Crossref Citations
This article has been cited by the following publications. This list is generated based on data provided by
Crossref.
Drinka, Paul
2009.
Treatment of Bacteriuria Without Urinary Signs, Symptoms, or Systemic Infectious Illness (S/S/S).
Journal of the American Medical Directors Association,
Vol. 10,
Issue. 8,
p.
516.
O'Fallon, Erin
Schreiber, Robert
Kandel, Ruth
and
D'Agata, Erika M. C.
2009.
Multidrug-Resistant Gram-Negative Bacteria at a Long-Term Care Facility: Assessment of Residents, Healthcare Workers, and Inanimate Surfaces.
Infection Control & Hospital Epidemiology,
Vol. 30,
Issue. 12,
p.
1172.
Eveillard, M.
Lemarié, C.
Cottin, J.
Hitoto, H.
Mahaza, C.
Kempf, M.
and
Joly-Guillou, M.-L.
2010.
Assessment of the usefulness of performing bacterial identification and antimicrobial susceptibility testing 24 h a day in a clinical microbiology laboratory.
Clinical Microbiology and Infection,
Vol. 16,
Issue. 8,
p.
1084.
O'Fallon, Erin
Kandell, Ruth
Schreiber, Robert
and
D'Agata, Erika M. C.
2010.
Acquisition of Multidrug-Resistant Gram-Negative Bacteria: Incidence and Risk Factors within a Long-Term Care Population.
Infection Control & Hospital Epidemiology,
Vol. 31,
Issue. 11,
p.
1148.
Luzzaro, Francesco
Ortisi, Giuseppe
Larosa, Monica
Drago, Monica
Brigante, Gioconda
and
Gesu, Giovanni
2011.
Prevalence and epidemiology of microbial pathogens causing bloodstream infections: results of the OASIS multicenter study.
Diagnostic Microbiology and Infectious Disease,
Vol. 69,
Issue. 4,
p.
363.
Das, Rituparna
Towle, Virginia
Ness, Peter H.Van
and
Juthani-Mehta, Manisha
2011.
Adverse Outcomes in Nursing Home Residents with Increased Episodes of Observed Bacteriuria.
Infection Control & Hospital Epidemiology,
Vol. 32,
Issue. 1,
p.
84.
Ohl, Christopher A.
and
Luther, Vera P.
2011.
Antimicrobial stewardship for inpatient facilities.
Journal of Hospital Medicine,
Vol. 6,
Issue. S1,
Cataldo, Maria Concetta
Bonura, Celestino
Caputo, Giuseppe
Aleo, Aurora
Rizzo, Giovanna
Geraci, Daniela Maria
Calà, Cinzia
Fasciana, Teresa
Mattaliano, Anna Rita
and
Mammina, Caterina
2011.
Colonization of pressure ulcers by multidrug-resistant microorganisms in patients receiving home care.
Scandinavian Journal of Infectious Diseases,
Vol. 43,
Issue. 11-12,
p.
947.
Drinka, Paul
Niederman, Michael S.
El-Solh, Ali A.
and
Crnich, Christopher J.
2011.
Assessment of Risk Factors for Multi-Drug Resistant Organisms to Guide Empiric Antibiotic Selection in Long Term Care: A Dilemma.
Journal of the American Medical Directors Association,
Vol. 12,
Issue. 5,
p.
321.
van Duin, D.
2012.
Diagnostic Challenges and Opportunities in Older Adults With Infectious Diseases.
Clinical Infectious Diseases,
Vol. 54,
Issue. 7,
p.
973.
Pop-Vicas, Aurora
Shaban, Eman
Letourneau, Cecile
and
Pechie, Angel
2012.
Empirical Antimicrobial Prescriptions in Patients withClostridium difficileInfection at Hospital Admission and Impact on Clinical Outcome.
Infection Control & Hospital Epidemiology,
Vol. 33,
Issue. 11,
p.
1101.
Chen, Yin-Yin
Chen, Liang-Yu
Lin, Seng-Yi
Chou, Pesus
Liao, Shu-Yuan
and
Wang, Fu-Der
2012.
Surveillance on secular trends of incidence and mortality for device–associated infection in the intensive care unit setting at a tertiary medical center in Taiwan, 2000–2008: A retrospective observational study.
BMC Infectious Diseases,
Vol. 12,
Issue. 1,
Choi, Jae-Phil
Cho, Eun Ha
Lee, Seung Joon
Lee, Seung Tae
Koo, Myung Sook
and
Song, Young-Goo
2012.
Influx of multidrug resistant, Gram-negative bacteria (MDRGNB) in a public hospital among elderly patients from long-term care facilities: A single-center pilot study.
Archives of Gerontology and Geriatrics,
Vol. 54,
Issue. 2,
p.
e19.
Koliscak, Lindsey P.
Johnson, James W.
Beardsley, James R.
Miller, David P.
Williamson, John C.
Luther, Vera P.
and
Ohl, Christopher A.
2013.
Optimizing Empiric Antibiotic Therapy in Patients with Severe β-Lactam Allergy.
Antimicrobial Agents and Chemotherapy,
Vol. 57,
Issue. 12,
p.
5918.
Nayak, Nabakishore
Lenka, Rajesh K.
and
Padhy, Rabindra N.
2014.
Surveillance of multidrug resistant suppurative infection causing bacteria in hospitalized patients in an Indian tertiary care hospital.
Journal of Acute Disease,
Vol. 3,
Issue. 2,
p.
148.
Lim, C. J.
Cheng, A. C.
Kennon, J.
Spelman, D.
Hale, D.
Melican, G.
Sidjabat, H. E.
Paterson, D. L.
Kong, D. C. M.
and
Peleg, A. Y.
2014.
Prevalence of multidrug-resistant organisms and risk factors for carriage in long-term care facilities: a nested case-control study.
Journal of Antimicrobial Chemotherapy,
Vol. 69,
Issue. 7,
p.
1972.
Nathwani, Dilip
Raman, Gowri
Sulham, Katherine
Gavaghan, Meghan
and
Menon, Vandana
2014.
Clinical and economic consequences of hospital-acquired resistant and multidrug-resistant Pseudomonas aeruginosa infections: a systematic review and meta-analysis.
Antimicrobial Resistance and Infection Control,
Vol. 3,
Issue. 1,
Venkatachalam, Indumathi
Yang, Hsu Li
Fisher, Dale
Lye, David C.
Lin, Ling Moi
Tambyah, Paul
and
Perl, Trish M.
2014.
Multidrug-Resistant Gram-Negative Bloodstream Infections among Residents of Long-Term Care Facilities.
Infection Control & Hospital Epidemiology,
Vol. 35,
Issue. 5,
p.
519.
Lim, Ching Jou
Cheng, Allen C
Kong, David CM
and
Peleg, Anton Y
2014.
Community-onset bloodstream infection with multidrug-resistant organisms: a matched case-control study.
BMC Infectious Diseases,
Vol. 14,
Issue. 1,
Cei, Marco
Pardelli, Riccardo
Sani, Spartaco
and
Mumoli, Nicola
2014.
Local resistance patterns to antimicrobials in internal medicine: a focused report from the REGIMEN (REGistro Infezioni in MEdicina INterna) study.
Clinical and Experimental Medicine,
Vol. 14,
Issue. 1,
p.
77.
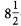 -year study period, the percentage of MDR gram-negative bacteria among bloodstream isolates increased from 2 (1%) of 199 to 34 (16%) of 216. Empiric therapy was ineffective for 38 (63%) of 60 patients with BSI caused by MDR gram-negative bacteria. The variables independently associated with BSI due to these bacteria were as follows: residency in a long-term care facility (odds ratio [OR], 4.9 [95% confidence interval {CI} 1.6–14.9]; P = .006), presence of an invasive device (OR, 6.0 [95% CI, 1.5–23.5]; P = .01), severe sepsis (OR, 7.9 [95% CI, 1.7–37.1]; P = .009), and delayed initiation of effective therapy (OR, 12.8 [95% CI, 3.9–41.1]; P<.001).
-year study period, the percentage of MDR gram-negative bacteria among bloodstream isolates increased from 2 (1%) of 199 to 34 (16%) of 216. Empiric therapy was ineffective for 38 (63%) of 60 patients with BSI caused by MDR gram-negative bacteria. The variables independently associated with BSI due to these bacteria were as follows: residency in a long-term care facility (odds ratio [OR], 4.9 [95% confidence interval {CI} 1.6–14.9]; P = .006), presence of an invasive device (OR, 6.0 [95% CI, 1.5–23.5]; P = .01), severe sepsis (OR, 7.9 [95% CI, 1.7–37.1]; P = .009), and delayed initiation of effective therapy (OR, 12.8 [95% CI, 3.9–41.1]; P<.001).

