2 results
Lessons from an evaluation of an antimicrobial resistance laboratory capacity telementoring program in Ethiopia and Kenya
- Kieran Hartsough, Jacqueline Safstrom, Martin Evans, Manise Pierre, Edward Schroder, Carolyn Herzig, Ana Da Costa, Susan Githii, Rajiha Abubeker, Gebrie Alebachew, Surafel Fentaw Dinku, Abera Abdeta, Estifanos Tsige, Maritza Urrego
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s123
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antimicrobial resistance (AMR) presents a global health threat. Training laboratory technicians to accurately identify and report AMR is critical in low- and middle-income countries (LMICs) to control the spread of AMR. Ethiopia and Kenya implemented a telementoring program, ECHO AMR, via the Project ECHO learning platform to improve laboratory technician capacity to isolate, identify, and report AMR organisms; to perform antimicrobial susceptibility testing (AST); and to develop a community of learning. Between January 2018 and January 2022, biweekly 1-hour sessions were held for 8 and 22 laboratories averaging 19 or 43 participants per session in Ethiopia and Kenya, respectively. Each session included a lecture, a laboratory challenge case presentation, and discussion. An evaluation was conducted to assess perceived strengths and weaknesses of the program and its usefulness in improving bacteriology capacity. Methods: In July–August 2022, semistructured key informant interviews of purposively and randomly selected laboratorians were conducted to understand participant perspectives of ECHO AMR, including session structure and content, changes in laboratory performance, and the virtual learning platform. Eligible participants attended at least one-third of available sessions in Ethiopia (8 of 26 sessions) or Kenya (5 of 16 sessions) during 2021. Key informant interviews were transcribed and systematically reviewed to identify key themes. Results: In total, 22 laboratory technicians participated in the key informant interviews: 12 in Ethiopia and 10 in Kenya. Participants reported that the ECHO AMR session structure was well organized but recommended increasing session duration to allow more time for discussion. Technical content was presented at an appropriate level and was highly rated. However, participants suggested including more subject-matter experts to provide the lectures. All participants reported positive change in laboratory practice, including implementation of international standards for AST, better quality control, improved confidence and critical thinking, and increased AMR awareness and reporting. Participants learned well in the virtual environment, with the platform providing wide-ranging geographic interactions to share skills and knowledge among sites without travel. However, there were connectivity issues, competing work priorities during sessions, and a lack of dedicated space for team participation. Conclusions: Laboratory technicians reported that virtual laboratory training was well-received, efficient, and impactful. Participants benefited both individually and collectively, as a laboratory. Suggested improvements included increasing session duration, connectivity support, and including more subject-matter experts to broaden technical content. Further assessment is needed to evaluate the ECHO AMR’s impact on laboratory practices through observation and laboratory data. Virtual programs, requiring less time and resources than traditional in-country trainings, can be optimized and used to share and increase bacteriology knowledge in LMICs.
Disclosures: None
Readiness assessment: Implications for COVID-19 infection prevention and control (IPC) preparedness in health facilities
- Evelyn Wesangula, Veronica Kamau, Felister Kiberenge, Emmanuel Tanui, Susan Githii, Linus Ndegwa, George Owiso, Irungu Kamau, Jennifer Njuhigu
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s79-s80
-
- Article
-
- You have access Access
- Open access
- Export citation
-
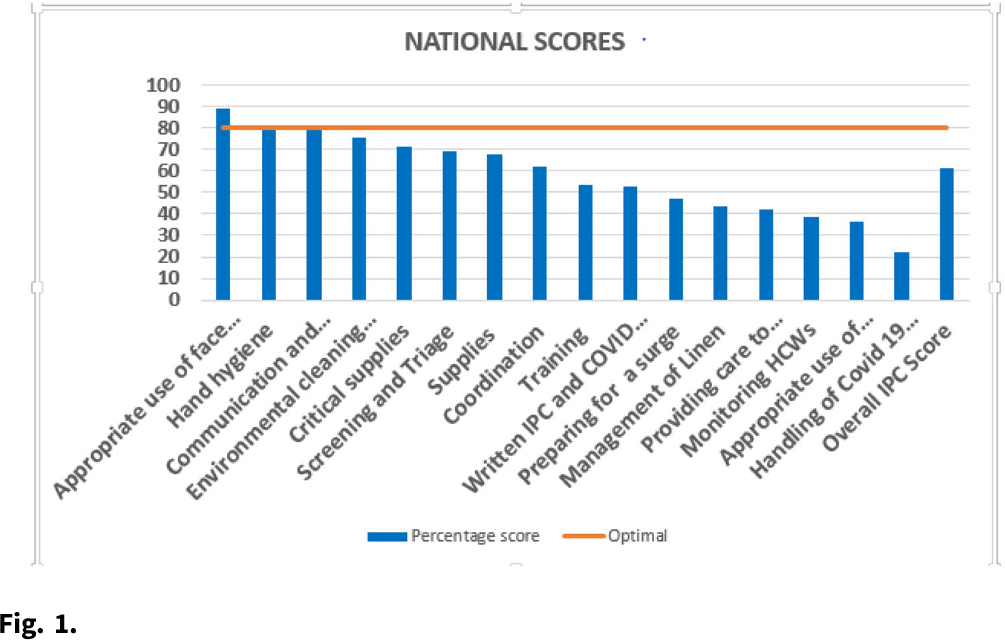
Background: Monitoring uptake of infection prevention and control (IPC) interventions is critical for the targeted and rational use of limited resources. A national facility readiness assessment conducted in August 2020 provided key information for targeted interventions to strengthen priority IPC areas. We assessed the level of COVID-19 preparedness in the facilities, identified priority COVID-19 IPC gaps, and generated a baseline report to further guide IPC investments at all levels. Methods: The Kenya Ministry of Health in collaboration with the CDC and International Training and Education Center for Health adapted a WHO Facility Readiness Assessment tool to include COVID-19–specific areas. In August 2020, data were collected using tablets through an Android-based electronic platform and were analyzed using descriptive statistics. Assessments were conducted in public, private, and faith-based health facilities nationally after 4 months of preparedness and investment in the healthcare system. Results: We assessed 684 facilities of the targeted 844 (81%). Overall facility readiness in Kenya was rated above average (61%), and the performance score significantly increased with the Kenya Essential Package for Health level, with level 5 and 6 facilities scoring an average of 83% and 79% respectively. Of the assessed facilities, 82% had an appointed IPC coordinator. Only 14% of the facilities had all the required guidelines, policies, and the appropriate COVID-19 case definitions. 67% of the facilities had updated supply inventories for past week. Only 50% of the facilities had adequate supplies of N95 masks. The assessment revealed that 52% of healthcare facilities had trained their healthcare workforce; morticians were the least trained (only 17% of facilities). Moreover, 41% of the facilities had clear work plans for monitoring healthcare workers exposures to COVID-19, but only 33% of the facilities had policies on the management of infected healthcare workers. Conclusions: The findings provided critical information for stakeholders at all levels to be used for policy decisions, to prioritize key intervention areas in leadership and governance of facility IPC programs, for guideline development, and for capacity building and targeted investment in IPC to improve COVID-19 facility preparedness.
Funding: None
Disclosures: None