In the aftermath of traumatic events, individuals are left with a host of easily reactivated neurobiological responses and an inadequate memory record (Reference Van der Kolk, McFarlane and Weisaethvan der Kolk 1996, Reference Van der Kolk and Shapiro2002). They report intense emotional responses without words and with no apparent connection to any precipitant or past experience. Long after the events have ended, traumatised individuals continue to experience intense emotions of fear, shame and rage, numbing of feelings and body sensation, loss of physical energy or chronic agitation and an inability to take purposeful action. Painful negative beliefs about the self often further intensify the distressing feelings and bodily responses (Reference Van der Kolk, McFarlane and Weisaethvan der Kolk 1996; Reference Courtois and FordCourtois 2009), affecting posture, breathing, freedom to move, and even heart rate and respiration.
Autonomic effects of trauma
It is well established that exposure to threat or danger stimulates autonomic nervous system activity governing animal defence survival responses such as fight, flight, freezing and total sub mission (Reference van der Kolk and Fislervan der Kolk 1995, Reference Van der Kolk, McFarlane and Weisaeth1996; Reference LeDouxLeDoux 2002; Reference PorgesPorges 2003; Reference Ogden, Minton, Pain and NortonOgden 2006a,Reference Ogden, Pain and Fisherb). Fight and flight responses are driven by the sympathetic branch of the autonomic nervous system via nor adrenaline release, increasing heart rate and respiration and maximising oxygen flow to muscle tissue. The parasympathetic branch of the autonomic nervous system, stimulated concurrently via the release of cortisol (Reference LeDouxLeDoux 2002), is characterised by rapid metabolism of adrenergic neurochemicals, lower than normal heart rate and respiration, loss of energy, exhaustion and numbing, facilitating total submission responses necessitated by inescapable danger. Freeze responses are characterised by high sympathetic activation coupled with physical immobility and are often implicated in date rapes in which the victim is unable to speak or resist.
Because observation or ref lection might negatively affect reaction time in the face of danger, the body responds automatically, often without conscious intention or awareness. Cortical activity is automatically inhibited to facilitate instinctual responding (Reference LeDouxLeDoux 2002). However, instinctive engagement of ‘bottom-up’ defensive responses compromises the individual's ability to perceive and process the entirety of the experience and interferes with memory encoding and cause–effect perception.
Psychiatric consequences of traumatic exposure
Subsequently, the body becomes sensitised to the particular stimuli associated with each traumatic experience: when individuals later face a reminder of that event or potential danger cue, the body responds with the same defensive responses that were previously adaptive and effective whether or not they are still appropriate (Reference Van der Kolk, McFarlane and Weisaethvan der Kolk 1996).
In the aftermath of prolonged trauma and/or early attachment failure, it is common for individuals to experience chronic alterations in autonomic nervous system responsiveness to daily life stress and especially to any subtle or obvious reminder of the traumatic events (Box 1). With a nervous system that does not easily recover from either heightened states of emotion or states of depression and numbing, survivors of trauma often report difficulty with affect regulation (Reference Van der Kolkvan der Kolk 2006). Autonomically driven emotional arousal may feel overwhelming and unmanageable or affect may be blunted, disconnected and numbed. Maintaining a state of calm or well-being can be challenged by heightened sensitivity to trauma-related stimuli. Patients report being driven by powerful internal forces to impulsive action or finding themselves frozen in terror or inexplicably collapsed and passive. Non-threatening situational cues reminiscent of the traumatic event or its context may activate sympathetic nervous system activity and fight–flight responses, whereas dangerous situations paradoxically elicit parasympathetic non-responsiveness and obliviousness to personal safety (Reference Herman and NortonHerman 1992).
BOX 1 After-effects of trauma and/or early attachment failure
-
• Defensive responses to trauma reminders or potential danger cues
-
• Autonomic nervous system alterations to stress and trauma-related stimuli responses
-
• Affect dysregulation (emotional arousal or numbing)
-
• Trauma-related disorders:
-
chronic depression
-
anxiety
-
chronic post-traumatic stress disorder
-
bipolar disorder
-
borderline personality disorder
-
-
• Secondary symptoms:
-
addictive disorders
-
eating disorders
-
self-destructive behaviour
-
suicidality
-
When the traumatic experiences have been chronic over many years or have occurred in the context of ‘enduring conditions’ (Reference SaakvitneSaakvitne 2002) of physical, emotional or sexual abuse coupled with neglect, the body and nervous system develop habitual responses adaptive in a traumatogenic environment (e.g. automatic obedience, hypervigilance, loss of sensation, heightened tolerance for pain).
Repeated activation of the autonomic nervous system in response to trauma-related stimuli inter feres with subsequent development of affect regulation and predisposes traumatised individuals to a number of mental disorders: chronic depression or anxiety, chronic post-traumatic stress disorder (PTSD), bipolar disorder and borderline personality disorder (Reference Courtois and FordCourtois 2009). When patients with these disorders present with a history of trauma, neglect and/or attachment failure, treatment is often complicated by sensitivity to trauma-related stimuli and autonomic dysregulation, resulting in frequent crises and a vulnerability to decompensation and regression.
The treatment of trauma-related depressive disorders, anxiety disorders and PTSD is further complicated by the array of secondary symptoms associated with them that provide chemically or behaviourally induced autonomic regulation (Reference Ogden, Minton, Pain and NortonOgden 2006a,Reference Ogden, Pain and Fisherb). These include addictive disorders, eating disorders, self-destructive behaviour and suicidality. Traditional talking therapies (including psychodynamic psychotherapy, psychoanalytic methods, cognitive–behavioural therapy and exposure techniques) can effectively address the emotional, relational and cognitive symptoms of trauma-related disorders and/or manage the secondary symptoms to ensure patient safety, but traditional psychotherapy models generally lack techniques that directly treat the autonomic and somatic effects perpetuating the psychological symptoms.
Introduction to sensorimotor psychotherapy
It is in this arena that the use of sensorimotor psychotherapy can be invaluable in treating the autonomic and affective dysregulation that constitutes the symptomatic legacy of traumatic events. Developed in the 1980s by Pat Ogden as a body-centred talking therapy, sensorimotor psychotherapy is designed to specifically address both the cognitive–emotional aspects and the bodily and autonomic symptoms of traumatic stress and attachment-related disorders without requiring the use of hands-on interventions (Reference Ogden, Pain and FisherOgden 2006b; Reference Fisher, Ogden, Courtois, Ford and van der KolkFisher 2009). Consequently, it is a somatic approach easily integrated into all traditional in-patient and out-patient treatments for trauma-related disorders.
Sensorimotor psychotherapy incorporates approaches drawn from psychodynamic psychotherapy, gestalt therapy, cognitive–behavioural treatments and the Hakomi method of body psychotherapy (Reference KurtzKurtz 1990). Its theoretical principles stem from neuroscience research findings on the effects of traumatic experiences on the brain and body, and its interventions emphasise attention to modulation of autonomic arousal and reinstatement of adaptive responses (Reference Van der Kolk, McFarlane and Weisaethvan der Kolk 1996; Reference Van der Hart, Nijenhuis, Steele and Nortonvan der Hart 2006) (Box 2).
BOX 2 Sensorimotor psychotherapy – characteristics
-
• Somatic approach
-
• Backed by neuroscience research
-
• No need for the patient to remember the details of trauma in order to treat its effects
-
• Draws on psychodynamic psychotherapy, gestalt therapy, cognitive–behavioural therapy and body psychotherapy
-
• Focuses not only on cognitive and emotional symptoms but also on bodily and autonomic effects
-
• Used in treatment of trauma and attachment-related disorders
-
• Addresses intrusive symptoms, numbing and avoidance, and autonomic/affective dysregulation
Mindful narratives
A typical session begins as would most psychotherapy sessions: with a client's narrative. However, rather than using narrative techniques to ‘talk about’ the experience, the sensorimotor psychotherapist instead directs the individual's focus to the procedurally learnt patterns evoked by the recollection. As the patient speaks of the traumatic event, the therapist observes their emotional and bodily responses to ascertain how these experiences have been encoded non-verbally and autonomically (Reference Ogden, Minton, Pain and NortonOgden 2006a,Reference Ogden, Pain and Fisherb). Even when different individuals are exposed to the same traumatic event, their organisation of it will differ (Reference TerrTerr 1989).
Each traumatised individual uniquely encodes an event or events as some combination of images, smells, sounds, autonomic responses, visceral and muscular sensations, movements and impulses, emotions and cognitive and narrative components. This phenomenon accounts for the difficulty many traumatised patients report in recounting their traumatic experiences: their narrative memories are fragmented rather than sequential and evoke the intense physical and emotional non-verbal components of the experience rather than contributing to its resolution. Therefore, the sensorimotor psychotherapist focuses on increasing the client's non-judgemental awareness of persistent physical, cognitive and emotional responses evoked by the narrative or by trauma-related stimuli (Box 3).
BOX 3 The therapist's role in sensorimotor psychotherapy
-
• Fosters the patient's dual awareness or observing ego
-
• Teaches the patient to observe, understand and distance from trauma-related thoughts and bodily sensations/responses (mindful observation) rather than becoming overwhelmed and/or acting out in response
-
• Teaches the patient somatic skills to manage activation and/or reorganise their response patterns
-
• Helps the patient to experience the event as ‘over’ rather than ‘happening now’ (i.e. to differentiate past from present)
-
• Helps to facilitate the patient's ability to ‘uncouple’ neutral stimuli from trauma-related stimuli
-
• Regulates the autonomic nervous system to decrease re-experiencing and other intense emotional states connected with the traumatic event (i.e., uncoupling over-associating stimuli)
-
• Stabilises and reorganises responses of the patient's autonomic nervous system
The client is asked to mindfully notice rather than interpret or analyse the succession of thoughts, feelings and body sensations or movements that occur when thinking or talking about distressing events or emotions. This emphasis on mindful noticing of thoughts and feelings is often affectively and autonomically regulating in itself. Narrative re-telling of distressing experiences or overlearned interpretations of what happened (e.g. ‘It was my fault’) activate left hemisphere long-term memory areas and associated affects, resulting in emotional and autonomic reactivity, whereas curiosity and mindfulness activate the medial prefrontal cortex (Reference Davidson, Kabat-Zinn and SchumacherDavidson 2003), thought to be an integrative centre and the part of the brain responsible for interoception or internal awareness. The medial prefrontal cortex has deep connections to both cortical and subcortical areas, including the amygdala, the brain's emotional memory centre that facilitates its ability to regulate emotional and autonomic activity (Reference Van der Kolkvan der Kolk 2006).
Numerous brain-scan studies of individuals practising mindfulness meditation (Reference Creswell, Way and EisenbergerCreswell 2007) demonstrate a reciprocal relationship between activation of the medial prefrontal cortex and deactivation of the amygdala (i.e. regulation of arousal).
Innovative techniques and interventions
Dual awareness
A significant clinical feature of sensorimotor psychotherapy is its emphasis on the fostering of ‘dual awareness’ (Reference Ogden, Pain and FisherOgden 2006b) or awareness of awareness. In a state of dual awareness, the client is able to observe an experience as well as feel its associated emotions or sensations facilitating affect regulation and social judgement. Effective resolution of post-traumatic symptoms and prevention of inadvertent retraumatisation, both during psychotherapy and in the context of normal life, requires the ability to maintain dual awareness in the face of post-traumatic dysregulation. Long after patients have reached the intellectual conclusion that they are safe in their current lives, the body's post-traumatic responses re-create an internal experience of threat (Reference Van der Hart, Nijenhuis, Steele and Nortonvan der Hart 2006) adversely affecting reality-testing. Dual awareness increases the ability to differentiate past from present and to accurately evaluate experiences of feeling endangered.
Mindful observation
In a mindful state that encourages observation rather than reaction, patients become more curious than fearful about their emerging thoughts, emotions, sense perceptions, internal body sensations and movements. Under the guidance of the therapist, they are asked to pause periodically as they speak, to observe the interplay of thoughts, feelings and visceral responses that arise moment to moment in response to recalling or even thinking about distressing or overwhelming events.
Mindful observation requires both practice and education: the therapist may need to teach the patient how to distance themselves from trauma-related sensations or to understand the role of autonomic activation and the body's defensive responses of fight–flight–freeze and submission. Psychoeducational input is utilised to educate patients about the effect of trauma on body experience and to increase their capacity to sustain dual awareness in the face of traumatic activation. Cognitive understanding of how their symptoms preserved physical and psychological integrity under threat or their role in driving current symptomatology (Reference Van der Kolkvan der Kolk 2006) is often helpful to patients, often facilitating treatment adherence, lessening self-judgement and increasing curiosity.
In each session, patients are asked to practise observing and naming, without judgement or interpretation, any thoughts, feelings, body sensations and movement impulses that arise as they are sitting with the therapist. In the course of these observations, patients typically begin to notice patterns of response. Guided by the therapist, the patient might observe how a trauma-related body sensation immediately leads to a cognition, how the cognition evokes emotional responses, which in turn evoke body responses, how the visceral reactions lead to another negative thought, then another, resulting in increased ‘emotional overwhelm’ (Box 4).
BOX 4 What the patient learns during sensorimotor psychotherapy
-
• To gain greater control over responses to trauma-related stimuli through the use of somatic, cognitive and behavioural skills
-
• To notice, without judging or interpreting, thoughts, feelings and bodily reactions to trauma-related stimuli, rather than focusing on the traumatic events themselves
-
• To understand the process of trauma recollection and its effects on patterns of thought, emotion and autonomic activation
-
• To regulate autonomic arousal by directing attention away from the event itself to the patient's physical and emotional response to recollection
-
• To differentiate past from present (i.e., experiencing that the event is over as opposed to still happening), thus achieving a sense of distance from the event
Through the practice of mindful observation, patients gradually develop increased ability to become aware of these inner experiences without becoming overwhelmed and to choose which to attend to and which to put aside for the time being. As they increase the ability to maintain greater distance from distress and to deliberately shift focus away from disturbing material until the autonomic arousal subsides, their confidence and sense of mastery are enhanced and feelings of helplessness diminished. In those moments, their relationship to the memory or event is ‘reorganised’. An ability to recall the event as distressing without becoming overwhelmed, to feel emotions without flooding or acting out, represents a transformation of the memory from ‘here now’ to ‘finally over’. Mindful study of how an event was once organised somatically and emotionally thus is also a precursor to its potential reorganisation and encoding as an event that is ‘finally over,’ rather than ‘still happening’ or ‘never over’.
Somatic functioning
In addition to increasing the patient's capacity to maintain dual awareness and thereby the capacity for states of optimal arousal, the sensorimotor therapist also teaches the use of somatic skills that prevent emotional overwhelm, increase ability to recover from traumatic reminders and restore states of calm. For example, the therapist may help a patient to notice that, each time they have the thought ‘It was my fault’, they experience an emotional flooding of shame leading to a simultaneous slump in their spine, collapse in the chest, and movement of the head down and away. Having noticed the pattern, the therapist then begins a process of helping the patient to reorganise it, first by noticing it and becoming curious, then by exploring how a physical intervention (e.g. lengthening the spine or lifting the head) affects this habitual organisation of experience. If the patient lengthens their spine and raises their head slightly, what happens? And what happens if they exaggerate the collapse and gaze aversion? Does the fear increase or decrease?
Such interventions for increasing somatic and ego functioning are termed ‘somatic resources’ (Reference Ogden, Pain and FisherOgden 2006b). Many somatic resources, such as feeling the ground under one's feet, placing a hand over the heart, lengthening the spine, turning towards or away, moving closer or farther, affect psychological functioning. Conversely, many psychological resources have somatic correlates: confidence is often experienced somatically as a feeling of being taller, physically stronger, more solid or more flexible. Acceptance or compassion is often accompanied by a warmth in the chest, sense of opening, relaxation of the musculature. The English language includes many expressions that capture this relationship between body and psyche: ‘keep your head held high’, ‘stiff upper lip’, ‘hang-dog’, ‘having backbone’, ‘weak in the knees’ or ‘having a warm heart’.
Regulation of autonomic arousal
Diagnostic criteria for PTSD reflect the role of dysregulated arousal in the symptom picture. The intrusive symptoms that have become the hallmark of PTSD are driven by sympathetic hyperarousal, whereas the numbing symptoms are the result of parasympathetic hypoarousal. Easy startle, difficulty sleeping, loss of interest and hypervigilance also reflect dysregulated arousal. Autonomic alarm responses occur both situationally and habitually in traumatised patients and are easily interpreted as a sign of threat in the here-and-now environment. For the client to experience a somatic sense of safety, the autonomic nervous system must be stabilised and the capacity for optimal arousal cultivated. Allowing patients simply to access traumatic reactions of fear, horror and helplessness in treatment is often of little therapeutic benefit. In sensorimotor psychotherapy practice, the therapist's goal is reorganisation rather than re-experiencing. Without the ability to regulate these intense emotional states, many patients are unable to resolve their post-traumatic symptoms. Thus, attention to the regulation of arousal must be a key feature of any effective treatment for trauma.
In sensorimotor psychotherapy practice, the therapist addresses this issue by helping patients observe their trauma-related tendencies towards either hyper- or hypoarousal moment by moment long before they cause dysregulation. For example, a therapist might notice that as the patient begins to speak about a traumatic event, their body tightens and their breathing becomes shallow. Using dual awareness, the patient is asked to practise orienting away from the event itself and towards the body sensations, physical impulses or movements that have been evoked by the memory. By continually observing the patient's body for signs of increasing regulation v. dysregulation, the therapist monitors the activity of the autonomic nervous system.
The patient is frequently reminded to maintain a curious observational attitude rather than becoming frightened by the activation and to notice the physical signs that indicate dysregulated arousal. In addition, the therapist teaches the patient how to make use of somatic resources such as body posture, gesture and movement to regulate arousal. As patients learn to notice their habitual reactions and to practise alternative somatic interventions, a sense of greater control is facilitated over both autonomic arousal and impulsive behaviour. With practice of these skills and increasing ability to self-regulate, patients may be able to become less reliant on psychotropic medications for autonomic regulation or may require smaller dosages.
Over-association of neutral and trauma-related stimuli
Traumatic experiences often result in conditioned ‘over-association’ or ‘coupling’ of unrelated stimuli. For example, for a woman who has been raped, the sight or visual stimulus of an adult male may become associated with autonomic hyperarousal and impulses to run; or normal increases in heart rate may become over-associated with the belief that something bad is going to happen. The result is that normal or even positive experiences (e.g. enjoyment of being in male company or increased sympathetic tone resulting from excitement or enjoyment) are experienced as threatening.
Using interventions that ‘uncouple’ traumatic memories from their intense emotional and somatic responses, patients are helped to experience a sense of safety in the body even when faced with reminders of past psychological trauma. The process of uncoupling over-associating stimuli involves the dual awareness technique of directing the focus of attention. The patient is asked to shift focus from a memory or description of a distressing event to the way in which the body and mind respond during the remembering. For example, as a patient recalls being beaten by their father as a child, what is their internal experience of the event? Does the recall trigger increased arousal or body sensations? A thought or belief? Some feelings or emotions? Or impulses to move in some way? With the guidance of the therapist, they are asked to notice ‘What is happening right here, right now’.
One of the characteristics of trauma-related disorders is the loss of present-time orientation and sensorimotor psychotherapy addresses that issue by helping individuals to differentiate past and present: ‘When you remember that experience then, what happens here and now inside you?’
Key benefits and disadvantages
The development of abilities that foster improved affect regulation is perhaps the most significant benefit of the use of sensorimotor psychotherapy. The use of dual awareness can increase the ability to think clearly and reality-test appropriately and thereby reduce impulsivity in patients with bipolar disorder and borderline personality disorder.
Use of somatic resources as alternatives to such behaviours as cutting, acting out sexually or misusing substances contributes to stabilisation of high-risk behaviour.
In patients without clear memories of traumatic events (e.g. young children or those who experienced drug-induced date rape), sensorimotor psychotherapy provides a method for treating the trauma without the necessity of remembering the details of it. Because of its emphasis on autonomic self-regulation, it avoids many of the pitfalls associated with other trauma treatments such as high dropout rates and potential emotional flooding (Reference Ogden, Minton, Pain and NortonOgden 2006a).
Among the potential disadvantages of sensorimotor psychotherapy is its dependence on the patient's ability to access body awareness and to sustain at least intermittent mindful awareness. Despite the attention paid to self-regulation, focus on internal states can suddenly precipitate abreaction or affective overwhelm. To prevent this, the therapist must initially proceed cautiously and titrate interventions to test the patient's capacity to undertake this type of work. Although sensorimotor therapy is appropriate in short- and long-term treatment, patients with phobic responses to body or internal awareness may require a period of desensitisation in order to benefit from it.
Conclusions
Historically, psychotherapeutic treatments for trauma and attachment failure have focused on the task of creating a narrative in order to access and express the affects connected to it (Reference Herman and NortonHerman 1992). In recent years, treatment focus has shifted to psychopharmacological symptom management and cognitive–behavioural therapy. In sensorimotor psychotherapy, exposure to the details of the event is used primarily to access the unresolved somatic and affective components of the memory. As the patient relates a traumatic experience, the therapist listens attentively, paying equal attention to the narrative and to the body responses until signs of unresolved emotional, muscular, visceral or autonomic activity are observed. Therapeutic interruption of the trauma-related reactions and refocusing the patient's attention to the somatic responses facilitate their being witnessed simply as sensations and emotions rather than experienced as signals of danger.
With the patient's growing ability to maintain dual awareness, reactivity diminishes and arousal gradually comes under greater control. Reorganisation of the experience leading to a well-regulated nervous system results not only in improved affect regulation but also improvements in mood, energy, interest, reality-testing and impulsivity. The patient now has a narrative that places the events in the past and a body that experiences these events as ‘over.’ The body and thus the patient can now appropriately respond to environmental stimuli as stressful or pleasurable but not dangerous and threatening.
MCQs
Select the single best option for each question stem
-
1 Which of the following is not among the sequelae of traumatic experience?
-
a dysregulated autonomic arousal
-
b intrusive emotions and body sensations
-
c depression and numbing
-
d delusions and hallucinations
-
e hypervigilance.
-
-
2 Development of affect regulatory abilities are dependent on which of the following:
-
a secure attachment
-
b temperament and heredity
-
c socioeconomic status of caregivers
-
d emotional maturity of parents
-
e cognitive enrichment.
-
-
3 Sensorimotor psychotherapy is characterised by which of the following features:
-
a use of touch
-
b catharsis-promoting techniques
-
c mindfulness and dual awareness
-
d focus on traumatic events
-
e non-verbal approach.
-
-
4 The benefits of mindfulness as a therapeutic technique result from which of the following:
-
a emphasis on the achievement of calm
-
b activation of the prefrontal cortex
-
c regulatory effects on amygdala activation
-
d effect on the transference
-
e opportunity to observe procedurally learned patterns.
-
-
5 Somatic resources have which of the following benefits:
-
a provide somatic support for psychological functioning
-
b increase immune system functioning
-
c increase muscle tone and body strength
-
d positively influence self-esteem
-
e support mindfulness.
-
MCQ answers
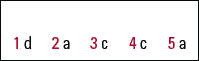
| 1 | d | 2 | a | 3 | c | 4 | c | 5 | a |


eLetters
No eLetters have been published for this article.