of adult ADHD (Reference Spencer, Biederman and WilensSpencer et al, 2001; Reference Michelson, Adler and SpencerMichelson et al, 2003).
Four experienced clinical interviewers (all PhD-qualified clinical psychologists) conducted the clinical reappraisal interviews. Each interviewer received 40 h of training from two board-certified psychiatrists, specialists in the treatment of adult ADHD, and successfully completed five practice interviews. All clinical interviews were tape-recorded and reviewed by a supervisor. Weekly calibrator meetings were used to prevent drift. A clinical diagnosis of adult ADHD required six symptoms of either inattention or hyperactivity–impulsivity during the 6 months before the interview (DSM–IV criterion A; American Psychiatric Association, 1994), at least two criterion A symptoms before age 7 years (criterion B), some impairment in at least two areas of living during the previous 6 months (criterion C) and clinically significant impairment in at least one of these areas (criterion D). No attempt was made to operationalise DSM–IV diagnostic hierarchy rules (criterion E).
The DIS questions used to assess ADHD in the main survey were treated as independent variables in the subsample of clinical reappraisal respondents who reported recent symptoms to predict masked clinician diagnoses of DSM–IV adult ADHD. As detailed elsewhere (Reference Kessler, Adler and BarkleyKessler et al, 2006), a strong association (with an area under the receiver operating characteristic curve of 0.86) was found between these independent variables and the clinical diagnoses, based on a four-category classification scheme that distinguished respondents in terms of whether they reported no childhood symptoms of ADHD, sub-threshold symptoms, threshold symptoms in the absence of adult persistence or threshold symptoms with adult persistence. This strong association between the DIS questions and the masked clinical diagnoses provided the empirical justification for using the DIS symptom recency questions to generate a predicted probability of adult ADHD for every respondent in the larger samples. It needs to be noted, however, that a major limitation in this approach is that we have no way of knowing from these data whether the same strong association between the DIS and clinical diagnoses holds in countries other than the USA.
Co-occurring DSM-IV disorders
Other DSM–IV disorders were assessed in the WMH surveys using the WHO Composite International Diagnostic Interview, version 3.0 (CIDI; Reference Kessler and UstunKessler & Ustun, 2004), a fully structured, lay-administered diagnostic interview. The core disorders include anxiety disorders, mood disorders and substance use disorders. Organic exclusion rules and diagnostic hierarchy rules were used in making diagnoses. As detailed elsewhere (Reference Haro, Arbabzadeh-Bouchez and BrughaHaro et al, 2007), masked clinical reappraisal interviews using the Structured Clinical Interview for DSM–IV (SCID; Reference First, Spitzer and GibbonFirst et al, 2002) with a probability subsample of respondents from the US survey found acceptable concordance of DSM–IV diagnoses based on the CIDI and SCID interviews in four WMH countries where clinical reappraisal studies were carried out. Each CIDI diagnostic section included questions about age at onset of the focal disorder. These retrospective reports of age at onset were compared for ADHD and other DSM–IV disorders among respondents who met criteria for adult ADHD with comorbid anxiety, mood and substance use disorders in order to study temporal priorities in these cases of co-occurrence.
Other correlates of adult ADHD
We examined associations of adult ADHD with socio-demographic data and role disability, assessed with the WHO Disability Assessment Schedule (WHO–DAS; Reference Chwastiak and Von KorffChwastiak & Von Korff, 2003). The WHO–DAS assesses frequency and intensity of restriction or lack of ability to perform activities in a number of domains over the past 30 days. Three areas of basic activity were considered – mobility (e.g. walking a mile), self-care (e.g. getting dressed) and cognition (e.g. remembering to do important things) – along with two areas of instrumental activity –‘ time out of role' (i.e. number of days totally unable to carry out normal daily activities) and social role performance (e.g. controlling emotions when around other people). Dichotomous measures of disability were defined for the dimensions of mobility, self-care, cognition and social role by giving equal weights to frequency and intensity and defining disability as having any difficulty in basic functioning or role performance. The dichotomy for time out of role was defined as having more than 8 days out of role.
We asked about treatment of specific emotional and substance problems in separate diagnostic sections of the CIDI. We also asked a more general series of questions about seeking treatment for any emotional problem in a separate treatment section of the interview. Comparison of responses about treatment of ADHD and about treatment of emotional problems more generally allowed us to pinpoint people with ADHD who had received treatment for comorbid mental or substance use problems but not for ADHD.
Analysis methods
A prediction equation estimated in the clinical reappraisal sample was used to generate a predicted probability of DSM–IV adult ADHD for each respondent who was administered the DIS ADHD section in the main interview but who did not complete a clinical reappraisal interview. The method of multiple imputation (Reference RubinRubin, 1987) was used to convert these predicted probabilities into dichotomous diagnostic classifications and to adjust significance tests for the fact that the predicted clinical diagnoses are imperfectly related to actual clinical diagnoses. This method is based on the assumption that the calibration of the DIS ADHD symptom and recency questions in the US clinical reappraisal study applies equally well to the other WMH countries – an assumption that cannot be tested here in light of the fact that no clinical reappraisal study for adult ADHD was conducted in any of the other countries.
Socio-demographic correlates were estimated using multiple imputation logistic regression analysis. Co-occurrence was assessed by obtaining multiply imputed estimates of odds ratios between adult ADHD and other DSM–IV disorders in logistic regression equations that controlled for age in 5-year age groups. Functional disabilities were also estimated using multiple imputation logistic regression. Twelve-month treatment was estimated using multiple imputation cross-tabulations. In each phase of analysis we generated estimates both separately for each of the ten samples and also in a combined cross-sample analysis that included nine dummy control variables to indicate country. Interactions were then estimated between the country dummies and the substantive predictors to evaluate the significance of between-country differences. Such differences, although few in number, are noted in the following presentation of substantive results.
Part I cases were weighted to adjust for differential probabilities of selection within and between households and to match sample distributions to population distributions on socio-demographic and geographic data. The part II sample was additionally weighted for the undersampling of part I respondents without core disorders. Because the sample design used this weighting as well as geographic clustering, all parameters were estimated using the Taylor series linearisation method (Reference WolterWolter, 1985), a design-based method implemented in the SUDAAN software system (Research Triangle Institute, North Carolina, USA). All significance tests used two-sided Wald χ2 tests based on design-corrected multiple imputation variance–covariance matrices.
RESULTS
Prevalence
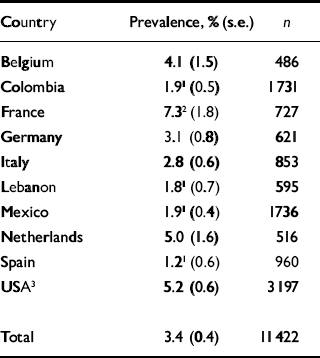
The estimated prevalence of DSM–IV adult ADHD in the total sample based on multiple imputation, using a combination of directly interviewed cases from the clinical reappraisal sample in the USA and multiply imputed cases in the remainder of the samples, was 3.4%, s.e.=0.4 (Table 2). Prevalence estimates were significantly higher than this average in France (7.3%, s.e.=1.8) and significantly lower in Colombia (1.9%, s.e.=0.5), Lebanon (1.8%, s.e.=0.7), Mexico (1.9%, s.e.=0.4) and Spain (1.2%, s.e.=0.6).
Table 2 Multiply imputed prevalence estimates of adult attention-deficit hyperactivity disorder
| Country | Prevalence, % (s.e.) | n |
|---|---|---|
| Belgium | 4.1 (1.5) | 486 |
| Colombia | 1.9 1 (0.5) | 1 731 |
| France | 7.3 2 (1.8) | 727 |
| Germany | 3.1 (0.8) | 621 |
| Italy | 2.8 (0.6) | 853 |
| Lebanon | 1.8 1 (0.7) | 595 |
| Mexico | 1.9 1 (0.4) | 1736 |
| Netherlands | 5.0 (1.6) | 516 |
| Spain | 1.2 1 (0.6) | 960 |
| USA 3 | 5.2 (0.6) | 3 197 |
| Total | 3.4 (0.4) | 11 422 |
1. The upper end of the 95% confidence interval of this estimate is below the prevalence estimate for the total sample
2. The lower end of the 95% confidence interval of this estimate is above the prevalence estimate for the total sample
3. This estimate differs somewhat from an estimate reported elsewhere (Reference Kessler, Adler and BarkleyKessler et al, 2006) because it is based on a different imputation equation. The equation used here is less complex because it had to be limited to variables included in all the surveys
Socio-demographic correlates
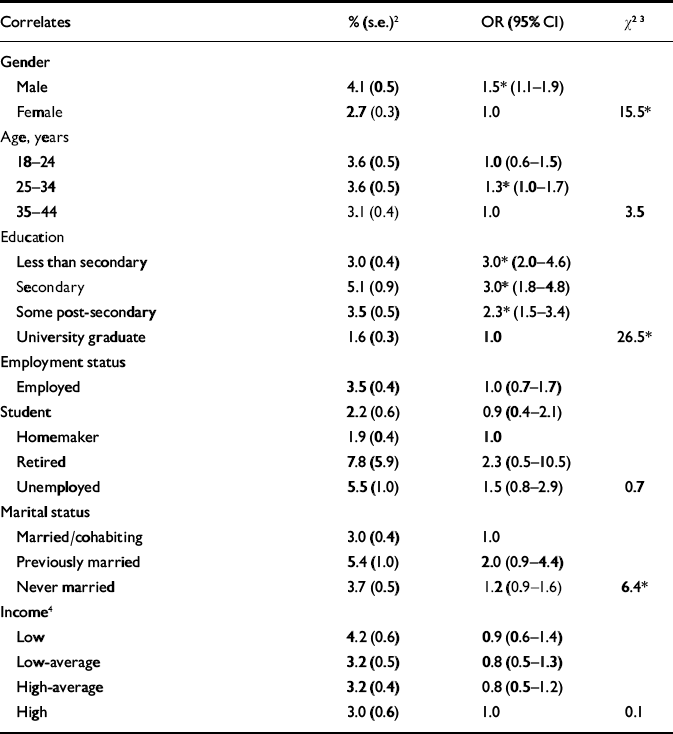
Multiple imputation prevalence estimates of clinician-assessed adult ADHD were significantly greater in the total cross-national sample among men and among people educated to less than university level (Table 3), but these effects were modest in magnitude (1.5<OR<3.0). No significant between-country difference was found in the magnitude of the effects of gender and education, although it is noteworthy that there was little power to detect such effects (further details available from the authors).
Table 3 Socio-demographic correlates of adult attention-deficit hyperactivity disorder (n=11 422)
| Correlates | % (s.e.) 2 | OR (95% CI) | χ 2 3 |
|---|---|---|---|
| Gender | |||
| Male | 4.1 (0.5) | 1.5 * (1.1–1.9) | |
| Female | 2.7 (0.3) | 1.0 | 15.5 * |
| Age, years | |||
| 18–24 | 3.6 (0.5) | 1.0 (0.6–1.5) | |
| 25–34 | 3.6 (0.5) | 1.3 * (1.0–1.7) | |
| 35–44 | 3.1 (0.4) | 1.0 | 3.5 |
| Education | |||
| Less than secondary | 3.0 (0.4) | 3.0 * (2.0–4.6) | |
| Secondary | 5.1 (0.9) | 3.0 * (1.8–4.8) | |
| Some post-secondary | 3.5 (0.5) | 2.3 * (1.5–3.4) | |
| University graduate | 1.6 (0.3) | 1.0 | 26.5 * |
| Employment status | |||
| Employed | 3.5 (0.4) | 1.0 (0.7–1.7) | |
| Student | 2.2 (0.6) | 0.9 (0.4–2.1) | |
| Homemaker | 1.9 (0.4) | 1.0 | |
| Retired | 7.8 (5.9) | 2.3 (0.5–10.5) | |
| Unemployed | 5.5 (1.0) | 1.5 (0.8–2.9) | 0.7 |
| Marital status | |||
| Married/cohabiting | 3.0 (0.4) | 1.0 | |
| Previously married | 5.4 (1.0) | 2.0 (0.9–4.4) | |
| Never married | 3.7 (0.5) | 1.2 (0.9–1.6) | 6.4 * |
| Income 4 | |||
| Low | 4.2 (0.6) | 0.9 (0.6–1.4) | |
| Low-average | 3.2 (0.5) | 0.8 (0.5–1.3) | |
| High-average | 3.2 (0.4) | 0.8 (0.5–1.2) | |
| High | 3.0 (0.6) | 1.0 | 0.1 |
1. Correlates of multiply imputed DSM–IV adult attention-deficit hyperactivity disorder (ADHD) in the pooled surveys, based on a multivariate logistic regression equation in which all predictors were included simultaneously
2. Percentages reported are the conditional prevalence estimates of ADHD in the socio-demographic subsamples
3. The χ2 tests all have one degree of freedom. Tests for age, education and income are based on continuous versions of those predictors. The test for employment status compares employed v. all others. The test for marital status compares married/cohabiting v. all others
4. Income is defined as the ratio of pre-tax family income to number of household members. Households with ratios half the median or lower were categorised as ‘low’ income; those with ratios between half the median and the median were categorised as ‘low-average’; those with ratios greater than the median up to three times the median as ‘high-average’; and those greater than three times the median as ‘high’
* P<0.05, two-sided test
Co-occurrence with other DSM-IV disorders
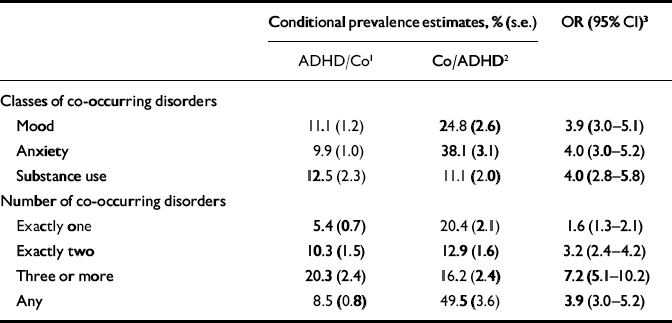
Adult ADHD was significantly associated with a wide range of other 12-month DSM–IV disorders (Table 4). The strength of these associations in terms of odds ratios was remarkably consistent across classes of disorder, with OR=3.9 (95% CI 3.0–5.1) for mood disorders, OR=4.0 (95% CI 3.0–5.2) for anxiety disorders and OR=4.0 (95% CI 2.8–5.8) for substance use disorders. A dose–response relationship exists between ADHD and number of other disorders, with the highest odds ratio (OR=7.2, 95% CI 5.1–10.2) associated with having three or more other disorders. Within-country patterns were similar to those in the combined sample, with a predominantly positive sign pattern (68 of the 70 odds ratios in the ten separate countries were greater than 1.0) and 56% of the within-country odds ratios significant at the P<0.05 level. However, this pattern was notably weaker in France (further details available from the authors).
Table 4 Bivariate lifetime co-occurrence of multiply imputed adult attention-deficit hyperactivity disorder and other DSM–IV disorders (n=11 422)
| Conditional prevalence estimates, % (s.e.) | OR (95% CI) 3 | |||
|---|---|---|---|---|
| ADHD/Co 1 | Co/ADHD 2 | |||
| Classes of co-occurring disorders | ||||
| Mood | 11.1 (1.2) | 24.8 (2.6) | 3.9 (3.0–5.1) | |
| Anxiety | 9.9 (1.0) | 38.1 (3.1) | 4.0 (3.0–5.2) | |
| Substance use | 12.5 (2.3) | 11.1 (2.0) | 4.0 (2.8–5.8) | |
| Number of co-occurring disorders | ||||
| Exactly one | 5.4 (0.7) | 20.4 (2.1) | 1.6 (1.3–2.1) | |
| Exactly two | 10.3 (1.5) | 12.9 (1.6) | 3.2 (2.4–4.2) | |
| Three or more | 20.3 (2.4) | 16.2 (2.4) | 7.2 (5.1–10.2) | |
| Any | 8.5 (0.8) | 49.5 (3.6) | 3.9 (3.0–5.2) | |
ADHD, attention-deficit hyperactivity disorder; Co, comorbid disorder
1. Conditional prevalence estimates of adult ADHD in the subsamples of respondents with the comorbid disorders
2. Conditional prevalence estimates of the comorbid disorders in the subsample of respondents with adult ADHD
3. All odds ratios significant at P<0.05, two-sided test
Temporal priorities among co-occurring disorders
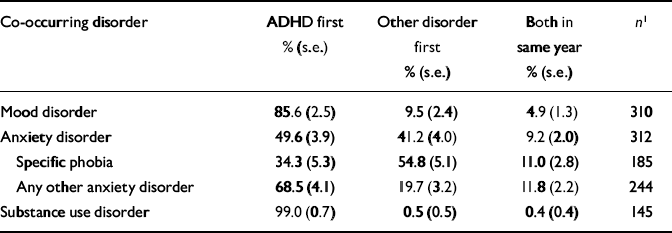
Retrospective reports of age at onset were used to compare temporal priority between the first onset of ADHD and that of co-occurring disorders among respondents with adult ADHD (Table 5). The ADHD was reported to have started at an earlier age than the vast majority of co-occurring mood disorders (85.6%), anxiety disorders other than specific phobia (68.5%) and substance use disorders (99.0%). However, co-occurring specific phobia was reported to start at an earlier age than ADHD more often than the reverse (54.8% specific phobia first v. 34.3% ADHD first). These patterns are very robust across countries (further details available from the authors).
Table 5 Temporal priorities in first onset of co-occurring adult attention-deficit hyperactivity disorder and other DSM–IV disorders
| Co-occurring disorder | ADHD first % (s.e.) | Other disorder first % (s.e.) | Both in same year % (s.e.) | n 1 |
|---|---|---|---|---|
| Mood disorder | 85.6 (2.5) | 9.5 (2.4) | 4.9 (1.3) | 310 |
| Anxiety disorder | 49.6 (3.9) | 41.2 (4.0) | 9.2 (2.0) | 312 |
| Specific phobia | 34.3 (5.3) | 54.8 (5.1) | 11.0 (2.8) | 185 |
| Any other anxiety disorder | 68.5 (4.1) | 19.7 (3.2) | 11.8 (2.2) | 244 |
| Substance use disorder | 99.0 (0.7) | 0.5 (0.5) | 0.4 (0.4) | 145 |
ADHD, attention-deficit hyperactivity disorder
1. Number of respondents with co-occurrence of adult ADHD and the type of disorder specified
Disability
Adult ADHD was associated with significantly elevated odds ratios of disability in two of the three WHO–DAS dimensions of basic functioning –mobility (OR=2.2, 95% CI 1.6–2.9) and cognition (OR=3.9, 95% CI 2.8–5.4) – but not in the third dimension of self-care (OR=1.5, 95% CI 0.8–2.8) (Table 6). Adult ADHD was also associated with elevated risk of high number of days out of role (OR=2.6, 95% CI 2.0–3.5) and with disability in social functioning (OR=3.1, 95% CI 2.1–4.5). These associations become somewhat weaker but remain statistically significant when controls are introduced for co-occurring anxiety, mood and substance use disorders. Within-country patterns are again similar to those in the combined sample, with 82% of within-country odds ratios greater than 1.0 and 46% significant at the P<0.05 level (further details available from the authors). The Netherlands is the only country where reported disability was consistently and significantly lower than the results in the combined sample. Only a handful of other within-country odds ratios differed significantly from the cross-national averages.
Table 6 Disability in 30-day functioning associated with adult attention-deficit hyperactivity disorder (n=11 422)

| Disability | % (s.e.) | With controls for socio-demographic data 1 OR (95% CI) | With controls for socio-demographic data and other DSM–IV disorders 2 OR (95% CI) |
|---|---|---|---|
| Self-care | 4.2 (1.0) | 1.5 (0.8–2.8) | 0.9 (0.5–1.6) |
| Mobility | 16.9 (1.9) | 2.2 * (1.6–2.9) | 1.5 * (1.1–2.0) |
| Cognitive | 20.5 (2.6) | 3.9 * (2.8–5.4) | 2.2 * (1.5–3.3) |
| Days out of role | 31.4 (3.0) | 2.6 * (2.0–3.5) | 1.8 * (1.3–2.5) |
| Social interaction | 10.7 (1.7) | 3.1 * (2.1–4.5) | 1.5 * (1.0–2.2) |
1. Based on logistic regression equations controlling for country, age, education, employment, marital status and income
2. Based on logistic regression equations controlling for country, age, education, employment, marital status, income, any mood disorder, any anxiety disorder and any substance use disorder
* P<0.05 level, two-sided test
Twelve-month treatment
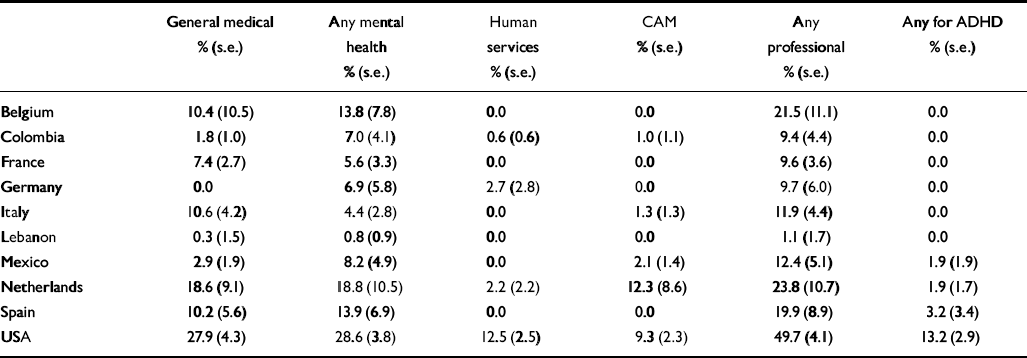
Patterns of treatment for emotional or substance use problems in the 12 months before interview among respondents with adult ADHD differed much more markedly across surveys than did any of the other statistics examined in this report (Table 7). The highest proportion of cases receiving treatment was in the USA, where nearly half (49.7%) of respondents reported some type of care, followed by roughly half as many (19.9–23.8%) receiving treatment in three of the European countries (Belgium, The Netherlands and Spain), roughly half this proportion (9.4–12.4%) in four other countries (Colombia, France, Germany and Mexico) and only 1.1% in Lebanon. The majority of people receiving treatment were seen in the specialty mental health sector in all countries other than France and Italy, where the majority were seen in the general medical sector. It is important to recognise that these patients were generally seen not for problems with attention, concentration, impulsivity or hyperactivity, but rather for other emotional or behavioural problems.
Table 7 Twelve-month treatment among respondents with multiply imputed adult attention-deficit hyperactivity disorder
| General medical % (s.e.) | Any mental health % (s.e.) | Human services % (s.e.) | CAM % (s.e.) | Any professional % (s.e.) | Any for ADHD % (s.e.) | |
|---|---|---|---|---|---|---|
| Belgium | 10.4 (10.5) | 13.8 (7.8) | 0.0 | 0.0 | 21.5 (11.1) | 0.0 |
| Colombia | 1.8 (1.0) | 7.0 (4.1) | 0.6 (0.6) | 1.0 (1.1) | 9.4 (4.4) | 0.0 |
| France | 7.4 (2.7) | 5.6 (3.3) | 0.0 | 0.0 | 9.6 (3.6) | 0.0 |
| Germany | 0.0 | 6.9 (5.8) | 2.7 (2.8) | 0.0 | 9.7 (6.0) | 0.0 |
| Italy | 10.6 (4.2) | 4.4 (2.8) | 0.0 | 1.3 (1.3) | 11.9 (4.4) | 0.0 |
| Lebanon | 0.3 (1.5) | 0.8 (0.9) | 0.0 | 0.0 | 1.1 (1.7) | 0.0 |
| Mexico | 2.9 (1.9) | 8.2 (4.9) | 0.0 | 2.1 (1.4) | 12.4 (5.1) | 1.9 (1.9) |
| Netherlands | 18.6 (9.1) | 18.8 (10.5) | 2.2 (2.2) | 12.3 (8.6) | 23.8 (10.7) | 1.9 (1.7) |
| Spain | 10.2 (5.6) | 13.9 (6.9) | 0.0 | 0.0 | 19.9 (8.9) | 3.2 (3.4) |
| USA | 27.9 (4.3) | 28.6 (3.8) | 12.5 (2.5) | 9.3 (2.3) | 49.7 (4.1) | 13.2 (2.9) |
ADHD, attention-deficit hyperactivity disorder; CAM, complementary and alternative medicine
DISCUSSION
Our findings have to be interpreted in the context of several important limitations. First, the diagnoses of adult ADHD in both the DIS and clinical reappraisal interviews were based on adult self-reports. Childhood ADHD is diagnosed on the basis of parent and teacher reports because children with ADHD often are unaware of their symptoms (Reference Jensen, Rubio-Stipec and CaninoJensen et al, 1999). Use of informants, such as spouses or work supervisors, to assess adult ADHD is much more difficult (although ideal in clinical settings), making it necessary to base assessment largely on self-report (Reference Wender, Wolf and WassersteinWender et al, 2001). Although the one study that compared adult self-reports with informant reports of ADHD symptoms in a non-clinical sample found fairly strong associations between the two reports (Reference Murphy and SchacharMurphy & Schachar, 2000), our use of self-report without confirmation by informant reports still has to be seen as a limitation.
More importantly, our use of imputation to estimate adult ADHD introduced several other important limitations that need to be recognised in interpreting our results. For one, the model relied on retrospective assessments of childhood symptoms in conjunction with only a single question about recent adult persistence. Even though these responses were strongly related to independent clinical assessments of adult ADHD in the US sample, the coarse classification created by relying on only a single question about recency limited the texture with which we could study correlates of adult ADHD. This coarseness reduces the precision of estimates and, with it, attenuates measures of association. In addition, the imputation model was based on a clinical calibration conducted only in the USA. We have no way of confirming the analytical assumption that the positive and negative predictive values estimated to calibrate the imputations are the same in the other countries studied – an assumption that is fundamental to the imputation method. This is especially problematic given that, as noted in the introduction, little research on adult ADHD has been conducted outside the USA, making it unclear if the same markers apply in other countries. Given the centrality of this issue, it is important that the CIDI assessment of adult ADHD is expanded for use in future CIDI surveys (an expansion that has, in fact, been implemented in the second flight of WMH surveys that are currently taking place) and that the validity of these diagnoses is assessed with clinician-administered diagnostic interviews in clinical reappraisal studies embedded within future surveys in countries other than the USA. Another limitation of the imputation model – which would be relevant even if the model were equally accurate in all countries – is that it understates the strength of associations of adult ADHD with covariates that, owing to limitations of sample size, were not included as predictors in the model. This means that the evidence regarding socio-demographic correlates of adult ADHD reported here is likely to be conservative.
Finally, a question can be raised about the validity of the DSM–IV ADHD criteria when applied to adults, considering they were developed with children in mind. Clinical studies make it clear that symptoms of ADHD are more heterogeneous and subtle in adults than in children (Reference De Quiros and KinsbourneDe Quiros & Kinsbourne, 2001), leading some clinical researchers to suggest that assessment of adult ADHD might require an increase in the variety of symptoms assessed (Reference BarkleyBarkley, 1995), a reduction in the severity threshold (Reference Ratey, Greenberg and BemporadRatey et al, 1992) or a reduction in the DSM–IV ‘six of nine’ symptom requirement (Reference Kooij, Buitelaar and van den OordKooij et al, 2005). To the extent that such considerations in the criteria would lead to a more valid assessment than in the current study, our prevalence estimate is conservative.
Within the context of these limitations, the results reported suggest that adult ADHD as currently defined in the DSM–IV is a commonly occurring and often seriously impairing disorder. The 3.4% estimated prevalence is likely to be conservative for the reasons described above. Although we would expect to find some variation in prevalence from one country to another, the amount of cross-national variation in the estimated prevalence is small compared with estimates for other disorders (Reference Demyttenaere, Bruffaerts and Posada-VillaDemyttenaere et al, 2004). This low variation might be due to methodological factors such as a general lack of awareness about ADHD that makes it difficult for respondents to discriminate between questions, or that leads to normative cultural interpretations of certain symptoms (e.g. a high tolerance of hyperactivity in boys). Another possibility, though, is that adult ADHD is less strongly related than other disorders to environmental determinants that can vary across countries.
The findings that adult ADHD is significantly more prevalent among men than women and among people with low rather than high educational levels are consistent with much previous research (Reference Scahill and Schwab-StoneScahill & Schwab-Stone, 2000) and, as noted above in the discussion of limitations, are likely to be underestimates of the strength of these associations owing to the attenuation introduced by the coarseness of the imputations. The failure to find an elevated prevalence of ADHD among unemployed people, however, is inconsistent with these same studies. Nonetheless, we do find that WMH respondents estimated to have ADHD report significantly more disability in role functioning, as indicated by more days out of role and more disability in social role functioning, than comparable respondents without ADHD. These results regarding role disability are consistent with much previous research on disability in adult ADHD (Reference Able, Johnston and AdlerAble et al, 2007). It is noteworthy that the WHO–DAS dimension associated with the highest impairment in the current study is the cognitive disability dimension. This finding is as one would expect, given the nature of the disorder. However, the WHO–DAS might underrepresent ADHD disability because some WHO–DAS dimensions tap areas where ADHD is not highly disabling (e.g. people with ADHD are often very mobile and overwork) and because the WHO–DAS does not assess many dimensions where people with ADHD are thought to function less adequately (e.g. poor sleep and nutrition, high rates of accidents, high levels of smoking). Moreover, people with ADHD often have poor insight into their functioning, possibly leading to underestimation of WHO–DAS scores. It might also be that the social and interpersonal disabilities associated with adult ADHD require more detailed probing to detect than provided in the WHO–DAS. Based on these considerations, along with the more general problem noted above that imputation leads to attenuation of associations, the disabilities due to ADHD are likely to be underestimated. This makes it all the more striking that adult ADHD is consistently associated across countries with substantial elevations in disability that cannot be accounted for by co-occurring disorders.
The estimate that adult ADHD often co-occurs with other DSM–IV disorders is consistent with clinical evidence (Reference BiedermanBiederman, 2004). Methodological analysis shows that the evidence of co-occurrence holds up when careful diagnoses are made aimed at adjusting for overlap of symptoms, imprecision of diagnostic criteria, or other methodological confounds (Reference Angold, Costello and ErkanliAngold et al, 1999). The results regarding co-occurrence in our report, however, are likely to be much less precise – both because diagnoses of co-occurring disorders are based on a fully structured interview that, due to its limited ability to make differential diagnoses, will cause overestimation of co-occurrence, and because the diagnoses of adult ADHD are based on coarse imputations that, due to their individual-level imprecision, will lead to attenuation of correlations with other variables and consequent underestimation of systematic co-occurrence (i.e. underestimation of odds ratios).
As one might expect from the early onset of ADHD, comparison of reports of age at onset showed that the estimated co-occurrence in the WMH surveys is due to temporally primary ADHD being related to the subsequent onset of other disorders. The main exception here is co-occurring specific phobia, which is typically temporally primary to ADHD. This last observation raises the question whether early successful treatment of childhood ADHD would influence secondary adult disorders, an issue that is beyond the scope of the current report to investigate. A related question is whether adult treatment of ADHD would have any effect on severity or persistence of co-occurring temporally secondary disorders. Long-term research is needed to answer these questions. The results reported here highlight the importance of such long-term research by documenting that adult ADHD is a relatively common disorder in a number of countries, often co-occurs with largely temporally secondary conditions, and that it is associated with substantial impairment in adult role functioning.
Acknowledgements
The surveys discussed above were carried out in conjunction with the World Health Organization World Mental Health (WMH) Survey Initiative. We thank the WMH staff for assistance with instrumentation, fieldwork and data analysis. These activities were supported by the US National Institute of Mental Health (R01-MH070884), the John D. and Catherine T. MacArthur Foundation, the Pfizer Foundation, the US Public Health Service (R13-MH066849, R01-MH069864 and R01-DA016558), the Fogarty International Center (FIRCA R01-TW006481), the Pan American Health Organization, Eli Lilly and Company, Ortho-McNeil Pharmaceutical, Inc., GlaxoSmithKline and Bristol-Myers Squibb. The current report was additionally supported by Eli Lilly and Company. A complete list of WMH publications can be found at http://www.hcp.med.harvard.edu/wmh/. The Chinese World Mental Health Survey Initiative is supported by the Pfizer Foundation. The Colombian National Study of Mental Health is supported by the Ministry of Social Protection, with supplemental support from the Saldarriaga Concha Foundation. The European Study of the Epidemiology of Mental Disorders (ESEMeD) project is funded by the European Commission (contracts QLG5-1999-01042; SANCO 2004123), the Piedmont Region (Italy), Fondo de Investigación Sanitaria, Instituto de Salud Carlos III, Spain (FIS 00/0028), Ministerio de Ciencia y Tecnología, Spain (SAF 2000-158-CE), Departament de Salut, Generalitat de Catalunya, Spain, RETICS RD06/0011 REM-TAP, and other local agencies and by an unrestricted educational grant from GlaxoSmithKline. The Lebanese Evaluation of the Burden of Ailments and Needs of the Nation (LEBANON) survey was partially supported by anonymous private donations to the Institute for Development, Research, Advocacy and Applied Care (IDRAAC), Lebanon (http://www.idraac.org), and by the Lebanese Ministry of Public Health, the World World Health Organization (WHO, Lebanon), Act 4 Lebanon, The National Arab-American Medical Association and unrestricted grants from Janssen Cilag, Eli Lilly and Company, GlaxoSmithKline, Roche and Novartis. The Mexico National Comorbidity Survey is supported by the National Institute of Psychiatry Ramon de la Fuente (INPRFMDIES 4280) and by the National Council on Science and Technology (CONACyT-G30544-H), with supplemental support from the Pan American Health Organization. The US National Comorbidity Survey Replication is supported by the National Institute of Mental Health (NIMH U01-MH60220) with supplemental support from the National Institute of Drug Abuse, the Substance Abuse and Mental Health Services Administration, the Robert Wood Johnson Foundation (RWJF grant 044780) and the John W. Alden Trust. Professor Kessler, as Director of the WMH Data Analysis Coordination Centre, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Professor Kessler was responsible for instrument design and supervision of data analysis. The co-authors co-authors were responsible for preparing the first draft of the manuscript, data collection and making critical revisions to the manuscript.












eLetters
No eLetters have been published for this article.