To the Editor—We read with interest the letter by Kazi et alReference Kazi, Shetty and Rodrigues 1 in which the authors reflect on the question of probable higher carbapenem minimum inhibitory concentrations (MICs) when dual carbapenem resistance mechanisms coexist.
Greece was the first country where double carbapenemase-producing Klebsiella pneumoniae (CPKP) were detected in 2009.Reference Meletis, Tzampaz, Protonotariou and Sofianou 2 Since then, they have reached approximately 5% of CPKPs isolated in Greek hospitals.Reference Giakkoupi, Papagiannitsis and Miriagou 3 These double CPKPs commonly bear KPC-2 plus VIM-1 carbapenemases. More recently, NDM-1-producing K. pneumoniae have also emerged in Greece.Reference Voulgari, Gartzonika and Vrioni 4
To further investigate the aforementioned question with a different carbapenemase combination than that used by Kazi et al, we performed the imipenem E-test (bioMérieux, Marcy l’Etoile, France) in 4 groups of nonduplicate CPKPs isolated from various clinical samples from patients hospitalized in AHEPA University Hospital of Thessaloniki. Group A consisted of 20 KPC-2-producers; group B consisted of 20 VIM-1-producers; group C consisted of 20 NDM-1-producers; and group D consisted of 20 KPC-2+VIM-1-producers. Bacterial identification and initial antimicrobial susceptibility testing of the isolates was performed using the VITEK2 automated system (bioMérieux, Marcy l’ Étoile, France), and the presence of carbapenemase-encoding genes was determined by phenotypic tests followed by polymerase chain reaction assays with specific primers to identify the presence of carbapenemases (ie, bla VIM, bla KPC, or bla NDM).Reference Tsakris, Poulou and Pournaras 5 , Reference Nordmann, Poirel, Carrër, Toleman and Walsh 6
The imipenem MICs for the 3 groups are shown in Table 1. Moreover, we calculated the geometric mean of the MIC values for each study group as the nth root (n=the number of isolates) of the product of the MIC values using a geometric mean calculator. (A value of 64 was used conventionally for isolates with MIC>32 μg/mL.) Groups A and C had lower geometric means (49.496 and 47.130, respectively) compared to the conventional 64.000 of B and D.
TABLE 1 Relation of Minimum Inhibitory Concentrations of Imipenem to Carbapenemase Presence in K. pneumoniae Isolates
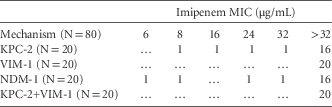
NOTE. MIC, minimum inhibitory concentration; KPC-2, Klebsiella pneumoniae carbapenemase-2; VIM-1, Verona integron-encoded metallo-β-lactamase-1; NDM-1, New Delhi metallo-β-lactamase-1.
Apparently, when studying large groups of carbapenemase-producing bacteria, more mechanisms may code for more resistance. This finding is in accord with the results of Kazi et al and with our previous study on carbapenem-resistant Pseudomonas aeruginosa, in which various mechanisms (eg, the VIM-2 carbapenemase, efflux pump over-expression, loss of the OprD porin, and the presence of inducible AmpC beta-lactamases) where taken into account.Reference Meletis, Vavatsi and Exindari 7
For single isolates, however, this cannot be considered the rule. Kazi et al found a Klebsiella spp. coproducing NDM-1 and VIM-1 with carbapenem MICs<2 μg/mL. Lower MICs in double-carbapenemase producers than those observed commonly in single-carbapenemase-producing isolates have also been observed elsewhere.Reference Meletis, Chatzidimitriou and Malisiovas 8 These findings can be attributed to the variable expression levels of the carbapenemase-encoding genes within bacterial cells and to the different hydrolytic potential of each enzymatic type. It is known, for example, that OXA-type carbapenemases have a lower potential of carbapenem hydrolysis than the metallo-beta-lactamases and Klebsiella pneumoniae carbapenemases.Reference Poirel, Potron and Nordmann 9
Interestingly, in our study, differences were not detected between groups B and D, probably because the presence of VIM-1 was enough to raise the imipenem MICs over 32 μg/mL for all 20 isolates of group B. Differences between these 2 groups may exist at higher MIC levels; however, these differences would be not relevant in clinical practice because the use of carbapenems, alone or in combination with other antibiotics, is not applicable with MIC values >32 μg/mL.
Overall, we agree with Kazi et al that the emergence of double-carbapenemase-producing bacteria is alarming and further confines the already limited treatment options.
ACKNOWLEDGMENTS
Financial support: No financial support was provided relevant to this article.
Potential conflicts of interest: All authors report no conflicts of interest relevant to this article.


