Background
The prevalence of mental health disorders among prisoners is considerably higher than that of the general population. Reference Fazel and Danesh1,Reference Singleton, Meltzer and Gatward2 In England, in the past, custodial healthcare had been criticised for being underfunded and provided by the prison service. A new policy in 2002 laid out plans for multiprofessional community mental health teams funded by local healthcare commissioners. 3 The target group for those teams were prisoners with a serious mental illness who were subject to the care programme approach (CPA). The CPA is the way, in England, that services are assessed, planned, coordinated and reviewed for someone with a serious mental illness. There are approximately 2700 prisoners on the CPA in English prisons. A number of national surveys allow progress with the implementation of this policy to be mapped.
Prison mental health in-reach: the national surveys
The first national prison mental health in-reach survey in 2006 identified a range of issues, from aspects of team organisation to therapeutic work and interventions, which proved extremely challenging for underresourced in-reach teams. Reference Ricketts, Brooker and Dent-Brown4 The second national prison mental health in-reach survey, in 2008, sought to examine workforce issues, team functioning, connections with primary care services, the role of in-reach, case-load activity, interventions provided, barriers to successful operation, and relationships with the wider National Health Service (NHS) during a prisoner's time in custody and at release. Reference Brooker and Gojkovic5 Key findings reported between the two survey periods were that: on average, team size increased from four to five staff members, and recruitment and retention of staff continued to be a major challenge with all teams running with vacant posts. Team leaders reported that 72% of clients were subject to the CPA – yet a core function of the teams when they were established was to manage only prisoners under the CPA, such that they were discharged with a care plan back into mainstream community services. In this manner, a focus solely only on those with serious mental illness was meant to help target scant resources. This had been the intention in prisons but general needs had been so high from other groups in prison (for example those with comorbid drug/alcohol problems or personality disorder) that ‘mission creep’ had been occurring. Reference Steel, Thornicroft, Birmingham, Brooker, Mills and Harty6 Indeed, by 2007, under half (49%) of prisoners on mental health in-reach case-loads had a serious mental illness. Reference Steel, Thornicroft, Birmingham, Brooker, Mills and Harty6 A further national survey of community mental health in-reach teams working in prisons has been reported, based on data collected in 2012. Reference Forrester, Exworthy, Olumoroti, Sessay, Parrott and Spencer7 This study concluded that even 5 years ago prison mental health spending remained sparse. It also found that there was a need for meaningful ‘inter-prison healthcare comparison’ given the inequity that exists between prisons in terms of resourcing. This survey established that in-reach team sizes had become smaller and had reduced on average to 2.9 mental health team members, although one service with eight community psychiatric nurses is reported.
In the latest national survey undertaken in 2016 it was clear that resources to provide mental healthcare in prison had increased. Reference Brooker and Webster8 In 2003 the average number of staff working in a prison mental health in-reach team was four and by 2016 this figure had increased significantly to eight. Many respondents took the time to describe whole-system approaches to mental healthcare. For example, a stepped model of care with primary care was often cited. Thus, workforce resources had increased and better organisational models of mental healthcare had evolved in comparison to previous survey periods.
Nonetheless both external reports (for example, see the report by the Prisons and Probation Ombudsman 9 ) and the qualitative data gleaned in the 2016 survey, show that the prison environment remains an extremely challenging one in which to deliver mental healthcare. Although case-loads are now of a more manageable size (17.6 prisoners per member of mental health staff), there can be immense practical difficulties in providing mental health support; obtaining an escort to prisoners' wings and abuse experienced by mental health staff are two examples. Currently, the proportion of those on case-loads who have serious mental illness has declined from 49% in 2007 to 38% now. Although in 60% of services surveyed in 2016 all those with a serious mental illness were on the CPA, figures were much lower in other teams. One service reported that the CPA was not in use at all.
Prisoners, the CPA and sexual violence
Across all prisons in England, the most recent survey allowed the following estimates to be derived. There are approximately 9850 prisoners on the case-loads of mental health in-reach teams of whom 3743 have a serious mental illness and there are 2695 prisoners on the CPA. In a freedom of information request (18 November 2016) to NHS England, the commissioners for prison mental health in-reach teams, the policy for adherence to the CPA was requested. NHS England replied as follows: ‘NHS England uses the Health and Justice Service Specification for Mental Health and Learning Disabilities. This specification includes registering patients under the Care Programme Approach where they require secondary care mental health services and the expectation that providers meet the national standards under the approach’.
In 2008 an important change was made to the CPA when it became mandatory to enquire about an individual's experience of sexual abuse or sexual violence at assessment. It is well known that prisoners have often experienced such trauma both as children and as adults. For example, a large study (n = 7500), undertaken in New York, Reference Wolff and Shi10 reported on the occurrence of abuse/trauma in relation to the presence of mental health disorder or otherwise (Table 1).
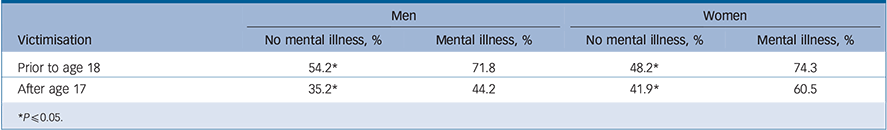
Table 1 Community victimisation history, adapted from Wolff & Shi Reference Wolff and Shi10
| Men | Women | |||
|---|---|---|---|---|
| Victimisation | No mental illness, % | Mental illness, % | No mental illness, % | Mental illness, % |
| Prior to age 18 | 54.2* | 71.8 | 48.2* | 74.3 |
| After age 17 | 35.2* | 44.2 | 41.9* | 60.5 |
* P ⩽ 0.05.
The strong relationship, for both male and female prisoners, between a history of victimisation and a mental illness is clearly shown. NHS England, as the commissioners of prison mental health services, were asked whether they expected staff to assess sexual abuse/violence under the CPA and whether they audited such routine enquiry, and they answered as follows: ‘NHS England expects its healthcare providers to clinically assess the individual needs of patients. Where appropriate, sexual assault would form one element of this assessment and would lead to the development, with the patient, of a care and treatment plan to address those needs. However, NHS England does not currently audit answers to the question in the CPA in relation to sexual abuse of sexual violence’ (freedom of information request 18 November 2016).
There is no reported research on the use of trauma counselling in English prisons although there are strong indications from the basic data presented here that this type of intervention should be offered. The Royal College of Psychiatrists have developed standards for the care of prisoners with mental health problems. Reference Georgiou, Souza and Holder11 However, their guidance in either the section on ‘admission and assessment’ or ‘case management and treatment’ makes no reference to the importance of routine enquiry.
Disappointing conclusions were reached in a study that examined the use of routine enquiry in mainstream mental health services. Reference Brooker, Tocque, Brown and Kennedy12 Despite the introduction of a national training programme, 2008/9, it was clear that routine enquiry was far from comprehensive. Indeed, it was estimated that of 335 727 on the CPA England, just 17% had been assessed for their experience of sexual abuse/violence. There is no reason to expect the figure to be higher in prisons and in fact, given the challenges apparent in the prison environment, it is likely the figure is considerably less than 17%. However, the resources for prison mental healthcare have never been better and case-loads are now manageable. Prison mental health staff should therefore be enquiring about a prisoner's history of victimisation and they should be trained to do so. Reference Read, Hammersley and Rudegeair13
Given this apparent service gap, it is time to ask, in the light of the new National Institute for Health and Care Excellence guidelines, 14 what interventions are prisoners receiving from prison mental health services and what are the outcomes?






eLetters
No eLetters have been published for this article.