5 results
Outpatient treatment and clinical outcomes of bacteriuria in veterans: A retrospective cohort analysis
- Suzette A. Rovelsky, Michelle Vu, Alexis K. Barrett, Kenneth Bukowski, Xiangming Wei, Muriel Burk, Makoto Jones, Kelly Echevarria, Katie J Suda, Francesca Cunningham, Karl J Madaras-Kelly, for the UTI Management Improvement Group
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 12 October 2022, e168
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To conduct a contemporary detailed assessment of outpatient antibiotic prescribing and outcomes for positive urine cultures in a mixed-sex cohort.
Design:Multicenter retrospective cohort review.
Setting:The study was conducted using data from 31 Veterans’ Affairs medical centers.
Patients:Outpatient adults with positive urine cultures.
Methods:From 2016 to 2019, data were extracted through a nationwide database and manual chart review. Positive urine cultures were reviewed at the chart, clinician, and aggregate levels. Cases were classified as cystitis, pyelonephritis, or asymptomatic bacteriuria (ASB) based upon documented signs and symptoms. Preferred therapy definitions were applied for subdiagnoses: ASB (no antibiotics), cystitis (trimethoprim-sulfamethoxazole, nitrofurantoin, β-lactams), and pyelonephritis (trimethoprim-sulfamethoxazole, fluoroquinolone). Outcomes included 30-day clinical failure or hospitalization. Odds ratios for outcomes between treatments were estimated using logistic regression.
Results:Of 3,255 cases reviewed, ASB was identified in 1,628 cases (50%), cystitis was identified in 1,156 cases (36%), and pyelonephritis was identified in 471 cases (15%). Of all 2,831 cases, 1,298 (46%) received preferred therapy selection and duration for cases where it could be defined. The most common antibiotic class prescribed was a fluoroquinolone (34%). Patients prescribed preferred therapy had lower odds of clinical failure: preferred (8%) versus nonpreferred (10%) (unadjusted OR, 0.74; 95% confidence interval [CI], 0.58–0.95; P = .018). They also had lower odds of 30-day hospitalization: preferred therapy (3%) versus nonpreferred therapy (5%) (unadjusted OR, 0.55; 95% CI, 0.37–0.81; P = .002). Odds of clinical treatment failure or hospitalization was higher for β-lactams relative to ciprofloxacin (unadjusted OR, 1.89; 95% CI, 1.23–2.90; P = .002).
Conclusions:Clinicians prescribed preferred therapy 46% of the time. Those prescribed preferred therapy had lower odds of clinical failure and of being hospitalized.
Implementation and outcomes of a clinician-directed intervention to improve antibiotic prescribing for acute respiratory tract infections within the Veterans’ Affairs Healthcare System
- Karl J. Madaras-Kelly, Suzette A. Rovelsky, Robert A. McKie, McKenna R. Nevers, Jian Ying, Benjamin A. Haaland, Chad L. Kay, Melissa L. Christopher, Lauri A. Hicks, Mathew H. Samore
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 5 / May 2023
- Published online by Cambridge University Press:
- 15 August 2022, pp. 746-754
- Print publication:
- May 2023
-
- Article
- Export citation
-
Objective:
To determine whether a clinician-directed acute respiratory tract infection (ARI) intervention was associated with improved antibiotic prescribing and patient outcomes across a large US healthcare system.
Design:Multicenter retrospective quasi-experimental analysis of outpatient visits with a diagnosis of uncomplicated ARI over a 7-year period.
Participants:Outpatients with ARI diagnoses: sinusitis, pharyngitis, bronchitis, and unspecified upper respiratory tract infection (URI-NOS). Outpatients with concurrent infection or select comorbid conditions were excluded.
Intervention(s):Audit and feedback with peer comparison of antibiotic prescribing rates and academic detailing of clinicians with frequent ARI visits. Antimicrobial stewards and academic detailing personnel delivered the intervention; facility and clinician participation were voluntary.
Measure(s):We calculated the probability to receive antibiotics for an ARI before and after implementation. Secondary outcomes included probability for a return clinic visits or infection-related hospitalization, before and after implementation. Intervention effects were assessed with logistic generalized estimating equation models. Facility participation was tracked, and results were stratified by quartile of facility intervention intensity.
Results:We reviewed 1,003,509 and 323,023 uncomplicated ARI visits before and after the implementation of the intervention, respectively. The probability to receive antibiotics for ARI decreased after implementation (odds ratio [OR], 0.82; 95% confidence interval [CI], 0.78–0.86). Facilities with the highest quartile of intervention intensity demonstrated larger reductions in antibiotic prescribing (OR, 0.69; 95% CI, 0.59–0.80) compared to nonparticipating facilities (OR, 0.89; 95% CI, 0.73–1.09). Return visits (OR, 1.00; 95% CI, 0.94–1.07) and infection-related hospitalizations (OR, 1.21; 95% CI, 0.92–1.59) were not different before and after implementation within facilities that performed intensive implementation.
Conclusions:Implementation of a nationwide ARI management intervention (ie, audit and feedback with academic detailing) was associated with improved ARI management in an intervention intensity–dependent manner. No impact on ARI-related clinical outcomes was observed.
Tier-based antimicrobial stewardship metrics for genitourinary-related antibiotic use in Veterans’ Affairs outpatient settings
- Matthew Samore, Matthew Goetz, McKenna Nevers, Jacob Crook, Suzette Rovelsky, Ben Brintz, Kelly Echevarria, Melinda Neuhauser, Sharon Tsay, Lauri Hicks, Karl Madaras-Kelly
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s5-s6
-
- Article
-
- You have access Access
- Open access
- Export citation
-
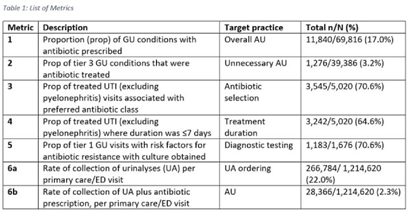
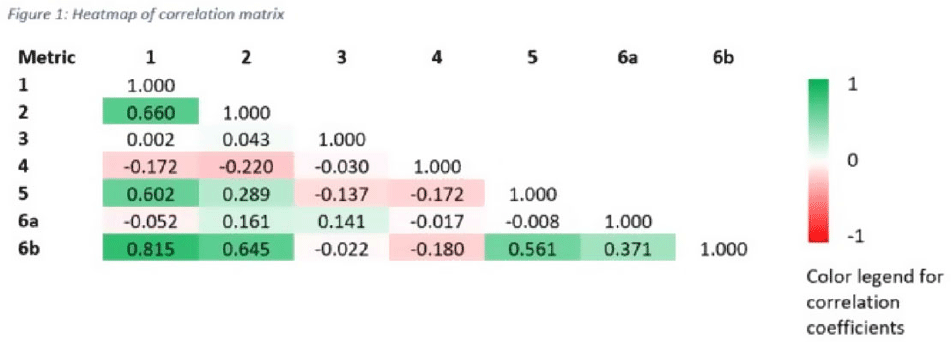
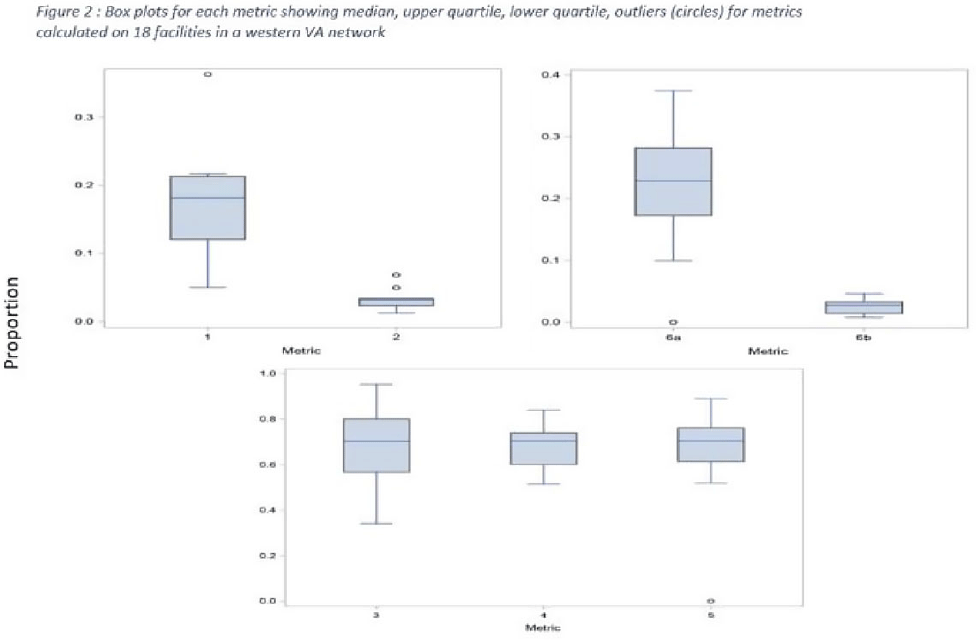
Background: Tracking antibiotic use is a core element of antimicrobial stewardship. We developed a set of metrics based on electronic health record data to support an outpatient stewardship initiative to improve management of urinary tract infections (UTIs) in Veterans’ Affairs (VA) emergency departments (EDs) and primary care clinics. Because UTI diagnostic codes only capture a portion of genitourinary (GU)-related antibiotic use, a tier-based approach was used to evaluate practices. Methods: Metrics were developed to target practices related to antibiotic prescribing and diagnostic testing (Table 1). GU conditions were divided into 3 categories: tier 1, conditions for which antibiotics are usually or always indicated; tier 2, conditions for which antibiotics are sometimes indicated; and tier 3, conditions for which antibiotics are rarely or never indicated (eg, benign prostatic hypertrophy with symptoms). Patients with visits related to urological procedures, nontarget providers, and concomitant non-GU infections were excluded. Descriptive analyses included calculation of the correlation matrix for the 7 metrics and the construction of box plots to display interfacility variability. Results: Metrics were calculated quarterly for 18 VA medical centers, including affiliated clinics, in a western VA network, from July 2018 to June 2020 (Table 1). Tier 3 GU conditions accounted for 1,276 of 11,840 (11%) of GU-related antibiotic use. Metrics 1 and 6b were strongly correlated with each other and were also positively correlated with metrics 2 and 5 (coefficients > 0.5) (Fig. 1). Substantial interfacility variation was observed (Fig. 2). Conclusions: Stewardship metrics for suspected or documented UTIs can identify opportunities for practice improvement. Broadly capturing GU conditions in addition to UTIs may enhance utility for performance feedback. Antibiotic prescribing for tier 3 GU conditions is analogous to unnecessary antibiotic use for acute, uncomplicated bronchitis and upper respiratory tract infections.
Funding: None
Disclosures: None
Increased Return Clinic Visits for Adults with Group A Streptococcal Pharyngitis Treated with a Macrolide
- Suzette Rovelsky, Benjamin Pontefract, McKenna Nevers, Adam Hersh, Matthew Samore, Karl Madaras-Kelly
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s295-s296
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: A multicenter audit-and-feedback intervention was conducted to improve management of acute respiratory infections (ARIs) including group A streptococcal (GAS) pharyngitis within 6 VA medical Centers (VAMCs). A relative reduction (24.8%) in azithromycin prescribing after the intervention was observed. Within these facilities during 2015–2018, 2,266 cases of GAS occurred, and susceptibility to erythromycin ranged from 55% to 70%. We evaluated whether prescribing a macrolide for GAS pharyngitis was associated with an increase in outpatient return visits. Methods: A cohort of ambulatory adults treated for GAS pharyngitis (years 2014–2019) at 6 VAMCs was created. Demographic, diagnostic, treatment, and revisit data were extracted from the Corporate Data Warehouse. GAS pharyngitis was defined by an acute pharyngitis diagnostic code combined with a GAS-positive rapid strep test or throat culture ≤3 days of index date. Antibiotic prescriptions were included if filled ≤3 days of index date and were classified as first line (penicillin/amoxicillin), second line (cephalexin/clindamycin), macrolides (azithromycin, clarithromycin, erythromycin), or other (remaining antibiotics). A return visit was defined as a new visit to primary care, urgent care, or the emergency department with a diagnostic code for an ARI ≤30 days from the index visit. Logistic regression was used to adjust for nonantibiotic covariates and to compare treatments. Results are reported as odds ratio (OR ± 95% CI; P value). Results: Of 12,666 patients with a diagnostic code for acute pharyngitis, 2,923 (23.1%) had GAS testing performed. Of those, 582 (19.9%) were GAS-positive and 460 (15.7%) received antibiotics. The mean age was 39.0 years (±SD, 11.7) and 73.7% were male. Antibiotics included penicillins for 363 patients (78.9%), cephalosporins for 21 (4.6%), clindamycin for 32 (7.0%), macrolides for 47 (10.2%), and other for 17 (3.9%). Penicillin allergy was documented in 48 patients (10.5%), and these patients received cephalosporins (18.8%), clindamycin (35.4%), macrolides (41.7%), and other antibiotics (4.2%). Return visits occurred in 47 cases (10.4%). Limited chart review indicated that 6 of 10 macrolide recipients (60.0%) with return visits had recurrence or unresolved symptoms. After adjustment for calendar month and facility, odds of a return visit for treatment with a macrolide relative to penicillins was 2.79 (OR, 1.19; 95% CI, ±6.56; P = .02). The audit-feedback intervention was not associated with ARI-related return visits (OR, 0.53; 95% CI, 0.26–1.06; P = .07). Conclusions: Return visit rates were higher for GAS pharyngitis patients treated with a macrolide than for those treated with penicillins. Macrolides were the most commonly prescribed non-penicillin therapy irrespective of penicillin allergy. Further work is necessary to determine the reason for the increase in return visits.
Funding: None
Disclosures: None
Update on Improving Outpatient Antibiotic Use Through Implementation and Evaluation of Core Elements of Outpatient Antibiotic
- Karl Madaras-Kelly, Christopher Hostler, Mary Townsend, Emily Potter, Emily Spivak, Sarah Hall, Matthew Goetz, McKenna Nevers, Jian Ying, Benjamin Haaland, Suzette Rovelsky, Benjamin Pontefract, Katherine Fleming-Dutra, Matthew Samore
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s422
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Acute respiratory infections (ARIs) are a key target to improve antibiotic use in the outpatient setting. The Core Elements of Outpatient Antibiotic Stewardship provide a framework for improving antibiotic use, but data on safety and effectiveness of interventions to improve antibiotic use are limited. We report the impact of Core Elements implementation within Veterans’ Healthcare Administration clinics on antibiotic prescribing and patient outcomes. Methods: The intervention targeting treatment of uncomplicated ARIs (sinusitis, pharyngitis, bronchitis, and viral upper respiratory infections [URIs]) in emergency department and primary care settings was initiated within 10 sites between September 2017 and January 2018. The intervention was developed using the Core Elements and included local site champions, audit-and-feedback with peer comparison, and academic detailing. We evaluated the following outcomes: per-visit antibiotic prescribing rates overall and by diagnosis; appropriateness of treatment; 30-day ARI revisits; 30-day infectious complications (eg,, pneumonia,); 30-day adverse medication effects; 90-day Clostridium difficile infection (CDI); and 30-day hospitalizations. Multilevel logistic regression was used to calculate rate ratios (RR) with 95% CI for each outcome in the postintervention period (12 months) compared to the preintervention period (39–42 months). Results: There were 14,020 uncomplicated ARI visits before the intervention and 4,866 uncomplicated ARI visits after the intervention. The proportions of uncomplicated ARI visits with antibiotics prescribed were 59.17% before the intervention versus 44.34% after the intervention. A trend in reduced antibiotic prescribing for ARIs throughout the entire (before and after) observation period was evident (0.92; 95% CI, 0.90–0.94); however, a significant reduction in antibiotic prescribing after the intervention was identified (0.74; 95% CI, 0.59–0.93). Per-visit antibiotic prescribing rates decreased significantly for bronchitis and URI (0.54; 95% CI, 0.44–0.65), pharyngitis (0.76; 95% CI, 0.67–0.86), and sinusitis (0.92; 95% CI, 0.85–1.0). Appropriate therapy for pharyngitis increased (1.43; 95% CI, 1.21–1.68), but appropriate therapy for sinusitis remained unchanged (0.92; 95% CI, 0.85–1.0) after the intervention. Complications associated with antibiotic undertreatment were not different after the intervention: ARI-related revisit rates (1.01; 95% CI, 0.98–1.05) and infectious complications (1.01; 95% CI, 0.79–1.28). A potential benefit of improved antibiotic use included a reduction in visits for adverse medication effects (0.82; 95% CI, 0.72–0.94). Furthermore, 90-day CDI events were too sparse to model: preintervention incidence was 0.08% and postintervention incidence was 0.06%. Additionally, 30-day hospitalizations were significantly lower in the postintervention period (0.79; 95% CI, 0.72–0.87). Conclusions: Implementation of the Core Elements was safe and effective and was associated with reduced antibiotic prescribing rates for uncomplicated ARIs, improvements in diagnosis-specific appropriate therapy, visits for adverse antibiotic effects, and 30-day hospitalization rates. No adverse events were noted in ARI-related revisit rates or infectious complications. CDI rates were low and unchanged.
Funding: None
Disclosures: None






