The huge majority of people with an alcohol dependence problem that is uncomplicated by serious mental illness or social chaos receive treatment in the community. Tackling Alcohol Together: The Evidence Base of a UK Alcohol Policy (Raistrick et al, 1999, chapter 9) provides strong evidence supporting the move towards briefer and community-based treatments, while at the same time recognising the need for intensive and in-patient treatments for people with more complicated problems. It follows that the traditional sequencing of care, which might be characterised as having four phases - assessing and engaging patients, detoxification, specific therapy and after-care - is less tidy than it used to be. Detoxification is seen much more as a standalone procedure that should be undertaken when the patient is ready, rather than as a prerequisite of starting treatment. Of course, there are also instances where detoxification may be required as an expedience, for example during an unplanned admission into hospital, or where regular high levels of intoxication are a barrier to treatment. Equally, where the focus of treatment is on mental illness rather than alcohol dependence, then detoxification may well be viewed as a necessary first step.
A debate is gathering momentum, not just in psychiatry, about the future role of the generalist. Given the high proportion of people who have a combined problem of mental illness and alcohol dependence, it is inevitable that general psychiatrists will need to be skilled in the management of detoxification, but whether they should also have skills in specific substance misuse treatments is more contentious. Patients, their friends or relatives and sometimes also doctors become so desperate when faced with a catalogue of alcohol-related harms that they seek a solution in detoxification; in itself, this may provide respite and be a caring intervention, but it cannot be expected to have a significant effect on drinking behaviour. The point to be made here is that detoxification should not take place in isolation, but rather should be integrated with a suitable psychosocial therapy or, where mental illness is judged the primary problem, with the usual treatment for the mental illness.
The particular purpose of detoxification is to minimise the severity of withdrawal symptoms that occur when alcohol consumption is abruptly stopped or markedly reduced, and thereby to achieve an alcohol-free state with maximum safety and minimum discomfort to the patient. The Substance Misuse Advisory Service (Health Advisory Service 2000, 1999) has set out guidelines for commissioning alcohol detoxification services and stresses that a variety of settings are an important component of a district alcohol treatment system.
Alcohol withdrawal
Anyone may develop a tolerance to the effects of alcohol within a matter of days or weeks, provided that they take a sufficiently high and regular dose. Withdrawal symptoms are generally thought of as a feature of the later stages of a drinking career, and once they have occurred then subsequent manifestations in terms of both frequency and severity depend upon a complex interaction of factors, but above all blood alcohol level seems to be important. Descriptions of what would now be recognised as withdrawal symptomatology, including alcoholic delirium, can be found throughout historical texts, but the scientific demonstration of alcohol tolerance and withdrawal, based on both observational and laboratory studies, is relatively recent and followed on from the classic study by Isbell et al (1955).
In a selective review of the research evidence, Gross (1977) concluded that the severity of the alcohol withdrawal syndrome related to the abruptness of withdrawal and alcohol intake modified by the contribution of residual effects of previous drinking. He went on to describe a factor structure of withdrawal:
-
• Factor 1 - hallucinogenic: consists of nausea, tinitus, visual disturbance, pruritis, parasthesiae, muscle pain, agitation, sleep disturbance, tactile hallucinations, and hallucinations which are auditory or visual or both;
-
• Factor 2 - affective and physiological: consists of anxiety, depression, tremor and sweats;
-
• Factor 3 - delirium: consists of clouding of the sensorium, impairment of consciousness, impairment of contact with the observer.
Factors 1 and 2 were seen as existing along a continuum of severity, whereas Factor 3 appeared more complex, since it increased both during drinking and on withdrawal. Many of the symptoms that commonly occur in alcohol withdrawal are also found in mental illnesses, stress disorders, and intoxication with a variety of psychoactive drugs (see Box 1). Negative mood states are highly likely to provoke drinking, which in turn is likely to relieve the symptoms: this holds true not only for people experiencing withdrawal, but also when negative mood states occur during a period of total abstinence from alcohol. In other words, negative mood states are a powerful relapse precipitant.
Box 1 The 10 most common and the 10 most specific symptoms of alcohol withdrawal (adapted from Hershon, 1977)
-
• Depression
-
• Anxiety
-
• Irritability
-
• Tiredness
-
• Craving
-
• Restlessness
-
• Insomnia
-
• Confusion
-
• Sweating
-
• Weakness
Most common symptoms
-
• Whole body shaking
-
• Hand/finger shaking
-
• Facial tremulousness
-
• Cannot face the day
-
• Panick
-
• Guilt
-
• Nausea
-
• Visual hallucinations
-
• Weakness
-
• Depression
Most specific symptoms
The characteristics of alcohol withdrawal are well known. For the majority of patients, there are no complications from withdrawal and there comes to be an expectation that all detoxification is risk-free. The danger is that clinicians may not exercise sufficient vigilance when monitoring withdrawal and may find themselves dealing with avoidable problems or, at worst, a fatality. It is the timing of withdrawal symptomatology that is particularly unpredictable - the tremulous state typically peaks within 6-24 hours of stopping or reducing alcohol consumption. Illusionary or transient hallucinatory phenomena superimposed on the tremulous state, but occurring within a similar time-scale, should alert clinicians to a more severe withdrawal and the need to review medication. The peak incidence for seizures is around 36 hours and for delirium around 72 hours, although both of these phenomena may occur while a person is still drinking. Probably the most important determinant of severity of withdrawal is the rate of fall in blood alcohol level, which in turn is a function of peak blood alcohol level. It is unlikely that the clinician will be able to gain sufficient insight into these from history taking and so observation is all-important.
The presence of withdrawal symptoms is sometimes seen to be the essence of addiction or at least of physical dependence. This preoccupation with withdrawal, which is often also associated with an emphasis on pharmacological treatment of the withdrawal, is unhelpful and distracting. In psychological terms, detoxification reduces the severity of withdrawal and thereby eliminates the negative reinforcement of relief drinking. In practice, a broad spectrum of drinking cues are diminished as the process of detoxification progresses. Neuroadaptation, that is, tolerance and withdrawal, is a function of recent alcohol intake that correlates highly with alcohol dependence but is theoretically distinct. Placing undue emphasis on substance-specific withdrawal fails to recognise the variety of cues and cue complexes that act as sources of reinforcement and contribute to building dependence, fails to take account of the transferability of dependence from one substance to another, and fails to take account of persistent dependence in people who have achieved long periods of abstinence. All of these have practical implications for future treatment plans.
Preparation for detoxification
The key to a successful, planned detoxification is preparation. The first job of therapy is to bring the patient to a point of readiness to change their drinking behaviour. In terms of the popular ‘stages of change’ model (DiClemente & Prochaska, 1998: pp. 3-24) this means at least reaching the determination stage. At this stage, patients are sufficiently well motivated to make a sustained effort to change. In other words, they have reached a good quality decision to change rather than opting for detoxification because they feel physically unwell, are under pressure from family or work, or simply feel the need for a temporary break from drinking. Motivation is not necessarily something that patients either have or do not have - rather, there are specific, typically brief interventions designed to enhance motivation; the UK Alcohol Treatment Trial is using a manual-based therapy called Motivational Enhancement Therapy for this purpose. Once the therapist is certain that the patient has reached the determination stage there is, ideally, a second step which involves more detailed and more practical preparation work.
This more detailed preparation for detoxification is probably best handled with the assistance of a leaflet or checklist that the patient can take away to work on alone. It is important for the doctor or therapist to work in a motivational style (Reference Rollnick, Bell, Miller and RollnickRollnick & Bell, 1991) with the aim of moving the patient through to the action stage of change prior to commencing detoxification. The hallmark feature of the action stage is having a positive outcome expectancy or, more simply, the patient needs to believe that life is going to be better after detoxification. Often, patients assume that this will be the case, but have not really thought through the implications of not drinking, which will often mean not seeing friends or drinking mates and having unfilled time. Not doing something is inherently unrewarding and it is crucial that positive alternatives to drinking are planned.
Second, patients need to be given accurate information about what to expect during detoxification. Information-giving is likely to reduce the severity of the withdrawal and increase compliance (Reference Phillips, Gossop and BradleyPhillips et al, 1986). In the course of this discussion, it is often useful to map out a timetable for the week in which detoxification will take place and for the following week. Filling out such a timetable in some detail is a convenient way to bring up a number of important issues. For example, if the patient is working, have they planned to take time off? If the patient has childcare responsibilities, have these been met? If the patient is travelling to an out-patient unit daily, are there any transport difficulties? Is there someone who is willing to support the patient throughout the first week of detoxification? The timetable for week two of detoxification raises rather different issues, which are generally in the area of relapse prevention. For example, has there been a discussion about prescribing disulfiram? Does the patient have leisure or work activities to pursue or is there a need to plan new activities? If the detoxification team does not include the patient's usual therapist, have hand-over arrangements been made? Local custom and practice determine to what extent relapse prevention work is integral to detoxification. What matters is that patients do not return to their usual drinking friends and environment, or at least that they do not do so without some preparation.
The most suitable setting for detoxification needs to be discussed, but safety and economic (rather than convenience) considerations are foremost. The need for admission into a medical in-patient facility is a matter of clinical judgement and depends upon social as well as medical risk factors. See Box 2 for factors predicting severe withdrawal.
Box 2. Factors predicting severe withdrawal
-
Recent high levels of alcohol intake
-
Previous history of severe withdrawal
-
Previous history of seizures or delirium
-
Concomitant use of psychoactive drugs
-
Poor physical health
-
High levels of anxiety or other psychiatric disorder
For those people who are homeless or socially disorganised, detoxification may best be carried out in a non-medical residential facility (Reference Mortimer and EdwardsMortimer & Edwards, 1994), provided that the staff are trained to pick up medical complications on the rare occasions that these occur. The elderly are likely to experience a prolonged withdrawal syndrome and to be sensitive to the side-effects of medication, so detoxification should always be supervised either at home or in a residential facility.
For the majority of people, a community-based detoxification delivered in the home, or on an out-patient or day patient basis, is ideal. Home detoxification is relatively expensive and cannot usually be offered as an option for patients, but rather is reserved for people who would have difficulty attending a central unit, for example, people with a disability or who have childcare commitments. In rural areas, there may be a cost-efficiency as well as a convenience case for home detoxification. The model developed by Stockwell et al (1990) involves daily visits from a trained psychiatric nurse who assesses the severity of withdrawal and monitors for complications; any medication is prescribed on a shared-care basis with a general practitioner or by a consultant-led team. In the future, there is an opportunity here to use the extended nurse prescribing role with uncomplicated cases (Reference Ryan, Cash and HannisRyan et al, 1999).
The configuration of services within a health district depends upon local need and local preference. There needs to be agreement, however, about who looks after people with different kinds of problem. The small number of patients who experience marked withdrawal, including seizures, delirium and the potential for medical complications, may best be managed in a liaison psychiatry setting. For people with severe mental illness, there is a choice between general psychiatry, addiction psychiatry or a shared-care approach, which might include both out-patient and in-patient settings. A day care facility as part of the specialist addiction psychiatry team may well be able to handle surprisingly severe problems of alcohol withdrawal. Voluntary sector agencies are probably best positioned to provide non-medical facilities for homeless people and those with unstable social circumstances for whom accommodation is the primary need - supported sobering up, rather than detoxification, being the principal intervention.
Measuring the severity of withdrawal
It is good practice to use a standardised rating scale to measure the severity of alcohol withdrawal. The rating is used as one of the clinical indicators that informs prescribing and to pick up any complications that might arise during detoxification. The most commonly used scales are all derived from a 20-item instrument developed by Gross et al (1971). The different scales have broadly similar items for rating mild to moderate severities of alcohol withdrawal, but diverge on items such as ‘seizures’, ‘quality of contact’ and ‘thought disturbance’, which some authors claim have predictive validity. Metcalfe et al (1995) have developed a 10-item scale which has been validated for use in the UK (see Box 3). Of course, any rating scale must be interpreted in the light of the whole clinical picture. For example, patients with the dual diagnosis of anxiety disorder and alcohol dependence can be expected to experience significantly greater levels of anxiety throughout detoxification than patients with alcohol dependence only (Reference Johnston, Thevos and RandallJohnston et al, 1991).
Box 3. Items on Windsor Clinic Alcohol Withdrawal Scale (see Metcalfe et al, 1995)
-
• Anxiety
-
• Tremor
-
• Agitation
-
• Auditory hallucinations
-
• Visual hallucinations
-
• Nausea and vomiting
-
• Thought disturbance
-
• Orientation
-
• Quality of contact
-
• Seizures
An accurate examination of mental state leading to a diagnosis of psychiatric disorder is problematic in people who are drinking heavily or going through a detoxification programme. Up to 80% of problem drinkers entering into treatment experience psychiatric symptoms that typically fall short of a mental illness and commonly disappear after a period of total abstinence from alcohol. Symptoms are often non-specific and include dysphoria, anxiety, depression, panic, insomnia and in severe cases ideas of self-harm or hopelessness or even disturbances of thought or perception. Driessen et al (1996) found that for alcohol misuse in-patients, who are expected to have high rates of comorbidity, the prevalence of psychiatric disorder 2 weeks post-detoxification was 3% schizophrenia, 13% affective disorder, 22% phobic disorders and 2% generalised anxiety. It follows that clinicians need to exercise caution when making a mental illness diagnosis in people who are also problem drinkers. Ideally, diagnosis should be delayed for a period of 3-4 weeks post-detoxification (Reference Raimo and SchuckitRaimo & Schuckit, 1998). Getting the balance right is a difficult clinical judgement: on the one hand, there is a huge waste of resource from both unnecessary prescribing and unnecessary psychological therapies given prematurely to people who, it transpires, have an uncomplicated problem of alcohol dependence; on the other hand, delaying treatment may be harmful or be viewed as unacceptable.
Treatment
Treatment of alcohol withdrawal is usually uneventful and the clinician has a generous margin of error within which to work. Where mistakes are made, they are usually in the related areas of insufficient prescribing and insufficient observation for the level of risk. In the four tiers of service delivery described below (and see Box 4), it is the two variables ‘amount of treatment’ and ‘amount of observation’ that determine the appropriate level of intervention.
Box 4. Tiers of intervention
-
• Tier 1: mainly voluntary sector or non-specialist
-
• Supportive counselling and ‘feel good’ therapies
-
• Tier 2: mainly non-specialist mental health teams
-
• Opportunistic detoxification with fixed regimens
-
• Tier 3: specialist substance misuse teams
-
• Complex cases and full range of treatments
-
• Tier 4: usually liaison psychiatry or general medical teams
-
• Urgent and severe cases with medical or psychiatric complications
Tier 1
This level of service is for people who are expected to have only mild to moderate severity of withdrawal and may include those individuals who have a high level of anxiety about the detoxification process rather than actual withdrawal symptoms. The essential therapeutic skill is the ability rapidly to form a working alliance with the patient while having confidence to refer to Tier 2 when necessary. Some sophistication can be added by the use of the increasingly popular ‘feel good’ therapies such as acupuncture, massage or homoeopathy. There is limited evidence that acupuncture may have specific efficacy beyond the generalised ‘feel good’ effect (Reference Bullock, Culliton and OlanderBullock et al, 1989).
Tier 2
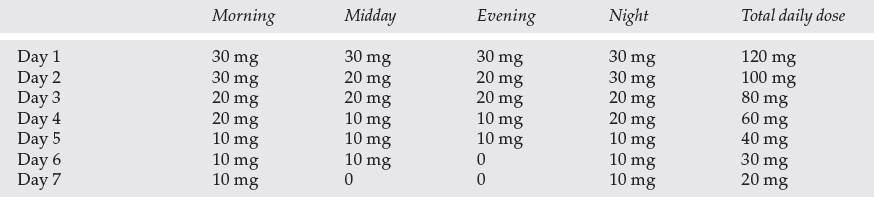
This tier is suitable for people with a moderate severity of withdrawal, but who none the less require some pharmacological treatment. It may be that the medical and nursing input available is quite limited and from staff who do not have specific addiction training. In these circumstances, it is sometimes useful to have a fixed-dose prescribing regimen in place (see Table 1). Primary care, medical and psychiatric out-patient clinics and some in-patient facilities function at this tier.
Tier 3
This is for people with moderate to severe withdrawal problems who can be managed by specialist staff working in the community or in a day facility. This tier requires medical and nursing staff who are trained and experienced in the management of addiction problems and who can handle complicated prescribing regimes. It is possible to manage patients who are hallucinating and who have a history of seizures provided that control of the withdrawal syndrome is rapidly achieved. This tier is likely to be part of a larger consultant-led service.
Tier 4
This is for people with the most severe withdrawal, which usually includes delirium and often includes seizures and medical complications associated with severe withdrawal, such as hypertension, Wernicke's encephalopathy, hepatic failure, subdural haematoma, hypoglycaemia, electrolyte imbalance (especially magnesium deficiency) and polydrug use. People with a severity of withdrawal requiring Tier 4 services should be regarded as a medical emergency requiring a liaison psychiatry or general medical team.
Alcohol enhances the inhibitory effects of the neurotransmitter γ-aminobutyric acid (GABA) and diminishes the activity of the excitatory N-methyl-d-aspartate (NMDA) receptors. Pharmacotherapy of withdrawal is therefore based on depressant drugs that enhance GABA. In turn, GABA influences other transmitter systems that are thought to contribute to the alcohol withdrawal syndrome (Reference NuttNutt, 1999) - dopaminergic induction of psychotic symptoms, NMDA excitability reducing the seizure threshold, and glutamate overdrive of noradrenergic sympathetic activity. Williams & McBride (1998) have reviewed the evidence for pharmacotherapies in the treatment of alcohol withdrawal: most of the studies had methodological flaws, but the evidence suggests that benzodiazepines and clomethiazole have similar efficacy for the treatment of withdrawal, including the prevention of seizures and delirium.
There is a strong argument against choosing clomethiazole as the first-line drug, in that it has a short half-life and high potency and is therefore of high addictive potential. Respiratory problems leading to death have been reported in people who combine alcohol and clomethiazole. However, intravenous infusion of clomethiazole may be the treatment of choice for the most severe withdrawal syndromes seen in Tier 4 services (Reference MorganMorgan, 1995). Among the benzodiazepines, there is a strong argument to choose chlordiazepoxide as the first-line drug. It is slowly absorbed, has a long half-life and low potency and is therefore of low addictive potential. There is some margin of safety when alcohol is taken along with chlordiazepoxide. It has unique metabolites so that supplementation with other benzodiazepines can be identified from toxicology screening, which may be of benefit where patients are polydrug users. The particular properties of other benzodiazepines may commend them for use in certain circumstances. For example, oxazepam can be useful where there is liver insufficiency, or lorazepam, which is well absorbed intramuscularly, is useful to achieve a loading dose rapidly.
As the severity of withdrawal increases, so does the likelihood of additional medical conditions. The rule of thumb is to treat these according to standard therapy (see Box 5). For example, where hallucinations are a feature of withdrawal then haloperidol is the treatment of choice. Somewhat different considerations apply when assessing nutritional status. People who misuse alcohol are at particular risk of Wernicke's encephalopathy, because they have low storage levels of thiamine and because the metabolism of alcohol requires significant amounts of thiamine. Where there is any suggestion of dietary neglect or in any case where there is a high withdrawal score, there is strong evidence in favour of giving multi-vitamin supplements containing at least thiamine 300 mg daily and magnesium (Reference Cook and ThomsonCook & Thomson, 1997).
Box 5. Common adjunctive medication
-
• Hypertension: beta-blockers
-
• Seizures: carbamazepine
-
• Hallucinations: haloperidol
-
• Poor nutrition: thiamine and magnesium
Audit
Most patients receiving treatment for alcohol dependence at some time enter a detoxification programme. Achieving successful detoxification is an important part of the overall treatment plan. Failure in detoxification is likely to engender a sense of hopelessness among both patients and staff. Significant resources are used for detoxification. For all these reasons, it is important that an effective audit system is in place. Audit should be a routine part of practice in specialist units, but is more difficult to organise in general psychiatry or primary care settings.
On the face of it, detoxification has a clearly defined end-point - being alcohol-free - and is therefore easy to evaluate. Certainly, it is important to know how many people successfully become alcohol-free, but equally it is important to know what quality of detoxification was delivered. There is a further problem in that most clinicians see completion of detoxification, that is reaching an alcohol-free state, to be an unsatisfactory end-point. Although not strictly part of detoxification, it is certainly part of the overall programme to see that effective steps have been taken to prevent relapse in the immediate post-detoxification period. Exactly what these steps might be varies from one service to another but might, for example, include prescribing disulfiram and ensuring attendance at an after-care appointment. Table 2 summarises the audit measures used by the Leeds Addiction Unit. A follow-up at one month post-detoxification has been judged to be a long enough time period to check that the detoxification team succeeded in starting after-care plans, but a short enough period that the outcome will not be unduly contaminated by factors beyond the control of the detoxification programme.
Conclusion
Detoxification is not usually a technically difficult procedure. Whether detoxification is an expedience, or part of a planned care programme, it is always an opportunity to help people change their drinking behaviour. There is a persuasive argument in favour of selecting chlordiazepoxide as the first-line pharmacotherapy for most alcohol withdrawal problems. Other benzodiazepines have equal efficacy and may be preferred by clinicians, but their pharmacokinetics are generally less suitable than those of chlordiazepoxide. It may be necessary to prescribe high doses in order to achieve rapid containment of the withdrawal syndrome.
What has changed in recent years is the pattern and range of alcohol treatment services. There has been a broadening of the base of treatment both in terms of the settings in which it commonly occurs and also the variety of staff now involved in therapy. This all means that integrating detoxification into an overall care plan becomes more difficult. Wherever practical, detoxification followed by a 3- to 4-week period of abstinence from psychoactive drugs should precede making any definitive diagnosis or commencing treatment for mental illness.
Multiple choice questions
-
1. Where depression and anxiety are prominent pre-detoxification features, they:
-
a should be treated with standard pharmacotherapy
-
b should receive an ICD diagnosis immediately
-
c commonly disappear three weeks post-detoxification
-
d indicate the need for in-patient detoxification
-
e predict drop-out from detoxification.
-
-
2. The following items are part of the Windsor Clinic Alcohol Withdrawal Assessment Scale that predict serious withdrawal problems:
-
a quality of contact
-
b tremulousness
-
c thought disturbance
-
d seizures
-
e pulse rate.
-
-
3. Severe withdrawal is often associated with the following medical complications:
-
a Wernicke's encephalopathy
-
b magnesium deficiency
-
c hyperglycaemia
-
d hypotension
-
e polydrug use.
-
-
4. Preparation for detoxification should include:
-
a checking the patient is at the determination or action stage of change
-
b planning the post-detoxification week
-
c identifying a support person
-
d agreeing the detoxification regimen
-
e making an after-care appointment.
-
-
5. The following can be considered as suitable first-line drugs for detoxification:
-
a carbamazepine
-
b chlordiazepoxide
-
c clomethiazole
-
d chlorpromazine
-
e clonidine.
-
Table 1 A fixed protocol for a chlordiazepoxide withdrawal regimen
| Morning | Midday | Evening | Night | Total daily dose | |
|---|---|---|---|---|---|
| Day 1 | 30 mg | 30 mg | 30 mg | 30 mg | 120 mg |
| Day 2 | 30 mg | 20 mg | 20 mg | 30 mg | 100 mg |
| Day 3 | 20 mg | 20 mg | 20 mg | 20 mg | 80 mg |
| Day 4 | 20 mg | 10 mg | 10 mg | 20 mg | 60 mg |
| Day 5 | 10 mg | 10 mg | 10 mg | 10 mg | 40 mg |
| Day 6 | 10 mg | 10 mg | 0 | 10 mg | 30 mg |
| Day 7 | 10 mg | 0 | 0 | 10 mg | 20 mg |
Table 2 Leeds Addiction Unit - alcohol detoxification audit schedule

| Pre-detoxification | Day 1 to end day | End day | 1 month |
|---|---|---|---|
| Age | Windsor Clinic | Adverse events | Current intake |
| Gender | Rating Scale | Total number of days | Medication |
| LDQ | Pulse and blood pressure | Drop-out/completion | LDQ |
| SSQ | Medication | Disulfiram | SSQ |
| GHQ | Side-effects | Keyworker appointment date | GHQ |
| Current intake | Therapist contact | ||
| Duration | Psychiatric diagnosis | ||
| Other drugs | Treatment satisfaction questionnaire | ||
| Medication | |||
| Blood screen | |||
| Urine toxicology screen | |||
| Illnesses | |||
| Detoxification preparations | |||
| Stage of change | |||
| Setting |
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | T | a | F |
| b | F | b | F | b | T | b | T | b | T |
| c | T | c | T | c | F | c | T | c | F |
| d | F | d | T | d | F | d | F | d | F |
| e | F | e | F | e | T | e | T | e | F |





eLetters
No eLetters have been published for this article.