The strong association between blood pressure (BP) and BMI has been well documented in various populations including adults and children( Reference Ma, Wang and Dong 1 – Reference Hvidt, Olsen and Ibsen 5 ). It was reported that an increase of 1 sd in BMI was associated with 2·63–3·70 mmHg increment of systolic blood pressure (SBP) in children( Reference Ma, Wang and Dong 1 ). Nowadays, along with the increasing trend of obesity worldwide( Reference Swinburn, Sacks and Hall 6 ), there is no surprise to see the rising prevalence of hypertension in adults and high BP in paediatric populations( Reference Ibrahim and Damasceno 7 , Reference Chockalingam, Campbell and Fodor 8 ). This situation is particularly marked in children of the biggest developing country, China. The prevalence of obesity of 7–18-year-old children increased thirty-eight times from 1985 to 2010( Reference Ma, Cai and Wang 9 ). Mirroring the obesity epidemic, the BP level among Chinese children has also increased substantially in recent years( Reference Dong, Wang and Wang 10 ).
Previous studies have explored potential mechanisms linking adiposity and high BP, including sympathetic nervous system activation, activation of the renin–angiotensin system, inflammatory responses and insulin resistance( Reference Rahmouni 11 ). However, few studies explored the influence of an unfavourable blood lipid profile. Obese adolescents with moderate and high SFA intake presented higher plasminogen activator inhibitor-1, an independent predictor of BP( Reference Masquio, de Piano and Campos 12 ), and reduction in SFA intake improves cardiovascular risks (mean BP and LDL-cholesterol decreased)( Reference Masquio, de Piano and Campos 13 ). Genetic studies have shown a clear association between dyslipidaemia and hypertension( Reference Selby, Newman and Quiroga 14 ), and the Physicians’ Health Study, a prospective study with a mean follow-up of 14·1 years, showed that men with the highest quintile of total cholesterol (TC), TC:HDL-cholesterol ratio and non-HDL-cholesterol had significantly increased risks of developing hypertension of 23, 54 and 39 %, respectively, and men with the highest quintile of HDL-cholesterol had a 32 % decreased risk of developing hypertension, which implies that dyslipidaemia may contribute to the subsequent development of hypertension( Reference Halperin, Sesso and Ma 15 ). Another prospective study in China aimed to investigate the risks of hypertension development in relation to the level of lipid variables among populations who had normal BP at baseline( Reference Guo, Hu and Wu 16 ).The study showed that dyslipidaemia might occur before hypertension, and hypertension was associated with HDL-cholesterol, TC:HDL-cholesterol and TAG( Reference Guo, Hu and Wu 16 ). Dyslipidaemia was reported as a cause of endothelial damage( Reference Nickenig 17 , Reference Nickenig and Harrison 18 ), and the loss of physiological vasomotor activity that results from endothelial damage may manifest as increased BP( Reference Halperin, Sesso and Ma 15 ). Consequently, an unfavourable blood lipid profile may mediate the association between obesity and BP.
However, this mediating effect of blood lipids has not been reported yet. In this study, we hypothesised that the association between obesity and hypertension is partially mediated by abnormal blood lipids. Therefore, in the present study, we evaluated not only the direct association between BMI and BP but also the mediation role of blood lipids in the association between BMI and BP. These results were presented by sex, when potential covariates were controlled.
Methods
Participants
Participants aged 7–18 years were recruited from ten primary schools (grade two to five), junior schools (grade seven and eight) and senior schools (grade eleven and twelve) in Chaoyang District, Beijing, China in 2012. On the basis of students’ medical history, children who reported a previous diagnosis of overt heart, renal, lung and liver diseases, asthma or physical/mental deformities were excluded( Reference Dong, Wang and Wang 19 ). As Asian populations and other populations, including blacks and Hispanics, may have different growth patterns and fat accumulations( Reference Rao, Powell-Wiley and Ancheta 20 ), the BMI references for screening Chinese Children with overweight and obesity were used in children in this study (online Supplementary Table S1)( Reference Ji 21 ).
In this study, 796 children (486 boys and 310 girls) identified as overweight or obese were recruited. We excluded fourteen participants with missing data on blood lipids (n 8) and BP (n 1), and five participants aged >18 years or <7 years. A total of 782 children aged 7–18 years with completed data were included in the final analysis.
The study was approved by the medical ethics committee of Peking University Health Science Center. Written informed consent was obtained from all children and their parents.
Measurements
Anthropometric measurements, including height, weight and BP, were taken according to standard protocols( Reference Dong, Wang and Wang 19 ). Weight was measured to the nearest 0·1 kg using a lever scale. Height was measured to the nearest 0·1 cm using a stadiometer. BMI was calculated as weight (kg) divided by height (m) squared (kg/m2). BP was measured according to the recommendation of the National High Blood Pressure Education Program Working Group in Children and Adolescents( 22 ) using standard clinical sphygmomanometer. BP measurements were taken 5 min after resting. The first and fifth Korotkoff sounds were used for SBP and DBP measurements. If the measured difference was >10 mmHg, measurement was repeated until the final two measures differed <10 mmHg, and the mean of the final two measures was used in analyses.
Venous blood samples were collected after 12 h of fasting. Metabolic indicators such as TAG, TC, LDL-cholesterol and HDL-cholesterol were measured using the Automatic biochemical analyzer (Roche Modular P800 ISE900; Hoffmann-La Roche Ltd).
Statistical analyses
Data were analysed with SPSS 17.0. General characteristics were described as mean values and standard deviations. Differences of general characteristics between groups were analysed by t test. Mediation analyses were conducted to analyse the mediation effect of blood lipids on the association between BMI and BP, according to the mediation theory developed by Baron & Kenny( Reference Baron and Kenny 23 ). The mediation analysis procedure is illustrated in Fig. 1. First, we used linear regression to analyse associations (total association, c) between independent variable and dependent variable. The associations (a) between independent variable and potential mediators were also assessed. Then, associations between potential mediators and dependent variables were examined (b) and controlled for independent variables (direct association, c′). Finally, if c, a and b were all statistically significant, we included the term of multiplying a and b (indirect association, a×b) as the mediation effect of potential mediator, and use Sobel test to examine its mediating effect on the association between independent variable and dependent variable( Reference Sobel 24 ). SPSS procedures provided by Andrew Hayes were performed for the mediation analyses( Reference Preacher and Hayes 25 ).

Fig. 1 Model of mediation analysis. First, we used linear regression to analyse associations (total association, c coefficient) between independent variable X (e.g. BMI) and dependent variable Y (e.g. SBP, DBP). We thereafter used linear regression to analyse associations (a coefficient) between independent variable X (e.g. BMI) and potential mediators M (e.g. TC, TAG, HDL-cholesterol and LDL-cholesterol). Then, associations between potential mediators M (e.g. TC, TAG, HDL-cholesterol and LDL-cholesterol) and dependent variable Y (e.g. SBP, DBP) were examined (b coefficient) and controlled for the independent variable X (direct association, c′ coefficient). Finally, if c, a and b coefficients were all statistically significant, then the mediation effect of potential mediator M on the association between independent variable X and dependent variable Y was examined by multiplying a and b (indirect association, a×b coefficient).
Results
Table 1 showed the general characteristics of these children, and the mean age was 11·58 years. The concentrations of DBP (71·43 mmHg, sd 10·81), TC (3·82 mmol/l, sd 0·74), TAG (0·87 mmol/l, sd 0·43), HDL-cholesterol (1·26 mmol/l, sd 0·33) and LDL-cholesterol (1·94 mmol/l, sd 0·58) were similar in boys and girls. However, boys had significantly higher BMI and SBP compared with girls (P=0·025 and 0·012, respectively).
Table 1 General characteristics of the study sample (Mean values and standard deviations)

SBP, systolic blood pressure; DBP, diastolic blood pressure; TC, total cholesterol.
Associations between BMI and blood pressure measures (total association, c)
Significant associations were found between BMI and SBP in both boys and girls, after adjusting for age (Table 2). The total associations (c) were 1·28 (95 % CI 1·01, 1·54, P<0·001) and 1·21 (95 % CI 0·83, 1·60, P<0·001) for boys and girls, respectively. Similarly, DBP was associated with BMI in both boys and girls, adjusted for age (Table 3). The corresponding total associations (c) for DBP were 0·74 (95 % CI 0·49, 0·96, P<0·001) and 0·88 for boys and girls, respectively (95 % CI 0·59, 1·16, P<0·001).
Table 2 Association between BMI, blood lipids and systolic blood pressure in childrenFootnote * (β-Coefficients with their standard errors)

SBP, systolic blood pressure; TC, total cholesterol; c, total association between the independent variables (e.g. BMI) and the outcome variable (e.g. SBP); a, association between the independent variable (e.g. BMI) and the potential mediator (e.g. TC, TAG, HDL-cholesterol and LDL-cholesterol); b, association between the potential mediator and the outcome variable was assessed, controlled for the independent variable.
* All the analyses were adjusted for age. Independent variable X=BMI, mediator M=TC/TAG/HDL-cholesterol/LDL-cholesterol for model 1/2/3/4, dependent variable Y=SBP.
Table 3 Association between BMI, blood lipids and diastolic blood pressure in childrenFootnote * (β-Coefficients with their standard errors)

DBP, diastolic blood pressure; TC, total cholesterol; c, total association between the independent variables (e.g. BMI) and the outcome variable (e.g. DBP); a, association between the independent variable (e.g. BMI) and the potential mediator (e.g. TC, TAG, HDL-cholesterol and LDL-cholesterol); b, association between the potential mediator and the outcome variable was assessed, controlled for the independent variable.
* All the analyses were adjusted for age. Independent variable X=BMI, mediator M=TC/TAG/HDL-cholesterol/LDL-cholesterol for model 1/2/3/4, dependent variable Y=DBP.
Associations between BMI and potential mediators (a)
Associations between blood lipids and BMI were illustrated in Table 2. In boys, higher BMI was significantly associated with the increased levels of TC, TAG and LDL-cholesterol (P<0·05), whereas higher HDL-cholesterol was correlated with lower BMI (P<0·0001). However, in girls, only TAG and HDL-cholesterol were significantly positively associated with BMI (P<0·0001).
Associations between potential mediators and blood pressure (b)
Tables 2 and 3 showed the associations between potential mediators (blood lipids) and BP, after controlling for age and BMI. The significant associations between blood lipid indexes and SBP/DBP were observed in boys (P<0·05), except for HDL-cholesterol. However, no significant associations were found between blood lipids and SBP/DBP in girls (P>0·05).
Mediation role of potential mediators (indirect association, a×b)
On the basis of the mediation theory of Baron & Kenny( Reference Baron and Kenny 23 ), a subsequent mediation analysis was conducted to investigate the mediation effect (indirect association, a×b) of blood lipid indexes, such as TC, TAG and LDL-cholesterol, on the association between BMI and BP in boys (Table 4). The direct association between BMI and BP (c′) was also presented. A weak, but significant, mediation effect of TAG on the relationship between BMI and SBP was detected (a×b), with the mediation effect of 0·106 (95 % CI 0·024, 0·188, P=0·012) and the ratio of mediation effect in total association of 8·29 %. In addition, a slight mediation effect of TAG was also identified for the association between BMI and DBP (mediation effect=0·093, 95 % CI 0·017, 0·169, P=0·018; the ratio of mediation effect in total association=12·53 %). In the association between BMI and DBP, about 7·75 % was mediated by LDL-cholesterol, with a mediation effect of 0·57 (95 % CI 0·0002, 0·1138, P=0·046).
Table 4 Mediation effect of blood lipids on the association between BMI and blood pressure in boys
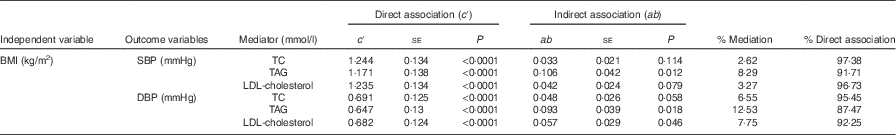
SBP, systolic blood pressure; DBP, diastolic blood pressure; TC, total cholesterol; c′, direct association between the independent variable and the outcome variable was determined; ab, indirect association between the independent variable and the outcome variable through the proposed mediator; % mediation, percentage mediation of the potential mediator (a×b/c).
In girls, as TC, TAG, HDL-cholesterol and LDL-cholesterol were no longer significantly associated with BP after BMI and age were adjusted, no significant mediation effect was detected (online Supplementary Table S2).
Direct association of BMI on blood pressure (direct association, c′)
As shown in Table 4, after potential mediator and age were adjusted for, the direct association between BMI and SBP was weak, but still significant. When TAG and age were adjusted for, the association between BMI and SBP changed from 1·277 to 1·171 (P<0·0001) in boys, excluding the mediation effect of TAG; the direct association between BMI and SBP was as large as 91·7 % of the total association. The corresponding direct association between BMI and DBP was 0·647 (P<0·0001), which explained 87·5 % of the total association. When the mediation effect of LDL-cholesterol and age was adjusted, the association between BMI and BP was mainly explained by the direct association (92·3 % of the total association).
Discussion
Our study confirmed that high BMI was associated with elevated BP. When adjusting for BMI, TC, TAG and LDL-cholesterol were associated with SBP in boys, whereas no significant association was detected in girls. Similar results were also found for DBP. Furthermore, in boys with overweight and obesity, TAG partially mediated the relationship between BMI and SBP, whereas TAG and LDL-cholesterol partially mediated the relationship between BMI and DBP. No mediation effect was identified in girls.
Our data suggested a strong crude linear association between BMI and BP measures, and an increase of one unit BMI was directly related to an about 1·2 mmHg increment in SBP and a 0·7–0·9 mmHg increment in DBP. Ma et al. ( Reference Ma, Wang and Dong 26 ) reported that SBP increased 3·70 and 2·63 mmHg in Chinese boys and girls, with a 1 sd increase in BMI (approximately 2–3 kg/m2 in 7–18-year-old girls and boys). Correia-Costa et al. ( Reference Correia-Costa, Santos and Severo 27 ) showed that SBP increased with BMI by 3·2 and 2·6 mmHg/sd of BMI Z-score, in 4-year-old girls and boys, respectively. Consistent with these studies, our study confirmed the significant association between BMI and BP in children. Moreover, we further showed that the association between BMI and BP remains significant even after excluding the indirect association of lipid profile.
Several studies have demonstrated the link between BP and serum lipids in adults, but few studies were conducted in children. Our data suggested that there was a sexual difference in the association between blood lipids and BP. Previous studies showed that TAG was associated with BP/hypertension( Reference Hunt, Stephenson and Hopkins 28 , Reference Haffner, Miettinen and Gaskill 29 ). Our study revealed that in boys, but not in girls, the significant associations of TC, TAG and LDL-cholesterol on SBP/DBP were detected after adjusting for BMI and age. This sexual dimorphism in the association between lipids and BP might be related to the different impacts of sex steroids on the regulation of serum lipoproteins. It has been demonstrated that sex steroids could regulate the activities of hepatic lipase, which has an important role in the removal of TAG and phospholipids from sub-fractions of HDL particles, and also functions in the lipolysis of TAG-rich particles( Reference Tikkanen and Nikkila 30 ). Skinner also suggested that the obesity-related cardio-metabolic risk factors (such as dyslipidaemia and abnormal SBP) occur earlier in boys than in girls( Reference Skinner, Perrin and Moss 31 ). However, as the information of sex hormone was not collected, we cannot draw a definite conclusion. Further study should be warranted to explore the mechanism in more depth.
For the mediation effects of blood lipids, we revealed that TAG mediated 8·29 % of the relation between BMI and SBP, and 12·53 % of the relation between BMI and DBP in boys. LDL-cholesterol mediated 7·75 % of the relation between BMI and DBP in boys. A previous study had suggested that the association between BMI and BP was additionally indirectly mediated by insulin resistance, which mediated 12·4 and 6·3 % of the association between adiposity and SBP, in girls and boys, respectively( Reference Correia-Costa, Santos and Severo 27 ). In terms of the association between BMI and DBP, the significant mediation effect was only found in boys, with a mediation ratio of 13·5 %. Comparing with insulin resistance, the mediation effect of blood lipids’ was less impressive but significant. Our data supported that in overweight boys the impact of BMI on BP profile was partly mediated by TAG, whereas LDL-cholesterol mediated the relationship between BMI and DBP. These results suggest that TAG and LDL-cholesterol may explain part of the association between BMI and BP. Future studies should endeavour to explore the mechanism between obesity and high BP.
Mechanistically, the plausible explanation linking elevated TAG and LDL-cholesterol with high BP was that dyslipidaemia can lead to the endothelial damage and loss of physiological vasomotor activities. These changes of blood vessels may result in the increase in BP levels( Reference Wong, Lopez and Tang 32 , Reference Anderson, Castelli and Levy 33 ). Nickenig et al. ( Reference Nickenig 17 , Reference Nickenig and Harrison 18 , Reference Nickenig and Harrison 34 ) demonstrated that abnormal lipid profile, as a strong predictor of CVD, may damage the nitric oxide production and activity, as well as alter endothelin A and B receptor and endothelin-1 expression, which would lead to endothelial dysfunction. In addition, a dysfunctional endothelium cannot normally respond to the changes in intravascular conditions to constrict and dilate ( Reference Nohria, Garrett and Johnson 35 ), and the damage of physiological vasomotor activity, which results from endothelial dysfunction, may result in elevated BP.
Strengths and limitations
It is novel to explore the contribution of blood lipids to the relationship of BMI and BP among children with overweight and obesity. In addition, the method of mediation analysis may provide a more objective direct association between BMI and BP. However, as a cross-sectional study, only associations but not causality can be inferred. A longitudinal study is needed to confirm our findings. Because the BP records were based on two measurements in a single occasion, BP levels from multiple visits would be more desirable in future studies. In addition, abnormal blood lipids, obesity, high BP and high blood glucose or insulin resistance usually coexisted, which are all components of the metabolic syndrome. Insulin resistance was reported as a mechanism of obesity-related hypertension( Reference DeMarco, Aroor and Sowers 36 ); we cannot confirm the mediation role of insulin resistance on the association between adiposity and BP because of the lack of data on insulin resistance, which is a limitation. Furthermore, because only overweight and obese participants were included in the study, it is a limitation that we are not sure of the external generalisability of this study. Future study involving normal weight should be warranted to confirm the results.
Conclusions
In conclusion, our results first highlighted the sexual difference in the mediation role of blood lipids in the association between BMI and BP. In addition to the direct association between elevated BP and BMI, a mediation role of TAG and LDL-cholesterol was detected in the association between BMI and BP. Our findings suggest that both lipid profile and BMI should be considered when the intervention aimed to reduce the burden of hypertension is conducted in children.
Acknowledgements
The authors would like to thank all the children and parents for their participation in this study, and also the head teachers of the schools for their help and cooperation in the research. The authors also want to express our thanks to Luke W. Arnold for his help in the English editing of our paper.
This work was supported by the Medical Research Council the Research Special Fund for Public Welfare of Health (201202010) and National Science Foundation of China (NSFC81402692). Funders had no role in the design, analysis or writing of this article.
Y. D. Y., J. M. and Z. Y. Z. conceived and designed the study. S. W., X. H. L. and B. D. carried out the study. Y. D. Y. and Z. Y. Z. analysed data and drafted the manuscript. All authors were involved in reviewing the article and had final approval of the submitted and published versions.
The authors declare that there are no conflicts of interest.
Supplementary Material
For supplementary material/s referred to in this article, please visit http://dx.doi.org/10.1017/S0007114516001744








