The literature on physical examination in psychiatric practice is sparse, much is dated and from overseas, and so of limited use in extrapolation to current practice in the UK. British studies have reported the recording of physical examination carried out on admission by psychiatric trainees to be ‘uniformly poor’ (Reference Rigby and OswaldRigby & Oswald, 1986) or ‘variable’ (Reference Hodgson and AdeyemoHodgson & Adeyemo, 2004). The earlier study found that significant positive findings were unrecorded, especially in the neurological and locomotor systems. The recent study showed little progress, with under 60% of patients having a comprehensive central nervous system (CNS) examination.
Why should psychiatrists be able to do a physical examination?
Age-adjusted annual death rates from all causes among psychiatric patients are 2–4 times higher than in the general population (Reference Harris and BarracloughHarris & Barraclough, 1998), with higher rates of physical disorder across the entire range of mental disorders.
The risks of reliance on the belief that the patient’s general practitioner or other referring doctor will have done a thorough examination have been emphasised (Reference SternbergSternberg, 1986). It has been reported that between 6 and 20% of patients with physical illness are misdiagnosed as having mental disorder (Reference KoranyiKoranyi, 1979; Reference Koran, Sox and MartonKoran et al, 1989). This discrepancy may be due to the fact that patients who are mentally disturbed may be unable to give a clear account of their symptoms, even in the presence of a life-threatening disorder (Reference KampmeierKampmeier, 1977). Studies have shown that, in many cases, physical diseases will not be diagnosed and treated when a patient is admitted to a psychiatric unit (Reference Felker, Yazell and ShortFelker et al, 1996; Reference Moos and MertensMoos & Mertens, 1996), which has potentially serious implications for patients’ overall health, delaying recovery and increasing length of stay. Consequently, an important aspect of psychiatric evaluation is differentiating organic disease from ‘functional’ psychiatric disorders. A competent assessment of patients’ physical health also helps to tailor drug use and reduce the risk of side-effects. Additionally, it gives a clear baseline for comparison, should a patient’s physical state change, thus informing the clinician of the severity of the effect of a drug and of the need for action.
Therefore, there appears to be compelling evidence that care of people with mental illnesses should encompass physical as well as mental healthcare. How can this be achieved and what barriers are there to overcome?
Barriers to overcome
Attitudes
Many psychiatrists have not used a stethoscope, let alone done a physical examination, for many years. Past surveys reported that most psychiatrists did not examine their patients routinely (Reference McIntyre and RomanoMcIntyre & Romano, 1977; Reference Summers, Munoz and ReadSummers et al, 1981; Reference Krummel and KatholKrummel & Kathol, 1987) and that a third had little confidence in their ability to do so (Reference McIntyre and RomanoMcIntyre & Romano, 1977), or believed that it should be done by a physician other than a psychiatrist (Reference Victoroff, Mantel Jnr and BailettiVictoroff et al, 1979). There is little evidence to show that the situation has changed. Thus, it is likely that many psychiatrists practice without any clear knowledge of their patients’ physical health and its impact on mental health or vice versa.
Isolation from acute health services
At present, national policy is for mental health services to be managed separately from other health services. The establishment of small in-patient units in the community is likely to lead to physical estrangement from medical colleagues and investigative support services, which are usually based in acute hospitals. As a consequence, service level agreements between acute and mental health trusts, which were designed to offer reciprocal and complementary services, may no longer be practicable.
Training
With the exception of vocational training in general practice, postgraduate medical training programmes are increasingly focused on specialty, which may be to the detriment of holistic patient care. As a consequence, the mental disorders of mentally ill patients may deter clinicians in acute hospitals from adequately managing medical illness, and diagnosis and treatment of a physical disorder may be overlooked by their counterparts in psychiatric services (Reference Bunce, Jones and BadgerBunce et al, 1982).
The MRCPsych Part I
The Royal College of Psychiatrists has been proactive in placing greater emphasis on retention of the skills of physical examination. The objective structured clinical examination (OSCE) in Part I of the College’s membership examinations (the MRCPsych) has at least one physical examination station in each circuit. As the bank of stations increases, there will be greater opportunity to assess skills in physical examination, with an emphasis on trainees demonstrating their ability to elicit signs from a number of systems in order to substantiate a clinical diagnosis.
The general physical examination
Physical examination should not be conducted in isolation from systemic enquiry. Just as a good psychiatric history informs our examination of mental state, so a good working knowledge of internal medicine, systemic enquiry and medical history help in focusing the physical examination. The essence of a skilled physical examination is not an immaculate examination of the various organs in isolation from each other. Rather, it is that clinicians use their knowledge selectively to inform an efficient search for signs from different systems to confirm or support a diagnosis.
Equipment and environment
Essential to a good physical examination are privacy, peace, light, warmth and good equipment (Table 1). Unfortunately, many psychiatrists work in offices or wards without examination couches and without basic equipment such as stethoscopes, sphygmomanometers or ophthalmoscopes.
Table 1 Equipment

| Essential | Desirable |
|---|---|
| Examination couch | Auroscope |
| Stethoscope | Alcometer |
| Sphygmomanometer | Oximeter |
| Thermometer | Neurological testing pins |
| Tendon hammer | Snellen chart |
| Tuning fork (256 Hz) | Height measure |
| Weighing scales | Disposable gloves |
| Urinalysis sticks |
Chaperones
Anything more than cursory examination of appearance, pulse or blood pressure should be conducted with a chaperone. A female member of staff should always accompany male doctors when examining a female patient. It is my view that the advice to be chaperoned should equally apply to female psychiatrists examining male patients, not just to prevent allegations of assault on the patient, but also to avoid assault by the patient. This precaution is of particular relevance when patients are intoxicated with alcohol or other substances or are elated, and as a consequence may be sexually disinhibited.
Timing
Ideally, physical examination should be carried out as part of the admission procedure. A survey of physical examination suggested that there is often a delay, with a mean of 62 h after admission and as long as 612 h (25.5 days) in some cases (Reference Hodgson and AdeyemoHodgson & Adeyemo, 2004). Although delay may be justified because of the patient’s mental state, reasons for the delay should be recorded clearly.
Observation
Knowledge of a patient’s weight is extremely important. It is obviously vital in anorexia nervosa, but it also helps to confirm the extent of weight loss due to neglect in a patient with psychosis and of weight variation in depression. Furthermore, a weight chart provides an important indicator of weight gain due to psychotropic drugs or dietary intake during admission.
Presence or absence of cyanosis should be noted. Although peripheral cyanosis is not unusual in patients with chronic cardiac or respiratory disorders, central cyanosis should alert the clinician to serious underlying physical problems and the need for urgent medical intervention. A foreign body should be suspected, especially in the elderly, those with swallowing disorders, conditions such as Huntington’s chorea and patients on neuroleptics. Rapid diagnosis in such circumstances is vital.
Anaemia as suggested by pallor of palmar creases and subconjunctiva may be seen in patients with a history of chronic self-neglect and poor dietary iron or folate intake due to illnesses such as depression, schizophrenia and anorexia nervosa. Very occasionally, anaemia in a patient with dementia results from vitamin B12 deficiency, which may be associated with other signs of autoimmune disorder such as vitiligo, alopecia and thyroid disease.
Complexion, a feature rarely mentioned in mental health texts, is often altered in depression, when it may appear sallow and grey. Plethora, while explicable in a landworker exposed to the elements, should alert the clinician to the possibility of alcohol misuse, and thus prompt a search for associated physical signs and mental health symptoms. Rashes due to medication are common, either as predictable responses such as photosensitivity to chlorpromazine or idiosyncratic responses to drugs such as fluoxetine. A true butterfly rash is rare. Its presence in association with an unusual mental health picture should prompt the clinician to look for other physical signs of systemic lupus erythematosus, a condition which is confirmed readily by investigation and is responsive to steroids, rather than psychotropics alone. Jaundice may be due to liver disease secondary to alcohol misuse, but can arise from use of a variety of psychotropic agents, some of which cause hepatitis, whereas others, such as chlorpromazine, cause cholestasis (British Medical Association & Royal Pharmaceutical Society of Great Britain, 2004). A lemon tinge to the skin may be seen in a patient with dementia secondary to vitamin B12 deficiency, and a bronze complexion is classically associated with haemochromatosis.
Examination of the hands and arms can also be informative. Although possession of a tattoo is increasingly prevalent in the British population, certain types of tattoo, in particular letters over the knuckles and collars around the neck, are commonly believed to have an association with psychopathy (Reference MacleodMacleod, 1983). These should alert the clinician to look for signs of substance misuse, such as needle tracks, to take particular care with venesection and to gain corroboration of the history. Splinter haemorrhages are rare, but should also raise concern in the intravenous drug misuser. Palmar erythema, Dupuytren’s contractures and clubbing should all raise suspicion of liver disease in a patient with depression or psychosis who professes abstinence or moderation. The development of clubbing in a patient who is a heavy smoker may suggest a lung cancer and the need for an urgent chest X-ray and possible referral.
Examination of the oral cavity is important in patients with mental illnesses, since dental hygiene and need for treatment are commonly neglected.
Palpation
A handshake is not only a mark of courtesy, but also a potential source of information. A warm, sweaty palm may give some clues about endocrine disorders such as thyroid disease or acromegaly. A fine tremor helps to add weight to a clinical diagnosis of thyrotoxicosis, whereas cold tremulous hands are seen in anxiety disorders. Tremor may be caused by medication such as lithium and neuroleptics. A symmetrical coarse tremor associated with the latter, together with bradykinesia and rigidity, suggest iatrogenic parkinsonism. Asymmetric signs, in the absence of medication, point to primary Parkinson’s disease, which is commonly associated with depressive disorder, but may also be associated with Lewy body dementia, especially if there are signs of autonomic instability.
Lymphadenopathy is not common in patients with mental health problems. However, it can be a feature of tuberculosis, to which people with mental health problems may be susceptible on account of self-neglect and living in institutional settings. Both tuberculosis and lymphoma are complications of HIV infection, which is known to be associated with cognitive impairment, especially in the later stages of the illness. An enlarged supraclavicular lymph node in a patient who smokes should raise suspicion of a bronchogenic carcinoma, and should indicate close examination of the chest and chest X-ray. Axillary lymphadenopathy may be a sign of metastatic breast disease. Examination of the breasts is an important part of the physical examination.
Examination of individual systems
Cardiovascular examination
Observation of the jugular venous pressure (JVP) is a conventional part of the cardiovascular examination, and should be carried out with the patient lying at an angle of 45°. In normal circumstances the venous pulse should be seen just above the clavicle, and will become more prominent with the patient lying flatter or with pressure placed over the right upper quadrant of the abdomen. Patients with congestive cardiac failure, other causes of right heart failure or vena caval obstruction will have a raised jugular venous pressure.
Presence of oedema should be noted: it is an important sign in congestive cardiac failure, but also may be due to hypoalbuminaemia resulting from liver disease. Rarely, it is seen in anorexia nervosa.
The importance of the baseline pulse, its rate and rhythm, and of blood pressure cannot be overstated. These simple measures often give valuable information about the patient’s physical well-being and provide comparators, should the patient’s health suddenly deteriorate. The nature of the pulse is particularly important in a number of conditions (Table 2). Blood pressure is also an essential baseline measurement. However, high readings seen on admission may be due to heightened arousal, and it is appropriate to monitor the blood pressure over a number of days before instituting medication or a referral for advice. Hypertension is usually essential, but it is also associated with alcohol misuse, thyroid disorder, clozapine therapy or high doses of venlafaxine, and renal failure. The latter should be considered if a patient on long-term lithium therapy develops hypertension, and proteinuria is a particularly ominous sign, but easy to detect with dipsticks.
Table 2 Importance of pulse

| Sign | Potential association |
|---|---|
| Sinus tachycardia | Infection, hyperthyroidism, autonomic instability and arousal, neuroleptic malignant syndrome |
| Bradycardia | Clozapine therapy, anorexia nervosa, hypothyroidism, tricyclic antidepressants |
| Atrial fibrillation | Hyperthyroidism, vascular dementia |
| Arrhythmias | Tricyclic antidepressants, some antipsychotics, lithium |
Phaeochromocytoma, a much loved subject of multiple choice questions, is extremely rare, but commonly considered, especially in patients with panic disorder who have resorted to alcohol to reduce anxiety. Urinary glucose may suggest a phaeochromocytoma, although 24-hour urinary adrenaline and noradrenaline are the definitive tests.
Hypotension is seen in anorexia nervosa and Addison’s disease. Postural hypotension is seen in autonomic dysfunction associated with diabetes mellitus and Lewy body dementia, as well as being an unwanted side-effect of chlorpromazine and tricyclic antidepressant treatment.
A swinging blood pressure, particularly in association with tachycardia and pyrexia, should raise the possibility of either acute intermittent porphyria or neuroleptic malignant syndrome. Fortunately, both are extremely uncommon. In the former, there is association with abdominal pain and darkening of urine left to stand. The latter usually occurs with neuroleptic treatment, particularly with rapid escalation of dose, and is also associated with muscle rigidity and raised creatine kinase levels.
The apical beat is best felt with the patient leaning forward. A thrusting beat should alert the clinician to the possibility of established hypertensive left ventricular hypertrophy or, more rarely, cardiomyopathy. Heart sounds and added sounds or murmurs should be noted. In particular, a mid-diastolic murmur due to mitral stenosis, with or without atrial fibrillation, is an important finding if a vascular dementia is suspected, since further vascular events may be reduced by anticoagulation and control of the rhythm disturbance. Murmurs may also be heard in bacterial endocarditis, which should be suspected in pyrexial patients with splinter haemorrhages, clubbing and a history of intravenous drug misuse.
Last, and of particular importance when a vascular aetiology is suspected, peripheral pulses should be systematically palpated and the perfusion of the extremities should be observed. This cannot be done through socks. As I have already said, patients with mental illnesses neglect themselves. An aversion to smelly socks is not an excuse for failing to examine the feet, which may be unkempt and simply in need of a chiropodist, or may have evidence of ischaemia. The presence of bruits, especially in the carotid and femoral arteries, should be sought if there is suspicion of a vascular disease.
Respiratory examination
A history of smoking, cough, recurrent respiratory tract infections, purulent sputum or haemoptysis should prompt the clinician to do a thorough examination of the chest. Tracheal deviation, symmetry of chest expansion and percussion, breath sounds and added sounds should all be recorded. Abnormalities should be followed up by chest X- ray.
Gastrointestinal system
Examination of the abdomen should always be carried out with the patient lying flat, unless they suffer from cardiac failure. Abdominal examination is important when alcohol misuse is suspected. Distended veins around the umbilicus (caput medusae) are an uncommon finding, but suggest portal hypertension due to cirrhosis. The abdomen itself may be distended owing to ascites, which can be confirmed by dullness on percussion in the flanks which shifts if the patient moves onto one side. The liver, which should normally extend to a fingerbreadth below the costal margin, may be enlarged and tender in the early stages of cirrhosis, or hard and shrunken once the disorder is established. Other signs of portal hypertension are splenomegaly and haemorrhoids.
Neurological examination
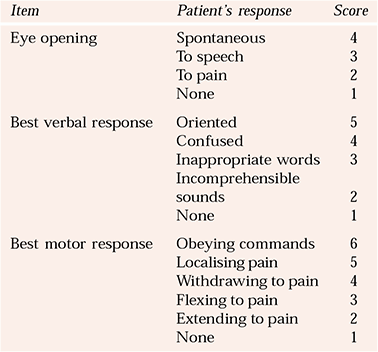
The principle objective of a neurological examination is localisation. A working knowledge of neuroanatomy greatly helps the clinician in conducting the examination. Neurological and mental state examination overlap, in that conscious level, orientation, memory, higher intellectual function and speech are common to both. The conscious level on admission should be recorded in all cases, as this gives an important baseline should the patient’s conscious state change. The Glasgow Coma Scale (Reference Teasdale and JennettTeasdale & Jennett, 1974) is easy to use and widely accepted throughout the UK (Table 3). Memory and intellectual function will influence the reliability of a history and ability to cooperate with further examination.
Table 3 The Glasgow Coma Scale (Reference Teasdale and JennettTeasdale & Jennett, 1974)
| Item | Patient’s response | Score |
|---|---|---|
| Eye opening | Spontaneous | 4 |
| To speech | 3 | |
| To pain | 2 | |
| None | 1 | |
| Best verbal response | Oriented | 5 |
| Confused | 4 | |
| Inappropriate words | 3 | |
| Incomprehensible sounds | 2 | |
| None | 1 | |
| Best motor response | Obeying commands | 6 |
| Localising pain | 5 | |
| Withdrawing to pain | 4 | |
| Flexing to pain | 3 | |
| Extending to pain | 2 | |
| None | 1 |
Speech is another important baseline assessment, as symptoms cannot be communicated readily without it. Dysphasia, be it receptive or expressive, is a key localising sign. However, it is important to establish whether the patient is right- or left-handed, as this helps to determine cerebral dominance and the location of speech areas. Conventional neuroleptics can cause dysarthria, as can anticonvulsants in high doses. Cerebrovascular disease, multiple sclerosis, cerebellar disease and tardive dyskinesia may also be associated with dysarthria.
Full neurological examination, which takes about 40 min, should be conducted in a systematic manner, starting with examination of the cranial nerves, then sensation, then the motor system and coordination. Reflexes are usually tested at the end. Although full neurological examination might be desirable, it is often not done, even in specialist settings. In practice, particularly in the out-patient clinic, a brief assessment is all that is possible. The next section presents an assessment that can be performed in about 3 min, as long as the method is understood. Once this assessment has been done, there can be reasonable certainty that there is no major brain pathology.
The 3-minute neurological examination
The examination begins with Romberg’s test (steps 1 and 2 in Box 1). It is usual for normal people to waver slightly when their eyes are closed. Some patients may wobble a great deal with this test. A number of these people have non-organic disease and usually perform the tandem test (heel–toe) without difficulty.
Box 1 Quick neurological examination
The patient should be asked to do the following:
-
1 Stand with feet together
-
2 Close eyes
-
3 Open eyes and walk heel to toe in a straight line forwards and backwards
-
4 Walk on tiptoes and then on heels
-
5 Hold their arms outstretched with palms facing upwards
-
6 Hold this position for a few seconds
-
7 With eyes closed, touch the nose with the tip of the index finger that the examiner has just lightly touched. Then touch the nose with the tip of the middle finger that the examiner has just lightly touched
-
8 Pretend to play the piano with the arms still outstretched
-
9 Pat the back of each hand with the opposite palm
-
10 While facing the examiner, screw eyes tight
-
11 Give a grin
-
12 Protrude the tongue
-
13 Wiggle the tongue
-
14 Stare at the examiner’s face and, as the examiner wiggles one finger in each outer quadrant on the left, then on the right and then wiggles one finger on the left and right at the same time, the patient should point to the moving fingers
-
15 Follow the examiner’s finger, with head still: the finger should move across the mid-line to shoulder width on either side and then move up and down; this procedure should be repeated on the opposite side
-
16 Sit on the examining couch while the examiner tests the patient’s reflexes
-
16 Allow the examiner to examine the fundi with an ophthalmoscope
Walking on the heels and then the toes (steps 3 and 4) is a useful test of plantar and dorsiflexion.
With the drift test (steps 5 and 6), normal people are able to hold their pronated arms outstretched and in the same position. Patients with a left-hemisphere lesion may show flexion of the right arm. If there is neglect, there may be downward drift.
In testing light touch and coordination (step 7), the patient’s index finger on one hand and the middle finger on the other should be touched, and then the patient should be asked to touch their nose with the tip of each of these fingers.
Fine finger movement is a useful test of extrapyramidal function.
Rapid tapping movements (step 8) are a good screen for ataxia. If the patient has difficulties in doing this, you can then test the more difficult way by asking them to tap rapidly and alternately the back and palm of each hand with the back and palm of the opposite hand (step 9). Most people perform this test better with their dominant hand.
Asking the patient to close their eyes, bury their eyelashes and then to give a grin (steps 10 and 11) can be used to assess muscles innervated by the facial nerve. The patient’s face should be watched closely for signs of asymmetry. On opening the eyes, it should be noted whether the pupils constrict. The presence of Horner’s syndrome can be checked by looking for signs of ptosis, a slightly quizzical raising of the eyebrow and a constricted pupil. The latter is better seen in a darkened rather than bright room.
Rapid tongue movements (steps 12 and 13) test for presence of pseudobulbar palsy.
The first part of step 14 (wiggling a finger in the outer quadrants to the left and then to the right of the head) achieves adequate visual-field screening. The second part of step 14 (wiggling a finger on both sides of the head at the same time) tests for inattention. If any abnormality is observed, the visual fields must be assessed more thoroughly using a red pin by the standard confrontation method described by Reference MacleodMacleod (1983).
Step 15 tests for occulomotor palsies (cranial nerves III, IV and VI) and nystagmus.
Reflexes should be tested while the patient’s limbs are in a relaxed position (step 16). Lateralising signs indicating an upper (increased reflexes) or lower (diminished reflexes) motor neurone problem should be looked for.
Step 17 looks for papilloedema, optic atrophy and system vascular disease (e.g. diabetes or hypertension).
If the 3-minute neurological examination is performed, it is important to follow up any abnormality with a more detailed neurological examination pertaining to it. Reference MacleodMacleod (1983) and specialist neurological texts (Reference Bickerstaff and SpillaneBickerstaff & Spillane, 1989; Reference KaufmanKaufman, 1995; Reference Malhi, Matharu and HaleMalhi et al, 2000) give excellent descriptions of appropriate methodology.
The extrapyramidal system
Specific attention should be paid to the extrapyramidal system. Abnormality on inspection (abnormal movements and poverty of movement), testing of tone (lead pipe or cogwheel rigidity) and assessment of gait (festinant) should all be noted.
Abnormal involuntary movements and general neurological impairment have been reported in neuroleptic-naïve patients (Reference Manschreck, Keuthen and SchneyerManschreck et al, 1990; Reference Ismail, Cantor-Graae and McNeilIsmail et al, 2001). The presence of extrapyramidal signs seems to predict acute extrapyramidal side-effects of typical neuroleptic drugs, such as rigidity, tremor, akathisia and dystonia (Reference Chatterjee, Chakos and KoreenChatterjee et al, 1995). Hyperkinetic signs in neuroleptic-naïve patients, in addition to abnormalities of manual dexterity and coordination, may prove useful in assessing vulnerability to tardive dyskinesia (Reference Sanders, Keshavan and GoldsteinSanders et al, 2003).
The sensory system
Examination of the sensory system needs a lot of cooperation from the patient and is less objective, as it depends on patient report rather than the clinician’s observations. Sensation is conventionally tested in two anatomical groups. Neurons conducting sensations of vibration and proprioception are situated in the dorsal columns. These tracts are affected in vitamin B12 deficiency and syphilis. Vibration is also affected in diabetic neuropathy. Sensation of pain, pinprick and light touch is conducted in the spinothalamic tracts. It is helpful to know where each dermatome is located, as this can help with localisation. It is also a useful way of discriminating between functional and organic lesions, since the former may not follow a recognised dermatomal pattern.
The motor system
In examining the motor system, attention should be paid to the pattern of any weakness, as opposed to its extent or severity, because this is more likely to indicate the origin of the weakness. There are three essential patterns:
-
1 weakness on one side of the body (hemiplegia) is indicative of contralateral brain damage;
-
2 weakness of both legs (paraparesis) suggests spinal cord damage or, rarely, a parasagittal meningioma;
-
3 weakness limited to the distal portions of the limbs is a feature of damage to the peripheral nervous system rather than to the central nervous system.
Hoover’s sign is particularly useful in patients with medically unexplained hemiparesis. While lying supine on a couch, the patient is first asked to raise the affected leg as the examiner holds a hand under the heel of the opposite leg. The examiner should be able to raise the heel of the affected leg because the patient is exerting so little downward force with this leg. The patient is then asked to raise the unaffected leg while the examiner holds a hand under the heel of the ‘paralysed’ leg. Intact strength in the affected leg is revealed as it is unconsciously forced down.
Reflexes
The tendon reflexes should be graded (Table 4). Sluggish reflexes, particularly with a delayed relaxation phase, should prompt tests for hypothyroidism. Hyperreflexia is seen with upper motor neuron lesions. Absent reflexes are seen with lower motor neuron lesions or peripheral neuropathy, such as that associated with diabetes mellitus and alcohol misuse. Plantar reflexes should also be tested; an upgoing plantar (Babinski’s sign) indicates upper motor neuron pathology, which may be located in the spinal cord or brain.
Table 4 Grading of tendon reflexes

| Tendon reflex | Grade |
|---|---|
| Very brisk | +++ |
| Brisk | ++ |
| Normal | + |
| Absent | 0 |
| Present with reinforcement | +/− |
| Clonus | cl |
The uncooperative patient
Lack of facilities, time and poor cooperation are common reasons for failure to examine patients in psychiatric units. However, external inspection can be carried out in environments with minimal facilities, with little or no cooperation from the patient, and it provides opportunity to learn about the physical state and what systems may be of particular importance when more comprehensive physical examination and investigation is permitted. Both in physical medicine specialties and in psychiatry, examination should start as soon as the patient is met. The cleanliness and state of clothing may give clues about the level of self-care. Dentition can usually be seen without physical examination, and obvious neglect in this area should prompt the clinician to examine visual acuity, hearing and foot care, when the patient permits. Observation should also give some clue as to the nutritional status of the patient, although baggy or eccentric clothing may mask emaciation. A bulge in the neck and exophthalmos might indicate thyroid disease. Facial expression, although an integral part of the mental state examination, may also point to underlying physical problems such as endocrine disorders, Parkinson’s disease and other neurological illness. Tardive dyskinesia or other extrapyramidal signs are often evident at initial assessment. Observations of gait may also indicate neurological or psychomotor disturbance and, in particular, the effect on function.
If the patient is standing upright, is shouting or able to talk without becoming breathless, the airway is probably intact, he or she is not likely to be severely hypotensive and is likely to have reasonable respiratory function.
How to maintain skills
However detailed a text on physical examination may be, it is no substitute for observation of clinical examination being performed by an expert, either in person or on video. It is my view that every training scheme should invest in audio-visual aids on physical examination for trainees, or should invite a local physician to conduct a session during which trainees can both observe and be observed.
What about more senior clinicians? At present there is no consensus on how to maintain competence in physical examination, and there are no guidelines either. Competence in basic resuscitation, a core medical skill, falls far short of requirement to conduct competently a physical examination. Attendance at medical case presentations is a useful way of refreshing knowledge. However, it does not maintain examination skills, and the only way to do so is to perform physical examinations regularly.
MCQs
-
1 The following are often neglected by patients with mental disorders:
-
a teeth
-
b eyes
-
c feet
-
d diet
-
e hygiene.
-
-
2 Stigmata of liver disease include:
-
a splinter haemorrhages
-
b spider naevae
-
c jaundice
-
d ascites
-
e cyanosis.
-
-
3 Complications of diabetes include:
-
a absent foot pulses
-
b peripheral neuropathy
-
c auditory impairment
-
d ankle oedema
-
e gangrene.
-
-
4 Hypertension is associated with:
-
a left ventricular hypertrophy
-
b venlafaxine
-
c carcinoid syndrome
-
d alcohol misuse
-
e liver failure.
-
-
5 Extrapyramidal side-effects include:
-
a tremor
-
b clasp-knife rigidity
-
c hypotonia
-
d abnormal fine finger movements
-
e bradykinesia.
-
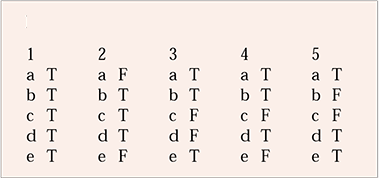
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | F | a | T | a | T | a | T |
| b | T | b | T | b | T | b | T | b | F |
| c | T | c | T | c | F | c | F | c | F |
| d | T | d | T | d | F | d | T | d | T |
| e | T | e | F | e | T | e | F | e | T |







eLetters
No eLetters have been published for this article.