Introduction
In Western societies, cardiovascular (CV) disease is the primary cause of mortality, and high blood pressure (BP) is the main reversible factor leading to CV disease (Kearny et al., Reference Kearny, Whelton, Reynolds, Muntner, Whelton and He2005; Cooper, Reference Cooper2007; Mancia et al., Reference Mancia, Laurent, Agabiti-Rosei, Ambrosioni, Burnier, Caulfield, Cifkova, Clément, Coca, Dominiczak, Erdine, Fagard, Farsang, Grassi, Haller, Heagerty, Kjeldsen, Kiowski, Mallion, Manolis, Narkiewicz, Nilsson, Olsen, Rahn, Redon, Rodicio, Ruilope, Schmieder, Struijker-Boudier, Van Zwieten, Viigimaa and Zanchetti2009). Dietary habits play a major role in preventing or even addressing the establishment of hypertension (Dickinson et al., Reference Dickinson, Mason, Nicolson, Campbell, Beyer, Cook, Williams and Ford2006; Cook et al., Reference Cook, Cutler, Obarzanek, Buring, Rexrode, Kumanyika, Appel and Whelton2007; Forman et al., Reference Forman, Stampfer and Curhan2009). It is also suggested that psychosocial stress contributes to the establishment of hypertension, while its role in the control of high BP is currently examined (Rainforth et al., Reference Rainforth, Schneider, Nidich, Gaylord-King, Salermo and Anderson2007; Khan et al., Reference Khan, Hemmelgarn, Herman, Rabkin, McAlister, Bell, Touyz, Padwal, Leiter, Mahon, Hill, Larochelle, Feldman, Schiffrin, Campbell, Arnold, Moe, Campbell, Milot, Stone, Jones, Ogilvie, Hamet, Fodor, Carruthers, Burns, Ruzicka, deChamplain, Pylypchuk, Petrella, Boulanger, Trudeau, Hegele, Woo, McFarlane, Vallée, Howlett, Katzmarzyk, Tobe and Lewanczuk2008; Spruill, Reference Spruill2010).
Several studies have searched into the role of specific dietary interventions, including low-sodium intake, high consumption of fruits and vegetables as well as low-fat dairy products, in the treatment of hypertension (Hooper et al., Reference Hooper, Barlett, Smith and Ebrahim2002; Sacks et al., Reference Sacks, Sacks, Appel, Brands, Daniels, Karanja and Patricia2006). The most popular dietary pattern that is currently recommended from the European guidelines for the control of high BP is the Dietary Approach to Stop Hypertension (DASH) diet with or without restriction of sodium intake (Mancia et al., Reference Mancia, Laurent, Agabiti-Rosei, Ambrosioni, Burnier, Caulfield, Cifkova, Clément, Coca, Dominiczak, Erdine, Fagard, Farsang, Grassi, Haller, Heagerty, Kjeldsen, Kiowski, Mallion, Manolis, Narkiewicz, Nilsson, Olsen, Rahn, Redon, Rodicio, Ruilope, Schmieder, Struijker-Boudier, Van Zwieten, Viigimaa and Zanchetti2009). In addition, the adherence to the Mediterranean dietary pattern, which is traditionally characterized by high intake of vegetables, fruits, legumes, unrefined cereals, nuts as well as high olive oil consumption instead of saturated lipids, moderately high intake of fish, low to moderate intake of dairies, meat and poultry, as well as a regular but moderate consumption of red wine mostly during meals (Willett et al., Reference Willet, Sacks, Trichopoulou, Drescher, Ferro-Luzzi, Helsing and Trichopoulos1995), has been found to be associated with lower prevalence of hypertension according to epidemiological studies (Psaltopoulou et al., Reference Psaltopoulou, Naska, Orfanos, Trichopoulos, Mountokalakis and Trichopoulou2004; Panagiotakos et al., Reference Panagiotakos, Pitsavos, Arvaniti and Stefanadis2007), whereas several published interventions have examined the effect of Mediterranean diet on CV risk (Singh et al., Reference Singh, Dubnov, Niaz, Ghosh, Singh, Rastogi, Manor, Pella and Berry2002; Vincent-Baudry et al., Reference Vincent-Baudry, Defoort, Gerber, Bernard, Verger, Helal, Portugal, Planells, Grolier, Amiot-Carlin, Vague and Lairon2005; Estruch et al., Reference Estruch, Angel, Martinez-Gonzalez, Corella, Salas-Salvado, Ruiz-Gutierrez, Covas, Fiol, Gomez-Gracia, Lopez-Sabater, Vinyoles, Aros, Conde, Lahoz, Lapetra, Saez and Ros2006; Salas-Salvadó et al., Reference Salas-Salvadó, Fernández-Ballart, Ros, Martínez-González, Fitó, Estruch, Corella, Fiol, Gómez-Gracia, Arós, Flores, Lapetra, Lamuela-Raventós, Ruiz-Gutiérrez, Bulló, Basora and Covas2008).
Several stress management techniques have been tested for their efficacy in reducing high BP (ie, biofeedback, yoga, transcendental meditation; Sandhu et al., Reference Sandhu, Berri, Gupta, Arya, Singh and Sandhu2004; Yucha et al., Reference Yucha, Tsai, Calderon and Tian2005). Although some interventions show contradictory results and nearly all underline the need for better designed studies, there is evidence supporting the positive effect of such techniques in reducing high BP. Among them, progressive muscle relaxation, diaphragmatic respirations (Wadden Reference Wadden1984; Knox et al., Reference Knox, Theorell, Malmberg and Lindqvist1986; Lucini et al., Reference Lucini, Malacarne, Solaro, Busin and Pagani2009) and cognitive-behavioral techniques, such as psychoeducation, cognitive restructuring, problem solving and time management skills (Timio et al., Reference Timio, Verdecchia, Venanzi, Gentili, Ronconi, Francucci, Montanari and Bichisao1988; Beck, Reference Beck1993; Campbell et al., Reference Campbell, Burgess, Choi, Taylor, Wilson, Cleroux, Fodor, Leiter and Spence1999) have been found to reduce high systolic and diastolic BP either alone or in combination in several studies (Bruning and Frew, Reference Bruning and Frew1987; Van der Hek and Plomp, 1997; Batey et al., Reference Batey, Kaufmann, Raczynski, Hollis, Murphy, Rosner, Corrigan, Rappaport, Danielson, Lasser and Kuhn2000).
To our knowledge, there are few interventional studies published that examine the combined effect of dietary education and stress management on the control of hypertension (Stuart et al., Reference Stuart, Caudill, Leserman, Dorrington, Friedman and Benson1987; Leserman et al., Reference Leserman, Stuart, Mamish, Deckro, Beckman, Friedman and Benson1989); in Greece there is, also, lack of such trials. Therefore, a combined intervention was designed to evaluate the effect of stress management techniques and dietary education, on the basis of the Mediterranean diet principles, on hypertensive individuals. The aim of the present pilot study was to detect the feasibility of such a project and detect methodological drawbacks that should be addressed in the design of the definitive study.
Methodology
Population
From November 2009 to February 2010, consecutive subjects, examined at the outpatient clinic of the hypertension center of two university hospitals, were asked to participate in the current study, on the basis of the following inclusion criteria: age: >18 years old; diagnosed hypertension according to the international guidelines (Mancia et al., Reference Mancia, Laurent, Agabiti-Rosei, Ambrosioni, Burnier, Caulfield, Cifkova, Clément, Coca, Dominiczak, Erdine, Fagard, Farsang, Grassi, Haller, Heagerty, Kjeldsen, Kiowski, Mallion, Manolis, Narkiewicz, Nilsson, Olsen, Rahn, Redon, Rodicio, Ruilope, Schmieder, Struijker-Boudier, Van Zwieten, Viigimaa and Zanchetti2009) under steady medical treatment (ie, for at least one month steady BP lowering drugs as well as any other type of drug); and office systolic/diastolic BP <20/10 mmHg above the individually defined BP target (Mancia et al., Reference Mancia, Laurent, Agabiti-Rosei, Ambrosioni, Burnier, Caulfield, Cifkova, Clément, Coca, Dominiczak, Erdine, Fagard, Farsang, Grassi, Haller, Heagerty, Kjeldsen, Kiowski, Mallion, Manolis, Narkiewicz, Nilsson, Olsen, Rahn, Redon, Rodicio, Ruilope, Schmieder, Struijker-Boudier, Van Zwieten, Viigimaa and Zanchetti2009). Exclusion criteria included inability to provide informed written consent and to participate in the intervention program because of mental or physical causes. Approval from the local ethics authorities was obtained.
Study design
This is a randomized controlled study. The eligible patients who agreed to participate in the study and signed the informed consent form were randomly assigned into the control and the intervention groups, based on a predefined automatically generated list. During the recruitment (ie, the baseline visit at the outpatient clinic), the baseline characteristics (socio-demographic and lifestyle characteristics – smoking, alcohol consumption, physical activity and employment and family status – CV risk factors and medication) were collected. At baseline as well as at the end of the study (second consecutive visit at the outpatient clinic after eight weeks), office BP, perceived stress levels and the degree of adherence to the Mediterranean diet were recorded by validated questionnaires. The pharmaceutical regimen did not change throughout the eight-month period in both groups. Participants were directed to keep the same level of physical activity during the intervention period as well.
As this was a pilot study, no sample size was calculated. We wished to identify the feasible recruitment rate in such a study within the reasonable time limits of a four-month period, taking into consideration that the pool of both eligible and non-eligible subjects visiting the two outpatient hypertension clinics is around 400.
Control group
The control group received the standard care, that is, their medication and the usual medical consultation on lifestyle modification based on the European Guidelines within the usual time frame (∼15 min) of the outpatient clinic.
Intervention group
The whole intervention lasted eight weeks. Participants in the intervention group were educated both on practicing stress management techniques as well as on the Mediterranean diet principles. After the recruitment, three appointments (one every 15 days: weeks two, four and six) took place, until the next evaluation of the BP at the outpatient clinic. These appointments took place at the facilities of the two hospitals and not at the outpatient clinic. Each appointment lasted about 90 min in groups of two to four people. At each appointment, participants first discussed issues regarding their dietary habits and Mediterranean diet and later were introduced to a stress management technique.
Education on nutrition – Mediterranean diet principles
The nutritional intervention consisted of counseling and education carried out by an experienced nutritionist. Personal dietary regimens based on the principles of Mediterranean diet, without altering energy balance (ie, isocaloric) and thus not promoting weight loss were also administered to the participants at the first appointment. During the second appointment, patients were informed about the role of sodium in the control of high BP and how to reduce its consumption. The third appointment provided the patients with further counseling, education and support to better adhere to the principles of Mediterranean dietary pattern in their daily life. During the second and the third session, matters of compliance were discussed.
Education on stress management techniques
At the first appointment, participants were introduced to the progressive muscle relaxation technique by a psychologist specialized in stress management and asked to perform it twice daily. Instructions were provided in recorded tapes to increase home adherence to the techniques. Each performance lasted about 15–20 min. At the second appointment, patients discussed with the psychologist the 15-day compliance with the foresaid technique, while participants were trained in performing diaphragmatic respirations and discussed problem solving techniques as well. At the last (third) appointment and after discussing matters of compliance, participants discussed the role of time management in the levels of perceived stress and were presented relevant techniques.
BP and anthropometric measurements
Office brachial BP was recorded at the outpatient clinic both at baseline as well as at the end of the study (during the regular follow-up visits) after at least 5 min of rest at the sitting position with validated automatic oscillometric devices (OMRON 750 IT, China (Coleman et al., Reference Coleman, Freeman, Steel and Shennan2006) or Microlife A100 plus, Switcherland (Stergiou et al., Reference Stergiou, Yiannes and Rarra2006)) and by applying the appropriate cuff size, according to the international guidelines (Mancia et al., Reference Mancia, Laurent, Agabiti-Rosei, Ambrosioni, Burnier, Caulfield, Cifkova, Clément, Coca, Dominiczak, Erdine, Fagard, Farsang, Grassi, Haller, Heagerty, Kjeldsen, Kiowski, Mallion, Manolis, Narkiewicz, Nilsson, Olsen, Rahn, Redon, Rodicio, Ruilope, Schmieder, Struijker-Boudier, Van Zwieten, Viigimaa and Zanchetti2009). The average of three consecutive BP readings, with 1 min interval in between, was used in the current analysis. In each subject, the same device at baseline and follow-up end was used. The physician who recorded the BP was blinded regarding the treatment allocation of each subject. Height and weight were measured at both visits, and body mass index (BMI) was calculated.
Questionnaires
Mediterranean diet score (MedDiet Score)
The MedDiet Score applied in the present study has been developed to evaluate the degree to which the Mediterranean dietary pattern is adopted; its total score ranges from 0 to 56, representing the lowest and highest stress levels, respectively. Consumption of foods close to the Mediterranean pattern was rated with higher values (ie, from 0 = never to 5 = highest consumption), whereas consumption of foods away from the Mediterranean diet principles was rated with an inverse scoring (Panagiotakos et al., Reference Panagiotakos, Polystipioti, Papairakleous and Polychronopoulos2007).
International physical activity questionnaire (IPAQ)
The shorter form of the IPAQ (Craig et al., Reference Craig, Marshall, Sjostrom, Bauman, Booth, Ainsworth, Pratt, Ekelund, Yngve, Sallis and Oja2003) was used in the present study, which examines various aspects of physical activity performed during the last week. IPAQ evaluates the type, frequency and duration of physical activity performed by people aged from 18 to 65 years in developed, as well as developing countries.
Perceived stress scale (PSS-14)
The PSS-14 evaluates the extent to which someone perceives his environment as stressful (Andreou et al., Reference Andreou, Alexopoulos, Lionis, Varvogli, Gnardellis, Chrousos and Darviri2011). Its officially translated Greek version (Cronbach's alpha 0,82) of the original PSS-14 was used in the present study. Half of the questions are considered as the positive items of the scale and the other half as the negative. The total score ranges from 0 to 56, representing the lowest and highest stress levels, respectively.
Statistical analysis
For the statistical analysis between the two groups at baseline and follow-up independent t-test, Wilcoxon or Fisher's exact test were used as appropriate, as well as paired for measuring the within-group difference before and after the intervention. SPSS.16 was used for all the above statistical analyses. The level of statistical significance was 0.05.
Results
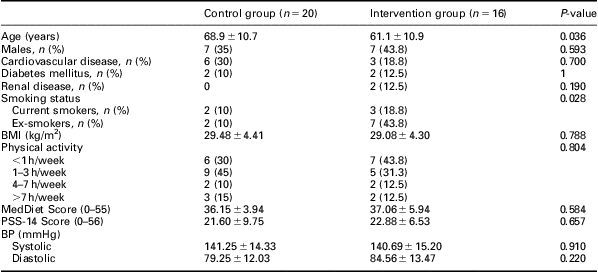
Thirty-six subjects were included in the final analysis (control group = 20 (31.8%, males) and intervention group = 16 (47%, males)) (Figure 1). The average age was significantly higher in the control versus the intervention group (69 ± 11 and 61 ± 11 years, P = 0.036, respectively). All participants were under steady treatment, except for one patient who did not receive pharmacological treatment at all. At baseline, the prevalence of CV disease risk factors between the two groups was similar, except for the prevalence of past and current smokers, which was higher in the intervention group. BP, MedDiet score, PSS-14 and physical activity (assessed by the IPAQ) were similar between the two groups at baseline (Table 1).

Figure 1 Study design and population.
Table 1 Baseline characteristics of participants assigned to both the control group and the intervention group

BMI = body mass index; PSS = perceived stress scale; BP = blood pressure.
Data are expressed as mean ± SD or number (%) of subjects.
P-values were assessed by independent t-test, Wilcoxon or Fisher's exact test as appropriate.
As shown in Table 2, no significant changes (end of the study – baseline) in the MedDiet score and PSS-14 were observed in the control group; BMI significantly increased at the end of the study in the control group. What is more, no significant changes regarding physical activity were observed in the two groups after completion of the study (data not shown in Table 2). In the intervention group, BMI did not change significantly from baseline, but PSS-14 significantly decreased and MedDiet score significantly increased, without any changes at the level of physical activity (as assessed by IPAQ). Finally, Table 2 describes the differences observed in BP; the intervention group showed significantly lower systolic BP after the completion of the intervention (P = 0.009); and the mean differences also appeared marginally significantly different between the two groups (P = 0.056). In addition, the intervention group showed significantly lower diastolic BP (P = 0.016), whereas no significant changes regarding diastolic BP between the two groups were observed.
Table 2 Changes after eight weeks (ie, end of the study – baseline) in the characteristics of the participants in both the control and the intervention group
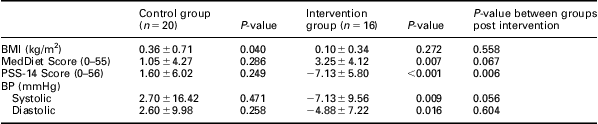
BMI = body mass index; PSS = perceived stress scale; BP = blood pressure.
All values are expressed as mean ± SD or n (%).
Discussion
In the present pilot study, the combined intervention on psychosocial stress management and nutrition education according to the Mediterranean diet principles reduced significantly office BP, both systolic and diastolic, in a small sample of hypertensive patients. Moreover, in the intervention group, significant reduction in the perceived stress and an increase in the adherence in Mediterranean diet principles were found, without changes in the physical activity levels and BMI. On the contrary, no significant changes were observed in BP, MedDiet score and PSS-14 score in the control group. Most importantly, a high percentage of eligible patients who declined to participate, after detailed description of the interventional protocol just before the randomization, were observed in the eligible for participation in the study subjects.
Regarding the psychosocial stress evaluation, participants of both groups were characterized by moderate levels of perceived stress at baseline. Only the intervention group presented a significant reduction in perceived stress levels by the completion of the study, suggesting that frequent performance of relaxation techniques may facilitate the individual's adjustment to stressful situations.
In the studied population, the adoption of the Mediterranean pattern was moderate and similar to the level of adherence of the general Greek population (Panagiotakos et al., Reference Panagiotakos, Pitsavos, Chrysohoou, Skoumas, Papadimitriou, Stefanadis and Toutouzas2003). Although no significant difference in the adoption of the Mediterranean dietary pattern was found in the control group after the eight-week period, the intervention group increased its compliance to the Mediterranean dietary principles (Panagiotakos et al., Reference Panagiotakos, Pitsavos and Stefanadis2006).
The parameters of BMI and physical activity were kept generally constant in the intervention group, as was intended from the study design. The intervention group showed a small increase regarding their overall physical activity. We speculate that increasing physical activity leads to a reduction in perceived stress through one of two mechanisms: active people are distracted from thinking about stress, or that activity stimulates biochemical changes that dampen stress perception.
Most importantly, it is interesting to point out the difficulty of some participants to accept the nature of the intervention and thus were not randomized, whereas others (see Figure 1) did not complete the study. These facts underline the unfamiliarity of the Greek population regarding such interventions (no similar studies have been conducted or at least published in Greece) and a relevant lack of motivation to participate and comply.
Limitations
The current pilot study was not double-blinded and the study sample was small. The randomization procedure was confounded by the relative high rate of refusal to participate and to continue to follow the intervention correctly. However, at least the main co-morbidities were explored and found to be comparable between the two groups, except for the higher prevalence of smoking in the intervention group. What is more, as the average age of the intervention group was smaller than in the control group, we cannot exclude the fact that this might have an impact on the BP changes that were observed. The observed decrease in BP, although statistically significant, has to be further verified by future studies that will assess out-of-office BP as well. In parallel, the long-term compliance to these non-pharmacological treatment strategies remains a major unresolved issue that may potentially restrict the efficacy of these interventions and the extrapolation of the results from short-term studies (Appel et al., Reference Appel, Moore, Obarzanek, Vollmer, Svetkey, Sacks, Bray, Vogt, Cutler, Windhauser, Pao-Hwa, Karanja, Simons-Morton, McCullough, Swain, Steele, Evans, Miller and Harsha1997; Sacks et al., Reference Sacks, Svetkey, Vollmer, Appel, Bray, Harsha, Obarzanek, Conlin, Moore, Miller, Simons-Morton, Karanja and Pao-Hwa2001). Furthermore, there was no tool used to assess compliance with dietary advice and stress management techniques in between the sessions, although matters of compliance were thoroughly discussed orally. Finally, the age of participants did not fall precisely enough into the age range that IPAQ has been tested as valid and, probably, the high rate of refusal to participate may have contributed. Finally, the present study cannot provide a direct association between the reduction of the perceived stress, the adherence to Mediterranean diet principles and the reduction of BP because of the limited sample size and lack of measurement of potential mediators (eg, cortisol and catecholamine).
Conclusions and perspectives
A combined intervention of stress management techniques and Mediterranean diet education seems to be beneficial, despite the methodological limitations of the current study. Such interventions could possibly serve as a complementary treatment along with drug therapy in favor of high BP control. However, BP response to treatment is limited in the presence of established arterial alterations, even when intense pharmacological treatment (ie, combination of drugs) is used (Protogerou et al., Reference Protogerou, Blacher, Stergiou, Achimastos and Safar2009). For that reason, the 2009 reappraisal of the European guidelines favors the early treatment on high BP before the development of target organ damage (Mancia et al., Reference Mancia, Laurent, Agabiti-Rosei, Ambrosioni, Burnier, Caulfield, Cifkova, Clément, Coca, Dominiczak, Erdine, Fagard, Farsang, Grassi, Haller, Heagerty, Kjeldsen, Kiowski, Mallion, Manolis, Narkiewicz, Nilsson, Olsen, Rahn, Redon, Rodicio, Ruilope, Schmieder, Struijker-Boudier, Van Zwieten, Viigimaa and Zanchetti2009). Future studies evaluating the efficacy of non-pharmacological treatment strategies, such as stress management techniques and adherence to Mediterranean diet principles, in the early treatment of high normal BP before arterial remodeling and stiffening takes places is therefore warranted. Most importantly, from a public health perspective, the current study highlights the need to increase awareness of the general population regarding the role of psychosocial stress in BP management.
Acknowledgements
The authors gratefully thank all the patients who participated in this work.