2 results
Optimizing Urine Collection Represents an Important Stewardship Opportunity in Primary Care
- Larissa Grigoryan, Jennifer Matas, Michael Hansen, Samuel Willis, Lisa Danek, Anna Katta, Kenneth Muldrew, Mohammad Zare, Forrest Hudson, Robert Atmar, Andrew Chou, Barbara Trautner
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s14-s15
-
- Article
-
- You have access Access
- Open access
- Export citation
-
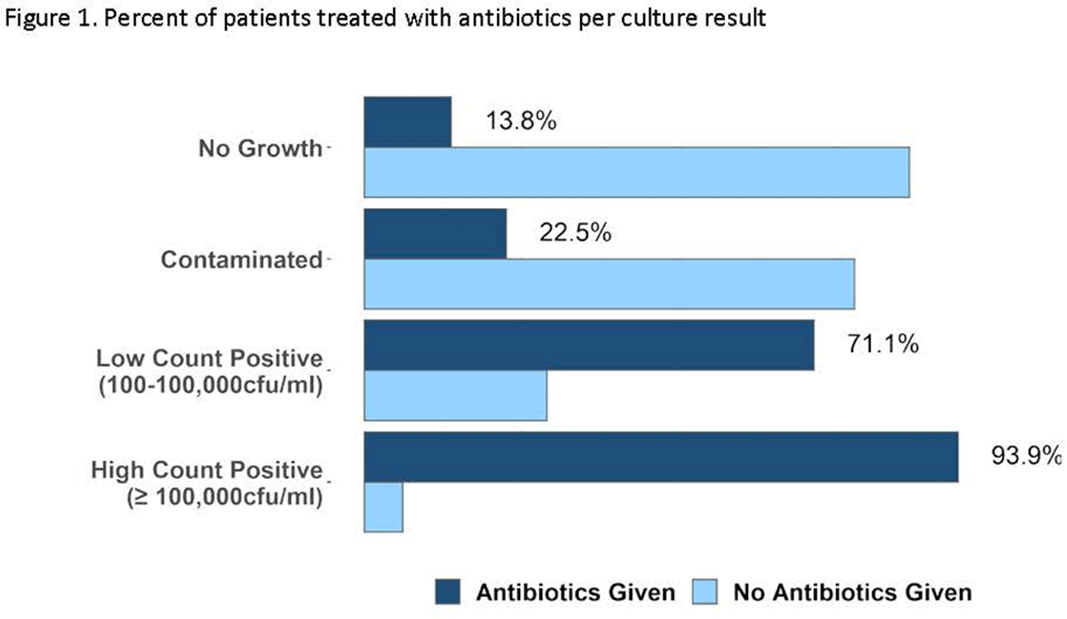
Background: Urine cultures are the most common microbiological tests in the outpatient setting and heavily influence treatment of suspected urinary tract infections (UTIs). Antibiotics for UTI are usually prescribed on an empiric basis in primary care before the urine culture results are available. However, culture results may be needed to confirm a UTI diagnosis and to verify that the correct antibiotic was prescribed. Although urine cultures are considered as the gold standard for diagnosis of UTI, cultures can easily become contaminated during collection. We determined the prevalence, predictors, and antibiotic use associated with contaminated urine cultures in 2 adult safety net primary care clinics. Methods: We conducted a retrospective chart review of visits with provider-suspected UTI in which a urine culture was ordered (November 2018–March 2020). Patient demographics, culture results, and prescription orders were captured for each visit. Culture results were defined as no culture growth, contaminated (ie, mixed flora, non-uropathogens, or ≥3 bacteria isolated on culture), low-count positive (growth between 100 and 100,000 CFU/mL), and high-count positive (>100,000 CFU/mL). A multivariable multinomial logistic regression model was used to identify factors associated with contaminated culture results. Results: There were 1,265 visits with urine cultures: 264 (20.9%) had no growth, 694 (54.9%) were contaminated, 159 (12.6%) were low counts, and 148 (11.7%) were high counts. Encounter-level factors are presented in Table 1. Female gender (adjusted odds ratio [aOR], 15.8; 95% confidence interval [CI], 10.21–23.46; P < .001), pregnancy (aOR, 13.98; 95% CI, 7.93–4.67; P < .001), and obesity (aOR, 1.9; 95% CI 1.31–2.77; P < .001) were independently associated with contaminated cultures. Of 264 patients whose urine cultures showed no growth, 36 (14%) were prescribed an antibiotic. Of 694 patients with contaminated cultures, 153 (22%) were prescribed an antibiotic (Figure 1). Conclusions: More than half of urine cultures were contaminated, and 1 in 5 patients were treated with antibiotics. Reduction of contamination should improve patient care by providing a more accurate record of the organism in the urine (if any) and its susceptibilities, which are relevant to managing future episodes of UTI in that patient. Optimizing urine collection represents a diagnostic stewardship opportunity in primary care.
Funding: This study was supported by the National Institute of Allergy and Infectious Diseases of the National Institutes of Health (grant no. UM1AI104681). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Disclosures: None
Table 1. 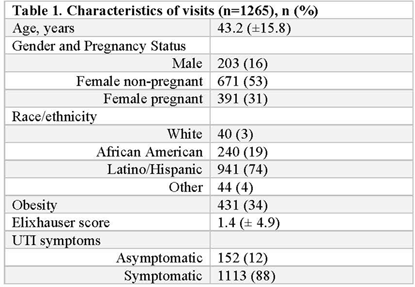
Figure 1.
Creating an Outpatient-Specific Antibiogram to Guide Treatment for Urinary Tract Infections
- Larissa Grigoryan, Melanie Goebel, Samuel Willis, Lisa Danek, Jennifer Matas, Neal Kachalia, Anna Katta, Kenneth Muldrew, Mohammad Zare, Forrest Hudson, Robert Atmar, Barbara Trautner
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s182-s183
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Outpatients with uncomplicated urinary tract infections (UTIs) are often treated empirically without culture, whereas urine cultures are typically collected from patients with complicated UTI. Susceptibilities for fosfomycin (a first-line agent) are not routinely performed or reported in the antibiogram. Understanding the prevalence of antibiotic resistance for UTI is critical for empiric treatment and antibiotic stewardship in primary care. Methods: We developed a UTI-focused antibiogram from a prospective sample of outpatients (women and men) with UTIs from 2 public family medicine clinics in an urban area with a diverse, international population (November 2018 to present). During the study period, providers ordered a urine culture for any adult patient presenting with UTI symptoms, including uncomplicated and complicated infections. We estimated the prevalence of resistance to UTI-relevant antibiotics in the overall study population and compared it between patients born in the United States and other countries. Results: We collected 678 urine cultures from 644 unique patients (79% female). Of these cultures, 158 (23.3%) had no growth, 330 (48.7%) grew mixed urogenital flora, and 190 (28.0%) were positive (>10,000 CFU/mL). Patients with positive cultures were mostly female (88.2%), and their mean age was 46.6 ± 14.8 years. Among patients with positive cultures, 42.7% were born in the United States and 57.3% were born Mexico or Central America. Escherichia coli was the most commonly isolated organism (Fig. 1). Susceptibility results for E. coli and all gram-negative organisms combined are presented in Fig. 2. Susceptibility of uropathogens to TMP-SMX was significantly higher in patients born in the United States compared to patients from Mexico or Central America (82% vs 61%; P = .03). Susceptibility to ciprofloxacin was similar in patients born in the United States and other countries (79% vs 72%; P = .50). Of 77 E. coli isolates, 11 (14%) were positive for extended-spectrum β-lactamase production, including 8 isolates from patients whose country of origin was Mexico or a Central American country. Conclusions: More than 20% of outpatients presenting with UTI symptoms had a negative urine culture. Among outpatients with uncomplicated and complicated UTI, uropathogens had a high prevalence of resistance to ciprofloxacin and TMP-SMX, but susceptibility to fosfomycin (restricted in our system) was 100%. Resistance rates for TMP-SMX were higher in patients from Mexico and Central America. Our findings question whether TMP-SMX should remain a first-line agent in US primary-care settings.
Funding: This project was supported by the National Institute of Allergy and Infectious Diseases of the National Institutes of Health under Award Number UM1AI104681.
Disclosures: None





