Widespread attention to the burden of food insecurity in the USA and increased understanding of its adverse health impact have prompted many health systems to initiate programmes to screen for food insecurity. In October 2015, the American Academy of Pediatrics issued a position statement recommending universal screening for food insecurity in the clinical setting( 1 ). Soon afterwards, the American Diabetes Association released its Standards of Medical Care in Diabetes – 2016, which for the first time recognized the unique self-management challenges associated with food insecurity( 2 ). The Center for Medicare & Medicaid Innovation recently launched a 5-year, $US 157 million programme to test the impact of clinical screening for health-related social needs, specifically including food insecurity. These Accountable Health Communities will test models for linking patients with social needs to community resources in order to reduce health-care costs and utilization( Reference Alley, Asomugha and Conway 3 ).
Food insecurity (defined as a household-level economic and social condition of limited access to food) has emerged as a leading health-care issue for two central reasons. First, food insecurity rates in the USA continue to be very high: in 2015, 12·7 % of US households, comprising more than 42 million people, were food insecure( Reference Coleman-Jensen, Rabbitt and Gregory 4 ). Second, food insecurity is associated with higher health-care costs( Reference Tarasuk, Cheng and Oliveira 5 ) and poor health outcomes( Reference Gundersen and Ziliak 6 ) for both adults and children, suggesting it may be an important driver of some health disparities.
Many food insecurity screening programmes have thus been recently implemented in clinical settings, under the assumption that provider recognition and action will mitigate poor health outcomes. These programmes generally use a two-item clinical screening tool based on the US Department of Agriculture’s eighteen-item Core Food Security Module (CFSM)( 7 , 8 ). However, these screeners have been formally tested only in narrow populations (caregivers of children enrolled in a single study, or forty-nine HIV-positive patients) and their relevance to the broader population is unclear( Reference Hager, Quigg and Black 9 , Reference Young, Jeganathan and Houtzager 10 ). Prior to widespread dissemination of screening programmes such as those being advocated by professional organizations, it is critical to understand the test characteristics of measurement tools in the general population and among high-risk demographic groups.
Methods
We used data from the December Supplement to the 2013 Current Population Survey (CPS)( 7 , 8 ). CPS is a household-level survey conducted monthly by the US Census Bureau for the Bureau of Labor Statistics with the primary goal of tracking the labour market. It includes data collected in-person or by telephone from 60 000 nationally representative households. Food insecurity estimates from CPS are used to construct official estimates of US food insecurity( Reference Coleman-Jensen, Rabbitt and Gregory 4 ). The eighteen items of the CFSM have been included during a single administration of CPS annually since 1996. This annual administration has occurred in December since 2001.
We calculated sensitivity and specificity of various two-item combinations suitable for use as clinical screening tools using the US Department of Agriculture’s CFSM as a reference measure. We examined: the two items recommended as screening tools in previous studies( Reference Hager, Quigg and Black 9 , Reference Young, Jeganathan and Houtzager 10 ) (items 1 and 2 or items 2 and 3 on the CFSM); all possible two-item combinations from an often-used six-item subset of the CFSM( Reference Young, Jeganathan and Houtzager 10 ) (items 2–7); and items 1 and 3 on the CFSM (Table 1). For each, we considered an affirmative response to either question to indicate food insecurity, as previous clinical screening tools for food insecurity have done. We used standard definitions of sensitivity, specificity and overall accuracy( Reference Alberg, Park and Hager 11 ). Because risks associated with misidentifying a patient as food insecure are low, we sought to maximize sensitivity without unreasonably decreasing specificity.
Table 1 Core Food Security Module items examined for use in two-item screeningFootnote *

* The US Department of Agriculture provides public access to the complete Core Food Security Module and its scoring algorithm at http://www.ers.usda.gov/topics/food-nutrition-assistance/food-security-in-the-us/survey-tools.aspx ( Reference Nord 14 ).
† Response options considered affirmative are: Often true, Sometimes true, Yes, Almost every month, and Some months but not every month.
Results
Sensitivity of each two-item combination was high for the US population and high-risk demographic groups compared with the eighteen-item CFSM (Table 2). Sensitivity ranged from 96·4 % for items 2 and 3 for households with children and incomes <200 % of the federal poverty line, to 99·8 % for items 1 and 3 for Spanish-speaking households. (results for all combinations are available from the corresponding author upon request). Specificity was lower, ranging from 73·7 % for items 1 and 2 for households with children and incomes <100 % of the federal poverty line, to 94·5 % for items 2 and 3 for households with a respondent aged >60 years. Accuracy was high for all two-item combinations.
Table 2 Sensitivity and specificity for two-item combinations from the Core Food Security ModuleFootnote *
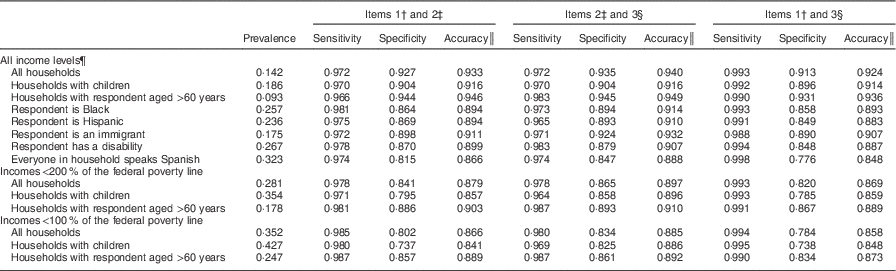
* Data are from the 2013 December Supplement of the Current Population Survey.
† Item 1 asks: ‘We worried whether our food would run out before we got money to buy more.’ Was that often, sometimes, or never true for you in the last 12 months? (responses of sometimes or often are counted as ‘affirmative responses’).
‡ Item 2 asks: ‘The food that we bought just didn’t last and we didn’t have money to get more.’ Was that often, sometimes, or never true for you in the last 12 months? (responses of sometimes or often are counted as ‘affirmative responses’).
§ Item 3 asks: ‘We couldn’t afford to eat balanced meals.’ Was that often, sometimes, or never true for you in the last 12 months? (responses of sometimes or often are counted as ‘affirmative responses’).
║ Defined as sensitivity×prevalence+specificity×(1–prevalence).
¶ The total number of unweighted observations is 42 081 households.
Discussion
Nationally representative data suggest a two-item screening tool can accurately identify household food insecurity. Any combinations described have acceptable sensitivity and specificity for widespread clinical use, and each combination has advantages: items 1 and 2 have been widely disseminated as the Hunger Vital Sign™ and were recommended by the American Academy of Pediatrics( 1 , 12 ); items 2 and 3 are a subset of the six-item scale; and items 1 and 3 have the highest sensitivity across the population.
There are limitations to using a two-item screening tool, rather than the US Department of Agriculture’s full eighteen-item (or six-item subset) reference measure acceptable for research. First, clinical screening tools do not allow assessment of the severity of food insecurity (food secure, marginally food secure, low food secure, very low food secure). Second, two-item measures cannot address all aspects of the complex experience of food insecurity. However, longer food insecurity measurement tools are not compatible with the time demands of clinical practice.
We thus believe that a two-item measure is an acceptable compromise for clinical practice. Based on our findings, we recommend clinical screening programmes use items 1 and 2 from the CFSM for screening (with a response of ‘sometimes’ or ‘often’ true to either question consistent with food insecurity), as follows:
Now I’m going to read you several statements that people have made about their food situation. For these statements, please tell me whether the statement was often true, sometimes true, or never true for (you/your household) in the last 12 months – that is, since last (name of current month).
-
∙ The first statement is ‘We worried whether (my/our) food would run out before (I/we) got money to buy more.’ Was that often true, sometimes true, or never true for (you/your household) in the last 12 months?
-
∙ ‘The food that (I/we) bought just didn’t last and (I/we) didn’t have money to get more.’ Was that often true, sometimes true, or never true for (you/your household) in the last 12 months?
We recommend items 1 and 2 because a common tool implemented across clinical settings greatly expands our ability to monitor food insecurity and its clinical consequences. Items 1 and 2 are the most frequently used in clinical screening programmes and some electronic health record systems are already working to integrate these two items. In addition, item 3 is susceptible to varying interpretations by age and cultural background( Reference Wolfe, Frongillo and Valois 13 ).
Conclusions
Brief measures of food insecurity have adequate test characteristics for widespread clinical adoption. Positively identifying patients living in food-insecure households in the clinical setting may allow health-care providers to better tailor diet counselling, link patients with food resources, or alter clinical management to accommodate the challenges of living in a food-insecure household.
Acknowledgements
Financial support: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Conflict of interest: None. Authorship: C.G. did the analytical work and contributed to the construction of the paper and its write-up. H.K.S., A.S.C. and E.E.E. contributed to the construction of the paper and its write-up. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects/patients were approved by the UCSF Human Research Protection Program Institutional Review Board. Written informed consent was obtained from all subjects/patients.







