Psychiatric battle casualties are a significant feature of modern warfare. However, the exact magnitude of the problem, and its relationship to the experience of combat, has been a cause for debate. In 1900 the idea that soldiers could suffer psychological damage in action was barely acknowledged and yet 40 years later psychiatrists were routinely deployed to fighting units. This paper is based on original sources from the Royal Army Medical Corps (RAMC) collection and the archives of the Wellcome Institute for the History of Medicine, supplemented by contemporary literature. It is primarily concerned with combat stress and acute psychiatric casualties of battle treated in the field rather than at base hospitals. We will not consider the relatively recent phenomenon of delayed psychiatric disorder, exemplified by the modern condition of post-traumatic stress disorder (PTSD).
Earlier wars
Few reliable casualty statistics are available for wars fought in the late 19th century and, given the inconsistent nature of diagnosis, at best these figures remain estimates. Although the concept of combat stress did not then exist, it was recognised that soldiers could become debilitated by the accumulated effects of active service (Reference Jones and WesselyJones & Wessely, 1999). Having treated the sick and wounded of the Boer War, Anthony Bowlby (1855-1929) concluded that “the excitement of battle often following prolonged mental strain and bodily fatigue” could produce a form of neurasthenia characterised by “the appearance of functional nervous symptoms” (Reference Bowlby, Tooth and WallaceBowlby et al, 1901: 129). He detected no clinical difference between cases of military and civilian neurasthenia, adding that
Among the symptoms we find prominently in the foreground pain, in the form of headache, generally posterior, pains in the neck, pains in the back and limbs, so that these cases are generally sent back as rheumatism; general feebleness of the muscular system amounting to paralysis more or less pronounced (Reference Bowlby, Tooth and WallaceBowlby et al, 1901: 129).
Excluding the 14 pensions awarded for psychosis and 22 for depression, our survey of 6200 cases of soldiers medically discharged after the Boer War found only 11 examples where a psychological cause was diagnosed. These comprised six cases of nervous debility, three of neurasthenia, one of hysteria and one of nervous shock (Anon., various years). The last was Private John Lyons of the Royal West Surrey Regiment, who had been concussed but not wounded by a shell explosion at the battle of Colenso in December 1899. Returning to duty after a hospital admission, he continued to experience fatigue and weakness with a functional paralysis of his right arm and leg, tremor, dizziness and free-floating anxiety. Lyons was discharged from the Army in November 1900 with a war pension (Anon., various years; PIN71/3959). In time, his paresis remitted and he died in 1950 at the age of 82. This was, perhaps, one of earliest documented cases of what would later be called shell-shock. It appears, therefore, that unambiguous cases of combat fatigue were rarely identified in the Victorian period and that soldiers traumatised by the stress of battle appear to have somatised their fears often in the form of disordered action of the heart (DAH) or psychogenic rheumatism.
First World War
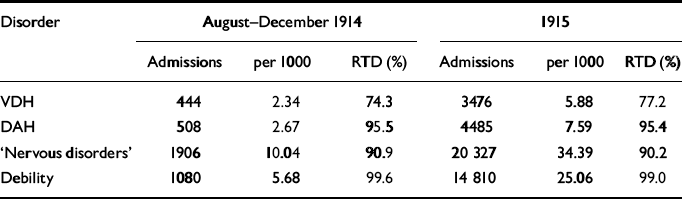
Military psychiatry was in its infancy during the First World War, as physicians gradually appreciated that shell-shock, certain forms of trench fever and DAH were functional disorders related to the stress of combat, whether actual or envisaged. The collection of data about soldiers suffering from psychological breakdown was haphazard and inconsistent. The statistical appendix to the official medical history of the war, based on hospital admission cards, provides an approximate guide to the incidence of psychiatric casualties (Table 1). The analysis was only performed for the first 2 years of the hostilities and showed that psychological disorders accounted for 2.5% and 3.8% of all admissions in 1914 and 1915 respectively (Reference Mitchell and SmithMitchell & Smith, 1931: 115). These percentages greatly understate the true figures as they do not include functional somatic cases.
Table 1 British psychiatric casualties and return to duty (RTD) rates in France and Belgium (1914-1915)
| Disorder | August-December 1914 | 1915 | ||||
|---|---|---|---|---|---|---|
| Admissions | per 1000 | RTD (%) | Admissions | per 1000 | RTD (%) | |
| VDH | 444 | 2.34 | 74.3 | 3476 | 5.88 | 77.2 |
| DAH | 508 | 2.67 | 95.5 | 4485 | 7.59 | 95.4 |
| ‘Nervous disorders’ | 1906 | 10.04 | 90.9 | 20 327 | 34.39 | 90.2 |
| Debility | 1080 | 5.68 | 99.6 | 14 810 | 25.06 | 99.0 |
Treatment of combat fatigue
At first, cases of combat fatigue were invalided to hospitals in the UK. In July 1916, Lieutenant Colonel Charles Myers, consulting psychologist to the British Expeditionary Force, persuaded the medical authorities to treat them at base hospitals in France. However, the proximity to England and the expectation of evacuation home tended to reinforce symptoms. At the end of the year, Myers set up four special centres at the rear of ‘Army Areas’ for the reception of shell-shock cases, with the result that the return to duty rate rose from 50% to 90% (Reference MyersMyers, 1940: 92). Captain William Brown, working at a casualty clearing station in December 1916 recorded that of 200 psychiatric admissions, 34% were transferred to base hospitals and 66% returned to front-line units after an average of 7 days' treatment (Reference SalmonSalmon, 1917: 521). Lieutenant Colonel Gordon Holmes, consulting neurologist, confirmed these figures, writing that 80% of men returned to duty within 2-3 weeks, whereas if sent to a base hospital in France the proportion fell to 30-40% and as low as 5% if invalided to the UK (Reference Holmes1939: 12). However, neither Myers nor Holmes recorded what proportion returned to combat and of these how many relapsed. In the year ending 30 June 1917, the military psychiatric hospital for other ranks at Maghull succeeded in returning only 20.9% of its patients to duty and, in the opinion of R. G. Rows, its senior medical officer, few were fit for combat (Reference SalmonSalmon, 1917: 525). Similarly, Thomas Lewis recorded that of 249 cases of functional heart disease discharged from specialist cardiac hospitals in Hampstead and Colchester between May and October 1917, only 23 (9.2%) went back to fighting units overseas (Reference Lewis c. 1919: 1). The rates reported by physicians, therefore, were noticeably lower than those presented in the official history (Table 1).
The French military pioneered specialist neuropsychiatric centres situated close to the front line for the rapid treatment of combat stress. André Léri, working in the centre attached to the French Second Army, reported that 91% of admissions between July and October 1916 were returned to the fighting line (Reference SalmonSalmon, 1917: 521). A review by G. Roussy and J. Boisseau in La Presse Médicale for 1916 concluded that these centres avoided:
“… sojourns (more dangerous the more they are prolonged) in the hospitals at the rear where these patients are generally lost. It allows of the treatment of other nervous and mental cases that are quickly curable and the direct evacuation to the special centres in the interior of those more seriously affected” (quoted by Reference SalmonSalmon, 1917: 521).
Drawing on the French example and against considerable opposition, Myers opened an Advanced Sorting Centre close to the front early in 1917 where soldiers could be rapidly treated. Captain F. Dillon was apparently the officer responsible for implementing “the method of sedation, rest, occupation and return to duty carried out at a hospital centre close to the lines of trenches occupied by the Third Army” (Reference PhillipsPhillips, 1944: 8). However, Sir Arthur Sloggett, Director-General of the Medical Services of the British Forces in the Field, soon ordered the unit's closure, arguing that “we can't be encumbered with lunatics in Army Areas!” (Reference MyersMyers, 1940: 90).
Salmon and US forces
Through the work of Major Thomas Salmon, the US Army had the opportunity to study the incidence and treatment of psychiatric disorders before it entered the War. Salmon recommended the setting up of ‘Advanced Section Lines of Communication’ with 30-bed wards for the emergency treatment of mental and nervous cases, concluding that:
“much can be done in dealing with [shell-shock] cases if they can be treated within a few hours after the onset of severe nervous symptoms. There is data to show that even by the time these cases are received at base hospitals additions have been made to the initial neurological disability and a colouring of invalidism given which frequently influences the prospects of recovery” (Reference SalmonSalmon, 1917: 539-540).
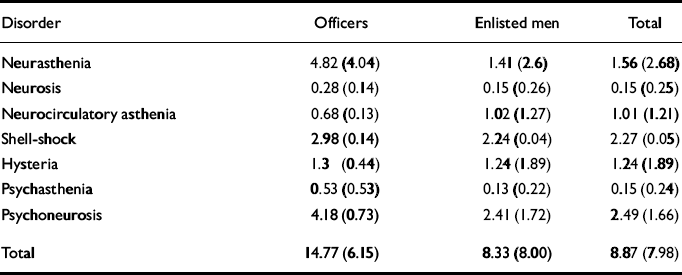
Salmon also embarked on a major study of psychiatric disorders in the US Army. The incidence in 1918, he reported, was about twice that of the adult male population of the US and “no higher than in the armies of our Allies” (Reference SalmonSalmon, 1918: 1). Further work demonstrated that combat or the threat of combat doubled the incidence of psychological disorders in officers but had little effect for enlisted men (Table 2). However, the latter showed an increased incidence of somatoform disorders such as neurocirculatory asthenia. For several diagnoses deployment to the Continent appeared to have little effect, although shell-shock was markedly greater for officers and men, as was psychoneurosis. The figures supported Mott's hypothesis that officers were more likely to exhibit the symptoms of neurasthenia, although his associated claim that other ranks had more conversion disorders was not confirmed (Reference MottMott, 1919: 131). Yet this study did not represent a straight comparison between men exposed to war and those deployed in home defence, as the European cohort includes troops with 13 months of occupation and peace-keeping duties.
Table 2 Psychiatric disorders for the US Army in Europe between 1 April 1917 and 31 December 1919 (rates per 1000 per annum)
| Disorder | Officers | Enlisted men | Total |
|---|---|---|---|
| Neurasthenia | 4.82 (4.04) | 1.41 (2.6) | 1.56 (2.68) |
| Neurosis | 0.28 (0.14) | 0.15 (0.26) | 0.15 (0.25) |
| Neurocirculatory asthenia | 0.68 (0.13) | 1.02 (1.27) | 1.01 (1.21) |
| Shell-shock | 2.98 (0.14) | 2.24 (0.04) | 2.27 (0.05) |
| Hysteria | 1.3 (0.44) | 1.24 (1.89) | 1.24 (1.89) |
| Psychasthenia | 0.53 (0.53) | 0.13 (0.22) | 0.15 (0.24) |
| Psychoneurosis | 4.18 (0.73) | 2.41 (1.72) | 2.49 (1.66) |
| Total | 14.77 (6.15) | 8.33 (8.00) | 8.87 (7.98) |
Although it had now become clear that psychiatric casualties were a major feature of modern warfare, military authorities continued to underestimate their incidence and a range of conflicting conclusions were drawn about their nature. Psychologically minded physicians, like Myers, believed that they were inevitable and that the solution lay in rapid and effective treatment, while many senior officers argued that with effective training and good leadership they were avoidable. Lord Gort, giving evidence to the Southborough Committee in 1921, argued that shell-shock would have been practically non-existent “ in the face of strong morale and esprit de corps” (Southborough, 1922: 50).
Second World War
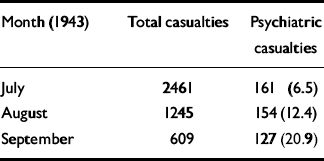
A retrospective War Office report estimated that between 5% and 30% of all sick and wounded evacuated from battle areas in all theatres during the Second World War were psychiatric casualties and that this figure depended largely on the type of warfare fought. In the retreat to Dunkirk, it was calculated that combat stress accounted for 10% of admissions to regimental aid posts (Reference PhillipsPhillips, 1944: 6). In view of the large numbers of servicemen admitted to psychiatric wards once they had returned to the UK, this figure may understate the true incidence of psychological disorders (Reference Sargent and SlaterSargent & Slater, 1940). It was argued that the fluid campaign in the Western Desert in 1940-1941 produced low rates (sometimes only 2%), while fighting in north-west Europe, akin to trench warfare, led to far higher figures (War Office, 1951: 1). In fact, detailed reports from the Western Desert reveal that the percentages were considerably higher than claimed (Table 3). Between July and September 1943 psychiatric casualties and total battle casualties were correlated at a significant level (Spearman's ρ=1.0, P=<0.001). In part, these variations can be explained by the different phases of battle, as Major Craigie had observed that the incidence of psychiatric casualties in the desert during 1942 depended “to some extent on the nature of the action itself — for instance, it is likely to be higher during unsuccessful, purely defensive or unduly prolonged actions” (Reference CraigieCraigie, n.d.: 1).
Table 3 UK forces in the Western Desert: casualty rates
| Month (1943) | Total casualties | Psychiatric casualties |
|---|---|---|
| July | 2461 | 161 (6.5) |
| August | 1245 | 154 (12.4) |
| September | 609 | 127 (20.9) |
I Canadian Division in Italy
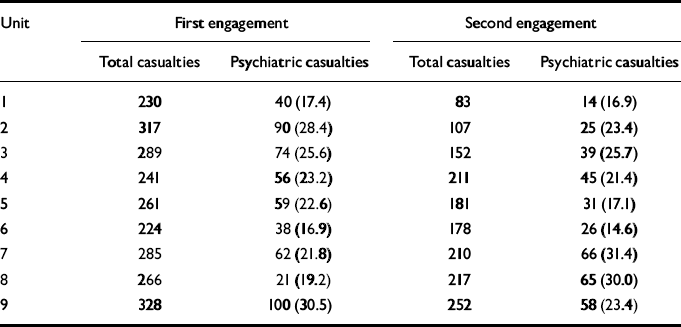
A comparison between the various units that made up 1 Canadian Division fighting in Italy during 1944 showed that great differences could arise not only between engagements but also between battalions (Reference DoyleDoyle, n.d.: 8). In the first battle, for example, Unit 1, which was in action for only 1 of the 10 days' fighting, recorded low psychiatric casualties (Table 4). Unit 6, however, which saw more intense combat, had an even lower figure, attributed to the quality and training of its troops. Having had high psychiatric casualties in the first battle, Unit 7 was thought to have improved its fighting qualities by the time of the second engagement, when it had one of the lowest percentages. Hence, psychiatric casualties are not simply an indicator of the severity of combat but are also a reflection of the experience and preparedness of soldiers. Interestingly, the division had been instructed before the second action to adopt a severe disciplinary attitude to psychiatric casualties in the belief that they were due to laxness and weakness. Yet the overall percentages for the two battles were similar (22.1% and 23.2%). Psychiatric admissions were found to be closely correlated with total battle casualties for both engagements (Spearman's ρ=0.8, P=0.005 and 0.8, P=0.005, respectively). During this campaign, the German 6-inch mortar and the six-barrelled mortar were feared beyond their actual capacity to inflict harm. “Officers and mortar specialists”, recorded an Eighth Army morale report in 1944, “ appear to be generally of the opinion that their destructive effect is not sufficient to justify their introduction to the British Army. The morale effect of these weapons, however, in particular of the Nebelwerfer is so great that the introduction of a similar weapon might well be considered on this ground alone” (Anon., 1944: 1-2).
Table 4 Canadian Division in Italy: battle casualties
| Unit | First engagement | Second engagement | ||
|---|---|---|---|---|
| Total casualties | Psychiatric casualties | Total casualties | Psychiatric casualties | |
| 1 | 230 | 40 (17.4) | 83 | 14 (16.9) |
| 2 | 317 | 90 (28.4) | 107 | 25 (23.4) |
| 3 | 289 | 74 (25.6) | 152 | 39 (25.7) |
| 4 | 241 | 56 (23.2) | 211 | 45 (21.4) |
| 5 | 261 | 59 (22.6) | 181 | 31 (17.1) |
| 6 | 224 | 38 (16.9) | 178 | 26 (14.6) |
| 7 | 285 | 62 (21.8) | 210 | 66 (31.4) |
| 8 | 266 | 21 (19.2) | 217 | 65 (30.0) |
| 9 | 328 | 100 (30.5) | 252 | 58 (23.4) |
The Normandy offensive
In the Normandy campaign, the 21st Army Group encountered such intense German resistance during July 1944 that it tested the endurance of even seasoned troops. Planners had anticipated psychiatric casualties of the order of 10-30% and, although the recorded rate fell within this range, it caused “ considerable anxiety amongst certain officers, some of whom believed that the psychiatric problem would be negligible” (Reference MainMain, 1944: 2). During the first 16 days of the campaign, psychiatric casualties in 8 Corps varied considerably. The overall rate was 14.6%, while the three divisions recorded rates of 21%, 11.6% and 14.7% (Reference PhillipsPhillips, 1944: 12-13). The second battle, a fast-moving armoured thrust lasting only 5 days, led to a greatly reduced the Corps' rate of 11.6%. The third battle, in which British troops encountered severe opposition, saw an increase to 18%, although great variations occurred between units. These high percentages were also a function of widespread battle fatigue in soliders who had already fought in North Africa, Sicily and Italy, and, as a War Office report concluded, “a number of men who broke down were experienced veterans with excellent past records” (War Office, 1951: 7). Although some planners believed that the battle exhaustion crisis had passed, heavy fighting involving the 1 Canadian Army north of Falaise during August produced even higher rates of psychiatric casualties (Reference Copp, Addison and CalderCopp, 1997: 150). It became clear that the only effective way to reduce battle exhaustion levels was to lower the intensity and duration of combat.
Return to duty rates
The main justification for deploying army psychiatrists to forward areas was to facilitate the treatment of battle-fatigued troops so that they could be returned to their units as quickly as possible. Although both Myers and Holmes suggested that over 80% of soldiers treated in specialist centres in the First World War returned to duty, they did not record how many went to fighting units. The experience of the Second World War suggests that most servicemen returned to non-combatant activity, although the percentage varied considerably according to the intensity of battle and provision of psychiatric services (Table 5). Major Doyle of 1 Canadian Division concluded that “less than 20% of psychiatric casualties can be returned to full combat duty after treatment” (Reference DoyleDoyle, n.d.: 11). These figures were confirmed by Brigadier Sandiford, who visited Corps' psychiatric teams in Italy after the battle of Casino. Between May and November 1944, the return to duty rate fluctuated between 32% and 16%, while the specialist base unit at Assisi sent only 19% of men back in the same medical category (Reference SandifordSandiford, 1944: 45-46).
Table 5 Return to duty rates

| Unit | Campaign | Returned to combat |
|---|---|---|
| 8 Army | Italy (1944) | 25-30% |
| 21 Army | Normandy (July 1944) | 50% with 10% relapsing |
| 8 Corps | Normandy (July 1944) | 49% with 10% relapsing |
| 1 Canadian Division | Italy (July 1943-April 1945) | 22% reduced to 15% after relapses |
US forces
Although individual psychiatrists collected statistics as campaigns were fought and these guided decisions about treatment, systematic studies were not undertaken until the postwar period. A retrospective study by Beebe & DeBakey (Reference Beebe and DeBakey1952) analysed casualties for units engaged in combat, comparing the wounded with all other admissions. They calculated correlation coefficients for two theatres in 1944, the south-west Pacific and the Mediterranean, and for the 34 and 45 Divisions in October—November 1943. Admissions to neuropsychiatric units were closely correlated with the total wounded, with the exception of the south-west Pacific (Reference Beebe and DeBakeyBeebe & DeBakey, 1952: 28). Incomplete data and a failure to recognise the nature and importance of psychiatric casualties were proposed as reasons for the anomaly. Three of the four examples showed that battle intensity was the crucial variable. A further study by Beebe & Apple (Reference Beebe and Apple1958) involved a representative sample of 2419 soldiers drawn from 150 companies that fought in the Mediterranean and European theatres. Unit losses and the arrival of replacements were recorded during periods of combat and showed a correlation between the number of killed and wounded and the incidence of combat stress reactions. The average breaking point for a rifleman in the Mediterranean theatre of operations, for example, was 88 days of company combat — days in which the unit sustained at least one casualty (Reference Beebe and AppleBeebe & Apple, 1958). Blood & Gauker (Reference Blood and Gauker1993) examined the relationship between the wounded in action rate (WIA) and disease and non-battle injury rate (DNBI) for the 1 and 6 Divisions of the US Marine Corps during their assault on Okinawa between April and June 1945. The two rates were significantly correlated. As the fighting became more intense, so there was a concomitant rise in the DNBI rate (Reference Blood and GaukerBlood & Gauker, 1993: 342). They found a similar correlation between the two measures in a study of Marine units in Korea from February to June 1951.
Using the data collected by Beebe & Apple, Noy (Reference Noy1987) hypothesised that the intensity of battle accounted not only for the rate of psychiatric casualties but also for their general presentation. Comparing different types of departure from the battle-field, he found that psychiatric cases had experienced greater combat intensity than medical (excluding wounded in action) and disciplinary cases (Reference NoyNoy, 1987: 604). Most psychiatric casualties were of the dramatic, but transient, combat reaction type, while the medical and disciplinary cases appeared to be a response to sporadic stress.
Korean War
Total psychiatric casualties were recorded as 37 per 1000 among US servicemen (Reference DeanDean, 1997: 40). However, the Korean War can be divided into two distinct phases with markedly different rates of psychiatric casualties. During the first year, characterised by movement, an exceptionally cold winter saw battle injuries and wounds to US forces rise to 460 per 1000 (Reference Jones, Jones, Sparacino and WilcoxJones, 1995b : 41). From mid-1951, it became a static war of attrition, although troops were better equipped and trained for the harsh winters. Battle injuries and wounds to US forces fell to 170 per 1000 in 1951 and 57 per 1000 in 1952. No statistics survive for UK units in the early phase of the war but by December 1952 the proportion of battle exhaustion to battle casualty cases for 1 Commonwealth Division was 21 per 1000 and from May 1952 to the end of the war it fell to 18 per 1000 (Reference Jones and PalmerJones & Palmer, 2000: 258). Battle exhaustion cases were found to be closely correlated with battle casualties (Spearman's ρ=0.8, P=0.001).
Recent wars
The Vietnam War is often taken as an example of low-intensity combat and US troops suffered relatively minor rates of battle injuries and wounds (from 62 per 1000 in 1965 to 120 per 1000 in 1968). Psychiatric casualties were low: 12 per 1000 (Reference DeanDean, 1997: 40). The prolonged campaign also gave rise to a new term, post-Vietnam syndrome, which referred to servicemen suffering from chronic psychiatric symptoms or to those who appeared well when demobilised but later developed an enduring psychological disorder. The diagnosis of PTSD was developed as a consequence of, or some might say as a stimulus to, these observations, but it lies outside the scope of this paper.
The Yom Kippur War in 1973, by contrast, was a high-intensity campaign. At first, Israeli combat stress rates were reported as only 10% of total casualties but later were revised upwards to between 30% and 50% (Reference Jones, Jones, Sparacino and WilcoxJones, 1995a : 21). Initial reports had failed to include servicemen who had been treated at forward medical units and returned to duty, men with light wounds who also suffered from psychological stress, and psychiatric casualties that arose 2 days after the cease-fire. Figures from this war showed that the peak incidence of combat fatigue was in the first few days, when physical casualties were at their greatest (Reference AbrahamAbraham, 1982: 21-22). The Lebanon War of 1982 had a short period of high-intensity combat followed by prolonged low-intensity fighting, when snipers and booby traps accounted for many casualties. Although the war generated a moderate overall rate of 23% for psychiatric casualties, 90% of these fell within a 3-month period (Reference NoyNoy, 1987: 602).
The Falklands War of 1982 lasted only 74 days, including a 25-day campaign from the landing at San Carlos Water to the recapture of Stanley. British troops lost 237 killed and 777 wounded, with 446 requiring significant hospital treatment. Psychiatric casualties were reported as 2% of all wounded, with 16 declared cases evacuated from the hospital ship Uganda (Reference PricePrice, 1984: 109). Further research by Abraham suggested that somatic presentations, such as functional deafness, concealed the true rate, which was about 8% — a figure well below that of many of the battles fought during the Second World War (Reference AbrahamAbraham, 1982: 113). Explanations have included the fact that British troops were considered the élite of the army, with high morale. In addition, the 2-week transatlantic voyage gave them time to prepare for the conflict ahead, while they were also able to practise amphibious assault landings on St George's Island, which remained under British control (Reference O'Connell, Pichot, Berner and WolfO'Connell, 1985). For the Argentine forces, psychiatric casualties also appear to have been surprisingly low and were reported as 4-5% (Reference Jones, Jones, Sparacino and WilcoxJones, 1995a : 23). It has been suggested that the impossibility of evacuating casualties from the island helped to keep these figures down, in the same way that a firm regimental medical officer in the First World War could discourage cases of shell-shock (Reference Jones, Jones, Sparacino and WilcoxJones, 1995a : 23).
DISCUSSION
The relationship
Today there is a consensus that a constant relationship exists between the incidence of the total killed and wounded and the number of psychiatric casualties. Several factors, however, act as mediators or effect modifiers between these two variables: the physical nature of the fighting; the state of morale and preparedness of the troops; and the quality of leadership. These may reduce the size of the association but not the association itself.
Cultural factors
Military and health beliefs of the society from which the soldiers were drawn also need to be considered. In particular, ideas about acceptable levels of casualties and the general level of psychological understanding are pertinent. In the decade before the Boer War, when life expectancy for UK males was only 44 years and knowledge about combat syndromes was embryonic, observed psychiatric casualty rates were low, almost non-existent. But this hides, as we have shown, psychiatric morbidity in the shape of DAH, rheumatism and cases of sunstroke. The First World War saw a greater appreciation of the stress of warfare, such that doctors became increasingly alert to psychiatric symptoms and soldiers were better able to interpret their own responses to traumatic situations. Such understanding remained at an early stage and judgements continued to be clouded by Edwardian notions of courage and duty.
By the Second World War, suggestions that psychiatric breakdown was due to a failure of personal morality or social degeneration had largely been abandoned. In their place, psychiatrists and military strategists sought measurable causes such as quality of training. In addition, Western society was less tolerant of the high casualty levels that had been incurred between 1914 and 1918, and offensives were planned so as to minimise losses. Nevertheless, some battles saw high rates of killed and wounded, notably the early stages of the Normandy campaign and the Monte Casino offensive in Italy, where concentrated shelling is said to have raised psychiatric casualties to 54% in the US 2 Armoured Division (Reference Holmes, Addison and CalderHolmes, 1997: 218).
Trauma
The relationship between physical and psychological trauma is a complex one. Advances in medical science have progressively reduced the proportion of troops who die from their injuries, the rate falling from 20% in the Crimean War to 6.1% in the First World War, 4.5% in the Second World War and 2.5% in Korea (Reference Beebe and DeBakeyBeebe & DeBakey, 1952: 77). Improved survival rates may have increased the number of potential psychiatric casualties and allowed the focus of attention to move towards psychological issues. Alternatively, wounds could serve as a protector against post-combat syndromes. Physicians during the First World War commented that soldiers injured in battle were less likely to suffer from shell shock and that many men with this disorder had not been wounded.
Psychiatric casualties may continue to be underreported. As the causes of combat fatigue have become better understood, it has been suggested that commanders may be reluctant to refer cases for treatment as they will be considered a sign of poor morale or indifferent leadership. Today, when adults expect to survive most diseases and when great emphasis is placed on the elimination of risk, Western society has little tolerance of death and wounding. It appears that this fundamental cultural change is reflected in the incidence of psychological disorders both during combat and as a delayed effect.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Psychiatric battle casualties are an enduring and significant feature of modern warfare and their incidence is largely but not solely determined by the intensity of battle.
-
▪ If treated rapidly by psychological means, most servicemen can be returned to duty, although fewer than half go back to combat units.
-
▪ There has been a tendency to misdiagnose soldiers suffering from functional somatic disorders, thereby understating the true incidence of psychiatric battle casualties.
LIMITATIONS
-
▪ Although data appear to have been collected accurately from the Second World War onwards, there are few standardised measures and studies often rely on the judgement of clinicians.
-
▪ The statistics for psychiatric disorders in the First World War and the calculations of return to duty rates have been shown to be inaccurate.
-
▪ Among military clinicians there has not always been agreement about the nature of psychiatric casualties, as they often present with both psychological and physical symptoms.










eLetters
No eLetters have been published for this article.