At the start of the new millennium, despite a plethora of policy reforms and pockets of good practice, user involvement in mental health is still an essentially minority activity, acknowledged as a ‘good thing’ by many, but relatively rarely practised. The purpose of this article is to highlight what is meant by the terms ‘user’ and ‘involvement’ and to describe why user involvement is important. We offer some practical guidance on both the barriers that others have come across and ways in which meaningful user involvement is being implemented in practice.
What do we mean by ‘mental health service user’?
The language used to describe service users is perhaps more varied in mental health than in any other sector of health and social care.
Users are most frequently portrayed as patients – as objects of the clinical gaze of mental health professionals (Reference Pilgrim and RogersPilgrim & Rogers, 1999) – and therefore in terms of their illness. However, users can also be seen as consumers, survivors and providers, all of which imply different notions of the roles and responsibilities of people with mental health problems and the relationship between them and mental health services.
Consumerism is a relatively new ideology within UK health policy, linked to the rise of general management principles in the National Health Service (NHS) during the 1980s and the growing acknowledgement of the importance of satisfaction with healthcare. Users are increasingly seen as customers who can exercise an informed choice about the services they receive and can shop around, which means that if they are not satisfied, they can take their ‘business’ elsewhere. However, the more recent Mental Health Bill (Department of Health, 2002) focuses on risk management and the safety of the general public rather than the rights of mental health service service users as consumers. Poverty can also limit choice, with private sector mental health services beyond the reach of many service users. It is possible that those who have access to information systems and to transport and travel may be more easily able to exercise their right to choose than more socially excluded, hard-to-reach sectors of society, such as people with mental health problems.
The user as ‘survivor’ is linked to the growth, in the early 1970s, of collective activities of mental health service users, initially in The Netherlands and the USA. Recognising the wisdom of the dominant trade union philosophy of the time that ‘unity is strength’, organisations such as the Campaign Against Psychiatric Oppression and the British Network for Alternatives to Psychiatry were formed. The image and term ‘survivor’ is very particularly chosen by groups such as Survivors Speak Out, the United Kingdom Advocacy Network (UKAN) and the Hearing Voices Network to portray a positive image of people in distress as those who had the strength to survive the mental health system. ‘Survivor’ also implies a notion of rejecting forms of professionally led and produced information.
The conceptualisation of users as providers is reflected in the development of user-led services that are found in the voluntary and statutory sector across the USA and increasingly in the UK. The scope of user-led activities ranges from patients being mutually supported in professionally led services to projects that are managed and staffed by users themselves. The latter include safe houses and drop-in day centres and often reflect the user movement priorities of voluntary relationships, alternatives to hospital admissions and personal support and advocacy (Reference O'Donnell, Parker and ProbertsO’Donnell et al, 1999; Reference Chinman, Weingarten and StaynerChinman et al, 2001).
The recent policy context of mental health service user involvement
Since the establishment of Community Health Councils in 1973, the rhetoric of generic user involvement has become a central component of NHS policy. In 1990, the NHS and Community Care Act was the first piece of UK legislation to establish a formal requirement for user involvement in service planning. Subsequent key policies in the early 1990s include the Patient’s Charter (Department of Health, 1991) and plans set out in Local Voices (NHS Management Executive, 1992), which aimed to make services more responsible to patients’ needs but stressed consumerism rather than partnership or participation.
Since 1997, ‘patient and public involvement’ in healthcare has become one of the central tenets of New Labour’s NHS modernisation agenda. Under New Labour, the user involvement agenda has been formalised in policy terms through the NHS Plan (Department of Health, 2000), which emphasised the government’s commitment to creating a patient-centred NHS with users’ needs central to service design and delivery. The NHS Plan proposed the development of the Patient Advice and Liaison Service (PALS). The following year, Section 11 of the Health and Social Care Act 2001 required all NHS organisations to engage with users in service planning and evaluation as well as providing opportunities for treatment decision-making. The structural bodies responsible for the implementation of these requirements include the Commission for Patient and Public Involvement in Health (CPPIH), established through the NHS Reform and Health Care Professions Act 2002.
More recently, ‘patient choice’ has become a particularly strong political imperative and a topic of heated debate. Service users, influenced by increasing consumerism, now have greater access to information (mainly on the internet), and can enter the slowly growing private sector (Reference Appleby, Harrison and DevlinAppleby et al, 2003). The government’s response has been to appoint a ‘Patient Tsar’ to advise us on how service users’ experience can be improved, and to publish a series of measures to extend patient choice across primary, secondary and community care (Department of Health, 2003a).
At that time, user involvement in the specific context of mental health was encouraged in documents such as The Health of the Nation (Department of Health, 1992), Working in Partnership (Department of Health, 1994) and Building Bridges (Department of Health, 1995). Indeed, Working in Partnership declared:
‘The work of mental health nurses rests upon the relationship they have with people who use services. Our recommendations for future action start and finish with this relationship’ (Department of Health, 1994: p. 5).
However, there is also evidence to suggest that the often very good intentions of policy makers can sometimes fail to move beyond rhetoric into reality, particularly for mental health service users. User representatives on a national group convened by the Department of Health in 1998 to develop the National Service Framework (NSF) for Mental Health resigned when it became clear that the government was going to insist that compulsory treatment orders were non-negotiable (Reference DonnellyDonnelly, 1998). The final document (Department of Health, 1999) stated that specific arrangements should be in place to ensure service user and carer involvement, but there are few other references to users throughout the seven standards of the NSF or indeed directly in the recent Five Years On review (Department of Health, 2004).
User involvement in theory and practice
User involvement encapsulates a range of different ideas (as does the concept of user itself) (Reference Braye, Kemshall and LittlechildBraye, 2000), from active participation at the micro-level of individual decision-making, to more macro-level involvement in service planning and evaluation and, increasingly, in the training and research arenas.
Reference Peck, Gulliver and TowellPeck et al(2002) constructed a particularly useful schema building on theoretical models devised by a number of others, including Reference HirschmanHirschman (1970), Reference ArnsteinArnstein (1969) and Reference Pilgrim and RogersPilgrim & Rogers (1999). This uses three distinct conceptions of user involvement – as recipients, subjects of consultation and agents in control. They suggest that user involvement within mental health services operates at four levels:
-
1 in the interaction between service users and in the form of self-help;
-
2 in the interaction between individual users and professionals working with them;
-
3 in the management of local services;
-
4 in the planning of overall services.
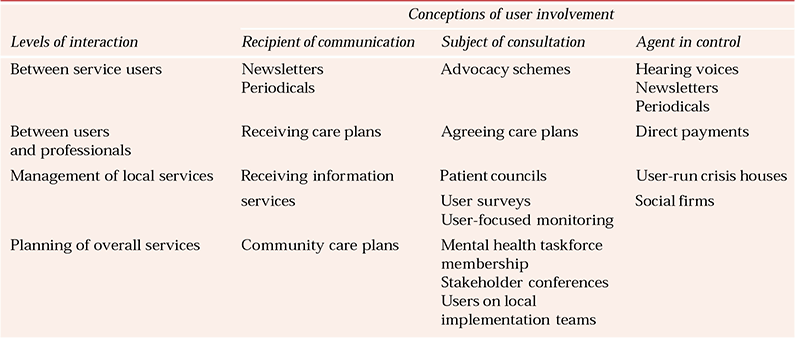
Peck et al argue that if these two frameworks are combined, it is possible to construct a matrix for user involvement with the conceptions of involvement forming one axis and the level of interaction forming the other (Table 1). Peck et al suggest that the matrix illustrates the sheer diversity of current mental health service user involvement activities in the UK, but also that many initiatives are clustered in the consultation category, with the ‘agent in control of the overall service planning’ cell significantly empty.
Table 1 Examples of user involvement in England (Peck et al,with permission)
| Conceptions of user involvement | |||
|---|---|---|---|
| Levels of interaction | Recipient of communication | Subject of consultation | Agent in control |
| Between service users | Newsletters | Advocacy schemes | Hearing voices |
| Periodicals | Newsletters | ||
| Periodicals | |||
| Between users and professionals | Receiving care plans | Agreeing care plans | Direct payments |
| Management of local services | Receiving information services | Patient councils | User-run crisis houses |
| User surveys | Social firms | ||
| User-focused monitoring | |||
| Planning of overall services | Community care plans | Mental health taskforce membership | |
| Stakeholder conferences | |||
| Users on local implementation teams | |||
In many ways, therefore, although ‘user involvement’ is a current buzzword and appears regularly in policy documents, mission statements and the academic literature, it may be less meaningful in practice. This view is supported by a survey of the mental health service user movement in England, which identified 318 user groups and found that
‘local service user groups play a very important role in mutual support, combating stigma, helping people to recover and stay out of services and participating in local service planning and development’ (Wallcraft, 2003: p. 1).
However, most groups were small, recently formed, poorly funded and non-representative of Black and minority ethnic communities, all of which limited their capacity to achieve change. In 2001 a large cross-sectional survey of users and providers of psychiatric services across Greater London found that none of the trusts had systems for involving users that met national standards (Reference Crawford, Aldridge and BhuiCrawford et al, 2003). So, although it is true that there are many more user groups than there used to be, it appears that their influence may be limited, with an emphasis on sharing information rather than partnership or user-led services.
Why is user involvement important?
There are a number of often interrelated reasons for believing that mental health service user involvement is more than a politically mandated ‘good thing’ and is a worthwhile activity with a range of practical and ethical benefits. These are summarised in Box 1 and briefly discussed below.
Box 1 The benefits of service user involvement
-
• Users are experts about their own illness and need for care
-
• Users may have different but equally important perspectives about their illness and care
-
• User involvement may increase the existing limited understanding of mental distress
-
• Users are able to develop alternative approaches to mental health and illness
-
• User involvement may be therapeutic in itself
-
• User involvement may encourage greater social inclusion
‘Expert patients’
There is widespread recognition that service users are experts, with an in-depth knowledge of mental health services and of living with a mental health problem (e.g. Chief Medical Officer, 2001). By definition, no one else, no matter how well trained or qualified, can possibly have had the same experience of the onset of mental illness, the same initial contact with services or the same journey through the mental health system. These experiences are an important resource that can help to improve individual packages of care as well as services generally. Reference BorrillBorrill (2000), for example, emphasises the way in which users can predict when they are about to become unwell and formulate appropriate responses at an early stage. If mental health professionals can tap into this expertise, they make their own jobs much easier and more productive by focusing on users’ considerable strengths.
Differences of perspective
Service users and mental health professionals often have very different perspectives. Reference Lindow and ParkerLindow (1999), for example, highlights the way in which users and service providers may have very different priorities, with users more concerned about poverty and housing than local commissioning arrangements. Involving users can provide insights that prompt practitioners to re-evaluate their work, challenge traditional assumptions and highlight key priorities that users would like to see addressed.
Insight into mental distress
Reference MayMay (2001) suggests that the inclusion of users’ experiences and knowledge through service user involvement will supplement the existing limited understanding of mental distress. User involvement in this sense may also lead to a new way of thinking about the nature of evidence itself, with what was considered anecdotal experience given new validity through viewing it as ‘human testimony.’
Alternative approaches
Users are able to develop alternative approaches to mental health that can complement existing services. The Strategies for Living group, for example, has highlighted the importance of alternative and complementary therapies (Reference Faulkner and LayzellFaulkner & Layzell, 2000; Mental Health Foundation, 2003), while the Hearing Voices Network (http://www.hearing-voices.org) encourages positive working practices with people who hear voices and works to promote greater tolerance and understanding of this condition.
Involvement as therapy
User involvement can be therapeutic. Helping to shape services, particularly when users work together collectively, can help to increase confidence, raise self-esteem and develop new skills (Mental Health Foundation, 2003).
Promotion of social inclusion
People with mental health problems are among the most socially excluded within any society, subject to the interlocking and mutually compounding problems of impairment, discrimination, diminished social roles, unemployment and lack of social networks (Office of the Deputy Prime Minister, 2004). Reference Webb, Clifford and FowlerWilkinson (1996) has suggested that it is relative rather than absolute poverty within societies that creates health inequalities through mediating factors such as powerlessness and social stress. Encouraging greater user involvement, including paid activity, can be empowering and address issues of poverty and may therefore act as one mechanism to encourage greater social inclusion (Reference Sayce and MorrisSayce & Morris, 1999).
Barriers to user involvement
Despite its benefits and the significant political encouragement in recent years, user involvement in mental health services remains patchy, with an emphasis on consultation rather than influence, partnership or control. A number of different, although often interlinked, barriers hinder greater user involvement (Box 2).
Box 2 Barriers to user involvement in mental health services
-
• Lack of information
-
• Financial and time costs
-
• Concerns over representativeness
-
• Resistance to the idea of users as experts
Information shortage
Accessible information is an essential prerequisite for meaningful involvement, yet there is evidence of a widespread lack of information for service users on the nature of mental health problems, the side-effects of medication, alternative forms of treatment and mental health law (Reference WallcraftWebb et al, 2000; Reference Hogman and SandamasHogman & Sandamas, 2001). As an example, the Users’ Voices project (Reference RoseRose, 2001), which included interviews with over 500 users in seven geographical areas across England, found very low levels of involvement in individual care planning and in the planning and delivery of services generally, and suggested that this was often related to a lack of information.
Costs of involvement
User involvement, if properly implemented, can be financially expensive and time-consuming for the organisation and service users themselves. A survey of policy and practice in payments to mental health service users and carers involved in service development in 46 secondary mental health service organisations in England found that only 12 (26%) made transport available to users and 14 (30%) to carers and only 15 (33%) paid service users and 12 (26%) paid carers for their time (Reference Ryan and BamberRyan & Bamber, 2002).
Representativeness
Professionals wishing to promote user involvement have frequently expressed concerns about the ‘representativeness’ of individual service users, sometimes suggesting that particular users may be ‘too well’, ‘too articulate’ or ‘too vocal’ to represent the views of users generally. However, Reference Lindow and ParkerLindow (1999) suggests that the concept of ‘representativeness’ may be used as a subconscious method of resisting user involvement:
‘When workers find what we [users] are saying challenging, the most usual strategy to discredit user voices is to suggest we are not to be listened to because we are too articulate, and not representative. Workers seem to be looking for someone, the ‘typical’ patient, who is so passive and/or drugged that they comply with their plans. We are developing our own strategies to respond to these challenges in an attempt to reveal to such workers their double standards… We ask how representative are they, and the others on the committee? We point out that as they are selected for their expertise and experience, so are we. Indeed, we are more likely to have been selected by a group than they are… We ask, would workers send their least articulate colleague to represent their views, or the least confident nurse to negotiate for a change in conditions?’ (Reference Lindow and ParkerLindow, 1999: p. 166).
Professional resistance
Some professionals find it difficult to view service users as experts and resist moves towards greater user involvement. Although there is evidence to suggest that professionals are generally supportive of user involvement, there are also discrepancies between expressed support and actual practice (Reference CampbellCampbell, 2001). This could reflect professionals’ perception of themselves as more supportive than users perceive them to be (Reference Peck, Gulliver and TowellPeck et al, 2002), resistance to the notion of sharing and transferring power to users, or a clash of professionals’ ‘scientific’ and users’ more ‘social’ ways of thinking and working (Reference SummersSummers, 2003).
Examples of positive practice in user involvement
Despite the gap between policy rhetoric and practice reality and the barriers to user involvement, there is increasing evidence of positive practice in many areas of user involvement in mental health and social care (Box 3).
Box 3 Examples of positive practice in mental health services
-
• Involvement in prioritising and conducting research
-
• Involvement in staff selection
-
• Employment as paid mental health workers
-
• Involvement in planning and redesign of mental health services
-
• Involvement in education and training
Research projects
User involvement in research is important for a number of different reasons. Service users’ priorities for research are often different from those of academics, health and social care professionals or funding bodies. For example, a consultation exercise organised by the South London and Maudsley NHS Trust with service users found that highly ranked research topics included discrimination and abuse, social welfare issues and arts as therapies (Reference Thornicroft, Rose and HuxleyThornicroft et al, 2002).
User-led research projects are still relatively rare but key contributions in this area include the Strategies for Living projects (Reference Faulkner and LayzellFaulkner & Layzell, 2000; Mental Health Foundation, 2003) and Reference RoseRose’s (2001) work on users’ experiences of mental health services. These projects have highlighted the importance of training service users to undertake research and the added value as participants ‘visibly relaxed and opened up once they realised the interviewer had ‘been through the system’ and understood their own situation’ (Reference RoseRose, 2001: p. 4). It is also probable that responses to questions about experiences of services are more ‘honest’ and include extremes of experience when the interviewer is a service user (Reference Clark, Scott and BoydellClark et al, 1999).
In the future, the expansion of the requirement for evidence of user involvement in research proposals beyond the NHS Executive, Wellcome and service delivery and organisation funding bodies, and the establishment of the Service Users’ Research Group for England (SURGE) within the National Institute for Mental Health research network, may help to raise the profile and, more importantly, the active participation of users in all aspects of the research process.
Staff selection
In some areas, mental health service users are involved in recruiting staff. This is not just a symbolic statement about the importance of user involvement: it can also improve the appointment process. Reference Newnes, Long and MacLachlanNewnes et al(2001) described an attempt to involve service users in recruiting a clinical psychologist. An evaluation suggested that some participants felt that questions from the service user were ‘wise and thought-provoking’. In particular, the user was seen as being able to offer a human perspective that was well respected: ‘She came up with questions none of us professionals would ever have thought of and got a much stronger sense of what the candidate was like as a person’.
Inclusion in the workforce
Proposals for the new mental health workforce include the development of ‘support, time and recovery’ (STR) workers (Department of Health, 2003b ). These people come from different walks of life with different backgrounds, including volunteers and existing and former services users who have the ability to listen to people without judging them. They will work as part of a team that provides mental health services and focus directly on the needs of service users, working across boundaries, providing support, giving time and promoting their recovery. They can be employed by any agency in the NHS or social care field, including the private and voluntary sector. It is envisaged that up to 3000 STR workers will be trained and working by the end of 2005. The Department of Health’s Best Practice Guidance for Graduate Primary Care Mental Health Workers also includes recommendations for employing in the role people with lived experience of mental illness (Department of Health, 2003c ).
Service planning and delivery
Involving users in the planning and delivery of generic health services has grown considerably over the past decade. A systematic review (Reference Crawford, Rutter and ManleyCrawford et al, 2002) identified 337 relevant studies, including a number in the field of mental health. As an example, ‘collaboratives’, part of the government’s modernisation agenda outlined in the NHS Plan (Department of Health, 2000), are a quality improvement approach based on the principles of continuous quality improvement and service redesign. They involve a network of organisations working together for a fixed time on a specific clinical area. The government sees collaboratives as a method of redesigning services so that they are responsive to the needs of the patients rather than the organisation.
Within mental health, 37 organisations across the former Northern and Yorkshire and Trent NHS regions participated in the Mental Health Collaborative (MHC) on in-patient care from October 2000 to November 2001. An evaluation of the MHC (Reference Roberts, Hardacre and LocockRoberts et al, 2003) found a strong ethos of user involvement across services and evidence of its positive effects. Users were invited to join project teams as members, to attend learning sessions and to be closely involved in all aspects of the work. Improvements made through service user involvement included changes to process issues such as improved documentation. Some of the improvements suggested by service users were not the changes that staff might have considered a priority but were perceived as valuable. Many staff also felt that user involvement had challenged their own assumptions and led to new insights about patient care. However, the evaluation also noted scope for future improvements and the need to increase the level of user involvement.
Education and training
There has been recent policy support for greater involvement of both mental health service users and carers throughout the whole education and training process (Department of Health, 2001). A literature review of the value of developing the role of patients as teachers also highlighted important educational benefits for learners (Reference WilkinsonWykurz & Kelly, 2002). Involving users in training certainly has the potential to challenge some of the myths surrounding mental illness and to enable those responsible for delivering mental health services to gain an insight into what it is like to be on the receiving end of such services (Reference McAndrew and SamocuikMcAndrew & Samocuik, 2003). However, there has as yet been very little published about the extent, quality or effectiveness of service user involvement. For the time being, this area of positive practice remains more of a policy ideal than a practical reality.
Encouraging user involvement in your own organisation
Meaningful user involvement requires organisations to think about the practical aspects of the process such as the financial and structural changes that need to happen. Effective collaboration with users may, for example, require a review and possible reconfiguration of existing professional structures, rather than expecting users to adapt to outmoded ways of working.
User involvement also requires organisations to examine their own cultural environment. Service cultures that encourage involvement share a number of common characteristics, including a commitment to genuine partnerships between users and professionals and to the development of shared objectives. As the National Schizophrenia Fellowship (now Rethink) observed:
‘Everyone involved in the delivery of care, including service users and carers, should be treated as equal partners. Occasionally, some professionals may initially feel threatened by the involvement of service users and carers and if this is the case, then it is important that this issue is addressed so that all of the parties involved can work well together. It is essential to remember that every care partner brings something different, but equally valuable, to the relationship and that successful delivery of care depends on effective collaboration between the care partners’ (National Schizophrenia Fellowship, 1997: p. 10).
The approaches and values of individual practitioners are also crucial to the success of user involvement initiatives (Reference Breeze and RepperBreeze & Repper, 1998), with good listening skills and valuing people key attributes. Above all, however, meaningful user involvement that makes a difference cannot be a one-off intervention or a discrete programme of work. It must be part of the fabric of mental health services that affects every aspect of mental health provision.
MCQs
-
1 User involvement in mental health is:
-
a a new phenomenon
-
b politically mandated
-
c an active part of most mental health trust work programmes
-
d usually representative of Black and minority ethnic communities
-
e therapeutic for many service users.
-
-
2 Barriers to user involvement include:
-
a the need for new ways of thinking about and working with service users
-
b health professionals’ perceptions that they are themselves sufficiently supportive
-
c too much information for service users
-
d financial implications for the service providers
-
e health professionals’ worries about representativeness of service users.
-
-
3 User involvement in research:
-
a can highlight new perspectives on well-researched issues
-
b is able to address aspects of social exclusion faced by many service users
-
c is never as valid or reliable as research by non-users
-
d needs to be underpinned by appropriate training for the user-researcher
-
e is being discouraged by national research funding bodies.
-
-
4 Users can be involved in:
-
a prioritising research ideas
-
b staff selection procedures
-
c providing mental health services
-
d educating students and staff
-
e health service redesign strategies.
-
-
5 Meaningful user involvement requires:
-
a little extra financial resource
-
b an appropriate organisational culture
-
c a genuine partnership with service users
-
d one or two interested individuals in each organisation
-
e commitment at every level of the organisation.
-
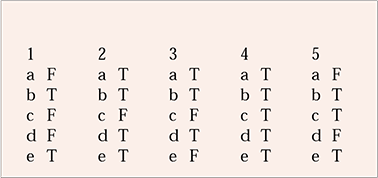
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | T | a | F |
| b | T | b | T | b | T | b | T | b | T |
| c | F | c | F | c | F | c | T | c | T |
| d | F | d | T | d | T | d | T | d | F |
| e | T | e | T | e | F | e | T | e | T |




eLetters
No eLetters have been published for this article.