6 results
Regional impact of multidrug-resistant organism prevention bundles implemented by facility type: A modeling study
- Samuel E. Cincotta, Maroya S. Walters, D. Cal Ham, Rany Octaria, Jessica M. Healy, Rachel B. Slayton, Prabasaj Paul
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 28 February 2024, pp. 1-8
-
- Article
- Export citation
-
Background:
Emerging multidrug-resistant organisms (MDROs), such as carbapenem-resistant Enterobacterales (CRE), can spread rapidly in a region. Facilities that care for high-acuity patients with longer stays may have a disproportionate impact on this spread.
Objective:We assessed the impact of implementing preventive interventions, directed at a subset of facilities, on regional prevalence.
Methods:We developed a deterministic compartmental model, parametrized using CRE and patient transfer data. The model included the community and healthcare facilities within a US state. Individuals may be either susceptible or infectious with CRE. Individuals determined to be infectious through admission screening, periodic prevalence surveys (PPSs), or interfacility communication were placed in a state of lower transmissibility if enhanced infection prevention and control (IPC) practices were in place at a facility.
Results:Intervention bundles that included PPS and enhanced IPC practices at ventilator-capable skilled nursing facilities (vSNFs) and long-term acute-care hospitals (LTACHs) had the greatest impact on regional prevalence. The benefits of including targeted admission screening in acute-care hospitals, LTACHs, and vSNFs, and improved interfacility communication were more modest. Daily transmissions in each facility type were reduced following the implementation of interventions primarily focused at LTACHs and vSNFs.
Conclusions:Our model suggests that interventions that include screening to limit unrecognized MDRO introduction to, or dispersal from, LTACHs and vSNFs slow regional spread. Interventions that pair detection and enhanced IPC practices within LTACHs and vSNFs may substantially reduce the regional burden.
An interactive patient transfer network and model visualization tool for multidrug-resistant organism prevention strategies
- Rany Octaria, Samuel Cincotta, Jessica Healy, Camden Gowler, Prabasaj Paul, Maroya Walters, Rachel Slayton
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s120-s122
-
- Article
-
- You have access Access
- Open access
- Export citation
-
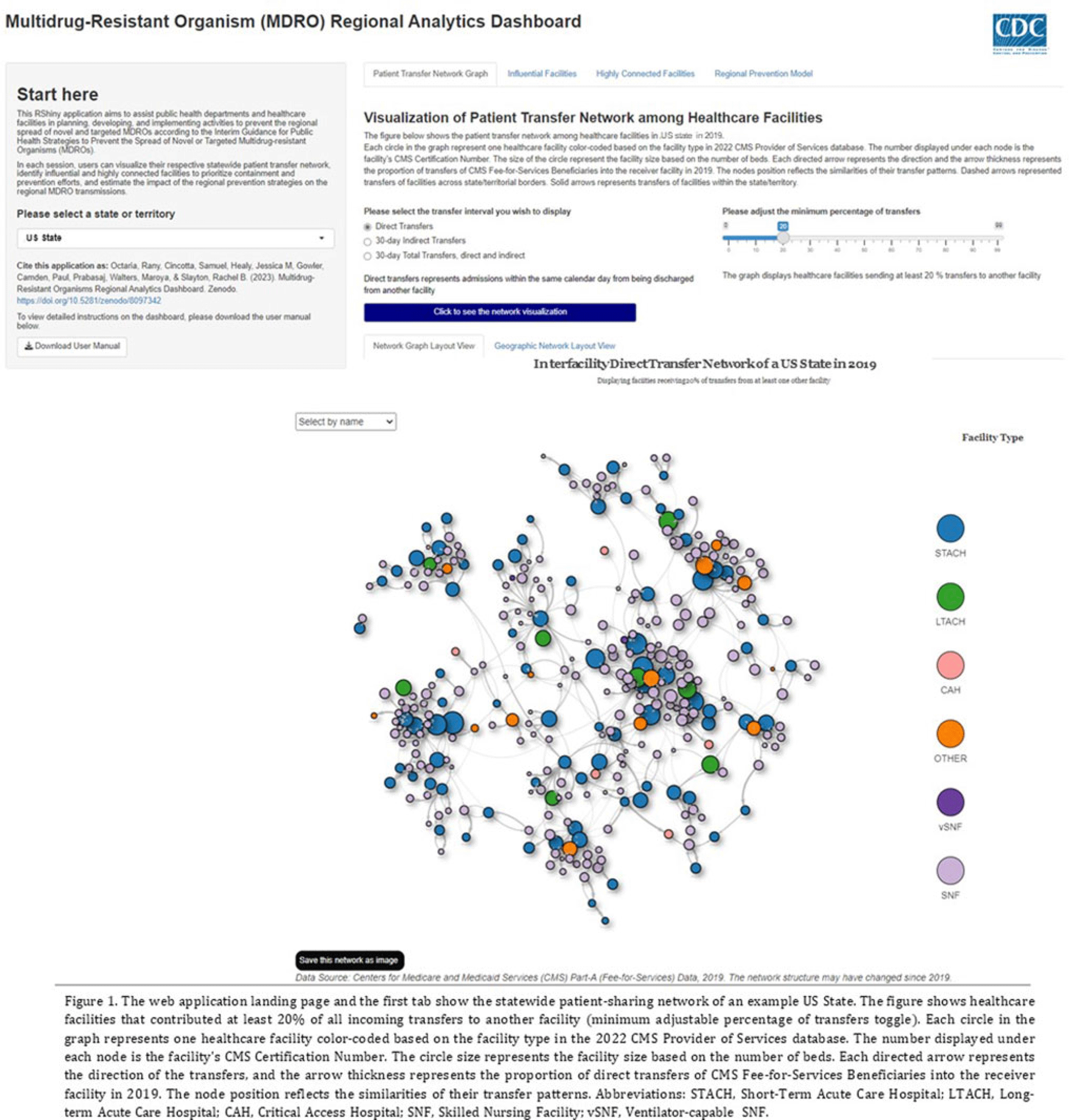
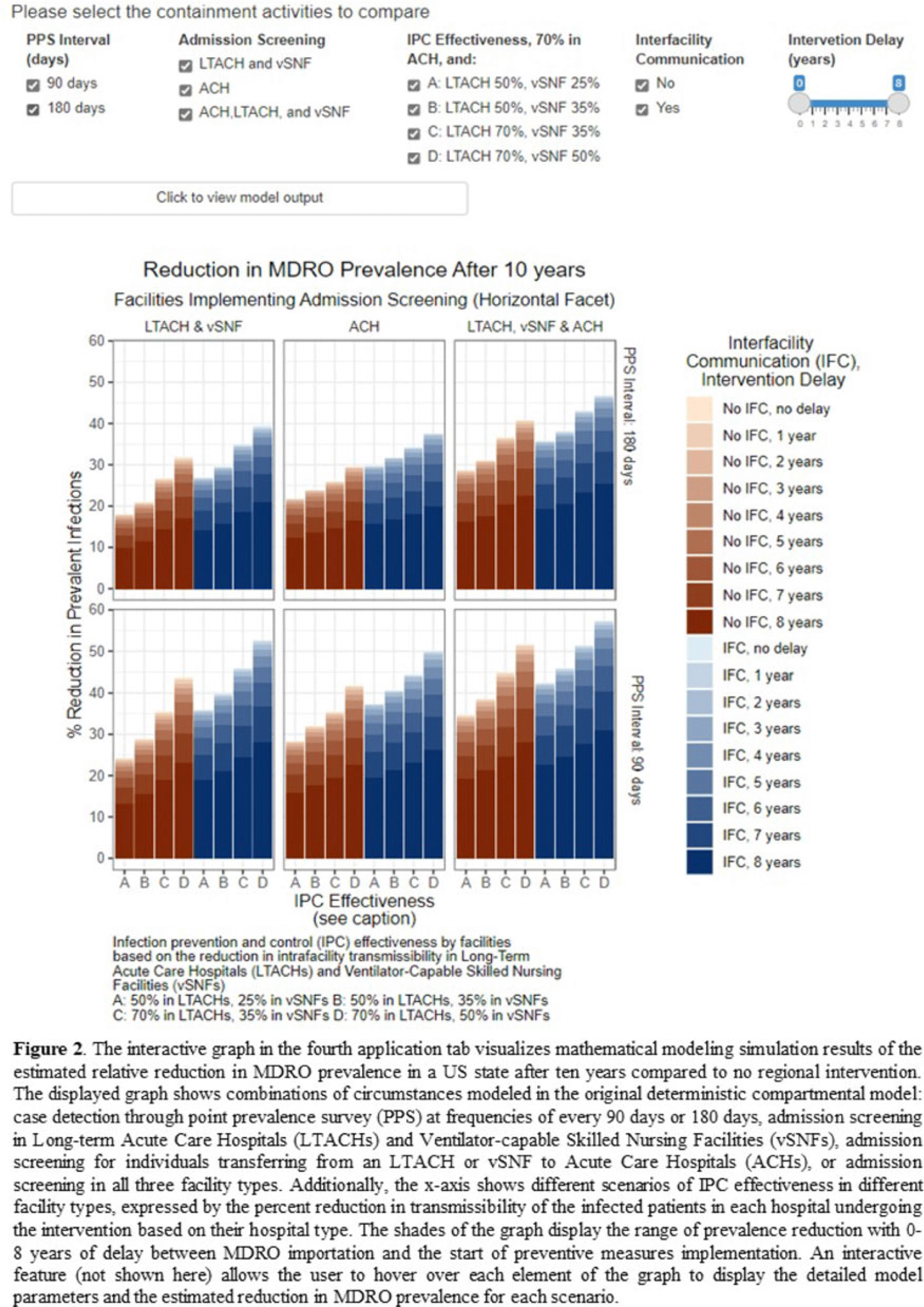
Background: The CDC’s new Public Health Strategies to Prevent the Spread of Novel and Targeted Multidrug-Resistant Organisms (MDROs) were informed by mathematical models that assessed the impact of implementing preventive strategies directed at a subset of healthcare facilities characterized as influential or highly connected based on their predicted role in the regional spread of MDROs. We developed an interactive tool to communicate mathematical modeling results and visualize the regional patient transfer network for public health departments and healthcare facilities to assist in planning and implementing prevention strategies. Methods: An interactive RShiny application is currently hosted in the CDC network and is accessible to external partners through the Secure Access Management Services (SAMS). Patient transfer volumes (direct and indirect, that is, with up to 30 days in the community between admissions) were estimated from the CMS fee-for-service claims data from 2019. The spread of a carbapenem-resistant Enterobacterales (CRE)–like MDROs within a US state was simulated using a deterministic model with susceptible and infectious compartments in the community and healthcare facilities interconnected through patient transfers. Individuals determined to be infectious through admission screening, point-prevalence surveys (PPSs), or notified from interfacility communication were assigned lower transmissibility if enhanced infection prevention and control practices were in place at a facility. Results: The application consists of 4 interactive tabs. Users can visualize the statewide patient-sharing network for any US state and select territories in the first tab (Fig. 1). A feature allows users to highlight a facility of interest and display downstream or upstream facilities that received or sent transfers from the facility of interest, respectively. A second tab lists influential facilities to aid in prioritizing screening and prevention activities. A third tab lists all facilities in the state in descending order of their dispersal rate (ie, the rate at which patients are shared downstream to other facilities), which can help identify highly connected facilities. In the fourth tab, an interactive graph displays the predicted reduction of MDRO prevalence given a range of intervention scenarios (Fig. 2). Conclusions: Our RShiny application, which can be accessed by public health partners, can assist healthcare facilities and public health departments in planning and tailoring MDRO prevention activity bundles.
Disclosures: None
Mortality rates among non-Hispanic Black and White persons in carbapenemase-producing Enterobacterales, Tennessee, 2015–2019
- Erika Kirtz, Rany Octaria, Carolyn Stover, Christopher Wilson, Allison Chan
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s64-s65
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Carbapenem-resistant Enterobacterales (CRE) are an urgent public health threat, particularly those that produce carbapenemase (CP-CRE). Certain risk factors associated with CRE acquisition have been well described, such as older age, indwelling devices, prior hospitalizations, and underlying conditions. However, data are limited regarding the association of CRE and health disparities, such as race and ethnicity. Published literature has consistently shown that minority groups, including but not limited to Non-Hispanic Black persons, have higher risks of developing adverse health outcomes. To better understand the impact of race and ethnicity in CP-CRE cases, we compared 1-year mortality rates among Non-Hispanic Blacks and Non-Hispanic Whites. Methods: CRE are reportable in Tennessee; isolates must be sent to the State Public Health Laboratory for carbapenemase detection and resistance mechanism testing. We linked 2015–2019 CP-CRE surveillance cases and laboratory data from our statewide surveillance system, the National Disease Surveillance System (NEDDS)-Base System, with the Tennessee Hospital Discharge Data System (HDDS) and vital records databases. Database linkage and data analyses were performed using SAS version 9.4 software. Results: Among 615 CP-CRE cases, the mean age was lower among non-Hispanic Blacks (59 years; SD, 16.6) compared to non-Hispanic Whites (mean, 65 years; SD, 15.7). Among 156 non-Hispanic Blacks with CP-CRE, 101 (64.7%) were nursing home residents, whereas 281 (71.1%) among the 395 non-Hispanic Whites were nursing home residents. Also, 64 Non-Hispanic Blacks (41%) died within 1 year of their first specimen collection date compared to 92 Non-Hispanic Whites (23.3%). Non-Hispanic Blacks with CP-CRE who died within 1 year had a mortality rate of 5.6 per 100,000 (95% CI, 4.21–6.94) Black population, which was 1.6 times higher than Non-Hispanic White persons at 3.5 per 100,000 (95% CI, 2.94–3.95; χ2P < .001) White population. Conclusions: Despite a lower mean age, non-Hispanic Black CP-CRE cases had a higher 1-year mortality rate than non-Hispanic Whites. Racial and ethnicity data often are missing or incomplete from surveillance data. Data linkages can be a valuable tool to gather additional clinical and demographic data that may be missing from public health surveillance data to improve our understanding of health disparities. Recognition of these health disparities among CRE can provide an opportunity for public health to create more targeted interventions and educational outreach.
Funding: None
Disclosures: None
Characteristics of patients positive for COVID-19 and multidrug-resistant organisms in Tennessee, 2020–2021
- Carolyn Stover, Erin Hitchingham, Kristina McClanahan, Zoe Durand, Rany Octaria, Christopher Wilson, Allison Chan
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s80-s81
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Multidrug-resistant organisms (MDROs) are a global threat. To track and contain the spread, the Tennessee Department of Health (TDH) performs targeted surveillance of carbapenemase-producing and pan-nonsusceptible organisms. When these MDROs are identified, TDH conducts a containment response and collects epidemiological data, which includes risk factors such as indwelling devices and previous hospitalizations. The impact of the COVID-19 pandemic on these MDROs is not well understood. Therefore, we have described the characteristics of cases positive for both COVID-19 and select MDROs. Methods: MDRO investigation data from January 1, 2020–September 30, 2021 were matched with all COVID-19 case data from the TDH statewide surveillance system, National Electronic Disease Surveillance System Base System. MDRO-positive date was defined as the specimen collection date; COVID-19 case date was first defined as the date of symptom onset and if missing, then diagnosis date, and investigation creation date, respectively. Descriptive statistics and Fisher exact tests were calculated using SAS version 9.4 software. Results: Among 336 MDRO cases, 50 had a reported SARS-CoV-2–positive result. MDRO types were Enterobacterales (CRE) (n = 31), Acinetobacter spp (CRA) (n = 18), and Pseudomonas aeruginosa (n = 1). Of these 50 cases, 20 were MDRO-positive before and 30 days after the COVID-19 case date, respectively. Of the 18 CRA cases, 16 (89%), were positive after the COVID-19 case date, compared to 13 (42%) among 31 CRE cases (P < .01). Also, 35 patients (70%) had a record of hospitalization, and 22 (63%) had their MDRO specimen collected after the COVID-19 case date (P = .37). Of these 22 patients, 4 had their MDRO specimen collected during their COVID-19 hospitalization, with an average duration from admission to MDRO collection date of 17 days (range, 4–36). Among the 50 coinfected cases, 8 died, 7 (88%) of whom were MDRO-positive after their COVID-19 case date. Data on indwelling devices at time of MDRO positivity were completed for 17 cases; 14 had an indwelling device and, among these, 13 (93%) were MDRO-positive after their COVID-19 case date. Conclusions: MDRO cases with specimen collections after COVID-19 comprised the majority of hospitalized patients, patients who died, and patients with indwelling devices compared to those with MDROs collected before their COVID-19 case date. These results show a stark difference with CRA as the most common MDRO among post–COVID-19 cases. Our data were limited by reporting gaps. We recognize that patients can remain colonized with MDROs for lengthy durations, which could have result in undetected MDRO cases prior to the COVID-19 case date. More data and analyses are needed to make targeted public health recommendations. However, these findings highlight the burden of MDROs among COVID-19 cases. including adverse health outcomes.
Funding: None
Disclosures: None
Carbapenemase Production and Mortality Risk Among Carbapenem-Resistant Enterobacteriaceae Cases in Tennessee, United States
- Rany Octaria, Allison Chan, Marion Kainer
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s150-s151
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Carbapenem-resistant Enterobacteriaceae (CRE) are an urgent public health threat associated with poor patient outcomes. CRE that produce carbapenemase (CP-CRE) are of particular concern because the mechanism-conferring genes in plasmids can be transferred to other bacteria. CRE are reportable in Tennessee (TN); isolate submission is required for CP production and resistance mechanism testing. We aimed to compare patient characteristics and outcomes between CP-CRE and non–CP-CRE patients to guide potential public health interventions. Methods: A retrospective cohort study to compare 30-day mortality, and clinical characteristics of CP-CRE to non–CP-CRE patients was conducted. Laboratory data were gathered from CRE isolates of Tennessee residents from July 1, 2015, to June 30, 2018. The most recent Council of State and Territorial Epidemiologists CRE and CP-CRE case definition was used to confirm and classify cases. Healthcare exposures within 1 year prior to onset, demographic characteristics, and clinical characteristics were obtained by linking surveillance data with the inpatient and outpatient Tennessee hospital discharge data. Cases were also matched with Tennessee vital statistics data to determine all-cause 30-day mortality from the event date. We evaluated risk ratios of 30-day mortality with a multivariable regression model. Results: Among 1,034 CRE cases that had at least 1 isolate submitted to public health, 445 (43.0%) were CP-CRE and 589 (57.0%) were non–CP-CRE. Among CP-CRE isolates, the blaKPC gene was found in 434 (98.9%). CP-CRE cases were more likely to have isolates from normally sterile sites, to have an organism with elevated resistance to meropenem (minimum inhibitory concentration, >16 µg/mL), to have prior admission to a long-term acute-care hospital, and to live in a nursing home (all P < .001). Also, 77 CP-CRE cases (17.3%) and 56 non–CP-CRE cases (9.6%) died within 30 days of infection onset. The risk of 30-day mortality was 57% higher for CP-CRE (adjusted risk ratio, 1.57; 95% CI:, 1.10–2.23) compared to non–CP-CRE patients after adjusting for comorbidities, nursing home residence, and prior healthcare exposures. Conclusions: CP-CRE cases had poorer outcomes than non–CP-CRE cases. This may be related in part to a higher proportion of sterile site infections among CP-CRE cases; our study was underpowered to analyze this subpopulation of sterile site cases. We plan to continue monitoring and performing analyses as mortality and hospital discharge data from more recent years become available and as more cases accumulate.
Funding: None
Disclosures: None
Comparing Automated Cluster Detection Methods for Carbapenem-Resistant Enterobacteriaceae (CRE): Rule-Based Versus Statistical
- Rany Octaria, Hannah Griffith, Matthew Estes, Caleb Wiedeman, Allison Chan, Marion Kainer
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s27
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: The Tennessee (TN) Department of Health (TDH) has been identifying clusters of reportable conditions using the Electronic Surveillance System for Early Notification of Community-Based Epidemics (ESSENCE), a cluster detection method using space-time scan permutation statistics based on patient ZIP code. CRE are reportable in Tennessee; isolate submission is required for carbapenemase (CP) production and resistance mechanism (eg, KPC gene) testing. The Council for Outbreak Response: Healthcare-Associated Infections (HAI) and Antimicrobial-Resistant (AR) Pathogens (CORHA) released proposed thresholds of reporting CRE to public health. Thresholds vary by healthcare facility type and regional epidemiology. The TDH HAI/AR program currently runs a daily automated SAS code using the CORHA reporting threshold to help public health identify suspect KPC clusters. We evaluated our rule-based CORHA method against 2 space-time statistic-based methods for KPC cluster detection in Tennessee. Methods: Simulations for each cluster detection method were performed using retrospective CP-CRE surveillance data for 2018. Simulations were conducted using (1) CORHA reporting thresholds by facility case count to flag clusters of 2 or more cases within 28 days, (2) ESSENCE using patient residence ZIP code and the earliest of collection date or symptom onset date as is used for other reportable conditions in Tennessee, and (3) a modified space-time statistical method using SaTScan in which reporting facility, rather than a geographic location, was used as space variable to detect within-facility clusters within 1–28 days. We compared the number and overlap of cases and clusters identified with each method. Univariate logistic regression with CORHA flagging as predictor and flagging by each ESSENCE or CORHA method as outcome variables, were used to compare cases tagged by each method pair, respectively. Results: Of 183 KPC CP-CRE cases, 54 (30.6%) were flagged as part of suspect clusters by at least 1 method. Simulations generated 16 alerts (36 cases) using CORHA, 10 clusters (25 cases) using modified SaTScan, and 10 clusters (20 cases) using standard ESSENCE protocol. Among KPC CP-CRE cases flagged by CORHA, 12 (33.3%) were also flagged by modified SaTScan and 2 (5%) by ESSENCE. A case flagged using CORHA method has 5.15 (95% CI, 2.10–12.64) times higher odds of also being flagged by the modified SaTScan method compared to cases not flagged by CORHA. Conclusions: An algorithm based on CORHA thresholds for reporting CRE to public health had strong agreement with modified SaTScan, a space-time method. We intend to explore the extension of the time interval for ESSENCE.
Funding: None
Disclosures: None





