The risk of premature death among psychiatric patients is higher than in the general population (Reference Amaddeo, Bisoffi and BonizzatoAmaddeo et al, 1995; Reference Sohlman and LehtinenSohlman & Lehtinen, 1999). Only few studies have dealt with the issue of mortality and diagnosed mental disorders in the community. A psychiatric diagnosis per se increases the risk of dying prematurely (Reference Rorsman, Hagnell and LankeRorsman et al, 1982; Reference Lehtinen, Veijola and LindholmLehtinen et al, 1993). Among men, alcohol-related disorders (Reference Ojesjo, Hagnell and OtterbeckOjesjo et al, 1998) and anxiety or panic disorder (Reference Grasbeck, Rorsman and HagnellGrasbecket al, 1996) are associated with excessive mortality. Our own earlier studies have shown that neurotic depression is associated with an elevated risk of death due to cardiovascular disease (Reference Aromaa, Raitasalo and ReunanenAromaa et al, 1994). As far as we know, no population study exists on cause-specific mortality related to mental disorders. Our aim was to establish the significance of mental disorders as predictors for disease-specific mortality, using a representative population sample and a 17-year follow-up period.
METHOD
Design
This study forms a part of the Mini-Finland Health Survey, an extensive epidemiological study of the adult Finnish population. The aim of the study is to measure the health status, morbidity and health needs of Finns aged 30 years or over. The illnesses chosen as the main targets were those most frequently causing working disability: diseases of the cardiovascular and respiratory systems, mental disorders, and diseases of the musculoskeletal system and connective tissue. Baseline examinations took place during the period 1977-1980 and the results have been described in detail elsewhere (Reference Aromaa, Heliövaara, Impivaara, Aromaa, Heliövaara and ImpivaaraAromaa et al, 1989).
Sample
The study population was a stratified two-stage cluster sample drawn from the population register to represent Finnish adults aged 30 years and over (Reference Aromaa, Heliövaara, Impivaara, Aromaa, Heliövaara and ImpivaaraAromaa et al, 1989). In the first stage, 40 representative areas were selected. In the second stage, a systematic sample of inhabitants was drawn from each area. The total sample consisted of 8000 persons (3637 men and 4363 women) from 69 municipalities. The data were collected between 1977 and 1980. The examinations were carried out by the mobile clinic of the Social Insurance Institution (SII) in two phases: a screening phase and a diagnostic (clinical) phase. A total of 7217 persons (90.2% of the sample) participated in the screening phase. Regarding the distributions of gender, age and level of education, the participants corresponded closely to the whole Finnish population (Reference Aromaa, Heliövaara, Impivaara, Aromaa, Heliövaara and ImpivaaraAromaa et al, 1989).
Instruments
Baseline examination
The methods used and the basic results concerning mental disorders in the Mini-Finland Health Survey have been described in detail elsewhere (Lehtinenet al, Reference Lehtinen, Joukamaa and Jyrkinen1990a,Reference Lehtinen, Joukamaa and Jyrkinenb). The screening for mental disorders was designed to be as sensitive as possible in order to minimise the number of false-negative cases, as no person screening negative was invited to join the clinical phase of the study. The most important part of the screen was the 36-item version of the General Health Questionnaire (GHQ-36; Reference GoldbergGoldberg, 1972). People were also invited to participate in the clinical phase if SII records indicated that they were receiving a disability pension because of a mental disorder, or were entitled to reimbursable medication for such disorders (according to the National Health Insurance scheme in Finland, all psychoses entitle the individual to reimbursable medication). Subjects were also included if they reported having used health services (including those provided by a general practitioner) for a mental disorder or there was a self-perceived mental disturbance. A total of 35% of the participants in the screening phase were picked out by various screening instruments; 95% of them cooperated when invited to participate in the clinical phase of the health examination.
The most important method of psychiatric case identification in the clinical phase was the short version of the ninth edition of the Present State Examination (PSE; Reference Wing, Cooper and SartoriusWing et al, 1974), administered by a specialist psychiatric nurse. The training for the use of the PSE interview was obtained from the developers of the method. The diagnoses were generated by the computer program CATEGO-ID (Reference Wing, Mann and LeffWing et al, 1978). Diagnostic information was also obtained from the following sources: diagnostic data on patients hospitalised for psychiatric care; data recorded by the SII on disability pensions granted because of a mental disorder; data recorded by the SII on the presence of mental disorders (psychoses) entitling the person to reimbursable medication; possible diagnoses of a mental disorder by the physician in the clinical phase of the survey; and diagnostic assessment made by the PSE interviewer. A panel of two psychiatrists went through the mental hospital case notes and psychiatric documents entitling the patient to SII benefits (disability pensions and reimbursable medicines), and checked the validity of the diagnoses. For the purpose of the final diagnostic assessment, all the information collected from the various sources was combined, taking into account its degree of certainty, and eliminating mutually incompatible diagnostic combinations.
In this study the following diagnostic categories were considered: any mental disorder; functional psychoses (especially schizophrenia); mood disorders (neurotic depression and affective psychosis); and all neuroses (anxiety neurosis, phobic neurosis, obsessive neurosis, neurotic depression and other neurosis).
Follow-up
The mortality of the survey participants has been systematically followed ever since the baseline examination. This information was obtained from the Central Statistical Office of Finland, and the principal causes of death were coded according to the eighth revision of the International Classification of Diseases (World Health Organization, 1974). This report covers the deaths occurring between 1978 and 1994, and represents an observation period of 15-17 years and an overall experience of 80 089 person years (men, 39 804 person years; women, 49 285 person years). During the follow-up period 1597 deaths occurred, of which 876 were caused by any cardiovascular disease (537 by coronary disease, 192 by cerebrovascular disease), 130 by respiratory disease, 341 by different kinds of cancers, 72 by injuries and 20 by suicides.
Statistical analyses
Cox's proportional hazards regression model (Reference CoxCox, 1972; Reference Kalbfleisch and PrenticeKalbfleisch & Prentice, 1980) was used to estimate the association between mental disorders and different types of mortality. Age-adjusted relative risks (RR) and their 95% confidence intervals (CI) were estimated based on this model. Interactions between gender and mental disorders were tested by entering interaction terms of gender and each disorder into the model in addition to age, gender and the disorder. The statistical significance of covariance terms was evaluated by the likelihood ratio test and expressed as exact P values. The proportional hazards assumption was tested by stratification for follow-up time. The SAS software package version 6.12 (SAS Institute, 1997) was used.
RESULTS
The presence of any mental disorder at the time of the baseline study was associated with a statistically significantly elevated risk of death in men (RR 1.56, 95% CI 1.32-1.84, Table 1) as well as in women (RR 1.38, 95% CI 1.18-1.63, Table 2). In men it was due to excess mortality from cardiovascular disease in general, coronary heart disease, respiratory disease, nonsuicidal injuries and suicide. Women with any mental disorder had a higher risk than other women of dying of cardiovascular disease in general, coronary heart disease, respiratory disease and suicide.
Table 1 Mental disorders and mortality adjusted for age, men

| Type of mental disorder | All cases (n) | All deaths (n=856) | Cardiovascular deaths (n=473) | Cancer deaths (n=182) | Injuries (excluding suicides) (n=42) | Suicides (n=16) | Cerebrovascular deaths (n=88) | Coronary deaths (n=319) | Respiratory deaths (n=72) | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | ||
| Any mental disorder | 494 | 182 | 1.56 | 1.32-1.84 | 89 | 1.34 | 1.06-1.69 | 32 | 1.24 | 0.84-1.81 | 14 | 2.89 | 1.52-5.49 | 7 | 5.06 | 1.88-13.64 | 15 | 1.18 | 0.68-2.07 | 62 | 1.39 | 1.06-1.84 | 19 | 2.08 | 1.23-3.52 |
| Functional psychosis | 62 | 32 | 2.71 | 1.90-3.87 | 15 | 2.34 | 1.40-3.91 | 5 | 1.95 | 0.80-4.75 | 1 | 1.52 | 0.21-11.04 | 3 | 14.82 | 4.21-52.21 | 3 | 2.70 | 0.85-8.57 | 9 | 2.01 | 1.03-3.90 | 6 | 7.05 | 3.04-16.35 |
| Schizophrenia | 46 | 25 | 3.29 | 2.21-4.91 | 12 | 2.92 | 1.65-5.20 | 4 | 2.43 | 0.90-6.56 | 1 | 2.20 | 0.30-16.00 | 2 | 12.39 | 2.81-54.66 | 2 | 2.86 | 0.70-11.69 | 7 | 2.40 | 1.13-5.09 | 5 | 9.50 | 3.79-23.84 |
| Mood disorders | 130 | 56 | 1.62 | 1.23-2.12 | 32 | 1.67 | 1.16-2.39 | 10 | 1.35 | 0.71-2.55 | 4 | 2.52 | 0.90-7.07 | 2 | 4.15 | 0.94-18.33 | 4 | 1.07 | 0.39-2.92 | 23 | 1.80 | 1.18-2.75 | 3 | 0.97 | 0.31-3.09 |
| Neuroses | 246 | 60 | 0.97 | 0.74-1.26 | 30 | 0.88 | 0.61-1.27 | 12 | 0.89 | 0.50-1.61 | 5 | 1.67 | 0.65-4.24 | 0 | - | 5 | 0.80 | 0.32-1.97 | 23 | 1.00 | 0.66-1.53 | 4 | 0.81 | 0.30-2.23 | |
| Neurotic depression | 120 | 52 | 1.65 | 1.25-2.19 | 29 | 1.66 | 1.14-2.42 | 9 | 1.34 | 0.68-2.61 | 4 | 2.77 | 0.99-7.78 | 2 | 4.49 | 1.02-19.82 | 2 | 0.58 | 0.14-2.36 | 22 | 1.89 | 1.23-2.92 | 3 | 1.07 | 0.34-3.42 |
| Phobic neurosis | 142 | 29 | 1.02 | 0.70-1.48 | 15 | 0.99 | 0.59-1.65 | 4 | 0.64 | 0.24-1.72 | 4 | 2.58 | 0.92-7.26 | 0 | - | 3 | 1.17 | 0.37-3.72 | 10 | 0.94 | 0.50-1.76 | 2 | 0.99 | 0.24-4.07 | |
| Other neurosis | 87 | 26 | 0.88 | 0.59-1.30 | 12 | 0.72 | 0.41-1.28 | 7 | 1.12 | 0.53-2.39 | 1 | 0.77 | 0.11-5.63 | 0 | - | 2 | 0.62 | 0.15-2.51 | 10 | 0.92 | 0.49-1.73 | 2 | 0.78 | 0.19-3.18 | |
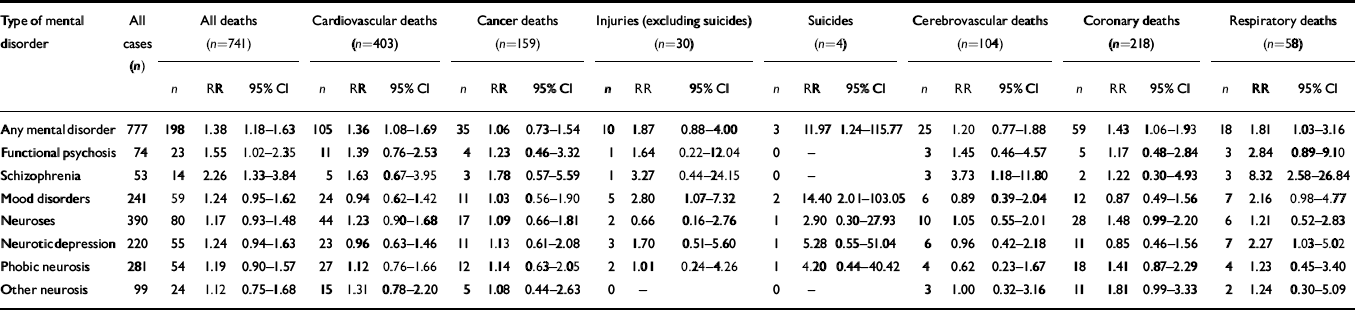
Table 2 Mental disorders and mortality adjusted for age, women
| Type of mental disorder | All cases (n) | All deaths (n=741) | Cardiovascular deaths (n=403) | Cancer deaths (n=159) | Injuries (excluding suicides) (n=30) | Suicides (n=4) | Cerebrovascular deaths (n=104) | Coronary deaths (n=218) | Respiratory deaths (n=58) | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | n | RR | 95%CI | ||
| Any mental disorder | 777 | 198 | 1.38 | 1.18-1.63 | 105 | 1.36 | 1.08-1.69 | 35 | 1.06 | 0.73-1.54 | 10 | 1.87 | 0.88-4.00 | 3 | 11.97 | 1.24-115.77 | 25 | 1.20 | 0.77-1.88 | 59 | 1.43 | 1.06-1.93 | 18 | 1.81 | 1.03-3.16 |
| Functional psychosis | 74 | 23 | 1.55 | 1.02-2.35 | 11 | 1.39 | 0.76-2.53 | 4 | 1.23 | 0.46-3.32 | 1 | 1.64 | 0.22-12.04 | 0 | - | 3 | 1.45 | 0.46-4.57 | 5 | 1.17 | 0.48-2.84 | 3 | 2.84 | 0.89-9.10 | |
| Schizophrenia | 53 | 14 | 2.26 | 1.33-3.84 | 5 | 1.63 | 0.67-3.95 | 3 | 1.78 | 0.57-5.59 | 1 | 3.27 | 0.44-24.15 | 0 | - | 3 | 3.73 | 1.18-11.80 | 2 | 1.22 | 0.30-4.93 | 3 | 8.32 | 2.58-26.84 | |
| Mood disorders | 241 | 59 | 1.24 | 0.95-1.62 | 24 | 0.94 | 0.62-1.42 | 11 | 1.03 | 0.56-1.90 | 5 | 2.80 | 1.07-7.32 | 2 | 14.40 | 2.01-103.05 | 6 | 0.89 | 0.39-2.04 | 12 | 0.87 | 0.49-1.56 | 7 | 2.16 | 0.98-4.77 |
| Neuroses | 390 | 80 | 1.17 | 0.93-1.48 | 44 | 1.23 | 0.90-1.68 | 17 | 1.09 | 0.66-1.81 | 2 | 0.66 | 0.16-2.76 | 1 | 2.90 | 0.30-27.93 | 10 | 1.05 | 0.55-2.01 | 28 | 1.48 | 0.99-2.20 | 6 | 1.21 | 0.52-2.83 |
| Neurotic depression | 220 | 55 | 1.24 | 0.94-1.63 | 23 | 0.96 | 0.63-1.46 | 11 | 1.13 | 0.61-2.08 | 3 | 1.70 | 0.51-5.60 | 1 | 5.28 | 0.55-51.04 | 6 | 0.96 | 0.42-2.18 | 11 | 0.85 | 0.46-1.56 | 7 | 2.27 | 1.03-5.02 |
| Phobic neurosis | 281 | 54 | 1.19 | 0.90-1.57 | 27 | 1.12 | 0.76-1.66 | 12 | 1.14 | 0.63-2.05 | 2 | 1.01 | 0.24-4.26 | 1 | 4.20 | 0.44-40.42 | 4 | 0.62 | 0.23-1.67 | 18 | 1.41 | 0.87-2.29 | 4 | 1.23 | 0.45-3.40 |
| Other neurosis | 99 | 24 | 1.12 | 0.75-1.68 | 15 | 1.31 | 0.78-2.20 | 5 | 1.08 | 0.44-2.63 | 0 | - | 0 | - | 3 | 1.00 | 0.32-3.16 | 11 | 1.81 | 0.99-3.33 | 2 | 1.24 | 0.30-5.09 | ||
Both male and female participants with functional psychoses at the time of the baseline study possessed statistically significantly elevated risks of death. This was especially true in the schizophrenia category. In people with schizophrenia the risk of dying of respiratory disease was almost 10 times that in the other participants. Deaths from respiratory disease in the schizophrenia group were due to chronic bronchitis in three men, bronchial asthma in one woman, and pneumonia in two men and two women. Regarding cardiovascular mortality there seemed to be an interaction with gender and schizophrenia (Tables 1 and 2), although it was not statistically significant (χ2=2.17, d.f.=1, P=0.14). In men the risk of dying was statistically significantly higher in the case of cardiovascular disease in general and especially with regard to coronary disease. In women the risk of dying was higher only in the case of cerebrovascular disease. In men with schizophrenia the risk of death by suicide was also statistically significantly elevated compared with other subjects.
When all the study participants were analysed together and the mortality rates had been adjusted for gender and age, there was a statistically significant association between schizophrenia and death due to cancers (RR 2.13, 95% CI 1.01-4.51), but this association did not reach statistical significance in either gender alone (Tables 1 and 2).
Men suffering from mood disorders also had an elevated risk of death. In cases of suicide and cardiovascular disease, especially coronary disease, the excess mortality was associated with neurotic depression. Mood disorders in women were associated with an elevated risk of death from injuries and suicide. Neurotic depression was associated with an elevated risk of death from respiratory disease among women. In women, unlike men, neurotic depression did not predict cardiovascular death (Tables 1 and 2). The interaction between gender and mood disorders for the prediction of cardiovascular mortality was statistically significant (χ2=4.63, d.f.=1,P=0.03).
To study whether the association between mental disorders and mortality remained during the long follow-up period, we deleted the first 10 years of follow-up from the analysis. Even then, the relative risk of death adjusted for age and gender in subjects with mental disorder was 1.68 (95% CI 1.37-2.07) compared with those without baseline mental disorder.
DISCUSSION
Our results show in a representative sample of adult people a clear association between clinically diagnosed mental disorders and mortality, with regard to both natural and unnatural deaths. Having a mental disorder predicted an elevated risk of death from cardiovascular diseases in total, coronary heart disease, respiratory disease and suicide. In particular, schizophrenia and depression are involved. Excess suicidal mortality associated with these disorders, earlier reported on the basis of patient studies, was now confirmed at population level. As far as we know, this is the first comprehensive study on this topic that deals not with patient series, but with different mental disorders in relation to the general population. A new finding of this study was the association of schizophrenia with mortality from respiratory disease. Our finding of a connection between neurotic depression and premature death due to coronary heart disease in men was in full agreement with our previous study with the same material in a 6-year follow-up (Reference Aromaa, Raitasalo and ReunanenAromaa et al, 1994).
Schizophrenia and mortality
We found a considerable excess mortality from respiratory disease in people with schizophrenia. In a meta-analysis, Brown (Reference Brown1997) reported that natural deaths account for about 59% of the excess mortality in the schizophrenia group, but there is no clear finding implicating any specific somatic disease. However, according to patient studies the greatest number of excess deaths in schizophrenia are due to infectious diseases and to endocrine, circulatory, respiratory, digestive and genito-urinary disorders (Reference Harris and BarracloughHarris & Barraclough, 1998). It has been suggested that ordinary and excessive smoking among patients with schizophrenia could elevate lung cancer mortality rates (Reference Masterson and O'SheaMasterson & O'Shea, 1984). Cancer deaths (combined) had only a weak association with schizophrenia in our study. On the other hand, this same Mini-Finland Health Survey material has been used to show that depressed mood was associated with an elevated risk for lung cancer (Reference Knekt, Raitasalo and HeliövaaraKnektet al, 1996). The excess mortality due to respiratory disease, especially chronic bronchitis, is probably associated with smoking. Smoking and other unhealthy habits in people with schizophrenia may also be responsible for the excess mortality from cardiovascular disease.
In earlier studies with patient samples, unnatural causes, suicides and accidents have been the most important reasons for excess mortality in schizophrenia (Reference BrownBrown, 1997; Reference Harris and BarracloughHarris & Barraclough, 1998). In our study the risk of committing suicide was highly elevated among men. This may be due to the small absolute number of cases of schizophrenia (n=99). In our study no statistically significant association between non-suicidal lethal injuries and schizophrenia was found.
Neurotic depression and mortality
In our study neurotic depression (in men only) was associated with excess mortality due to coronary heart disease. The relationship between depression and cardiovascular disease has recently come under scrutiny. Pratt et al (Reference Pratt, Ford and Crum1996) suggested that a history of dysphoria and major depressive episode increase the risk of myocardial infarction. The results of this study, as well as those of our earlier study (Reference Aromaa, Raitasalo and ReunanenAromaa et al, 1994), are in line with this finding. Musselman et al (Reference Musselman, Evans and Nemeroff1998) have even suggested that treatment of depression in patients with cardiovascular disease increases longevity. Why cardiovascular mortality was associated with mood disorders only in men needs to be investigated further.
We also found an association between suicide and mood disorder. Similar results have been reported in other studies with patient samples (Harris & Barraclough, Reference Harris and Barraclough1997, Reference Harris and Barraclough1998). In this study, non-suicidal lethal injuries also contributed to the excess mortality in cases of neurotic depression in women. Unfortunately, it is not possible to analyse probable suicidal intentions in these cases. It is hoped that future research will confirm our observation.
An interesting finding was that neurotic depression was associated with an elevated risk of dying from respiratory disease in women. Similar findings have been obtained also in patient studies of affective disorders (Reference Newman and BlandNewman & Bland, 1991) and of bipolar disorders (Reference Sharma and MarkarSharma & Markar, 1994). Further studies are needed to elucidate the meaning of this association. One possible explanation could be smoking, which is commonly associated with depression (Reference Covey, Glassman and StetnerCovey et al, 1998).
Anxiety disorders and mortality
Neurotic disorders other than depression did not exhibit any association with mortality in this study — a finding that is consistent with previous studies (Reference Rorsman, Hagnell and LankeRorsman et al, 1982; Reference Murphy, Monson and OlivierMurphy et al, 1989; Reference Lehtinen, Veijola and LindholmLehtinen et al, 1993). Much attention has been paid to the possible excess mortality in panic disorder due to cardiovascular disease and suicide (Reference NoyesNoyes, 1991). Panic disorder, as a type of anxiety disorder, was added to the diagnostic classifications after our study was completed. The prevalence of panic disorder is low in the normal population (Reference Weissman, Bland and CaninoWeissman et al, 1997), and consequently there was likely to be only a small number of subjects with panic disorder in our sample. This may be the reason for the lack of excess mortality among persons with neurotic disturbances, since these disorders were analysed as a single group in our study.
Limitations of the study
Our sample well represents the entire 30-year-old population of Finland. The large number of subjects made it possible to analyse in detail the associations between mental disorders and deaths due to different somatic diseases. A limitation of the study was the impossibility of using standardised diagnostic criteria for mental disorders. The baseline study was performed before the era of DSM—III—R or ICD—10 diagnostic classification rules. The main diagnostic tool was the ninth edition of the PSE, a semi-structured standardised psychiatric interview that yields the ICD—8 psychiatric diagnoses. It was at that time the foremost and most common psychiatric interview instrument in epidemiological studies in several countries (Reference Wing, Cooper and SartoriusWing et al, 1974). In addition to the PSE, diagnostic information was obtained from many other sources. A best-estimate diagnostic procedure (Reference Leckman, Sholomskas and ThompsonLeckman et al, 1982; Reference Klein, Ouimette and KellyKlein et al, 1994) was used. In this study it was not possible to analyse how consistent the diagnoses were during the long follow-up period, and confounding factors relevant to the associations between mental disorder and death were not analysed. Another limitation of the study was that it was not possible to assess the mental health of the participants after the baseline examination. It is highly probable that the group originally classified as free from mental disorder contained some people who subsequently developed a mental disorder. Thus, a cohort study such as this one is likely to provide a conservative estimate of the association between mental disorder and mortality.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
• Of the mental disorders examined, only schizophrenia and depression increased mortality.
• In people with schizophrenia the risk of dying of respiratory disease is increased.
• Mood disorders in men are associated with excess cardiovascular mortality.
LIMITATIONS
• A two-stage psychiatric interview was used. It was not possible to interview all subjects.
• Because the basic study was completed in the 1970s it was not possible to use standardised diagnostic criteria for the various mental disorders.
• The sample was not large enough to examine the relative risks for all possible mental disorders associating with mortality.







eLetters
No eLetters have been published for this article.