Eye movement desensitisation and reprocessing (EMDR) literally owes its beginnings to a walk in the park. In 1987 an American psychologist named Francine Shapiro noticed while walking through a park that some disturbing thoughts that had been troubling her had ‘suddenly disappeared’. She also noted that when she recalled these thoughts, they were not as disturbing or as valid as they had been previously. She postulated that upsetting thoughts in general have a repetitive quality that changes only if the individual intentionally does something to cause change. However, her disturbing thoughts had changed without conscious effort. After considering this, she realised that during her walk her eyes had moved from side to side and she speculated that this might have been a key factor in her ability to process the disturbing memories. After experiments involving over 70 people, she published the first paper on EMDR 2 years later (Reference ShapiroShapiro, 1989). Since that time EMDR has attracted supporters and detractors in equal numbers as it has rapidly spread through the international therapeutic community, especially in the field of trauma.
In this article we concentrate on EMDR therapy for trauma, only briefly discussing its use in other anxiety and adjustment conditions. We review the process of EMDR and evaluate biological mechanisms that may underly its therapeutic effect. We also summarise the current clinical and evidence-based case for its use in practice, and give a brief overview of areas of controversy.
The EMDR process
Eye movement desensitisation and reprocessing therapy focuses on traumatic images and the negative cognitions and affective responses associated with them. Its aim is to desensitise the individual to the affective responses, but also to reprocess a more positive cognition and affective association with the traumatic image. This is accompanied by bilateral stimulation, usually in the form of saccadic eye movements. The process of EMDR (Box 1) has been extensively reviewed in APT by Reference MacCullochMacCulloch (1999) and elsewhere by Reference Shapiro and MaxfieldShapiro & Maxfield (2002), and it is only briefly summarised here.
Phase 1: Assessment
During this phase the therapist takes a full history and draws up a treatment plan in conjunction with the individual.
Box 1 Procedural phases of EMDR
-
1 Assessment
-
2 Preparation
-
3 Assessment of target memory/image
-
4 Desensitisation
-
5 Installation (of positive cognition)
-
6 Body scan
-
7 Closure
-
8 Debriefing on the experience of the session
Phase 2: Preparation
This is the phase at which the individual is prepared for EMDR, and much emphasis is placed on establishing a rapport and cementing the therapeutic alliance. The method of EMDR is described and the explanation is tailored to the specific individual, i.e. to their level of education and psychological sophistication. It is agreed with the individual which type of bilateral stimulation they prefer.
Phase 3: Assessment of target memory/image
During the assessment phase the individual will have identified memories, cognitions and emotions they would like to change. Treatment normally focuses initially on the image that represents the worst part of the memory for the individual. The individual is asked to identify the negative cognitions associated with the image, as well as the desired positive cognition. He or she is then asked to rate the emotional impact of the negative cognition and the validity of the positive cognition.
Phase 4: Desensitisation
The individual is asked to hold in the mind the target image together with the negative cognition. The preferred method of bilateral stimulation is begun and continued until the memory has been processed along all the chains of association. The therapist constantly checks on the individual's progress and for the emergence of new material to be processed.
The stimulation procedure
Stimulation is mostly achieved through rapid eye movements (Box 2), but any bilateral stimulation can be used, the most popular alternatives being hand-tapping and auditory stimuli. It is the bilateral nature of the stimulation, particularly eye movements, that is thought to facilitate processing, and this belief underlies, to a greater or lesser extent, most theories of the mechanism of EMDR.
Box 2 Bilateral stimulation using rapid eye movement
-
1 The therapist sits to the side and in front of the patient
-
2 The patient is asked to identify the direction (horizontal, vertical, diagonal or circular) and frequency of finger movement they prefer
-
3 The patient is then asked to hold in mind the traumatic image, along with any negative traumatic thought associated with it, and follow the therapist's moving finger
-
4 Sets of around 30 movements are usually used, but this is adapted according to the individual
-
5 The process is repeated until the material is fully processed, i.e. the patient feels no negative emotional or physical response to the image
Phase 5: Installation
This is the stage at which positive cognition is the installed, using the same stimulation process.
Phase 6: Body scan
The individual is asked to ‘scan’ (concentrate on) their body and identify any sensations. If a negative sensation is reported, bilateral stimulation is repeated. If positive sensations are reported, bilateral stimulation is used to strengthen the positive feeling.
Phase 7: Closure
The therapist praises the patient for the effort made and any progress achieved, and offers encouragement and support. The therapist should also give containment exercises, especially if the session was incomplete and there is still unprocessed material. Containment exercises usually involve the use of anxiety and relation techniques practised and introduced during the assessment phase. Standard techniques such as deep muscle relation are most often used.
To induce rapid eye movement the patient follows the regular movement of the therapist's fore-finger.
Phase 8: Debriefing the experience
In this closing stage of the session, the individual is debriefed and the likely effects of the session are explained. The patient is warned that they may feel the effects of continued processing for some days after the session.
Proposed mechanisms of action
Shapiro's adaptive information processing model
The mechanism underlying the therapeutic effect of EMDR is perhaps the area that generates the most controversy and vigorous debate, as it so closely relates to the role of eye movement.
Shapiro suggested a model for the actions of EMDR based on an information-processing paradigm and has refined this with time. She now puts forward the adaptive information processing model (Reference Shapiro and MaxfieldShapiro & Maxfield, 2002). This hypothesises the presence of a system within the brain that processes information into an adaptive state. This involves the forging of associations with previously stored material, thus forming a learning process by which traumatic information is captured in a state that lessens the emotional distress associated with it. It is proposed that partially processed information is stored essentially in the way it was captured, along with the emotional distress and traumatic cognitions. The processing of these memories becomes stuck and this provides the basis of the reliving, affective dysregulation and distorted cognitions so prominent in PTSD. Shapiro & Maxfield believe that the eye movements in EMDR are responsible for enhancing and accelerating information processing, thus providing the impetus for processing to take place and enabling an adaptive state to be reached.
Survival and conditioning
Reference MacCulloch and FeldmanMacCulloch & Feldman (1996) proposed a model for the effects of EMDR based on Pavlovian and Darwinian theory.
The Darwinian theory of natural selection holds that an organism will survive only if it can respond to threats and opportunities presented by its environment. Therefore, it would need to evolve to respond appropriately to threats, and seek to confront or escape them. Organisms unable to adapt to threats will be deselected by the evolutionary process and become extinct.
Pavlovian theory holds that a stimulus can lead to a conditioned response, especially if the pairing has a notably favourable or detrimental outcome. An example would be the way a predator will learn to avoid a porcupine after attacking it is paired with experiencing its painful and dangerous defence.
Applying this Pavlovian model to humans, a person perceives an external stimulus, which gives rise to an orienting response in which lateral, searching eye movements are important. This allows it to locate the source of the stimulus, which in turn triggers an investigatory reflex. If danger is identified, either from previous Pavlovian learning or an instinctive response programmed by evolution, it evokes a negative visceral response that is associated with fear. This results in avoidance behaviour, which would cause the person to fight, flee or freeze. Conversely, if no danger is identified, the stimulus will evoke the positive visceral element of the investigatory reflex, which is associated with reassurance and approach behaviour. This would cause the person to interact with and explore the stimulus.
MacCulloch & Feldman suggest that EMDR uses this positive visceral element of the investigatory reflex to enable exploration and interaction with feared stimuli and their eventual integration.
Induced REM-like state
Reference StickgoldStickgold (2002) revisits Shapiro's original observation that the eye movements induced by EMDR are similar to those seen during rapid eye movement (REM) sleep. It is believed that this is the stage of sleep during which episodic memories (memories of events) are integrated into general semantic networks. He theorises that events initially processed in the sensory cortices via a perceptual representation system may be modified by semantic memories during REM-sleep integration. Faulty integration of traumatic or distressing events is involved in PTSD. This potential modification is further added to by the effect REM sleep has in facilitating interaction between episodic memories in the hippocampus and the affect they are associated with in the amygdala, which is involved in fear responses.
Stickgold proposes that, in EMDR, bilateral stimulation using eye movements keeps focusing attention across the midline of the brain, thereby inducing a REM-like state. As in REM sleep, this state aids in the processing of the memories and their eventual integration. Thus, it appears that EMDR can be used to mediate re-integration into semantic memory networks and lessen the effect of hippocampally mediated episodic memories and their associated negative, amygdala-dependent affect.
Mechanisms suggested by theories of PTSD
Psychological theories explaining PTSD may also help to explain the therapeutic action of EMDR. In this section we suggest how two models of PTSD (the cognitive appraisal and fear network models) might combine in the dual representation model to inform our understanding of EMDR.
The cognitive appraisal model of PTSD
Reference Janoff-BulmanJanoff-Bulman's (1992) cognitive appraisal model of PTSD centres almost exclusively on the content of pre-existing beliefs about the self and the world that the individual brings into a traumatic event. Janoff-Bulman argued that PTSD is the result of the shattering of any of the following basic assumptions about the self and the world:
-
a that we are invulnerable;
-
b that the world is meaningful and comprehensible;
-
c that it is reasonable to view ourselves and others in a positive light.
Janoff-Bulman postulates that these assumptions give individuals structure and meaning in their lives. However, they cannot always be maintained in the face of a traumatic experience and this shattering may plunge the individual into a chaotic, confused state, characterised by avoidance, intrusion and hyperarousal.
The fear network model of PTSD
Foa et al (1989) outlined an information processing theory of PTSD that centres on the formation of a ‘fear network’ in long-term memory. This network encompasses: stimulus information about the traumatic event; information about cognitive, behavioural and physiological reactions to the event; and information that links these stimulus and response elements together. Activation of the trauma-related fear network by cue stimuli (reminders of the trauma) causes information in the network to enter conscious awareness in the form of the symptoms of PTSD. Attempts to avoid and suppress activation of the network lead to a cluster of avoidance symptoms in PTSD. Foa et al argue that successful resolution of the trauma can occur only by integrating the information in the fear network with existing memory structures.
The dual representation model of PTSD
The most influential recent psychological theory of PTSD that has helped our understanding of how EMDR may alter post-traumatic stress reactions is dual representation theory (Reference Brewin, Dalgleish and JosephBrewin et al, 1996). This approach has been important in that it posits the existence of two levels of memory at which trauma-related information can be represented. The first level of representation is that of the individual's conscious experience of the traumatic event. Brewin et al call this the ‘verbally accessible memory’. Verbally accessible memories are characterised by their ability to be deliberately retrieved and edited. It is argued that verbally accessible memory representations, as with Foa's fear network, contain the sensory, response and meaning information about an event. The second level of representation consists of the ‘situationally accessible memory’. This contains information that cannot be deliberately accessed by the individual and is not available for editing. Situationally accessible memories, as the name suggests, are accessed only when aspects of the original traumatic situation cue their activation.
Dual representation theory hypothesises that verbally accessible and situationally accessible memory representations are encoded in parallel at the time of the trauma, and between them account for the range of PTSD phenomenology. Brewin et al propose that the emotional processing of trauma needs to proceed in both memory representations in order to be successful. Individuals must consciously integrate the information in their verbally accessible memory of the event with their pre-existing beliefs and models of the world and thereby restore a sense of safety and control by making appropriate adjustments to expectations about their self and the world. The second emotional processing element is activation of the situationally accessible memory of the event through exposure to cues related to it.
Therapy using EMDR may facilitate the successful emotional processing of information in verbally and situationally accessible memory concerning the trauma.
These two routes to successful emotional processing owe much to the theoretical ideas discussed above. For example, the editing of verbally accessible memory information to bring it to record pre-existing models of the world fits well with Janoff-Bulman's model, while the requirement of activation and the subsequent integration of new information into verbally accessible memories accords with Foa's implementation of fear networks. Therefore, Reference Brewin, Dalgleish and JosephBrewin et al’s (1996) model may provide some explanation of how EMDR fits in with psychological theories of PTSD.
Clinical efficacy
There have been many studies of the efficacy of EMDR therapy for a wide range of clinical problems. Many of these are of dubious quality and add further to the controversy. For the purposes of this article we focus on the highest-level evidence and, as mentioned earlier, restrict ourselves to the field of trauma (which is in fact where the most published evidence exists for the use of EMDR). There are currently three published meta-analyses on efficacy.
In an analysis of the results of 61 treatment-outcome trials for PTSD, Reference Van Etten and TaylorVan Etten & Taylor (1998) compared the effect sizes of various medications and psychological therapies, including EMDR and behavioural therapy. The psychological therapies had significantly lower drop-out rates than the pharmacotherapies (14% v. 32%). Overall, the most effective psychological therapies (EMDR and behavioural therapy, with little to choose between them) and pharmacological treatments (SSRIs and carbamazepine) were generally equally effective. The psychological therapies were more effective in terms of symptom reduction, but the SSRIs held advantages in treating depression.
Reference Davidson and ParkerDavidson & Parker (2001) conducted a much more selective meta-analysis of 34 studies of EMDR therapy. They included only published work (not conference papers) that permitted a clear evaluation of the immediate post-treatment effects of EMDR. They excluded reports on follow-up outcomes. This gave a relatively small number of trials and excluded a large body of evidence, but ensured the high quality of those included. They concluded that EMDR is as effective as other exposure techniques, although not superior. As discussed below, they also failed to demonstrate the need for eye movements.
In an attempt to reduce the ‘noise’ created by studies of dubious quality, Reference Maxfield and HyerMaxfield & Hyer (2002) included just 12 trials in their meta-analysis relating treatment efficacy and trial methodology. Importantly, they found that the greater the methodological rigour of the study, the greater the effect size in favour of EMDR for PTSD. All 12 trials were controlled treatment-outcome studies that measured EMDR against waiting-list controls or standard treatments. None of these used robust trauma-focused cognitive–behavioural therapy (CBT), which is considered the gold standard of treatment (National Institute of Clinical Excellence, 2005). The findings should therefore be viewed cautiously, as the increased effect size may be due both to the comparison of EMDR with treatments that do not have great benefits for PTSD and to the small number of trials studied, loading the outcome in favour of EMDR.
The use of EMDR with other clinical conditions
Since the introduction of EMDR as an effective clinical tool for trauma, it was inevitable that it would be tried for other clinical conditions. Positive therapeutic results have been reported for a wide variety of problems, including phobias and panic disorders (Reference De Jongh and Ten BroekeDe Jongh & Ten Broeke, 1998), morbid jealousy (Reference BloreBlore, 1997) and chronic pain (Reference Grant and ThrelfoGrant & Threlfo, 2002). However, many of these studies are single case reports. A number of studies and reports attest to the efficacy of EMDR with children as well (Reference LovettLovett, 1996; Reference Tinker and WilsonTinker & Wilson, 1999).
Chronic pain
The most promising alternative use has been for the treatment of chronic pain (Reference Grant and ThrelfoGrant & Threlfo, 2002). It is generally accepted that pain, particularly chronic pain, involves psychological factors, either as a reaction to or a predisposing factor for it. When associated with physical injury, trauma can also maintain or exacerbate pain. In a study of Vietnam war veterans who experienced chronic pain, participants who also had PSTD rated their pain and level of disability higher than those who did not have the disorder (Reference Beckham, Crawford and FeldmanBeckham et al, 1997).
It has also been found that pain can cause trauma. Women with PTSD following obstetric or gynaecological procedures attributed their trauma in part to excessive pain (Reference MenageMenage, 1993). Reference Schreiber and Galai-GatSchreiber & Galai-Gat (1993) reported the case of an individual who lost an eye in an accident and developed PTSD. The core trauma was found to be uncontrolled pain while waiting 7 hours for surgery.
In the psychological treatment of chronic pain, EMDR seems to improve coping, give relatively permanent reduction of pain and alter pain-related attitudes and beliefs (Reference Grant and ThrelfoGrant & Threlfo, 2002). However, physiological damage associated with long-term injury processes means that pain relief in these cases may be limited. Nevertheless, the use of EMDR for pain problems is an interesting and clinically useful development (Reference Grant and ThrelfoGrant & Threlfo, 2002).
Discussion
Both proponents and opponents of EMDR feel very strongly about their views, and this passion has only grown in intensity as the procedure has gained prominence as an effective treatment. Much of the early criticism was directed at Francine Shapiro herself. Her initial claims heralding EMDR as a panacea for traumatic memories served only as fuel for sceptics. Arguably, the commercialisation of EMDR training worldwide, even when the evidence-base was not robust, did little to appease detractors. Consequently, EMDR's increasing acceptance by the therapeutic community has been accompanied by equally vociferous condemnation and scepticism. Sadly, at times, true scientific debate seems to have fallen victim to extremely held opinions.
The evidence base
In their critical evaluation of EMDR, Reference Perkins and RouanzoinPerkins & Rouanzoin (2002) point out that there is still no empirically validated model capable of giving a convincing explanation for the effects of the therapy. They also criticise the quality of the research on which the claims of EMDR's efficacy are based (although this is an acknowledged problem in psychotherapeutic research generally). They point out that the body of evidence supporting EMDR comes from a relatively small number of authors, which may exaggerate results in its favour. Although they view the evidence for EMDR as inconclusive, they do think that the method has undergone considerable empirical validation. Perkins & Rouanzoin urge that more scientific debate and questioning are needed before wholehearted acceptance of the treatment.
EMDR without the EM?
Whether eye movements serve any function in the therapy remains a point of contention. Reference Cahill, Carrigan and FruehCahill et al (1999) acknowledge that EMDR works, but their review of dismantling studies failed to establish the necessity of eye movements. One of the key meta-analyses confirming the efficacy of EMDR (Reference Davidson and ParkerDavidson & Parker, 2001) also views the use of eye movements as unnecessary. Reference Herbert, Lilienfeld and LohrHerbert et al (2000) share this opinion and provide an eloquent critique on the commercialisation and promotion of EMDR, believing them to blur the boundaries between science and pseudo-science.
Imaginal exposure in another guise?
It has been suggested on numerous occasions that EMDR without eye movements amounts to no more than imaginal exposure, which therefore explains its efficacy.
The issue of whether EMDR is simply a variant of imaginal exposure has been hotly debated in the literature. As mentioned above, many have argued that it is similar to systematic desensitisation or prolonged exposure. However, the use of EMDR with children provides a different perspective on this issue. Reference Tinker and WilsonTinker & Wilson (1999: pp. 25–26) present the following explanation of the difference between EMDR and imaginal exposure:
‘If five or ten minutes of EMDR lead to cessation of symptoms in a child, due to the “exposure” of the child to memories of a traumatic event, and this is considered exposure therapy, then all therapy would have to be considered exposure therapy. Thus, with children, it becomes very difficult to see EMDR as a form of exposure, unless the term “exposure” is broadened to become all encompassing’.
Therefore, as EMDR uses intermittent stimulation and the results are not dose-related, it is difficult to attribute its effects to exposure alone (Reference Wilson, Becker and TinkerWilson et al, 1995).
Accelerated therapeutic effect?
Proponents of EMDR have claimed that the onset of therapeutic benefit is more rapid than with other psychological treatments, thus requiring fewer sessions. Although this assertion is supported by some randomised trials – for example Reference RothbaumRothbaum (1997) and Reference Scheck, Schaeffer and GilletteScheck et al (1998) report therapeutic change within three and two sessions respectively – it is not upheld by the National Collaborating Centre for Mental Health (NCCMH). In evidence-based clinical guidelines on the management of PTSD commissioned by the National Institute for Clinical Excellence, the NCCMH recommends that patients should be offered up to 12 sessions, regardless of the mode of therapy used (National Collaborating Centre for Mental Health, 2005).
In these guidelines it is concluded that EMDR is an effective treatment for PTSD, but that the evidence base is not as strong as that for trauma-focused CBT. However, direct comparisons of trauma-focused CBT, exposure CBT and EMDR showed that none had significant advantages over the others with respect to treatment outcome and the speed of therapeutic changes. All three interventions are currently considered superior to stress management, group CBT, psychodynamic psychotherapy, non-directive therapies and hypnotherapy. The guidelines recommend that all people with PTSD should be offered a trauma-focused psychological treatment that includes EMDR or CBT. The NCCMH recommendations for the psychological treatment of PTSD are summarised in Box 4.
Box 4 Summary of NCCMH guidelines for psychological therapy in PTSD
-
• All people with PSTD should be offered trauma-focused psychological treatments, either CBT or EMDR
-
• Psychological treatment should be offered regardless of time elapsed since trauma
-
• Treatment should be long enough (8–12 sessions of therapy should normally be allowed for), regular (weekly is recommended) and continuous with the same therapist
-
• In complicated cases, treatment should be extended beyond 12 sessions
-
• Competent individuals with appropriate training should deliver treatment
-
• If necessary, a therapeutic relationship should be established before the traumatic material is directly addressed, to prevent the client from feeling overwhelmed
-
• If individuals request treatments other than those recommended above, they should be informed of the lack of clinical evidence to support their use
-
• Non-trauma-focused interventions that do not address traumatic memories should not routinely be offered
-
• If clients fail to respond adequately to specific trauma-focused psychological treatment, they should be offered an alternative form of trauma-focused psychological treatment and/or augmentation thereof with pharmacological treatment
Conclusions
In its current form, EMDR is an established treatment for PTSD and its use is supported by sound empirical evidence to the level of meta-analyses. It appears to be as effective as the gold standard treatment of trauma-focused CBT. There may be considerable scope for EMDR to be part of a CBT repertoire, as many of the components of EMDR sit comfortably within a CBT framework. It is an active, directive and collaborative technique, which is imminently accessible to clinicians trained in CBT.
National Collaborating Centre for Mental Health (2005)
Published evidence justifies the clinical use of EMDR as a treatment for PTSD. Consequently, it should be one of the treatment options offered to people with PTSD, and the possibility should be examined of making it more available within the NHS.
However, significant concerns remain regarding the lack of a convincing theoretical model that can explain the effects of EMDR. Also, the function of bilateral stimulation needs to be further evaluated, which might result in future change to the method of EMDR.
The entire field of psychological therapies for PTSD would benefit from further study and clinical scrutiny, and EMDR is no exception.
MCQs
-
1 The credited founder of EMDR therapy is:
-
a Ivan Pavlov
-
b Francine Shapiro
-
c Robert Stickgold
-
d Charles Darwin
-
e Ronnie Janoff-Bulman.
-
-
2 The effectiveness of EMDR has been variously attributed to:
-
a the utilisation of the positive visceral effect of the investigatory reflex to integrate memories
-
b the facilitation of adaptive information processing to store memories in less distressing forms
-
c enhancement of the integration of memories into semantic memory networks by introducing a REM-like state
-
d lessening of the effect of episodic traumatic memories and their associated amygdala-dependent negative affect
-
e activation of the reticulo-activating system to suppress traumatic sensory information and the affective responses they trigger.
-
-
3 According to Shapiro, the following procedures are essential in the practice of EMDR:
-
a bilateral stimulation
-
b induction of a hypnosis-like state
-
c reaction formation
-
d imaginal exposure
-
e sublimation.
-
-
4 The following are proven treatments of PTSD:
-
a EMDR
-
b trauma-focused CBT
-
c hypnotherapy
-
d selective serotonin reuptake inhibitors
-
e exposure CBT.
-
-
5 EMDR involves the following procedural phases:
-
a assessment
-
b desensitisation
-
c installation
-
d restructuring
-
e body scan.
-
MCQ answers
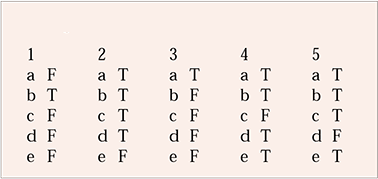
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | T | a | T |
| b | T | b | T | b | F | b | T | b | T |
| c | F | c | T | c | F | c | F | c | T |
| d | F | d | T | d | F | d | T | d | F |
| e | F | e | F | e | F | e | T | e | T |



eLetters
No eLetters have been published for this article.