4 results
Estimating racial differences in risk for CLABSI in a large urban healthcare system
- Giancarlo Licitra, Scott Fridkin, Zanthia Wiley, Lindsey Gottlieb, William Dube, Vishnu Ravi Kumar, Rachel Patzer, Radhika Prakash Asrani
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s50-s51
-
- Article
-
- You have access Access
- Open access
- Export citation
-
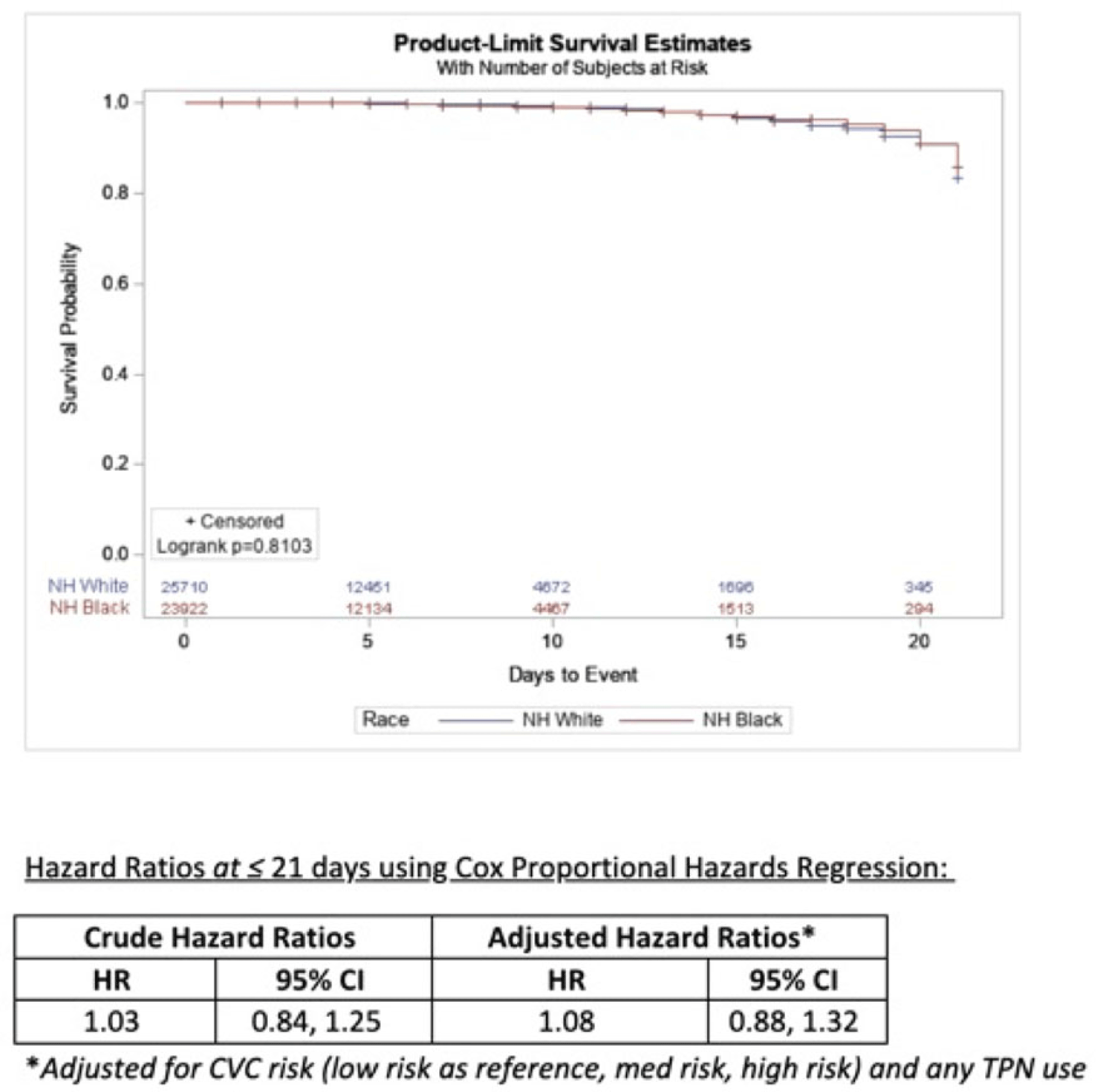
Background: Socioeconomic barriers or divergent implementation of prevention measures may impact risk of healthcare-associated infections by racial groups. We utilized a previously studied cohort of patients to quantify disparities in central-line–associated bloodstream infection (CLABSI) risk by race accounting for inherent differences in risk related to device utilization. Methods: In a retrospective cohort of adult patients at 4 hospitals (range, 110–733 beds) from 2012 to 2017, we linked central-line data to patient encounter data: race, age, comorbidities, total parenteral nutrition (TPN), chemotherapy, CLABSI. Analysis was limited to patients with >2 central-line days and <3 concurrent central lines. Patient exposures were calculated for each central-line episode (defined by insertion and removal dates); analysis of central-line episode-specific risk of CLABSI among Black versus White patients adjusted for clinical factors, duration of central-line episode, and central-line risk category (ie, low: single port, dialysis or PICC; medium: single temporary or nontunneled; or high: any concurrent central-lines) in Cox proportional hazards regression of time to CLABSI. Results: In total, 526 CLABSIs occurred a median of 14 days after insertion among 57,642 central-line episodes in 32,925 patients. CLABSIs occurred in similar frequency across racial groups: 217 (1.7%) among Black patients, 256 (1.6%) among White patients, and 11 (1.6%) among Hispanic patients (also 42 among unknown or other race). Duration of central-line episode was similar between racial groups (median, 5 days). Black patients were less likely to have medium-risk central lines (34%) compared to white patients (RR, 0.82; 95% CI, 0.79–0.84), but they had a similar frequency of high-risk central lines (21%; RR, 1.0; 95% CI, 1.0–1.1). Compared with low-risk central lines, risk of CLABSI was increased among medium-risk central lines (RR, 1.3; 95% CI, 1.0–1.7) and high-risk central lines (RR, 2.2; 95% CI, 1.8–2.7). CLABSIs were more likely in TPN central lines (RR, 2.3; 95% CI, 1.9–2.7) than others, but they were not more likely among Black patients than White patients (RR, 0.9; 95% CI, 0.1–1.1). In survival analysis, there were 24,700 central-line episodes among Black patients compared to 26,648 episodes among White patients; adjusting for central-line risk and TPN, the risk of CLABSI was similar during the first 21 days of central-line use (adjusted hazard ratio, 1.08; 95% CI, 0.88–01.32) (Fig. 1). Conclusions: After accounting for central-line configuration, Black patients did not have a higher risk of CLABSI within 21 central-line days. Further evaluation is warranted to assess racial disparities in risks of other healthcare-associated infections and to determine whether a lack of CLABSI-specific racial disparities can be replicated in other regions and healthcare systems.
Disclosures: None
4354 The Impact of the 2014 Kidney Allocation System on Waitlisting Rates at the Dialysis Facility Level
- Taylor Andrew Melanson, Jennifer Gander, Rachel Patzer
-
- Journal:
- Journal of Clinical and Translational Science / Volume 4 / Issue s1 / June 2020
- Published online by Cambridge University Press:
- 29 July 2020, pp. 148-149
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: The new Kidney Allocation System (KAS) was implemented in 2014 and it is not fully understood how its changes to patient incentives may have impacted dialysis facility waitlisting rates. We examine differences in facility performance and how such differences may have been impacted by this policy change. METHODS/STUDY POPULATION: We used Dialysis Facility Report data from 2011 to 2017 to study waitlisting rates at 3,392 dialysis facilities in the US, using waitlisting counts in the numerator, and the total number of ESRD patients in a facility as the denominator. We examined changes in waitlisting rates over by year at the facility, regional, and national level, and report national trends in waitlisting pre- and post-KAS. Facilities were stratified based on waitlisting rate in 2011 and then we examined whether each facility moved into a higher or lower quartile or stayed in the same quartile in 2017. RESULTS/ANTICIPATED RESULTS: Among n = 3,392 dialysis facilities, the average change in dialysis facility waitlisting rates from 2011 to 2017 was −4.74 percentage points (range -54.4% to 42.3%). Average change in dialysis facility waitlisting rates from 2011 to 2014 was −0.57 percentage points while the average change in dialysis facility waitlisting rates from 2014 to 2017 was −4.17 percentage points. Half of facilities in the 2011 lowest quartile remained in the lowest quartile in 2017; 45% of facilities in the top 2011 quartile dropped into a lower quartile. The middle 2 quartiles were fairly evenly split between worsening, improving, and not changing. DISCUSSION/SIGNIFICANCE OF IMPACT: Average waitlisting rates have declined since KAS implementation. Many facilities switched quartiles from 2011-17 suggesting that facility waitlisting rates are unstable over time. The decline in waitlisting rates post-KAS suggests that new allocation rules may be discouraging patients and/or providers from getting ESRD patients waitlisted.
3259 Identifying the barriers and disparities for referral to kidney transplantation faced by HIV-infected patients with End Stage Renal Disease.
- Ruth Adekunle, Aneesh Mehta, Rachel Patzer, Wendy Armstrong, Ashley Burroughs
-
- Journal:
- Journal of Clinical and Translational Science / Volume 3 / Issue s1 / March 2019
- Published online by Cambridge University Press:
- 26 March 2019, p. 90
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: Our study aims to create a novel state level HIV-ESRD dataset and compare patient-level characteristics on rates of transplant referral, evaluation, waitlisting, and transplantation for HIV-positive versus HIV-negative patients. Our main hypothesis is that HIV-positive patients in Georgia are less likely to be referred to kidney transplant compared with HIV-negative patients. METHODS/STUDY POPULATION: Three datasets will be merged in order to create the HIV-ESRD dataset. The datasets are United States Renal Data System (USRDS), a southeast Transplant Referral Dataset and patient-level Georgia Department of Public Health HIV Incidence Database. The resulting study population will include patients that are older than 18, but less than 70, are HIV-positive and are on dialysis in Georgia. This dataset will also identify those patients who have been referred to transplantation, have been waitlisted, and have received kidney transplants between January 2012 and December 2017. If within a 1-year period, the prevalence of HIV-positive patients referred to transplant was lower than the 1-year period prevalence of HIV-negative patients for 3 consecutive years, the dialysis facility will be classified as having a within-facility disparity. We will then characterize patient level and dialysis facility-level factors that may contribute to observed findings. Patient characteristics will include demographic, clinical data, proxies of socioeconomic status, and geospatial relationships to transplant centers and rural vs urban neighborhoods. Facility-level characteristics includes profit status (profit vs. nonprofit), total number of staff (including full-time and part-time employees), aggregate demographic and clinical facility characteristics, and total number of treated patients. RESULTS/ANTICIPATED RESULTS:. We anticipate the successful creation of the proposed dataset that will allow for accurate identification of HIV-positive patients on dialysis in Georgia.. This dataset will provide the ability to determine referral, waitlisting, and transplantation rates.. We predict the overall rate of referral, waitlisting, and kidney transplantation in HIV patients will be relatively low, and that dialysis facilities with a higher proportion of HIV-positive will have lower referral rates compared to dialysis facilities treating a higher proportion of HIV-negative patients. It is foreseen that among patient-level characteristics, the strongest predictor for decreased referral rates will be HIV serostatus and among dialysis facility factors, profit status will be associated with decreased referral rates. DISCUSSION/SIGNIFICANCE OF IMPACT: This pilot study offers the creation of the first regional dataset of HIV-ESRD patients that will include patient-level characteristic of HIV-positive patients and provide a model for other states to adopt. We will contribute improved state-level description of incidence data of HIV-positive patients on dialysis, current rates of transplant referral, waitlisting, and transplantation, and offer potential associated factors that influence these processes. This knowledge will be used to determine the next steps in improving access to care; conducting qualitative research to understand dialysis facility views on transplant in HIV patients, understanding HIV patient’s position on transplantation, providing education on the value of kidney transplant referral, and expanding the approach of combining patient level HIV data to the southeast.
2279 Understanding care delivered to patients with a possible concussion at an urban level 1 trauma center
- Chet C. Zalesky, David W. Wright, Sanam Patel, Rachel K. Patzer
-
- Journal:
- Journal of Clinical and Translational Science / Volume 2 / Issue S1 / June 2018
- Published online by Cambridge University Press:
- 21 November 2018, p. 89
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: Background: Annually, 2.5 million traumatic brain injuries (TBI) occur with nearly 75% classified as mild TBI (mTBI), also known as a concussion. Mild TBI can be subtle and detection requires a high index of suspicion and a regimented evaluation process. This study was done to define the proportion of patients with a possible mTBI evaluated for concussion at a high volume urban trauma center. METHODS/STUDY POPULATION: Methods: A prospective cohort of patients was identified using a 3-question screen at the time of triage: did an injury occur; was the mechanism consistent with mTBI; was there a period of altered mental status. Patients who screened positive were thought to meet a minimum threshold for the evaluation of mTBI. Information about mTBI specific evaluation, management, and education was obtained from the patient’s charts. RESULTS/ANTICIPATED RESULTS: Results: 38,484 patients were screened over 16 weeks, of whom 453 (1.18%) screened positive for a possible mTBI and did not meet exclusion criteria. In total, 198 patients had documented loss of consciousness, 101 were diagnosed with mTBI, and 49 received mTBI discharge instructions. Overall, 32.5% of included patients had mTBI listed in the differential or as a diagnosis and 32.3% with loss of consciousness received a mTBI diagnosis. DISCUSSION/SIGNIFICANCE OF IMPACT: Conclusions: Many patients with a possible mTBI were not evaluated, managed, or educated for their potential injury. Changes in physicians’ approach to mTBI must occur to increase the proportion of patients receiving appropriate evaluation, management, and education. These results define the current reality of mTBI treatment in the Emergency Department and show the need for further experimental studies targeted at physician decision support interventions to improve mTBI care.




