Suicide is the cause of almost half of all violent deaths and results in almost a million fatalities every year. 1 A previous suicide attempt is one of the strongest predictors of future completed suicide Reference Beck and Steer2 or subsequent attempt Reference Leon, Friedman, Sweeney, Brown and Mann3 as well as being an indicator of extreme psychological distress. Reference Kessler, Berglund, Borges, Nock and Wang4 Epidemiological data suggest 12-month prevalence rates for suicide attempts of 0.4% Reference Kessler, Borges and Walters5 to 0.6%, Reference Kessler, Berglund, Borges, Nock and Wang4 but it has been suggested that there may be 8–25 suicide attempts for every death from suicide. Reference Moscicki6 Most individuals who complete or attempt suicide have a diagnosable psychiatric illness, with depressive disorders most often diagnosed. Reference Moscicki, O'Carroll, Rae, Locke, Roy and Regier7,Reference Harris and Barraclough8 However, the observations that a proportion of people who engage in suicidal acts have no psychiatric illness and that most individuals with a psychiatric disorder do not attempt suicide necessitate an increased understanding of physical health and psychosocial factors that may contribute. Previous research studies on suicide attempts and suicidal acts have been limited by heavy reliance on clinical samples, Reference Schmidtke, Bille-Brahe, DeLeo, Kerkh of, Bjerke, Crepet, Haring, Hawton, Lonnqvist, Michel, Pommereau, Querejeta, Phillipe, Salander-Renberg, Temesvary, Wasserman, Fricke, Weinacker and Sampio-Feria9 the relevance of which to the larger population of people at risk of suicide is questionable. Most people who complete suicide have neither made a previous attempt nor received mental healthcare. Reference Isometsa and Lonnqvist10 Only a few population-based studies have reported suicide attempt data, Reference Moscicki, O'Carroll, Rae, Locke, Roy and Regier7,Reference Paykel, Myers, Lindenthal and Tanner11 and these were limited by the small numbers of people attempting suicide Reference Paykel, Myers, Lindenthal and Tanner11 and the lack of sufficient information about these individuals to yield new insights. Reference Moscicki, O'Carroll, Rae, Locke, Roy and Regier7,Reference Paykel, Myers, Lindenthal and Tanner11 In addition, both studies were conducted before the introduction and exponential rise in use of newer antidepressant medications, raising questions about the current relevance of their findings.
This study seeks to extend our knowledge about suicidal acts in the general population, using data from another population-based survey which sampled the Canadian population aged 15 years and over. We refer to ‘suicidal acts’, as no definition of suicide attempt was provided for respondents and no measure of suicidal intent was available to include in analyses. Our aims were to describe the characteristics of individuals who undertook a suicidal act in the 12 months preceding interview and to examine variables that have been associated with risk for suicide in previous research studies for their association with suicidal acts in this general population sample.
Method
Data source
The data for this study were obtained from the Canadian Community Health Survey 1.2: Mental Health and Well Being (CCHS 1.2), a large epidemiological national survey of community-dwelling individuals aged 15 years and older conducted by Statistics Canada in 2002. Residents of the territories, Indian reserves, institutions, certain remote areas and full-time members of the armed forces were not included. The survey employed a multistage stratified cluster design to sample dwellings within this area frame. One person aged 15 years or older was randomly selected from each of the sampled households. Further details of the survey design and the questionnaires used are available elsewhere. Reference Gravel and Béland12,13
Sample
The responding sample consisted of 36 984 community-dwelling individuals aged 15 years or older, with a response rate of 77%; this represents a weighted population of 23 662 430. In this study respondents were divided into two groups: those who did and those who did not engage in a suicidal act in the 12 months preceding the interview. A suicidal act was held to have occurred if the individual endorsed the statement, ‘In the last 12 months you attempted suicide or tried to take your own life’.
Variables
Demographic, social and clinical variables that had previously been associated with risk of suicide were included in the analyses. Reference Hawton and van Heeringen14
Demographic characteristics
Marital status was classified as married, cohabiting, single, separated, divorced, or widowed. Ethnicity was selected by respondents from pre-defined categories used by Statistics Canada; for analysis purposes, because of small cell sizes, this variable was dichotomised into ‘White’ v. ‘other’. Education was categorised as less than secondary, secondary graduate, other post-secondary, or post-secondary school graduate. Respondents characterised themselves as employed (defined as having worked at a job or business in the preceding 12 months), unemployed (including those unable to work owing to illness or disability, and full-time homemakers) or retired; as living in either an urban or a rural area; and whether they were an immigrant to Canada (yes/no). Income adequacy was based on the number of people in the household and the total household income from all sources, and was divided into five groups ranging from low to high. Definitions of income adequacy (in Canadian dollars) were as follows:
-
(a) low: one to four persons earning less than $10 000, or five or more persons earning less than $15 000;
-
(b) lower middle: one or two persons earning $10 000–14 999, three or four persons earning $10 000–19 999, or five or more persons earning $15 000–29 999;
-
(c) middle: one or two persons earning $15 000–29 999, three or four persons earning $20 000–39 999, or five or more persons earning $30 000–59 999;
-
(d) upper middle: one or two persons earning $30 000–59 999, three or four persons earning $40 000–79 999, or five or more persons earning $60 000–79 999;
-
(e) high: one or two persons earning in excess of $60 000, or three or more persons earning in excess of $80 000.
Psychiatric diagnoses
Psychiatric symptoms were assessed using the World Health Organization World Mental Health 2000 version of the Composite International Diagnostic Interview (WMH–CIDI), Reference Kessler, Abelson, Demler, Escobar, Gibbon, Guyer, Howes, Jin, Vega, Walters, Wang, Zaslavsky and Zheng15,Reference Kessler and Ustun16 a fully structured and validated interview that generates DSM–IV diagnoses. 17 All interviews were conducted by trained interviewers using a computer-assisted application. Most interviews were conducted in person (86%), the remainder by telephone. Data were available for analyses of lifetime and 12-month diagnoses of major depressive episode, substance dependence in the past 12 months (alcohol and/or drug) and select anxiety disorders (lifetime panic disorder and panic attacks in the past 12 months, and social phobia – lifetime and 12-month).
Health status
Interviewers enquired about the presence of chronic medical conditions including arthritis or rheumatism, back problems (excluding fibromyalgia or arthritis), chronic bronchitis, emphysema or chronic pulmonary disease, diabetes, thyroid disease, heart disease, cancer, stomach or intestinal ulcers, bowel disorder or Crohn's disease, epilepsy and stroke. Each condition was required to have been present for at least 6 months and diagnosed by a health professional (Table 1). For the purposes of analysis the variable was dichotomised as the presence or absence of at least one chronic condition.
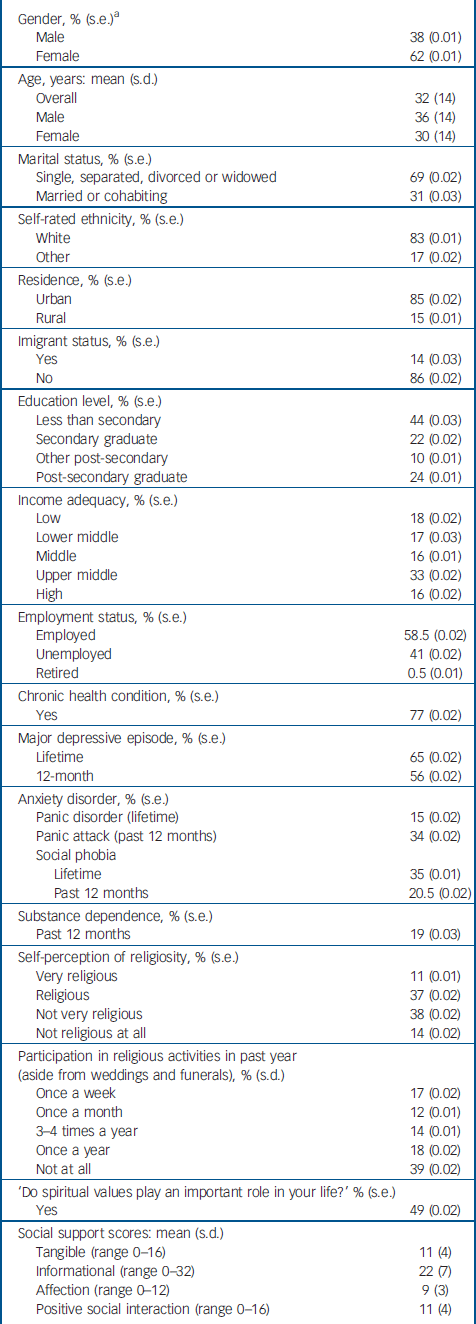
Table 1 Socio-demographic and clinical characteristics of those reporting a suicidal act occurring in the previous 12 months (unweighted n=222, weighted n=130 143)
| Gender, % (s.e.) a | |
| Male | 38 (0.01) |
| Female | 62 (0.01) |
| Age, years: mean (s.d.) | |
| Overall | 32 (14) |
| Male | 36 (14) |
| Female | 30 (14) |
| Marital status, % (s.e.) | |
| Single, separated, divorced or widowed | 69 (0.02) |
| Married or cohabiting | 31 (0.03) |
| Self-rated ethnicity, % (s.e.) | |
| White | 83 (0.01) |
| Other | 17 (0.02) |
| Residence, % (s.e.) | |
| Urban | 85 (0.02) |
| Rural | 15 (0.01) |
| Imigrant status, % (s.e.) | |
| Yes | 14 (0.03) |
| No | 86 (0.02) |
| Education level, % (s.e.) | |
| Less than secondary | 44 (0.03) |
| Secondary graduate | 22 (0.02) |
| Other post-secondary | 10 (0.01) |
| Post-secondary graduate | 24 (0.01) |
| Income adequacy, % (s.e.) | |
| Low | 18 (0.02) |
| Lower middle | 17 (0.03) |
| Middle | 16 (0.01) |
| Upper middle | 33 (0.02) |
| High | 16 (0.02) |
| Employment status, % (s.e.) | |
| Employed | 58.5 (0.02) |
| Unemployed | 41 (0.02) |
| Retired | 0.5 (0.01) |
| Chronic health condition, % (s.e.) | |
| Yes | 77 (0.02) |
| Major depressive episode, % (s.e.) | |
| Lifetime | 65 (0.02) |
| 12-month | 56 (0.02) |
| Anxiety disorder, % (s.e.) | |
| Panic disorder (lifetime) | 15 (0.02) |
| Panic attack (past 12 months) | 34 (0.02) |
| Social phobia | |
| Lifetime | 35 (0.01) |
| Past 12 months | 20.5 (0.02) |
| Substance dependence, % (s.e.) | |
| Past 12 months | 19 (0.03) |
| Self-perception of religiosity, % (s.e.) | |
| Very religious | 11 (0.01) |
| Religious | 37 (0.02) |
| Not very religious | 38 (0.02) |
| Not religious at all | 14 (0.02) |
| Participation in religious activities in past year (aside from weddings and funerals), % (s.d.) | |
| Once a week | 17 (0.02) |
| Once a month | 12 (0.01) |
| 3–4 times a year | 14 (0.01) |
| Once a year | 18 (0.02) |
| Not at all | 39 (0.02) |
| ‘Do spiritual values play an important role in your life?’ % (s.e.) | |
| Yes | 49 (0.02) |
| Social support scores: mean (s.d.) | |
| Tangible (range 0–16) | 11 (4) |
| Informational (range 0–32) | 22 (7) |
| Affection (range 0–12) | 9 (3) |
| Positive social interaction (range 0–16) | 11 (4) |
a. All percentages are weighted
Respondents were asked, ‘During the past 12 months have you seen, or talked on the telephone, to a professional about committing suicide or taking your own life?’ Respondents were then asked to name all of the professionals they had spoken to from the following list: psychiatrist, family doctor, psychologist, nurse, social worker or counsellor, religious or spiritual advisor such as a priest, chaplain or rabbi, teacher or guidance counsellor, or other.
Social support
Respondents were asked to rate four categories of social support on a four-point scale ranging from ‘none of the time’ to ‘all of the time’. These categories were informational support (the offering of advice, information, guidance or feedback); tangible support (the provision of material aid or behavioural assistance); positive social interaction (the availability of other people to share enjoyable activities, relax with); and affection (involving expressions of love and affection). A higher score reflects higher levels of social support.
Religiosity
Respondents were asked to indicate their participation in religious activities, aside from weddings and funerals, in the preceding year. Five responses were given ranging from ‘not at all’ to ‘once a week’. Respondents were also asked to agree or disagree with the statement, ‘Spiritual values play an important role in my life’.
Statistical analysis
To account for survey design effects, the variance used in the calculation of prevalence estimates, coefficients of variation (standard error of the estimate) and confidence limits were estimated with the bootstrap technique. Weighted cross-tabulations were used to estimate the number and proportion of people who engaged in suicidal acts in the past 12 months. All reported sample sizes and percentages are weighted. Multivariate logistic regression was used for analysis; the binary outcome variable was a suicidal act in the preceding 12 months (yes/no). We estimated the association of each demographic and psychosocial variable with the outcome and all determinants for which the association was significant at the P<0.01 level were included in a preliminary multivariate model. The final multivariate logistic regression model was obtained by removing variables one at a time until all remaining variables were significant at the P<0.01 level. All analyses were performed using the Statistical Package for the Social Sciences version 13.0 for Windows. Odds ratios and 95% confidence intervals are presented for the main findings.
Results
There were 36 984 individuals interviewed (response rate 77%), which represents a weighted sample of 23 662 430. Of the sample, 0.6% (unweighted n=222, weighted n=130 143) reported a suicidal act in the 12 months preceding the interview. Of those acts, 32.8% (n=42 687) resulted in injury, of which 55.5% (n=23 691) received medical attention. Nearly three-quarters (73.4%, n=17 389) of those requiring medical attention were hospitalised overnight. Over a quarter (26%, n=33 837) of those who reported a suicidal act said that they had had consulted a professional about suicidal feelings or ideation in the 12 months prior to interview. Individuals could have been in contact with more than one professional. Social workers were the most frequently consulted professionals (51%, n=17 257), followed by family doctors (39%, n=13 196) and psychiatrists (40%, n=13 535). Twenty-six per cent (n=33 837) acknowledged having performed a suicidal act at some time prior to the past 12 months.
The demographic, clinical and psychosocial characteristics of the respondents who reported a suicidal act in the 12 months preceding the interview are shown in Table 1. In comparison with the rest of the sample, these respondents were predominantly female, were less likely to be married or cohabiting, were younger, had a lower level of education, and a high proportion were unemployed. More than three-quarters of these respondents (77%) reported having one or more chronic health conditions. Almost two-thirds met lifetime criteria for a major depressive episode, with more than half meeting criteria for one or more episodes in the same 12-month period as the suicidal act. Rates of anxiety disorders and substance dependence were considerably lower. Almost half indicated that religion and spiritual values had an important role in their lives.
The associations between psychosocial and clinical variables and risk of 12-month suicidal act expressed as adjusted odds ratios are shown in Table 2. All variables are significant at the P<0.01 level. Younger age, female gender, unemployment and income inadequacy were associated with having made a suicidal act in the past 12 months. Education level revealed an inconsistent pattern. A previous major depressive episode was a significant correlate of suicide act status, as were substance dependence and one or more chronic medical conditions in the past 12 months. Suicidal acts were significantly associated with higher levels of tangible social support. Respondents who rated themselves as being less religious were more likely to report a suicidal act than those who participated in religious activities weekly. However, the odds of a suicidal act were considerably higher among those who participated intermittently than among those who never participated in religious activities.
Table 2 Demographic, clinical and psychosocial correlates of 12-month suicidal act

| OR (95% CI) | |
|---|---|
| Increasing age | 0.91 (0.90–0.91) |
| Female gender | 4.27 (4.05–4.50) |
| Education level | |
| Less than secondary a | |
| Graduated secondary | 0.90 (0.87–0.97) |
| Other post-secondary | 2.01(1.88–2.15) |
| Post-secondary graduate | 0.57 (0.53–0.61) |
| Income adequacy | |
| Low a | |
| Lower middle | 1.00 (0.93–1.1) |
| Middle | 1.00 (0.96–1.12) |
| Upper middle | 0.30 (0.28–0.32) |
| High | 0.34 (0.31–0.37) |
| Marital status | |
| Married a | |
| Cohabiting | 1.84 (1.72–1.97) |
| Widowed | 2.90 (2.56–3.33) |
| Separated | 37.88 (33.92–42.31) |
| Divorced | 7.79 (7.22–8.41) |
| Single | 3.15 (2.92–3.4) |
| Employment status | |
| Unemployed | 1.70 (1.5–1.8) |
| MDE in past 12 months | 9.10 (8.65–9.59) |
| Substance dependence in past 12 months | 2.62 (2.44–2.81) |
| Having a chronic condition | 1.70 (1.67–1.86) |
| Higher levels of tangible social support | 1.16 (1.15–1.17) |
| Self-perception of religiosity | |
| Very religious a | |
| Religious | 1.08 (0.99–1.18) |
| Not very religious | 2.17 (2.02–2.36) |
| Not religious at all | 2.27 (2.12–2.43) |
| Participation in religious activities in past year | |
| Once a week a | |
| Once a month | 2.10 (1.98–2.23) |
| 3–4 times a year | 4.27 (3.97–4.60) |
| Once a year | 2.94 (2.75–3.14) |
| Never | 1.18 (1.10–1.25) |
MDE, major depressive episode
a. Referent category
Discussion
This study examined the prevalence of 12-month suicidal acts in a Canadian national population survey and the demographic, clinical, and psychosocial correlates of suicidal acts in the year preceding interview. We found that 0.6% of the sample endorsed having performed a suicidal act, comparable to figures previously reported by Kessler et al in the USA Reference Kessler, Berglund, Borges, Nock and Wang4,Reference Kessler, Borges and Walters5 and by Paykel et al in the UK for attempted suicide. Reference Paykel, Myers, Lindenthal and Tanner11
Psychosocial correlates of suicidal acts
In addition to the demographic characteristics of female gender, Reference Schmidtke, Bille-Brahe, DeLeo, Kerkh of, Bjerke, Crepet, Haring, Hawton, Lonnqvist, Michel, Pommereau, Querejeta, Phillipe, Salander-Renberg, Temesvary, Wasserman, Fricke, Weinacker and Sampio-Feria9 younger age Reference Kreitman18 and White ethnicity, Reference Kessler, Borges and Walters5 a number of correlates for suicidal acts and attempts have been identified from studies of clinical samples. These include being separated or divorced, having a lower level of education, poverty, unemployment and social isolation, Reference Kessler, Borges and Walters5,Reference Schmidtke, Bille-Brahe, DeLeo, Kerkh of, Bjerke, Crepet, Haring, Hawton, Lonnqvist, Michel, Pommereau, Querejeta, Phillipe, Salander-Renberg, Temesvary, Wasserman, Fricke, Weinacker and Sampio-Feria9 and physical illness. Reference Nielsen, Wang and Brille-Brahe19 Religious beliefs and participation in religious activity are thought to be protective against suicidal behaviour. Reference Ellis and Smith20,Reference Koenig, Cohen, Blazer, Pieper, Meador, Shelp, Goli and DiPasquale21 In our study the psychosocial correlates of suicidal acts in this general adult population are consistent with those reported previously, namely female gender, Reference Schmidtke, Bille-Brahe, DeLeo, Kerkh of, Bjerke, Crepet, Haring, Hawton, Lonnqvist, Michel, Pommereau, Querejeta, Phillipe, Salander-Renberg, Temesvary, Wasserman, Fricke, Weinacker and Sampio-Feria9 being separated or divorced, Reference Kessler, Berglund, Borges, Nock and Wang4,Reference Kessler, Borges and Walters5,Reference Kreitman18 younger age, Reference Kessler, Berglund, Borges, Nock and Wang4,Reference Kreitman18 lower level of education, Reference Kessler, Berglund, Borges, Nock and Wang4,Reference Kessler, Borges and Walters5 and being unemployed. Reference Kessler, Berglund, Borges, Nock and Wang4,Reference Kessler, Borges and Walters5,Reference Schmidtke, Bille-Brahe, DeLeo, Kerkh of, Bjerke, Crepet, Haring, Hawton, Lonnqvist, Michel, Pommereau, Querejeta, Phillipe, Salander-Renberg, Temesvary, Wasserman, Fricke, Weinacker and Sampio-Feria9 Although ecological studies have long demonstrated associations between income and suicide, Reference Stack22 we are not aware of previous population-based survey data having confirmed this link. Probable relationships between perceived income adequacy and depression, substance dependence, physical illness burden and other unmeasured factors should be considered, however, and the finding interpreted with caution. It should also be noted that given the cross-sectional nature of the data, it is not possible to comment on the temporal ordering of events. Therefore, one cannot distinguish between whether the suicidal act, or the psychiatric symptoms linked with it, led to or were a consequence of psychosocial adversity. Reference Mann23
Physical conditions
Using National Comorbidity Survey (NCS) data from 1990–2, Goodwin et al found that even after controlling for socio-demographic variables, mental disorder diagnosis and regular physical activity, there were significantly increased odds of lifetime suicide attempt associated with having AIDS, lung disease or ulcers. Reference Goodwin, Marusic and Hoven24 Further, there was a linear association between the likelihood of suicide attempt and the total number of physical illnesses. These authors' findings were consistent with previous studies of physical illness and completed suicide, Reference Harris and Barraclough8 an issue particularly pertinent to older adults. Reference Waern, Rubenowitz, Runeson, Skoog, Wilhemson and Allbeck25 Our observation of increased odds for suicidal acts within the past 12 months and having one or more chronic medical conditions in that same time frame reinforces the need to consider primary and specialty medical practice as a venue for suicide risk assessment and prevention. Reference Bruce, Ten Have, Reynolds, Katz, Schulberg, Mulsant, Brown, McAvay, Pearson and Alexopoulos26
Psychiatric conditions
Most individuals who complete or attempt suicide have a diagnosable psychiatric illness; Kessler et al reported that 88–89% of suicide attempters met criteria for one or more 12-month DSM disorders. Reference Kessler, Berglund, Borges, Nock and Wang4 Depressive disorders are most often diagnosed. Reference Moscicki, O'Carroll, Rae, Locke, Roy and Regier7,Reference Harris and Barraclough8 This data-set allowed us to examine fewer psychiatric disorders than Kessler et al; Reference Kessler, Borges and Walters5 nevertheless, the nine times greater odds of suicidal act among respondents with a major depressive episode that we observed is similar to the strength of the association they reported (OR=11). In contrast, the presence of a substance dependence diagnosis, social phobia or panic attacks in the past 12 months did not increase the odds of an act in that same time frame in the Canadian sample, whereas substance use disorders and anxiety disorders (including social phobia and panic disorder) were significant predictors in the NCS, albeit at considerably lower odds ratios than for major depression. Vigilance for mood disorders in health settings and routine screening for suicidal ideation and intent when depression is present are warranted. Although similar caution is indicated for suicide among patients with other psychiatric diagnoses, additional study is needed to translate the implications of population-based observations to health policy.
The finding that increased levels of tangible support were associated with increased risk of suicidal act appears contradictory at first. Although we cannot comment on the temporal relationship between the suicide act and the other factors studied, this finding may reflect that individuals received increased practical support following the act.
Religious beliefs
Previous research suggests that religious beliefs and participation in religious activities protect against suicide. Reference Ellis and Smith20,Reference Koenig, Cohen, Blazer, Pieper, Meador, Shelp, Goli and DiPasquale21,Reference Nisbet, Duberstein, Conwell and Seidlitz27 Consistent with these reports, we found a linear relationship between self-perceived religiosity and the odds of a suicidal act in the past 12 months. The relationship with participation in religious activities was less straightforward. Weekly participants were clearly at lowest risk, underscoring the protective effect of religious engagement. We also observed, however, that those who never participated in religious activities were at less risk of suicidal acts than individuals who did so three or four times a year, and those who participated monthly and once a year were at intermediate risk. The means by which frequent and regular religious participation protects from suicide remains obscure. Postulated mechanisms include a broader social network and increased instrumental support that may result from frequent participation. Reference Ellis and Smith20 Alternatively, if frequent participation is linked to closer adherence to a religious doctrine that strongly proscribes suicide (as does, for example, the Catholic church), these individuals might be less likely to harm themselves. Reference Ellis and Smith20 The greater risk associated with intermediate or irregular participation than none is more difficult to explain. This pattern could result if irregular participation were an indicator of ambivalent religiosity, an episodic response to crises in one's life, or a means of managing ongoing stress. Greater attention should be given to opportunities for detection and prevention of suicide through programming based in the faith community.
Study limitations
This study is subject to a number of limitations. First, we refer here to ‘suicidal acts’ as no definition of suicide attempt was provided for respondents and no measure of suicidal intent was available to include in analyses. Consequently, suicidal ideation and self-harming behaviours without intent to die might have been endorsed by some respondents and included as suicidal acts. Such misclassification would inflate the rates reported here. Evidence suggests that those who injure with intent to die differ significantly from ideators and those who act without lethal intent; they engage in more serious self-injury, and are more likely to die subsequently by suicide. Reference Nock and Kessler28 Our findings, therefore, should be interpreted with caution.
Because of the construction of the survey, we were unable to determine whether participants who reported no suicidal act in the past 12 months had one or more suicidal acts earlier in life. Nor could we establish the number of suicidal acts in those who did endorse one or more in the past 12 months, or examine their level of lethality of implementation or intent. Repeat suicidal acts and acts with high potential lethality may have different implications for risk assessment and prevention. Reference Hawton and Fagg29,Reference Hawton, Harriss and Zahl30 Subsequent population-based surveys should include measures that allow more refined analyses of subgroups of suicidal people. The data are based on self-disclosure from respondents and may be an under-representation of suicidal acts. However, the fact that identical 12-month prevalence figures were reported from the NCS in the USA Reference Kessler, Berglund, Borges, Nock and Wang4 and by Paykel et al in the UK Reference Paykel, Myers, Lindenthal and Tanner11 lend confidence, at least, to the reliability of the findings. Respondent bias may influence reporting of psychiatric symptoms such as depression, which in turn might influence reporting of physical conditions, income adequacy, social support and spirituality. Although the sample is representative of the Canadian population aged over 15 years, the number who endorsed suicidal acts was insufficient to allow examination of subgroups (categorised for example by gender, age, ethnicity, reason for unemployment or urban/rural residence) without threatening to compromise respondent anonymity. Neither could the sample size support modelling of potentially important interactions between correlates. Future studies should include even larger samples to enable more fine-grained analyses of putative risk factors, and their interactions, in specific segments of the population.
The interviews were conducted by lay interviewers and not clinicians. Therefore, it was not possible to distinguish between affective disorders due to the direct physiological effects of a substance (e.g. illicit drugs or medication and those due to a general medical condition). For that reason, we refer only to ‘major depressive episode’ rather than major depressive disorder.
Implications of the study
Suicide and suicidal acts are a major cause of morbidity and mortality throughout the world. Strategies that target the detection and treatment of individuals at high risk of suicidal behaviour are an essential element of any comprehensive prevention strategy. Strategies that target high-risk populations alone are insufficient; Reference Knox, Conwell and Caine31 they must be complemented by population-based strategies that target vulnerable individuals and groups prior to the development of suicidal crises and entry into the clinical care system – or death. Survey data from representative samples of the general population yield information that is essential to the design and ongoing evaluation of those strategies. Consistent with findings from the NCS, this study reinforces the importance to the determination of suicide risk and its prevention not only of psychiatric illness, but of physical and psychosocial factors as well.
Acknowledgements
Data analysis for this study was supported in part by a grant from the Canadian Institutes of Health Research (ACC65796). The views and opinions expressed in this report are those of the authors and should not be construed to represent the views of the sponsoring organisation or Statistics Canada. We wish to thank the staff of the Statistics Canada at the Toronto RDC, particularly Veronica Yei, Angela Prencipe and Byron Lee for their assistance with this project. E.D.C. and Y.C. were supported in part by National Institutes of Health grant P20 MH071897.







eLetters
No eLetters have been published for this article.