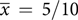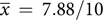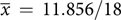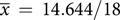Original Article
The Cardiac Neurodevelopmental Outcome Collaborative: a new community improving outcomes for individuals with congenital heart disease
- Part of:
- Erica Sood, Jeffrey P. Jacobs, Bradley S. Marino
-
- Published online by Cambridge University Press:
- 03 December 2020, pp. 1595-1596
-
- Article
- Export citation
-
Improved survival of patients with paediatric and congenital cardiac disease has led to a heightened awareness of the cognitive, neurodevelopmental, psychosocial, and physical functioning deficits that limit health, academic functioning, adaptive functioning, behavioural and emotional outcomes, health-related quality of life, and well-being for children and adults with congenital heart disease. The Cardiac Neurodevelopmental Outcome Collaborative was founded in 2016; its mission is to determine and implement best practices of neurodevelopmental and psychosocial services for individuals with paediatric and congenital heart disease and their families through clinical, quality improvement, and research initiatives.
Cardiology in the Young is devoted to cardiovascular issues affecting the young, and older patients with congenital heart disease, or with other cardiac diseases acquired during childhood. The journal serves the interests of all professionals concerned with these topics. By design, the journal is international and multidisciplinary in its approach, and members of the editorial board take an active role in its mission, helping to make it an indispensable reference for paediatric and congenital cardiac care. All aspects of paediatric and congenital cardiac care are covered in the journal. The content includes original articles, brief reports, editorials, reviews, and papers devoted to continuing professional development. High-quality colour figures are published on a regular basis, and without charge to the authors. Regular supplements are published containing the abstracts of the annual meetings of the Association for European Paediatric and Congenital Cardiology, along with other occasional supplements. These supplements are supplied free to subscribers.
The vision of Cardiology in the Young is to use print and electronic media to improve paediatric and congenital cardiac care. The mission of Cardiology in the Young is to be a premier global journal for paediatric and congenital cardiac care – an essential journal that spans the domains of patient care, research, education, and advocacy, and also spans geographical, temporal, and subspecialty boundaries.
Cardiology in the Young and the Cardiac Neurodevelopmental Outcome Collaborative are pleased to announce that Cardiology in the Young will serve as the official journal of the Cardiac Neurodevelopmental Outcome Collaborative. This new partnership between the Cardiac Neurodevelopmental Outcome Collaborative and Cardiology in the Young will facilitate the dissemination of knowledge and recommendations to the scientific, clinical, and patient advocacy communities, ultimately improving paediatric and congenital cardiac care and outcomes for individuals with paediatric and congenital heart disease and their families.
Review Article
Perioperative care of the newborns with CHDs in the time of COVID-19
- Part of:
- Dilek Dilli, Irfan Taşoğlu
-
- Published online by Cambridge University Press:
- 25 June 2020, pp. 946-954
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Coronavirus disease 2019 (COVID-19), caused by a novel betacoronavirus (SARS-CoV-2), has led to an unexpected outbreak affecting people of all ages. The first data showed that COVID-19 could cause severe pulmonary disease, cardiac injury, and death in adults, especially the elderly and those with concomitant diseases. Currently, it was demonstrated that severe COVID-19 may also develop in neonatal age, although rarely. Newborns with CHD are known to be at high risk for increased morbidity from viral lower respiratory tract infections because of underlying anatomical cardiac lesions. There are limited data on the implications of COVID-19 on patients with cardiovascular disease, especially for those with CHD. Herein, we aimed to summarise the COVID-19-specific perioperative management issues for newborns with CHD by combining available data from the perspectives of neonatology and paediatric cardiovascular surgery.
Original Article
Off-pump ascending aorta or aortic arch to descending aorta bypass with a pericardial roll for the treatment of critically ill infants with interrupted aortic arch
- Didem M. Oztas, Mert Meric, Metin O. Beyaz, Senay Coban, Gizem Sari, Yahya Yildiz, Mustafa O. Ulukan, Orcun Unal, Orhan Rodoplu, Zerrin Sungur, Yilmaz Yozgat, Turkay Saritas, Abdullah Erdem, Murat Ugurlucan, Emin Tireli, Halil Turkoglu
-
- Published online by Cambridge University Press:
- 18 June 2020, pp. 1095-1102
-
- Article
- Export citation
-
Aim:
Standard surgical treatment of the interrupted aortic arch with the use of cardiopulmonary bypass is risky especially in critically ill babies. In this manuscript, we present the results of off-pump pericardial roll bypass for the treatment of aortic interruption.
Material and methods:The technique was applied in nine critically ill infants between July 2011 and December 2019. Data were reviewed retrospectively. There were four girls and five boys. The types of the interruption were type B in six cases and type A in three babies. Additional cardiovascular anomalies were ventricular septal defect in all, atrial septal defect or patent foramen ovale in all, single-ventricle pathologies in two and bicuspid aortic valve in three cases. All the patients were in critical situations such as intubated, having symptoms of infection, congestive heart failure or ischaemia and malperfusion leading visceral organ dysfunction.
Results:All patients underwent off-pump ascending aorta or aortic arch to descending aorta bypass with a pericardial roll. Post-operative early mortality occurred in one patient with severe mitral regurgitation due to cardio-septic shock. One patient who had single-ventricle pathology underwent bidirectional Glenn and was lost on the post-operative 26th day due to sepsis 2 years after operation. Two patients presented with dilatation of the pericardial tube 18 and 24 months after the operations and one underwent reconstruction of the neo-arch. The remaining patients are asymptomatic, active and within normal limits of body and mental growth.
Conclusion:Treatment of interrupted aortic arch with a bypass with an autologous pericardial roll treated with gluteraldehyde without cardiopulmonary bypass seems a safe and reliable technique especially for the treatment of critically ill infants.
Unexpected increase of aortic stiffness in juvenile Spondyloarthropathies
- Reyhan Dedeoglu, Mehmet Yildiz, Fatih Karagozlu, Funda Oztunc, Nujin Ulug, Beste Akdeniz, Amra Adrovic, Fatih Haslak, Sezgin Sahin, Kenan Barut, Ozgur Kasapcopur
-
- Published online by Cambridge University Press:
- 17 September 2020, pp. 1806-1814
-
- Article
- Export citation
-
Juvenile spondyloarthropathy is an umbrella term for a group of childhood rheumatic diseases that can cause chronic arthritis extending to the axial skeleton before the age of 16. Although ankylosing spondylitis has aortic involvement as one of its most important effects, this relationship has not been extensively studied in children with juvenile spondyloarthropathy. Here, a cross-sectional study of the elastic properties of the aorta of 43 patients with juvenile spondyloarthropathy and 19 healthy controls is reported. Aortic stiffness assessed by echocardiography was used to predict the presence of aortitis, supplemented by pulsed-wave tissue Doppler indices. The right ventricular fractional area change was found to be significantly lower in the patients with juvenile spondyloarthropathy than in the healthy controls; aortic strain and distensibility were also significantly lower, and aortic stiffness index β was significantly higher; and the aortic root diameter change was significantly lower. According to HLA-B27 positivity, there was no difference in the stiffness parameters between the two groups. There was a significant correlation between juvenile Ankylosing Spondylitis Disease Activity Index and aortic diameter change, between juvenile Ankylosing Spondylitis Disease Activity Index and aortic stiffness. Thus, juvenile spondyloarthropathy is linked to high aortic stiffness parameters.
Experience with balloon pulmonary valvuloplasty and predictors of outcome: a ten-year study
- Sonia A. El-Saeidi, Hala S. Hamza, Hala M. Agha, Mohammed M. Soliman, Wael A. Attia, Rania El-Kaffas, Faten Abdel-Aziz, Osama Abdel-Aziz, Sahar Shaker, Amira Esmat, Rasha Ammar, Aya Fattouh, Khalid Mohi-eldin, Amal M. El-Sisi
-
- Published online by Cambridge University Press:
- 19 February 2020, pp. 482-488
-
- Article
- Export citation
-
Background:
Balloon pulmonary valvuloplasty is the treatment of choice for patients with moderate to severe pulmonary valve stenosis.
Methods:An observational retrospective cross-sectional study including neonates, small infants, and children who underwent balloon pulmonary valvuloplasty in the period from 2007 to 2016 in the cardiac catheterisation unit of the paediatric cardiology department in Cairo University. Multivariable models were built to report the predictors of the outcome of balloon pulmonary valvuloplasty and its complications.
Results:A total of 1200 patients were included in the study and divided according to age into 3 groups: neonates and early infants (n = 282), infants (n = 362), and children (n = 556). Procedural success, defined as a drop pressure gradient across the pulmonary valve to less than or equal to 50% of the baseline measurements, was achieved in 82.7% of the patients. Multivariate analysis revealed that only infundibular pulmonary stenosis (p value 0.032), supravalvular in association with valvular pulmonary stenosis (p value <0.001), and pulmonary valve diameter by angiogram (p value <0.001) were significant predictors of success. The presence of supravalvular in association with valvular pulmonary stenosis (p value <0.001) was associated with a lower weight (p value 0.007) and higher right ventricular pressure before the intervention (p value <0.001), and a minor immediate drop in the pressure gradient post-intervention (p value <0.001) was found to be the most significant predictor of the occurrence of complications.
Conclusion:The absence of infundibular and supravalvular stenosis and a large pulmonary valve diameter were the most significant predictors of success.
Prevalence of breastfeeding and its obstacles in patients with CHD in southern Brazil
- Maíra Ribas Goulart, Julia Lima, Marcelo Ahlert, Sandra Barbiero, Daniela Schneid Schuh, Lucia Pellanda
-
- Published online by Cambridge University Press:
- 24 July 2020, pp. 1417-1421
-
- Article
- Export citation
-
Introduction:
Breast milk is nutritionally adequate and is related to the reduction of various health problems in childhood. Its offer is widely recommended in health guidelines.
Objective:To estimate the prevalence and obstacles to breastfeeding in patients with CHD in southern Brazil.
Methods:Cross-sectional study of patients with CHD between 2 and 18 years of age. Patients with genetic syndromes and patients whose mothers had died were excluded from the analysis. The variables on breastfeeding in the first 2 years of life were collected through a phone call to the mothers, which was conducted by trained evaluators. Prevalence was described in proportions and the continuous variables as means and standard deviation. Bivariate analyses were evaluated using a chi-square test to measure the association between the variables and the outcome.
Results:A total of 351 patients with CHD were analysed. There was a predominance of males (53%) and a mean age of 9.54 ± 4.52 years. Breastfeeding up to the sixth month was present in 40% of the cases.
Conclusion:The mothers of babies with CHD face great challenges to maintain the supply of breast milk, whether inherent to the practice of breastfeeding or related to CHD.
Prolonged length of stay after surgery for adult congenital heart disease: a single-centre study in a developing country
- Russell S. Martins, Zaiba S. Dawood, Muhammad K. Y. Memon, Saleem Akhtar
-
- Published online by Cambridge University Press:
- 15 July 2020, pp. 1253-1260
-
- Article
- Export citation
-
Background:
With the growing number of adults requiring operations for CHD, prolonged length of stay adds an additional burden on healthcare systems, especially in developing countries. This study aimed to identify factors associated with prolonged length of stay in adult patients undergoing operations for CHD.
Methods:This retrospective study included all adult patients (≥18 years) who underwent cardiac surgery with cardiopulmonary bypass for their CHD from 2011 to 2016 at a tertiary-care private hospital in Pakistan. Prolonged length of stay was defined as hospital stay >75th percentile of the overall cohort (>8 days).
Results:This study included 166 patients (53.6% males) with a mean age of 32.05 ± 12.11 years. Comorbid disease was present in 59.0% of patients. Most patients underwent atrial septal defect repair (42.2%). A total of 38 (22.9%) patients had a prolonged length of stay. Post-operative complications occurred in 38.6% of patients. Multivariable analysis showed that pre-operative body mass index (odds ratio: 0.779; 95% confidence interval: 0.620–0.980), intraoperative aortic cross-clamp time (odds ratio: 1.035; 95% confidence interval: 1.009–1.062), and post-operative acute kidney injury (odds ratio: 7.392; 95% confidence interval: 1.036–52.755) were associated with prolonged length of stay.
Conclusion:Predictors of prolonged length of stay include lower body mass index, longer aortic cross-clamp time, and development of post-operative acute kidney injury. Shorter operations, improved pre-operative nutritional optimisation, and timely management of post-operative complications could help prevent prolonged length of stay in patients undergoing operations for adult CHD.
Outcome of congenital tracheal stenosis in children over two decades in a national cardiothoracic surgical unit
- Colin J. McMahon, Karim Ayoubi, Rania Mehanna, Eithne Phelan, Eoin O’Cearbhaill, John Russell, Lars Nölke
-
- Published online by Cambridge University Press:
- 20 November 2019, pp. 34-38
-
- Article
- Export citation
-
Objective:
To assess the outcomes of congenital tracheal stenosis among children.
Materials and methods:A retrospective review of all children who underwent surgical repair of congenital tracheal stenosis reviewing charts, operative notes, echocardiograms, CT and MRI data from January 2002 to February 2019.
Results:Twenty-six children underwent surgical treatment for tracheal stenosis. The median age was 3 months (range 0.3–35 months) and the median weight was 4.7 kg (range 2.5–13 kg) at the time of surgical intervention. Stridor was the most common presenting symptom in 17 patients (65% of patients). Twenty-one patients (81%) had concurrent cardiac anomalies, with pulmonary arterial sling being the most common, present in nine patients (34%). Extracorporeal life support was utilised in seven patients (27%) pre-operatively. Laryngeal release was required in 16 patients. In 7 patients an end-to-end anastomosis was performed, in 18 patients slide tracheoplasty, and 1 patient had a double slide tracheoplasty. The median cardiopulmonary bypass time was 106 minutes (range 25–255 minutes). The median cross-clamp time was 30 minutes (range 5–67 minutes). The median post-operative duration of ventilation was 5 days (range 0.5–16 days). The median ICU length of stay was 12.5 days (range 2–60 days). There were three hospital mortalities with 88% survival. One patient only required reintervention with balloon dilation. Twenty-two patients (85%) remained symptom-free on median follow-up at 7.6 years (range 0.2–17 years). Two patients since 2017 had 3D printed tracheas produced from CT imaging to assist surgical planning.
Conclusion:Congenital tracheal stenosis can be managed effectively with excellent outcomes and 3D printed models assist in planning the optimal surgical intervention.
Two females with coronary artery occlusion caused by presumed Kawasaki disease would have delivered without recognition of ischaemic heart disease
- Etsuko Tsuda, Takashi Noda, Teruo Noguchi
-
- Published online by Cambridge University Press:
- 08 May 2020, pp. 785-789
-
- Article
- Export citation
-
We report two females with coronary artery occlusion caused by presumed Kawasaki disease that delivered children without any special treatment. After a 58-year-old female had ventricular tachycardia, a giant coronary artery aneurysm with calcification at the bifurcation of the left coronary artery and segmental stenosis of the right coronary artery were pointed out by CT angiography. She had an episode of sepsis when 3 years old. Further, she remembered chest pain during sleep after that episode. She had delivered twice without any complication during her 20s. Her diagnosis was undiagnosed coronary artery lesions caused by presumed Kawasaki disease and a previous myocardial infarction, and she underwent radiofrequency catheter ablation and implantable cardioverter defibrillator implantation. The other 48-year-old female was accidentally discovered to have coronary artery calcification on CT, while experiencing pneumonia. Her CT angiograms revealed a right coronary artery occlusion and coronary artery calcification at segments 1, 6, and 11. She had a history of “scarlet fever” before 12 months. Premature ventricular contractions were detected, while delivering her first child when 31 years old. However, she was not diagnosed as ischaemic heart disease and delivered twice by a vaginal delivery without any complication. Current guidelines recommend systemic anti-coagulation and anti-platelet therapy for all patients with giant aneurysms resulting from Kawasaki disease in childhood. The two women reported here were fortunate not to have had complications during pregnancy and delivery despite their severe coronary artery aneurysms, which were unrecognised clinically until later in life. They were lucky cases.
A transition clinic intervention to improve follow-up rates in adolescents and young adults with congenital heart disease
- Stephanie S. Gaydos, Shahryar M. Chowdhury, Rochelle N. Judd, Kimberly E. McHugh
-
- Published online by Cambridge University Press:
- 13 April 2020, pp. 633-640
-
- Article
- Export citation
-
Background:
Children with congenital heart disease (CHD) require lifelong cardiology follow-up. Many experience gaps in care around the age of transition to adult-oriented care with associated comorbidity. We describe the impact of a clinic-based intervention on follow-up rates in this high-risk population.
Methods:Patients ≥11 years seen in a paediatric outpatient CHD Transition Clinic completed self-assessment questionnaires, underwent focused teaching, and were followed on a clinic registry with assessment of care continuation. The cohort “lost to follow-up” rate, defined as absence from care at least 6 months beyond the recommended timeframe, was compared with a control group. Secondary outcomes included questionnaire scores and adult cardiology referral trends.
Results:Over 26 months, 53 participants completed an initial Transition Clinic visit; 43% (23/53) underwent a second visit. Median participant age was 18.0 years (interquartile range 16.0, 22.0). The cohort’s “lost to follow-up” rate was 7.3%, which was significantly lower than the control rate (25.9%, p < 0.01). Multivariable regression analyses demonstrated clinic participation as the only factor independently associated with follow-up rates (p = 0.048). Transition readiness was associated with older age (p = 0.01) but not sex, univentricular heart, interventional history, or surgical complexity. One-third of adult participants transferred to adult care.
Conclusions:A CHD Transition Clinic intervention can improve follow-up rates in adolescents and young adults. Age is an important factor in transition readiness, and retention of adults in paediatric care appears multi-factorial. We postulate that serial assessments of self-management, focused education, and registry utilisation may improve patient outcomes by reducing lapses in care.
Everolimus for cardiac rhabdomyomas in children with tuberous sclerosis. The ORACLE study protocol (everOlimus for caRdiac rhAbdomyomas in tuberous sCLErosis): a randomised, multicentre, placebo-controlled, double-blind phase II trial
- Erica V. Stelmaszewski, Daniella B. Parente, Alberto Farina, Anna Stein, Anthony Gutierrez, Antonio F. Raquelo-Menegassio, Carla Manterola, Carolina F. de Sousa, Carolina Victor, Dina Maki, Elias M. Morón, Fabiano F. de Abrantes, Fatima Iqbal, Jazmin Camacho-Vilchez, Joanna Jimenez-Pavón, Juan P. Polania, Lorenzo Thompson, Lygia Bonanato, Matthias Diebold, Maria V. C. P. Da Silva, Mariam W. J. Nashwan, Marianna A. G. Galvani, Osama E. A. Idris, Pierina Danos, Rocio Ortiz-Lopez, Rofida A. A. Mahmoud, Sergio Gresse, Jr, Karla L. Loss
-
- Published online by Cambridge University Press:
- 27 January 2020, pp. 337-345
-
- Article
- Export citation
-
Introduction:
Tuberous sclerosis complex is a rare genetic disorder leading to the growth of hamartomas in multiple organs, including cardiac rhabdomyomas. Children with symptomatic cardiac rhabdomyoma require frequent admissions to intensive care units, have major complications, namely, arrhythmias, cardiac outflow tract obstruction and heart failure, affecting the quality of life and taking on high healthcare cost. Currently, there is no standard pharmacological treatment for this condition, and the management includes a conservative approach and supportive care. Everolimus has shown positive effects on subependymal giant cell astrocytomas, renal angiomyolipoma and refractory seizures associated with tuberous sclerosis complex. However, evidence supporting efficacy in symptomatic cardiac rhabdomyoma is limited to case reports. The ORACLE trial is the first randomised clinical trial assessing the efficacy of everolimus as a specific therapy for symptomatic cardiac rhabdomyoma.
Methods:ORACLE is a phase II, prospective, randomised, placebo-controlled, double-blind, multicentre protocol trial. A total of 40 children with symptomatic cardiac rhabdomyoma secondary to tuberous sclerosis complex will be randomised to receive oral everolimus or placebo for 3 months. The primary outcome is 50% or more reduction in the tumour size related to baseline. As secondary outcomes we include the presence of arrhythmias, pericardial effusion, intracardiac obstruction, adverse events, progression of tumour reduction and effect on heart failure.
Conclusions:ORACLE protocol addresses a relevant unmet need in children with tuberous sclerosis complex and cardiac rhabdomyoma. The results of the trial will potentially support the first evidence-based therapy for this condition.
Emotional quality-of-life and patient-reported limitation in sports participation in children with uncorrected congenital and acquired heart disease in healthcare-restricted settings in low- and middle-income countries
- Gali S Kolt, Barbara R Ferdman, Jessica Y Choi, Janine Henson, Van-Trang Nguyen, Emily A Farkas, Vinicius JDS Nina, Rachel VAH Nina, Renzo O CiFuentes, William F Zeman, John E Connett, Aubyn Marath
-
- Published online by Cambridge University Press:
- 05 February 2020, pp. 188-196
-
- Article
- Export citation
-
Background:
Little is known about emotional quality-of-life in paediatric heart disease in low- and middle-income countries where the prevalence of uncorrected lesions is high. Research on emotional quality-of-life and its predictors in these settings is key to planning interventions.
Methods:Ten-year retrospective cross-sectional study of children aged 6–17 years with uncorrected congenital or acquired heart disease in 12 low- and middle-income countries was conducted. Emotional functioning score of the PedsQL TM 4.0 generic core scale and data on patient-reported limitation in sports participation were collected via in-person interview and analysed using regression analyses.
Results:Ninety-four children reported mean emotional functioning scores of 71.94 (SD 25.32) [95% CI 66.75–77.13] with lower scores independently associated with having a parent with a chronic illness or who had died (p = 0.005), having less than three siblings (p = 0.007), and reporting a subjective limitation in carrying an item equivalent to a 4 lb load (p = 0.021). Patient-reported limitation in sports participation at least “sometimes” was present in 69% and was independently associated with experiencing symptoms at least once a month (p < 0.001).
Conclusion:Some of the factors which were associated with better emotional quality-of-life were similar to those identified in previous studies in patients with corrected defects. Patient-reported limitation in sports participation is common. In addition to corrective surgery and exercise, numerous other interventions which are practicable during surgical missions might improve emotional quality-of-life.
Usefulness of N-terminal pro-B-type natriuretic peptide (NT-ProBNP) as a marker for cardiotoxicity and comparison with echocardiography in paediatric carbon monoxide poisoning
- Caner Turan, Eser Dogan, Ali Yurtseven, Eylem Ulas Saz
-
- Published online by Cambridge University Press:
- 23 June 2020, pp. 1103-1108
-
- Article
- Export citation
-
Objectives:
To demonstrate the usefulness of N-Terminal Pro-B-Type natriuretic peptide (NT-proBNP) as an early biomarker of carbon monoxide-induced myocardial injury in children. It also aimed to identify the correlation between NT-proBNP and left ventricular systolic dysfunction findings shown by echocardiography.
Methods:Prospective, observational study conducted at a paediatric emergency department between October 2017 and April 2019 which involved children aged 0–17 years. The patients were divided into three groups based on severity; mild, moderate and severe groups. The patient characteristics, carboxyhaemoglobin, CK-MB Mass (CKMB-M), troponin-T, and NT-proBNP levels were measured, and echocardiography was performed and left ventricular ejection fraction was measured.
Results:Sixty-nine patients and 60 healthy controls were included. Male gender, younger age, higher carboxyhaemoglobin levels, and altered mental status were found as independent predictors of carbon monoxide-induced myocardial injury. If the cut-off value for NT-proBNP level is >480 pg/ml, the sensitivity–specificity for decreased left ventricular ejection fraction, which is the strongest carbon monoxide-induced myocardial injury sign, were 100–96%, respectively. A high negative correlation was found between NT-proBNP levels and left ventricular ejection fraction (r = −0.769, p < 0.01) in the carbon monoxide poisoning group, and there was a positive correlation between the carboxyhaemoglobin and NT-proBNP levels (r = 0.583, p < 0.01).
Conclusion:Echocardiography is an ideal tool and very sensitive, but its routine use is limited due to its non-availability. An increased level of NT-proBNP (>480pg/ml) may be useful as an ideal biomarker for early detection of carbon monoxide-induced myocardial injury sign and reduced left ventricular ejection fraction which is the most crucial point in making a decision on hyperbaric oxygen therapy.
Utility of biomarkers in adult Fontan patients with decompensated heart failure
- Vidang P. Nguyen, Song Li, Stephen J. Dolgner, Zachary L. Steinberg, Jonathan Buber
-
- Published online by Cambridge University Press:
- 02 June 2020, pp. 955-961
-
- Article
- Export citation
-
Background:
The incidence of heart failure is increasing within the Fontan population. The use of serological markers, including B-type natriuretic peptide, has been limited in this patient population.
Methods:This was a single-centre retrospective study of Fontan patients in acute decompensated heart failure. Fontan patients underwent a 1:2 match with non-Fontan patients for each heart failure hospitalisation for comparative analysis. A univariate logistic regression model was used to assess associations between laboratory and echocardiographic markers and a prolonged length of stay of 7 days or greater.
Results:B-type natriuretic peptide levels were significantly lower in Fontan patients admitted for heart failure than that in non-Fontan patients [390.9 (±378.7) pg/ml versus 1245.6 (±1160.7) pg/ml, respectively, p < 0.0001] and were higher in Fontan patients with systemic ventricular systolic or diastolic dysfunction than that in Fontan patients with normal systemic ventricular function [833.6 (±1547.2) pg/ml versus 138.6 (±134.0) pg/ml, p = 0.017]. The change from the last known outpatient value was smaller in Fontan patients in comparison with non-Fontan patients [65.7 (±185.7) pg/ml versus 1638.0 (±1444.7) pg/ml, respectively, p < 0.0001]. Low haemoglobin and high blood urea nitrogen levels were associated with a prolonged length of stay.
Conclusion:B-type natriuretic peptide levels do not accurately reflect decompensated heart failure in Fontan patients when compared to non-Fontan heart failure patients and should, therefore, be used with caution in this patient population.
Implementation of a standardized oral screening tool by paediatric cardiologists
- Shelley I. McCargar, Joanne Olsen, Robert J. Steelman, Jennifer H. Huang, Elizabeth A. Palmer, Grant H. Burch, Richard Reed, Sara K. LaBarge
-
- Published online by Cambridge University Press:
- 22 September 2020, pp. 1815-1820
-
- Article
- Export citation
-
Background:
An examination of invasive procedure cancellations found that the lack of pre-procedural oral screening was a preventable cause, for children with congenital heart disease. The purpose of this study was to implement an oral screening tool within the paediatric cardiology clinic, with referral to paediatric dental providers for positive screens. The target population were children aged ≥6 months to <18 years old, being referred for cardiac procedures.
Methods:The quality implementation framework method was used for this study design. The multi-modal intervention included education, audit and feedback, screening guidelines, environmental support, and interdisciplinary collaboration. Baseline rates for oral screenings were determined by retrospective chart audit from January 2018 to January 2019 (n = 211). Provider adherence to the oral screening tool was the outcome measure. Positive oral screens, resulting in referral to the paediatric dental clinic, were measured as a secondary outcome. Provider adherence rates were used as a process measure.
Results:Data collected over 14 weeks showed a 29% increase in documentation of oral screenings prior to referral, as compared to the retrospective chart audit. During the study period, 13% of completed screenings were positive (n = 5). Provider compliance for the period was averaged at 70% adherence.
Conclusion:A substantial increase in pre-procedural oral screenings by paediatric cardiologists was achieved using the quality implementation framework and targeted interventions.
Risk stratification of patients with hypoplastic left heart syndrome and intact atrial septum using fetal MRI and echocardiography
- Ryan M. Serrano, Sabena Hussain, Brandon Brown, Eric S. Ebenroth, Anne Farrell
-
- Published online by Cambridge University Press:
- 14 May 2020, pp. 790-798
-
- Article
- Export citation
-
Despite prenatal diagnosis, prenatal intervention, and immediate postnatal intervention, patients with hypoplastic left heart syndrome and intact or highly restrictive atrial septum have the highest risk for mortality. Charts for all infants diagnosed with hypoplastic left heart syndrome from 2009 to 2017 were retrospectively reviewed and compared, including pulmonary vein Doppler patterns on fetal echocardiogram and evidence of pulmonary lymphangiectasia on fetal MRI. Of the 81 newborns with hypoplastic left heart syndrome, we defined two groups. Group 1 patients had an adequate atrial septal communication (n = 69), while Group 2 met criteria for intact/restrictive septum (n = 12). No patient in Group 1 had a type C pulmonary vein Doppler pattern, while no patient in Group 2 had a type A pulmonary vein Doppler pattern. The two patients with pulmonary lymphangiectasia had type C pulmonary vein Doppler pattern and an intact atrial septum and did not survive. Survival to discharge for Group 1 was 83% compared to 58% for Group 2 (p = 0.116). Survival to stage 2 palliation was 71% for Group 1 compared to 50% for Group 2 (p = 0.186). Only 4 of the initial 12 patients from Group 2 are alive, which is an overall survival of 33%. Our experience supports previous evidence that fetal echocardiography can identify those patients with the greatest likelihood for postnatal intervention as well as those at highest risk for mortality. Fetal MRI is a novel imaging modality that may help providers separate patients at highest risk for mortality, regardless of pulmonary vein Doppler pattern.
Short- and intermediate-term results of balloon aortic valvuloplasty and surgical aortic valvotomy in neonates
- Nicholas B. Zaban, Jeremy L. Herrmann, Mark H. Hoyer, John W. Brown, Ryan D. Alexy
-
- Published online by Cambridge University Press:
- 24 February 2020, pp. 489-492
-
- Article
- Export citation
-
Background:
Balloon aortic valvuloplasty and open surgical valvotomy are procedures to treat neonatal aortic stenosis, and there is controversy as to which method has superior outcomes.
Methods:We reviewed the records of patients at our institution since 2000 who had a balloon aortic valvuloplasty or surgical valvotomy via an open commissurotomy prior to 2 months of age.
Results:Forty patients had balloon aortic valvuloplasty and 15 patients had surgical valvotomy via an open commissurotomy. There was no difference in post-procedure mean gradient by transthoracic echocardiogram, which were 25.8 mmHg for balloon aortic valvuloplasty and 26.2 mmHg for surgical valvotomy, p = 0.87. Post-procedure, 15% of balloon aortic valvuloplasty patients had moderate aortic insufficiency and 2.5% of patients had severe aortic insufficiency, while no surgical valvotomy patients had moderate or severe aortic insufficiency. The average number of post-procedure hospital days was 14.2 for balloon aortic valvuloplasty and 19.8 for surgical valvotomy (p = 0.52). Freedom from re-intervention was 69% for balloon aortic valvuloplasty and 67% for surgical valvotomy at 1 year, and 43% for balloon aortic valvuloplasty and 67% for surgical valvotomy at 5 years (p = 0.60).
Conclusions:Balloon aortic valvuloplasty and surgical valvotomy provide similar short-term reduction in valve gradient. Balloon aortic valvuloplasty has a slightly shorter but not statistically significant hospital stay. Freedom from re-intervention is similar at 1 year. At 5 years, it is slightly higher in surgical valvotomy, though not statistically different. Balloon aortic valvuloplasty had a higher incidence of significant aortic insufficiency. Long-term comparisons cannot be made given the lack of long-term follow-up with surgical valvotomy.
Lymphopenia in adults after the Fontan operation: prevalence and associations
- Tarek Alsaied, Mathias Possner, Nicole Brown, Hassan Almeneisi, Cassandra Szugye, Andrew T. Trout, Omar Niss, Joseph J. Palermo, Faizeen Zafar, Jonathan R. Dillman, Gruschen R. Veldtman, Alexander R. Opotowsky, Adam M. Lubert
-
- Published online by Cambridge University Press:
- 06 April 2020, pp. 641-648
-
- Article
- Export citation
-
Lymphopenia is common in adults who have had a Fontan operation although its aetiology and clinical implications remain unknown. Previous work suggests an association between lymphopenia and both liver disease and splenomegaly. The objective of this study was to assess the prevalence of lymphopenia in adults with a Fontan circulation and evaluate its associations with risk factors and clinical outcomes. Using a retrospective cohort study design, we studied 73 adult Fontan patients (age 25.0 ± 8.4 years) who had a complete blood count and abdominal imaging performed. Patients with protein-losing enteropathy were excluded. Clinical data were extracted from hospital records. The mean white blood cell count was 6580 ± 220/ml with a mean lymphocyte count of 1223 ± 508/ml. Lymphopenia, defined as lymphocyte count <1000/ml, was present in 23 (32%) patients. Patients with lymphopenia had a lower total white blood cell count (5556 ± 2517 versus 7136 ± 1924/ml, p = 0.009) and a lower platelet count (162 ± 69 versus 208 ± 69 k/ml, p = 0.008). Lymphopenia was also associated with findings of portal hypertension, including splenomegaly (36 versus 14%, p = 0.04), varices (22 versus 6%, p = 0.04), and ascites (39 versus 14%, p = 0.02). Lymphopenia did not correlate with any cardiac imaging, haemodynamic or exercise testing variables. In conclusion, lymphopenia is common in adult Fontan patients and is associated with markers of portal hypertension. Larger studies are needed to better define the relationship between lymphopenia and clinical outcomes.
“Why and how did this happen?”: development and evaluation of an information resource for parents of children with CHD
- Alexis V. Hunt, Desiree C. K. Hilton, Charlotte E. Verrall, Kristine K. Barlow-Stewart, Jane Fleming, David S. Winlaw, Gillian M. Blue
-
- Published online by Cambridge University Press:
- 10 January 2020, pp. 346-352
-
- Article
- Export citation
-
Background:
The causes of CHD are complex and often unknown, leading parents to ask how and why this has happened. Genetic counselling has been shown to benefit these parents by providing information and support; however, most parents currently do not receive this service. This study aimed to develop a brochure to determine whether an information resource could improve parents’ knowledge about CHD causation and inheritance and increase psychosocial functioning.
Methods:In development, the resource was assessed against several readability scales and piloted. Parents of children attending preadmission clinic for surgery were included. Assessments occurred pre- and post-receiving the information resource using a purpose-designed knowledge measure and validated psychological measures.
Results:Participant’s (n = 52) knowledge scores increased significantly from the pre-questionnaire (
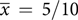 ${\overline x}\, = \,5/10$
, sd = 2.086) to post-questionnaire (
${\overline x}\, = \,5/10$
, sd = 2.086) to post-questionnaire (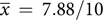 $\overline x\, = \,7.88/10$
, sd = 2.094, p < 0.001), with all aware that CHD can be caused by genetic factors after reading the brochure. Perceived personal control also increased from pre- (
$\overline x\, = \,7.88/10$
, sd = 2.094, p < 0.001), with all aware that CHD can be caused by genetic factors after reading the brochure. Perceived personal control also increased from pre- (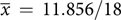 $\overline x\, = \,11.856/18$
, sd = 4.339) to post-brochure (
$\overline x\, = \,11.856/18$
, sd = 4.339) to post-brochure (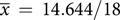 $\overline x\, = \,14.644/18$
, sd = 3.733, p < 0.001), and many reported reduced feelings of guilt. No negative emotional response to the brochure was reported. The information provided was considered relevant (88%), reassuring (86%), and 88% would recommend the brochure to other parents. However, some wanted more emotional support and assistance in what to tell their child.Conclusions:
$\overline x\, = \,14.644/18$
, sd = 3.733, p < 0.001), and many reported reduced feelings of guilt. No negative emotional response to the brochure was reported. The information provided was considered relevant (88%), reassuring (86%), and 88% would recommend the brochure to other parents. However, some wanted more emotional support and assistance in what to tell their child.Conclusions:Use of the information resource significantly enhanced parents’ knowledge of CHD causation and increased their psychosocial functioning. It is a valuable resource in the absence of genetic counselling; however, it should not replace formal genetic counselling when required.
Prenatal diagnosis of anomalous origin of one pulmonary artery branch by two-dimensional echocardiography: summary of 12 cases
- Li Wenxiu, Zhang Yuan, Huang Chaoning, Geng Bin, Wu Jiang, Yang Shuang
-
- Published online by Cambridge University Press:
- 17 December 2019, pp. 39-46
-
- Article
- Export citation
-
Objectives:
To improve the prenatal diagnosis for anomalous origin of pulmonary artery branches by comparing and analyzing different types of fetal echocardiography features.
Methods:Between June 2012 and December 2018, fetal echocardiographic features were analyzed retrospectively from fetuses with a prenatal diagnosis of anomalous origin of pulmonary artery branch. The main points of identification were summarized.
Results:A total of 12 fetuses were diagnosed, including anomalous origin of a pulmonary artery branch from the innominate artery and six cases with unilateral absence of pulmonary artery. The shared characteristic sonographic finding was the lack of confluence at the bifurcation of the main pulmonary artery. The differences between the two conditions are highlighted by the origin of the anomalous vessel. In fetuses with anomalous origin of one pulmonary artery branch, the affected pulmonary artery arose from the posterior wall of the ascending aorta as noted on three vessels and trachea view as well as the long axis of the left ventricular outflow tract. This is in contrast to fetuses with unilateral absence of pulmonary artery, where the origin of affected pulmonary artery arises from the base of the innominate artery via the ipsilateral patent arterial duct as evident on the three vessels and trachea view and the coronal view of innominate (brachiocephalic) artery.
Conclusion:(1) The main similarity is an absence of a confluence at the bifurcation of the main pulmonary artery. (2) The main distinguishing feature is the origin of the anomalous vessel from either the subclavian or directly from the aorta.