3 results
End-of-life care and hospital-acquired bloodstream infection
- Melanie Zarnoski, Patrick Burke, Steven Gordon, Joanne Sitaras, Thomas Fraser
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s50
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: All critically ill patients are at risk for hospital-acquired bloodstream infection (HABSI). At any time, however, there is heterogeneity among patients in the ICU; some patients have the added complexity of end-of-life discussions. We sought to better understand the patients in our medical intensive care unit (MICU) with HABSIs that do and do not meet the NHSN definition for a central-line–associated bloodstream infection (CLABSI) event by evaluating for the presence of a do-not-resuscitate (DNR) order. Methods: The study was conducted at our 66-bed MICU at the Cleveland Clinic Main Campus between January 2021 and September 2022. Surveillance for HABSI to include determination of CLABSI is performed prospectively according to the NSHN definition. The electronic health record was queried for each patient with a HABSI for the presence of a DNR order. DNR orders were categorized as follows: prevalent (DNR orders present at the time of admission to the MICU), incident (orders entered after admission to the MICU), or no DNR (for patients without an order at any time during their MICU stay). For incident orders, time from order to HABSI was recorded. Time to event was calculated as days between ICU admission to HABSI. Results: During the observation period there were 36,477 MICU patient days and 4,815 admissions. There were 112 HABSIs, of which 48 (43%) were CLABSIs. Overall, 65 patients were categorized as incident DNR, 7 were categorized as prevalent DNR, and 40 were categorized as no DNR. For patients with an incident DNR order, 50 HABSIs occurred on the date of or before the order and 15 occurred after the order. In patients in whom HABSI occurred after the incident DNR order, the median number of days between DNR order and HABSI was 11 days (range, 1–69). Discussion: In our MICU, >50% of HABSIs and 60% of CLABSIs occurred in patients with a DNR order incident to their MICU stay. Interventions to prevent hospital-acquired bloodstream infection and the analysis of the events are inextricably linked to issues of end-of-life care for critically ill patients. Further exploration of patient characteristics easily obtainable from the EHR, such as DNR orders, is necessary to inform best practices for prevention and risk adjustment of bloodstream infection rates.
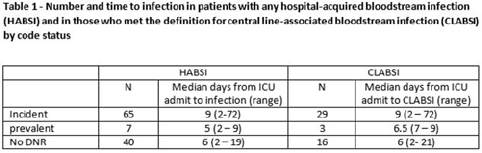
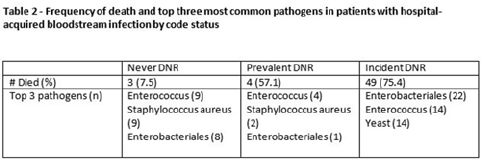
Disclosures: None
Rapid identification and isolation of patients with COVID-19 reduces the odds of transmission to hospital roommates
- Jessica Alban, Patrick Burke, Joanne Sitaras, Thomas Fraser
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s39-s40
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The Cleveland Clinic Main Campus is a multispecialty academic medical center with 1,200 adult patient beds, 58% of which are double occupancy. Our facility relies on double-occupancy rooms to provide needed care during the COVID-19 pandemic. Inherently, double occupancy poses a greater risk of exposure to SARS-CoV-2 despite mitigation efforts. We investigated the incidence of postexposure SARS-CoV-2 infection in double-occupancy rooms and evaluated risk factors for viral transmission. Methods: Early in the observation period patients were tested for SARS-CoV-2 based on clinical suspicion. By June 2020, all admitted patients were tested. Symptomatic patients were admitted with pending tests under transmission-based precautions. Asymptomatic patients were managed with standard precautions including patients admitted to double-occupancy rooms. A double-occupancy exposure event was defined as an uninfected patient sharing a room with a patient positive for SARS-CoV-2. All patient exposures were tracked and evaluated by the infection prevention (IP) team. The IP prospective review of source patients included determination of lowest cycle threshold (Ct) value of first COVID-19 test, and whether their infection was hospital or community onset. Review of exposed patients included sex, age, and exposure time (in hours) to the source patient. Postexposure infection was defined as a positive test for SARS-CoV-2 in the exposed population within 14 days of the defined exposure event. We fit a multivariable logistic regression model to estimate the effect of exposure time on the odds of postexposure infection in susceptible roommates. Results: From March 15 to December 15, 2020, 172 susceptible patients were exposed to a roommate with COVID-19. Also, 28 exposed patients met our definition for postexposure infection (attack rate, 16%). The frequency of postexposure infection was higher in patients for whom the source was hospital-onset versus community-onset disease (25% vs 10%; P = .01) and when the source patient’s Ct value was below the median value of 21.1 (26% vs 11% p Conclusions: We identified a postexposure infection attack rate of 16% for double-occupancy patients in the first 9 months of the pandemic. Time exposed to source patient was significantly associated with infection. Our experience demonstrates the potential benefit of asymptomatic admission testing with expedited turnaround time to mitigate viral transmission between patients in double-occupancy rooms.
Funding: None
Disclosures: None
Peripherally Inserted Central Catheters Present on Admission and the Risk of Central-Line–Associated Bloodstream Infection
- Patrick Burke, Elise Nickoli, Joanne Sitaras, Wanda Mullins, Patricia Dandache
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s349
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Patients presenting to hospitals often arrive with peripherally inserted central catheters (PICC) in place upon admission. The admitting facility may not be familiar with that device’s history and the unknown risk for bloodstream infection associated with it often prompts requests for device replacement. A blanket approach to “change all lines” must be balanced with the potential for patient discomfort and insertion-related complications. To better inform our approach to prevention, we determined the incidence of central-line–associated bloodstream infection (CLABSI) in adult patients presenting to hospitals in our health system with a PICC present on admission (POA), relative to those who have a PICC placed after admission (PAA). Methods: This retrospective cohort study included all adult hospital encounters at 11 Cleveland Clinic acute-care hospitals lasting > 2 days in 2018 with electronic medical record nursing care flowsheet documentation of a PICC during the stay. Patients whose admission diagnosis was related to intravascular catheter infection, children aged <18 years, and observation unit encounters were excluded. Patients were categorized as having a PICC POA if a nurse selected that option on a PICC flowsheet, otherwise the patient was categorized has having a PICC PAA. Surveillance for CLABSI was performed in all inpatient locations at all hospitals according to the NHSN protocol. Patients with ≥1 CLABSI were matched to encounters by name and date of admission. Repeat infections occurring to the same patient were excluded. Results: Of the 8,827 eligible hospital encounters, 1,799 (20%) involved a PICC POA and 7,028 (80%) had PICCs PAA. Across 11 hospitals, the median proportion of PICC-associated encounters with a device POA was 15% (range, 8%–25%). Moreover, 23 of the 112 CLABSIs (21%) in our cohort occurred in patients with a PICC POA and 89 (79%) occurred in patients with a PICC PAA (Table 1). The overall relative risk of CLABSI, whether the PICC was placed before or after admission, was 1.00 (95% CI, 0.64–1.60). Conclusions: Patients with a PICC present on admission to our hospitals were no more likely to experience a CLABSI than patients who had a PICC placed after admission. Replacing vascular catheters that are POA may not reduce the risk of CLABSI. With up to 25% of PICC-associated encounters having the device POA, universal device replacement at admission would involve hundreds of patients per year at our multihospital health system.
Funding: None
Disclosures: None





