Brain imaging has transformed psychiatric research in recent decades. Many of these imaging techniques, including computed tomography (CT) and magnetic resonance imaging (MRI), are also commonly used in clinical practice. These technologies are costly: in Ireland, each episode of brain CT costs £362 (€460) and each episode of brain MRI costs £476 (€605; costings provided by the Department of Radiology, Mater Misericordiae University Hospital, Dublin).
There is a paucity of research on the clinical usefulness of brain imaging in general adult psychiatric practice. Reference Sharma and Sheringham1 Although it is clear that imaging technologies provide researchers with ever-improving information about the structure and function of the brain, it is unclear to what extent, if any, these technologies contribute to diagnostic or therapeutic processes in general adult psychiatry settings. We aimed to explore clinical indications for, and results of, brain imaging in a department of general adult psychiatry in Dublin, Ireland.
Method
The study was performed in the Department of Adult Psychiatry at the Mater Misericordiae University Hospital, Dublin, Ireland. This department provides psychiatric care to adults (aged 16 years and over) residing in a geographically defined catchment area with a population of 33 000 in Dublin's inner city. This is one of the most socioeconomically deprived catchment areas in Ireland: over half of the population falls within the most deprived socioeconomic category (category 10). Reference Kelly and Teljur2,3 The department also provides a liaison psychiatry service to a busy general hospital with departments of medicine, surgery and various other specialties. In this department, it is not standard practice for every patient with first-episode psychosis to undergo brain imaging.
In January 2008, we reviewed the most recent 100 episodes of brain CT and MRI performed at the request of the Department of Adult Psychiatry; all scans included in this study were performed on in-patients in the psychiatry ward. For each scan, we used the hospital computer system to extract the patient's age, gender, the clinical indication for the scan and the result (as reported by the consultant radiologist).
Each computerised request and result was examined by two of the authors (M.D. and B.D.K.) and agreement was reached on relevant variables. Data were recorded, described and analysed using the SPSS version 12.0 for Windows.
Results
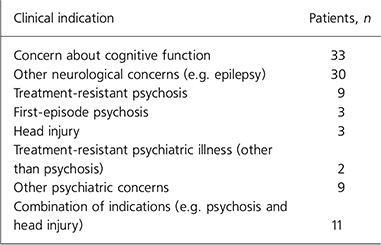
The most recent 100 scans performed on in-patients at the Department of Adult Psychiatry at the Mater Misericordiae University Hospital included 62 CTs and 38 MRIs of the brain. Patients had a mean age of 55.30 years (s.d. = 16.71, range 19–89). A total of 52 scans were performed on female patients and 48 on male patients. The most common indications for the scan were concern about cognitive function (n = 33) and other neurological concerns (n = 30), for example confusion and seizures; other indications are shown in Table 1.
Table 1. Clinical indications for brain imaging in general adult psychiatry (n = 100)
| Clinical indication | Patients, n |
|---|---|
| Concern about cognitive function | 33 |
| Other neurological concerns (e.g. epilepsy) | 30 |
| Treatment-resistant psychosis | 9 |
| First-episode psychosis | 3 |
| Head injury | 3 |
| Treatment-resistant psychiatric illness (other than psychosis) | 2 |
| Other psychiatric concerns | 9 |
| Combination of indications (e.g. psychosis and head injury) | 11 |
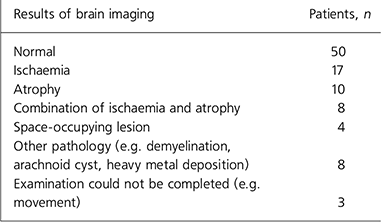
Overall, 50 scans were normal, 47 were abnormal and 3 could not be completed for technical reasons (e.g. patient movement). The most common abnormalities were ischaemia (n = 17), atrophy (n = 10) and a combination of the two (n = 8); other abnormalities are shown in Table 2. The mean age of patients with abnormal scans (61.9 years, s.d. = 12.51) was higher than that of patients with normal scans (48.7 years, s.d. = 17.86; t = –4.28, P < 0.001), but there was no gender difference between patients with normal and those with abnormal scans (χ2 = 0.16, P = 0.84). All three individuals with first-episode psychosis had normal scans.
Table 2. Results of brain imaging in general adult psychiatry (n = 100)
| Results of brain imaging | Patients, n |
|---|---|
| Normal | 50 |
| Ischaemia | 17 |
| Atrophy | 10 |
| Combination of ischaemia and atrophy | 8 |
| Space-occupying lesion | 4 |
| Other pathology (e.g. demyelination, arachnoid cyst, heavy metal deposition) | 8 |
| Examination could not be completed (e.g. movement) | 3 |
Discussion
Findings of clinical significance (e.g. ischaemia, atrophy) were found in 47% of scans examined in this study and abnormal findings were more likely with older age. The relatively high rate of abnormality in these scans suggests that brain imaging facilities are being used appropriately by the department and that there may be scope for greater use of brain imaging, especially for older patients. Our findings also provide broad support for the usefulness of brain imaging in day-to-day in-patient clinical psychiatry. Reference Sharma and Sheringham1
Limitations
One possible limitation of this study is our reliance on scan reports by radiologists rather than our own interpretation of the scans. However, this was a conscious decision on our part, as we sought to examine the usefulness of brain imaging in a real life setting in which psychiatrists are likely to rely significantly on reports by radiologists. All patients in this study were in-patients on a psychiatry ward and this limits the generalisability of findings to other groups. Another possible limitation relates to the structure of our department – it includes a liaison psychiatry service that may tend to generate a higher rate of abnormal scans than might be seen in departments without a liaison psychiatry service. On the other hand, our findings may be generalisable to the many departments of psychiatry that incorporate elements of both general adult and liaison psychiatry.
This study did not include data on whether or not the patients had diagnoses before brain scans (e.g. had dementia been diagnosed prior to a scan showing ischaemia?); whether or not previous imaging had been performed (e.g. did patients who had an MRI previously have a CT?); and whether or not any such previous scans were normal or abnormal. These issues could be usefully examined in future studies.
Strengths
The strengths of this study include its focus on the diagnostic usefulness of a common, costly and under-researched clinical investigation (brain imaging), and our use of a consecutive series of 100 episodes of brain imaging in order to reflect ‘real life’ in-patient clinical practice. The data on costings are particularly interesting – the 100 scans included in this study were at a total cost of £40 776 (€51510). We feel that the high rate of abnormality reported in these scans suggests that brain imaging facilities are being used appropriately in our department, and that there may be scope for greater use of brain imaging in the future, especially for older patients. Given the low number of individuals with first-episode psychosis in this study (n = 3), it is not possible to draw specific conclusions about the clinical usefulness of scanning in this group; future studies might address this. Future research could also usefully focus on the indications for, and results of, brain imaging in other comparable departments of adult psychiatry in order to identify any geographical variations in practices across different hospitals or different countries. In addition, it would be useful to follow-up such studies by reviewing clinical notes and identifying the extent to which scan results affect therapeutic practice in clinical psychiatry.
Declaration of interest
None.
Acknowledgements
We thank the Department of Radiology, Mater Misericordiae University Hospital, Dublin, for their cooperation with this study.





eLetters
No eLetters have been published for this article.