2 results
Transmission of multidrug-resistant organisms by VA CLC residents: A multisite prospective study
- Lona Mody, Kristen Gibson, Marco Cassone, Sanjay Saint, Sarah Krein, Julia Mantey, Mary Janevic, Alexandria Nguyen, Taissa Bej, Oteshia Hicks, Lillian Min, Andrzej Galecki, M Todd Greene, Laxmi Chigurupat, Robin Jump
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s116-s117
-
- Article
-
- You have access Access
- Open access
- Export citation
-
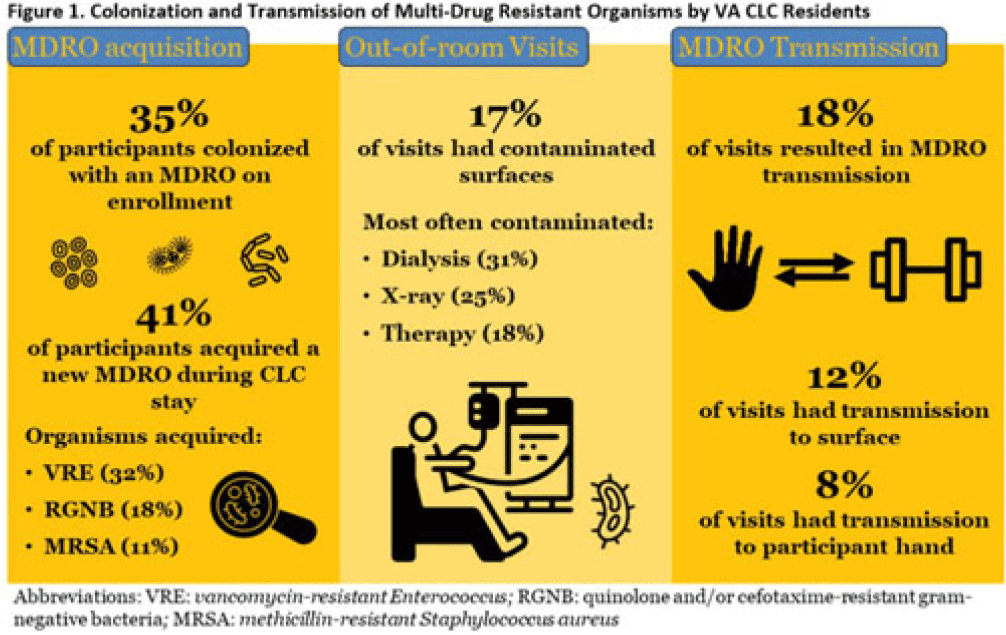
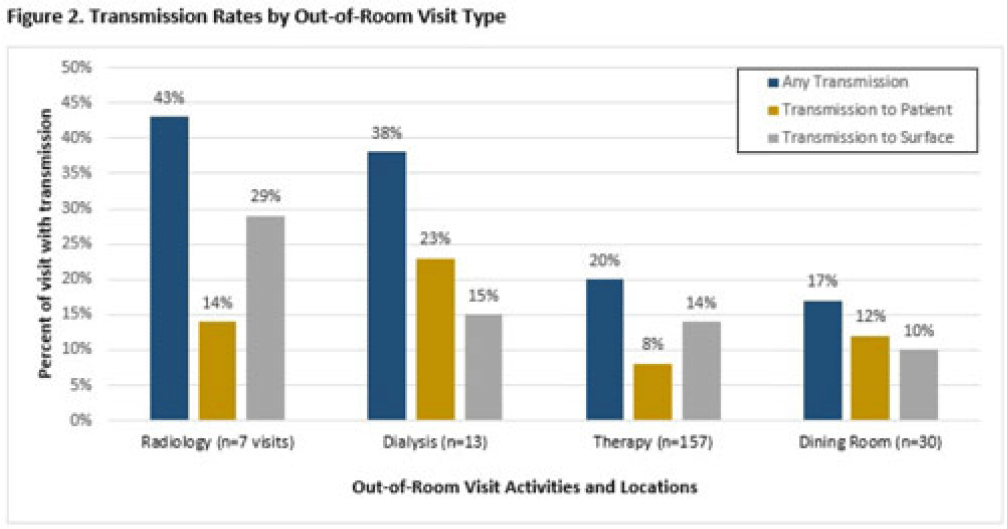
Background: Veterans Health Administration (VHA) community living centers (CLCs) provide postacute and long-term care. CLC veterans visit myriad locations outside their rooms (eg, rehabilitation, dialysis). Pathogen transmission during out-of-room visits is unknown. Methods: We recruited newly admitted veterans at 3 CLCs. After obtaining informed consent, we cultured nares, groin, hands, and 7 surfaces in the patient rooms. We accompanied veterans to up to 5 out-of-room visits and cultured patients’ hands and surfaces they touched. We tested for multidrug-resistant organisms (MDROs) including methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant Enterococcus (VRE), and quinolone, carbapenem, and/or ceftazidime-resistant gram-negative bacteria (R-GNB). We defined transmission as a positive culture following an initial negative culture during the same visit. Results: We enrolled 137 veterans (median follow-up, 29 days; mean, 5.9 visits); 97% were postacute patients. We conducted 539 patient-room sampling visits (mean, 3.9 per veteran; 5,490 swabs) and accompanied 97 veterans to 266 out-of-room sampling visits (mean, 2.7 per veteran; 2,360 swabs). Of 137 patients, 47 (35%) were colonized with an MDRO at enrollment and 74 (58%) of 128 patients were colonized on any follow-up patient-room visits. Of 133 patients, 55 (41%) acquired a new MDRO, most often VRE (31 of 97, 32%). In patient rooms, toilet seats [114 (21%) of 538], curtains [101 (19%) of 530] and bedrails [98 (18%) of 539] were most frequently contaminated. Among 266 out-of-room visits, 17% had surfaces contaminated with MDROs, most commonly involving dialysis [4 (31%) of 13], radiology [2 (25%) of 8], and rehabilitation therapy [29 (18%) of 159] (Fig. 1).Transmission of MDROs during out-of-room visits was common and occurred in 18% of visits with 8% (9 MRSA and 12 VRE) acquiring a new MDRO on their hands and 12% (9 MRSA and 23 VRE) of MDRO transmission occurring from hands to a surface that the patient touched (Fig. 1). In 18 (58%) of 31 cases, the organism transmitted to a surface was on patient hands at the start of the visit. Transmission was most common during visits to dialysis (3 to patients and 2 to surfaces), radiology (1 to a patient and 2 to surfaces), and rehabilitation therapy (13 to patients and 21 to surfaces) (Fig. 2). Conclusions: New MDRO acquisition during VHA CLC stay was common, and nearly one-fifth of out-of-room visits resulted in MDRO transmission. Our analyses suggest that veterans’ hands may shed MDROs (MRSA and VRE) to surfaces. Interventions to reduce MDRO transmission during visits for rehabilitation, dialysis, and other therapies are needed.
Disclosures: None
Using telehealth to support antimicrobial stewardship at four rural VA medical centers: Interim analysis
- Alexandria Nguyen, Mayyadah Alabdely, Taissa Bej, Tola Ewers, Tammy Walkner Amanda Vivo, Christopher Crnich, Daniel Livorsi, Rabeeya Sabzwari, Geneva Wilson, Brigid Wilson, Corinne Kowal, Oteshia Hicks, Charlesnika Evans, Robin Jump
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s110
-
- Article
-
- You have access Access
- Open access
- Export citation
-
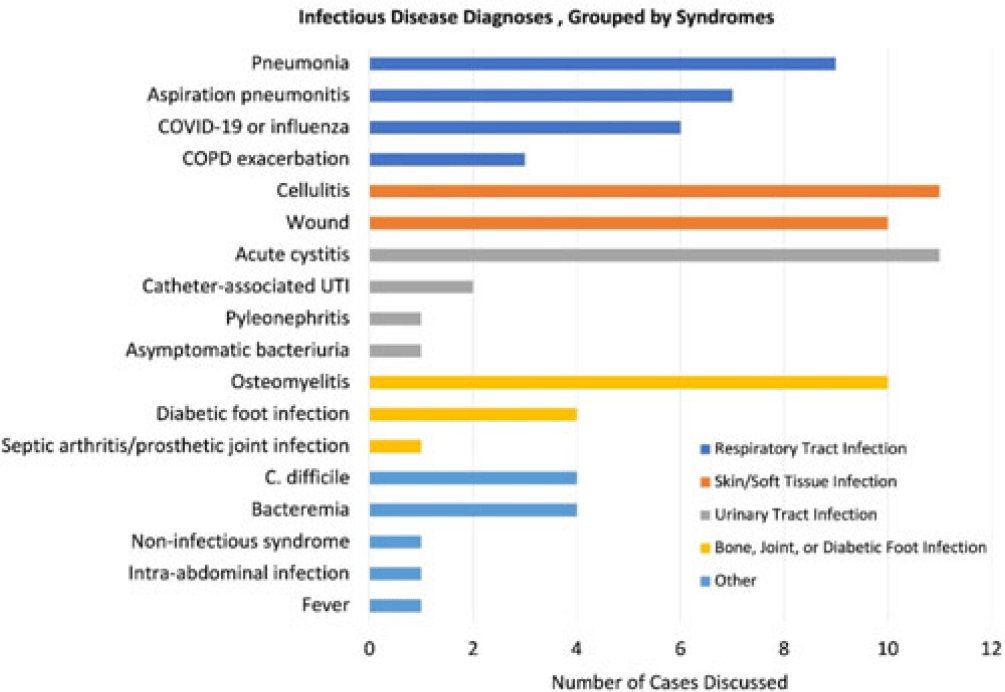
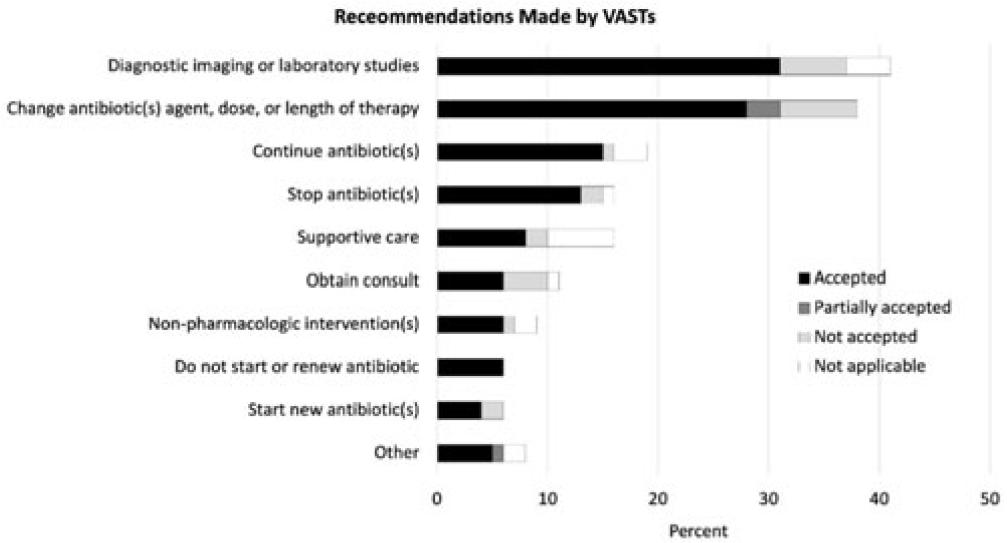
Background: Healthcare settings without access to infectious diseases experts may struggle to implement effective antibiotic stewardship programs. We previously described a successful pilot project using the Veterans Affairs (VA) telehealth system to form a Videoconference Antimicrobial Stewardship Team (VAST) that connected multidisciplinary teams from rural VA medical centers (VAMCs) with infectious diseases experts at geographically distant locations. VASTs discussed patients from the rural VAMC, with the overarching goal of supporting antibiotic stewardship. This project is currently ongoing. Here, we describe preliminary outcomes describing the cases discussed, recommendations made, and acceptance of those recommendations among 4 VASTs. Methods: Cases discussed at any of the 4 participating intervention sites were independently reviewed by study staff, noting the infectious disease diagnoses, recommendations made by infectious diseases experts and, when applicable, acceptance of those recommendations at the rural VAMC within 1 week. Discrepancies between independent reviewers were discussed and, when consensus could not be reached, discrepancies were discussed with an infectious diseases clinician. Results: The VASTs serving 4 different rural VAMCs discussed 96 cases involving 92 patients. Overall, infection of the respiratory tract was the most common syndrome discussed by VASTs (Fig. 1). The most common specific diagnoses among discussed cases were cellulitis (n = 11), acute cystitis (n = 11), wounds (n = 11), and osteomyelitis (n = 10). Of 172 recommendations, 41 (24%) related to diagnostic imaging or laboratory results and 38 (22%) were to change the antibiotic agent, dose, or duration (Fig. 2). Of the 151 recommendations that could be assessed via chart review, 122 (81%) were accepted within 1 week. Conclusions: These findings indicate successful implementation of telehealth to connect clinicians at rural VAMCs with an offsite infectious diseases expert. The cases represented an array of common infectious syndromes. The most frequent recommendations pertained to getting additional diagnostic information and to adjusting, but not stopping, antibiotic therapy. These results suggest that many of the cases discussed warrant antibiotics and that VASTs may use the results of diagnostic studies to tailor that therapy. The high rate of acceptance suggests that the VASTs are affecting patient care. Future work will describe VAST implementation at 4 additional VAMCs, and we will assess whether using telehealth to disseminate infectious diseases expertise to rural VAMCs supports changes in antibiotic use that align with principles of antimicrobial stewardship.
Disclosures: None







