The cognitive model of psychosis proposed by Garety et al (Reference Garety, Kuipers and Fowler2001) is a multidimensional model encompassing cognitive disturbances, emotional response and arousal, search for meaning, and social factors. Like other psychological models of psychotic symptoms (Reference BentallBentall, 1990; Reference MorrisonMorrison, 2001) it postulates a defining role for appraisals in determining the transition from anomalous experiences, reported in otherwise healthy people (Reference Johns and vanJohns & van Os, 2001), to full-blown psychosis. Multidimensional assessments of anomalous experiences and their appraisals, as well as the individuals' emotional, cognitive and behavioural responses to such experiences, are necessary to test the hypotheses generated by such models. The Appraisals of Anomalous Experiences Interview (AANEX) was therefore developed to measure psychotic-like experiences, and psychological and contextual variables relevant to individuals' interpretations and responses to them. The present study describes the AANEX and steps taken to validate it by comparing individuals reporting anomalous experiences with and without a diagnosis of psychosis and need for care.
METHOD
Sample
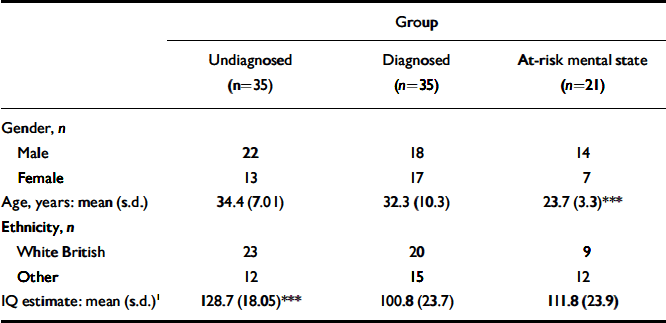
The sample consisted of three groups of participants reporting anomalous experiences associated with psychosis: (a) individuals with a DSM–IV (American Psychiatric Association, 1994) diagnosis of a psychotic disorder (‘diagnosed group’ n=35), (b) help-seeking individuals meeting criteria for an ‘at risk mental state’ (n=21), and (c) individuals who had never received treatment for a diagnosis of psychotic disorder but had at least occasional experiences of any Schneiderian first-rank symptom (‘undiagnosed group’ n=35). Table 1 summarises the demographic features of the three groups.
Table 1 Demographic details of groups
| Group | |||
|---|---|---|---|
| Undiagnosed (n=35) | Diagnosed (n=35) | At-risk mental state (n=21) | |
| Gender, n | |||
| Male | 22 | 18 | 14 |
| Female | 13 | 17 | 7 |
| Age, years: mean (s.d.) | 34.4 (7.01) | 32.3 (10.3) | 23.7 (3.3)*** |
| Ethnicity, n | |||
| White British | 23 | 20 | 9 |
| Other | 12 | 15 | 12 |
| IQ estimate: mean (s.d.)1 | 128.7 (18.05)*** | 100.8 (23.7) | 111.8 (23.9) |
The diagnosed group included 14 people recruited from an in-patient unit and linked community team specialising in the treatment of people with a first or second episode of psychosis (Lambeth Early Onset Team, LEO), and 21 people recruited via a specialist tertiary service providing psychological interventions for out-patients with psychosis (Psychological Intervention Clinic for Outpatients with Psychosis; PICuP), both in the South London and Maudsley Trust, UK.
The group with at-risk mental state was recruited through Outreach and Support in South London (OASIS), also based in the South London and Maudsley Trust, a clinical service for people meeting the Personal Assessment and Crisis Evaluation Clinic (PACE) criteria for an at-risk mental state (Reference Phillips, Yung and McGorryPhillips et al, 2000).
The undiagnosed group was recruited from multiple sources through advertisement to obtain a sample with as much variety in socio-economic and cultural background as possible. All volunteers were screened for suitability with a self-report questionnaire which enquired about lifetime incidence of the range of anomalous experiences that make up the inventory section of the AANEX. Only individuals with at least occasional experiences of any Schneiderian first-rank symptom which was not directly related to drug use and occurred under conditions of clear consciousness were invited to participate. Only those whose anomalous experiences had commenced more than 5 years previously but who had never been treated or sought clinical help were included. This was to distinguish this group from those with at-risk mental state by minimising the likelihood that they would develop a need for care relative to these experiences in the future.
Exclusion criteria for all three groups were inability to speak fluent English, a history of neurological problems, head injury or epilepsy, evidence of current substance dependence and estimated current IQ<70.
The undiagnosed and diagnosed groups did not differ significantly significantly in age; however, those with at-risk mental state were significantly younger than the undiagnosed group (mean difference 0.362, 95% 0.201–0.524, P<0.001), as a result of the selection criteria (i.e. anomalous experiences having been present for at least 5 years). There were no group differences in gender ratio or ratio of British Whites to other ethnic categories. There were significant group differences in estimated IQ (Bonferroni corrected), with the undiagnosed group having a higher mean IQ than either of the clinical groups (undiagnosed>diagnosed, mean difference 26.4, 95% CI 10.2–42.6; P<0.001; undiagnosed>at-risk mental state, mean difference 16.9, 95% CI 33.3–0.48, P=0.04).
Development of the AANEX
The AANEX was developed in sequential stages, beginning with exploratory in-depth interviews. Initially, a preliminary interview schedule was created to explore the variables suggested to be pertinent by the cognitive models (e.g. Reference Fowler, Birchwood, Fowler and JacksonFowler, 2000; Reference Garety, Kuipers and FowlerGarety et al, 2001) and to gather information that might suggest additional dimensions of interest. Interviews were then carried out with six participants with a history of anomalous experiences, three of whom had been treated for a psychotic disorder and three of whom had not.
On the basis of the information gained from the preliminary interviews, a more structured interview schedule was developed. The in-depth interviews demonstrated that people's appraisals and responses do not remain static but change over time. For this reason, a format was developed that enabled assessment of more than one time period in an individual's life, including the first onset and current experiences, and also other intermediate time periods. Sets of items can be repeated to yield scores for each relevant time period and/or each particular form of anomalous experience that is reported, giving different ‘response sets’.
The next stage involved the piloting of this interview schedule on 10 participants, including individuals diagnosed with a psychotic disorder, those considered to be at risk of psychosis and those who had not received a diagnosis.
All elements of the interview schedule were tested repeatedly in a process of iterative modification and trial, until a final version was reached, which only incorporated useful and reliable questions that yielded easily and usefully codable responses. Particular attention was paid to establishing a flexible structure that would allow responses of different groups to specific experiences to be compared. The development of the scoring scheme, using ordinal (rather than dichotomous) ratings and open-ended questions, aimed to reflect and capture the continua of belief, feelings and responses expressed by the participants.
A cross-sectional pilot comparison was then carried out between a sample of undiagnosed participants (n=8) and diagnosed participants (n=8), using the final version of the interview. Results included two trends towards significant differences in types of appraisal between the two groups, despite the small samples. The interview was acceptable to all participants. Copies of the AANEX Interview and the users' manual are available from C.M.C.B.
Components of the AANEX
AANEX-Inventory
The first section of the AANEX is the inventory, which includes items reflecting Schneiderian first-rank symptoms and anomalies of perception, cognition, affect and ‘individuation’ (sense of distinction between self and other), as well as some ‘paranormal’ experiences. This was generated by drawing on experiences enquired about in the Wisconsin Manual for Assessing Psychotic-like Experience WMAPE; Reference Kwapil, Chapman and ChapmanKwapil et al, 1999), the Comprehensive Assessment of At-Risk Mental States (CAARMS; PACE clinic, 2000 version; Reference YungYung, 2000) and items taken from the Bonn Scale for the Assessment of Basic Symptoms (BSABS; Reference Gross, Huber and KlosterkotterGross et al, 1987), which were reported to be predictive of subsequent psychotic illness (Reference Klosterkotter, Ebel and Schultze-LutterKlosterkotter et al, 1996), as well as additional experiences drawn from the accounts of participants in the early stages of piloting.
Particular emphasis was placed on distinguishing experiences from their appraisals but at the same time developing probe questions that allowed for endorsement of the experience by a range of individuals with differing interpretations. Several experiences were included which might usually be considered examples of delusional content but which emerged during the pilot phases as common, relatively autochthonous experiences (e.g. the sense of ‘revelation’ of insights or personal missions). The inventory generates two sets of scores: lifetime and state. For the lifetime scores each item is rated between 1 and 5 based on the frequency or pervasiveness of the experience across an individual's lifetime. The data can be summarised into five lifetime component scores, derived from a principal components analysis (further details on request).
The state scores capture an individual's experiences during a specified period, such as the time of assessment, or the period when particular experiences first began. A subset of 19 key items (Appendix) are rated between 0 and 2 (absent, marginal and present) at each selected time point and can be summarised into four state component scores. For each component the scores of each of the 19 items were multiplied by the correlation between the item and the component, and the results summed to yield a continuous component score. The anomalous experiences reported at each time point are then used to anchor the second section of the interview.
AANEX-CAR
The second section assesses appraisals, context and response (AANEX–CAR) pertaining to particular anomalous experiences endorsed from the inventory. It can also be used independently from the inventory to explore anomalies elicited with other clinical instruments. Responses are rated on Likert scales ranging from 0 to 2, 1 to 5, or 0 to 5. Verbatim responses can be recorded for all items for qualitative analysis.
Domains relevant for assessment were initially identified on the basis of psychological models of the development of psychosis published by Bentall (Reference Bentall1990), Garety et al (Reference Garety, Kuipers and Fowler2001) and Morrison (Reference Morrison2001). Further domains were subsequently derived from the in-depth and pilot interviews. The variables assessed by the final version of the AANEX can be seen in Table 2. Probe questions used to elicit the data are shown in the data supplement to the online version of this paper.
Table 2 Summary of domains and items comprising the AANEX, and the scoring scheme for each item.1

| Domain | Item(s) | Scoring scheme | |
|---|---|---|---|
| Scale | Anchors | ||
| Inventory | See Appendix | ||
| Lifetime | 1-5 | 1=never; | |
| 5=very frequent | |||
| State | 0-2 | 0=no | |
| 1=marginal; | |||
| 2=yes | |||
| Context of onset | |||
| Situation | Significant change | 0-2 | 0=no |
| Social isolation | 0-2 | 1=marginal | |
| Crisis/impasse | 0-2 | 2=yes | |
| Drug use | 0-2 | ||
| Trauma | 0-2 | ||
| Religious/spiritual practice | 0-2 | ||
| Cultural context | 0-2 | ||
| From childhood | 0-2 | ||
| Feelings | Exhaustion | 0-2 | 0=no |
| Depression | 0-2 | 1=marginal | |
| Anxiety | 0-2 | 2=yes | |
| Deep relaxation | 0-2 | ||
| Elation | 0-2 | ||
| Appraisal | |||
| Dimensions | Valence | 1-5 | 1=negative, 5=positive |
| Dangerousness | 1-5 | 1=benign, 5=dangerous | |
| Externality | 1-5 | 1=internal, 5 = external | |
| Agency | 1-5 | 1=impersonal, 5=personal | |
| Categories | Biological | 0-2 | 0=no |
| Psychological | 0-2 | 1=marginal | |
| Drug-related | 0-2 | 2=yes | |
| Spiritual | 0-2 | ||
| Supernatural | 0-2 | ||
| Normalising | 0-2 | ||
| Other people | 0-2 | ||
| No interpretation | 0-2 | ||
| Emotional response | Neutral arousal | 1-5 | 1=none |
| Negative emotional response | 1-5 | 5=predominantly | |
| Positive emotional response | 1-5 | ||
| Self-rated anxiety | 1-5 | 1=not at all | |
| Self-rated excitement | 1-5 | 5=as anxious/excited as ever been | |
| Cognitive and behavioural response2 | Avoidance | 1-5 | 1=no responses of this kind |
| Cognitive control | 1-5 | 5=only responses of this kind | |
| Reappraisal | 1-5 | ||
| Immersion | 1-5 | ||
| (Rumination) | |||
| (Neutral) | |||
| Context of appraisal | Impact on self esteem | 1-5 | 1=greatly ↓, 5=greatly ↑ |
| Perceived social understanding | 1-5 | 1=keep quiet | |
| 5=definitely understand | |||
| Perceived controllability | 1-5 | 1=none, 5=total | |
| Attempted control | 1-5 | 1=not at all, 5=total effort | |
| Premorbid awareness | 1-5 | 1=no prior awareness | |
| 5=knew all about | |||
| 1=not at all (0%) | |||
| Intellectual involvement | 1-5 | 5=crucial need to understand (100%) | |
| Alternative Interpretations | Appraisal categories (see above) each of which is probed in turn | 0-2 | 0=definitely not valid |
| 1=perhaps | |||
| 2=definitely valid | |||
| Implications of appraisal | Perceived prevalence of experience | 0-5 | 0=unique |
| 5=100% of social group | |||
| Perceived potential for others to have experience | 0-5 | 0=unique | |
| 5=everyone has potential | |||
| Impact on worldview plus open-ended probe | 1-5 | 1=no effect | |
| 5=completely changed plus verbatim answer | |||
| Impact on self-understanding plus open-ended probe | 1=no effect | ||
| 5=completely changed plus verbatim answer | |||
| Open section | Other important aspects of your experience? | NA | Verbatim answer |
| Anything that has helped you to cope with having the experiences? | NA | Verbatim answer | |
The format is flexible: subsections can be omitted to constitute a brief form which assesses a person's current style of appraising and responding to anomalous experiences (administration time 10–15 min). The full format, which is reported in this paper, provides a comprehensive assessment of an individual's history of experiencing different types of anomalies, and the changes in their interpretation and response style from first onset to the present (administration time varies widely depending on the length of the individual history and range of experiences assessed).
Procedure
Participants were administered the AANEX as part of a wider battery of tests. Interviews were carried out in person, and were tape-recorded with the consent of the participants. Initial ratings made at the time of the interview were checked on the basis of the taped interviews.
A subset of participants (n=9) were administered the AANEX over two sessions (no more than a week apart) when the interview was too long or tiring to be completed in a single sitting. The administration time varied from 45 to 300 min (mean 130 minutes), depending upon the individual's style of response, and the number of different anomalies and time points to which the interview questions were anchored. The number of response sets ranged from 1 to 18, with a mean of 3.7 per person. All participants were paid an honorarium for their time.
Statistical analyses
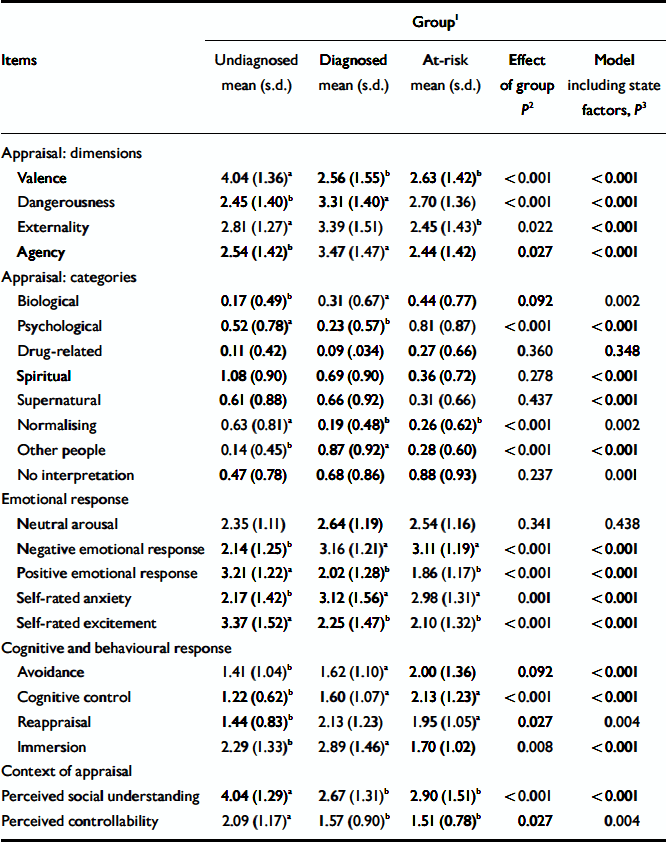
Since all of the variables being tested were ordinal (either rated between 0 and 2 or 1 and 5), the group comparisons were made using multinomial logistic regression analyses (Reference Tabachnick and FidellTabachnick & Fidell, 2001). The responses of the three groups were pooled and group was entered as two dummy variables, with the undiagnosed group as the reference category. P values of predictor variables were based on the Wald statistic. Since analysis of the AANEX data needed to account for the fact that repeated observations within participants (i.e. appraisals of different kinds of anomalies or at different time points) were not independent, robust standard errors were used to account for the correlation between repeated observations from the same participant. The group scores for the interview variables in Table 3 have been summarised using means and standard deviations, treating the scales as interval data for this purpose only. Statistical analyses were conducted using STATA version 8.1.
Table 3 Summary of item scores for the three groups of participants
| Group1 | |||||
|---|---|---|---|---|---|
| Items | Undiagnosed mean (s.d.) | Diagnosed mean (s.d.) | At-risk mean (s.d.) | Effect of group P 2 | Model including state factors, P 3 |
| Appraisal: dimensions | |||||
| Valence | 4.04 (1.36)a | 2.56 (1.55)b | 2.63 (1.42)b | < 0.001 | < 0.001 |
| Dangerousness | 2.45 (1.40)b | 3.31 (1.40)a | 2.70 (1.36) | < 0.001 | < 0.001 |
| Externality | 2.81 (1.27)a | 3.39 (1.51) | 2.45 (1.43)b | 0.022 | < 0.001 |
| Agency | 2.54 (1.42)b | 3.47 (1.47)a | 2.44 (1.42) | 0.027 | < 0.001 |
| Appraisal: categories | |||||
| Biological | 0.17 (0.49)b | 0.31 (0.67)a | 0.44 (0.77) | 0.092 | 0.002 |
| Psychological | 0.52 (0.78)a | 0.23 (0.57)b | 0.81 (0.87) | < 0.001 | < 0.001 |
| Drug-related | 0.11 (0.42) | 0.09 (.034) | 0.27 (0.66) | 0.360 | 0.348 |
| Spiritual | 1.08 (0.90) | 0.69 (0.90) | 0.36 (0.72) | 0.278 | < 0.001 |
| Supernatural | 0.61 (0.88) | 0.66 (0.92) | 0.31 (0.66) | 0.437 | < 0.001 |
| Normalising | 0.63 (0.81)a | 0.19 (0.48)b | 0.26 (0.62)b | < 0.001 | 0.002 |
| Other people | 0.14 (0.45)b | 0.87 (0.92)a | 0.28 (0.60) | < 0.001 | < 0.001 |
| No interpretation | 0.47 (0.78) | 0.68 (0.86) | 0.88 (0.93) | 0.237 | 0.001 |
| Emotional response | |||||
| Neutral arousal | 2.35 (1.11) | 2.64 (1.19) | 2.54 (1.16) | 0.341 | 0.438 |
| Negative emotional response | 2.14 (1.25)b | 3.16 (1.21)a | 3.11 (1.19)a | < 0.001 | < 0.001 |
| Positive emotional response | 3.21 (1.22)a | 2.02 (1.28)b | 1.86 (1.17)b | < 0.001 | < 0.001 |
| Self-rated anxiety | 2.17 (1.42)b | 3.12 (1.56)a | 2.98 (1.31)a | 0.001 | < 0.001 |
| Self-rated excitement | 3.37 (1.52)a | 2.25 (1.47)b | 2.10 (1.32)b | < 0.001 | < 0.001 |
| Cognitive and behavioural response | |||||
| Avoidance | 1.41 (1.04)b | 1.62 (1.10)a | 2.00 (1.36) | 0.092 | < 0.001 |
| Cognitive control | 1.22 (0.62)b | 1.60 (1.07)a | 2.13 (1.23)a | < 0.001 | < 0.001 |
| Reappraisal | 1.44 (0.83)b | 2.13 (1.23) | 1.95 (1.05)a | 0.027 | 0.004 |
| Immersion | 2.29 (1.33)b | 2.89 (1.46)a | 1.70 (1.02) | 0.008 | < 0.001 |
| Context of appraisal | |||||
| Perceived social understanding | 4.04 (1.29)a | 2.67 (1.31)b | 2.90 (1.51)b | < 0.001 | < 0.001 |
| Perceived controllability | 2.09 (1.17)a | 1.57 (0.90)b | 1.51 (0.78)b | 0.027 | 0.004 |
RESULTS
Interrater reliability
Interrater reliability was assessed by comparing ratings from C.M.C.B. with those from two independent raters (L.C.J. and E.P.P.) who are chartered clinical psychologists with clinical and research experience of assessing psychotic phenomena. Each rated four interviews. Combined, the eight interviews yielded eight sets of inventory ratings and 36 response sets on the AANEX–CAR, since each interview comprised several sets of responses anchored to different time points in the respondent's life or different kinds of experiences.
The raters scored the interviews from tapes on the basis of the written scoring manuals following a brief training session. This involved both raters initially being given the same transcribed interview to score. Their scores were checked and any areas of concern were discussed and clarified. The raters were masked to the diagnostic status of the participants.
The degree of agreement between C.M.C.B. and those of the independent raters (treated as one data-set) was analysed pairwise using weighted kappa. The weight matrices used for the comparison of ratings were determined for each variable, taking into account the rating scale, whether it was ordinal and the relative intervals between each anchor on the scale.
AANEX–inventory
The average kappa for all 40 items was 0.67, which can be interpreted as substantial agreement; 92.5% of the items had at least fair agreement (>0.4), 42.5% had substantial agreement (>0.6) and 17.5% had almost perfect agreement (>0.8).
Of the 40 items, receptivity, reference experiences and thought pressure achieved weighted kappa <0.4. The raw percentage agreements for these three items were 62%, 79% and 54% respectively. The reference experiences items ranged between 3 and 5 in the data-set compared; combined with the substantial raw agreement, this suggests that the low kappa value might have reflected the incomplete range of scores being represented. However, the receptivity and thought pressure scores in the data-set ranged between 1 and 5 and 1 and 4 respectively, suggesting that the kappa value was not overly conservative.
Subsequently, the scoring guidelines were altered to facilitate the rating of these items. Further assessment is necessary to establish the interrater reliability of the revised version. The data reported here were collected by C.M.C.B. only.
AANEX–CAR
The level of agreement for the variables assessing the categories of appraisal, dimensions of appraisal (valence, dangerousness, externality and agency), emotional response, context and implications did not fall below 0.4; 65% had at least substantial agreement and 35% almost perfect agreement.
The subsection assessing cognitive and behavioural response to anomalies contained three items that did not achieve satisfactory interrater reliability: reappraisal, rumination and neutral response. Of these, the reappraisal item showed raw agreement of over 80%, whereas the latter two items showed raw agreement of 66% and 58% respectively, suggesting that amendments are required to either the scoring guidelines or the categorisation of responses to this section. The scoring guidelines have subsequently been amended and further work is needed to establish the current reliability of these rating categories. The other three categories in this section (avoidance, cognitive control and immersion) demonstrated fair to substantial agreement. Data from the rumination and neutral response categories have not been included in the analyses currently reported. Future data generated by the probe item may be analysed to identify alternative schemes of categorisation.
Validity
Content validity was addressed by developing items on the basis of both the psychological literature and a range of existing clinical measures, as well as in-depth interviews with a range of individuals having anomalous experiences. It was not feasible to assess concurrent validity since no single existing instrument measures the same variables. The cross-sectional study reported here assesses the construct validity of the AANEX by exploring whether the interview can distinguish those with and without a need for care in the context of psychotic-like experiences. Specifically, based on the model of Garety et al (Reference Garety, Kuipers and Fowler2001), good construct validity would be demonstrated by:
-
(a) emotional response (the diagnosed and at-risk mental state groups reporting greater emotional distress and arousal in relation to anomalies than the undiagnosed group;
-
(b) dimensions of appraisals (the diagnosed and at-risk mental state groups appraising anomalies as more negative, dangerous and with more external and personal causes than the undiagnosed group;
-
(c) categories of appraisal (the diagnosed group making more externalising appraisals and less internalising appraisals than the undiagnosed group);
-
(d) perceived controllability and social support/understanding (the undiagnosed group reporting higher perceived controllability and higher perceived social support pertaining to their experiences than the diagnosed or at-risk mental state groups);
-
(e) cognitive and behavioural responses (although no specific cognitive and behavioural responses to anomalies are predicted by the model of Garety et al (Reference Garety, Kuipers and Fowler2001), it might be expected that different patterns of response would be reported by the undiagnosed group compared with the other groups.
Therefore, cross-sectional analyses relevant to these predictions are reported, based on a subset of the full data generated by the AANEX.
Group comparisons
Table 3 summarises the item scores for the three groups and the results of the regression analyses. The ‘state’ component scores were entered as covariates in all the analyses. The following sections report the analyses carried out to test construct validity via the predictions of the model of Garety et al (Reference Garety, Kuipers and Fowler2001).
Emotional response
There was a significant main effect of group on negative emotional response, which was accounted for by significantly higher odds of distress in the diagnosed and at-risk mental state groups than the undiagnosed group (diagnosed OR=4.01, 95% CI 2.18–7.37; at-risk mental state, OR=2.94, 95% CI 1.62–5.33). There was also a significant main effect of group on positive emotional response, reflecting significantly higher scores in the undiagnosed group than both the diagnosed group (OR=0.21, 95% CI 0.12–0.40) and the group with at-risk mental state (OR= 0.28, 95% CI 0.12–0.64). However, there was no significant effect of group on neutral arousal (P=0.341).
These findings were corroborated by the participants' self-ratings for anxiety and excitement in response to their anomalies. There was a significant main effect of group on anxiety, reflecting increased odds of higher anxiety in both clinical groups relative to the undiagnosed group (diagnosed: OR=3.11, 95% CI 1.65–5.86, P<0.001; at-risk mental state OR=2.22, 95% CI=1.20–4.10, P=0.011). Conversely, there was a significant main effect of group on excitement, reflecting lower odds of higher excitement in the clinical groups relative to the undiagnosed group (diagnosed, OR=0.28, 95% CI 0.15–0.52, P<0.001; at-risk mental state OR=0.40, 95% CI 0.19–0.84, P=0.016).
In summary, the first prediction was partially borne out in that the diagnosed and at-risk mental state groups reported greater distress and less positive affect in relation to anomalies, but not greater arousal than the undiagnosed group.
Dimensions of appraisal
There was a significant effect of group on the appraised valence of anomalies, with the undiagnosed group reporting more positive appraisals than the diagnosed (OR=0.19, 95% CI 0.11–0.32) or at-risk mental state groups (OR=0.37, 95% CI 0.20–0.66). There was also a significant group effect on appraised dangerousness of anomalies, with the diagnosed group appraising their experiences as more dangerous to them than the undiagnosed group (OR=2.85, 95% CI 1.60–5.06, P=0.01). The diagnosed group was also more likely than the undiagnosed group to appraise their experiences as being caused by some agency rather than an impersonal cause (OR=2.36, 95% CI 1.22–4.55, P=0.01).
The diagnosed group was associated with increased odds of making an external appraisal relative to the undiagnosed group (OR=2.08, 95% CI 1.16–3.74, P=0.01). However, when the state component scores were incorporated into the regression model there was no longer any significant predictive value for the diagnosed group and the group with at-risk mental state had reduced odds of an external appraisal, although this was only marginally significant (OR=0.56, 95% CI 0.31–1.00, P=0.05).
In summary, the prediction was predominantly fulfilled since the clinical groups appraised anomalies as more negative, dangerous and personally caused than the undiagnosed group. However, the clinical groups did not appraise anomalies as being more externally caused when the types of anomalies were controlled for.
Categories of appraisal
Group contributed significantly to the prediction of four of the categories of appraisal. The diagnosed group was significantly more likely to make a ‘biological’ appraisal (OR=2.39, 95% CI 1.05–5.45, P=0.039), and an ‘other people’ appraisal (OR= 9.01, 95% CI 4.02–20.22, P<0.001) than the undiagnosed group.
The diagnosed group was significantly less likely than the undiagnosed group to make a ‘psychological’ appraisal (OR= 0.34, 95% CI 0.15–0.76, P=0.008). Both the clinical groups were less likely to make a ‘normalising’ appraisal than the undiagnosed group (diagnosed, OR=0.16, 95% CI 0.07–0.40, P<0.001; at-risk mental state, OR=0.27, 95% CI 0.11–0.64, P=0.003).
There was no group effect on the likelihood of making a ‘drug-related’ (P=0.35), ‘no interpretation’ (P=0.23), ‘supernatural’ (P=0.19) or ‘spiritual’ appraisal (P=0.28). For the latter category, there was a significant effect of group (reflecting increased odds of ‘spiritual’ appraisal in the undiagnosed group compared with both clinical groups) before the state component scores were entered into the model, indicating that group differences were secondary to the association between particular types of anomaly and this type of appraisal.
In summary, the prediction was partially fulfilled, since the diagnosed group made more ‘other people’, and less ‘psychological’ appraisals than the undiagnosed group. However, the diagnosed group was more likely to make ‘biological’ appraisals and there was no difference in the likelihood of making ‘supernatural’ or ‘drug-related’ appraisals between the two groups.
Perceived controllability and social support/understanding
The undiagnosed group was more likely to report higher perceived control over their anomalies than the diagnosed (OR=0.42, 95% CI 0.21–0.84, P=0.014) and at-risk mental state (OR=0.43, 95% CI 0.20–0.90, P=0.025) groups, in accordance with the prediction.
The undiagnosed group was more likely to report higher perceived social understanding relative to their experiences than either clinical group (diagnosed, OR=0.15, 95% CI 0.08–0.29, P<0.001; at-risk mental state, OR=0.28, 95% CI 0.13–0.62, P=0.002), in accordance with the prediction.
Cognitive and behavioural responses
The diagnosed group was more likely to report responses categorised as avoidance (OR=2.31, 95% CI 1.08–4.98, P=0.03), cognitive control (OR=3.04, 95% CI 1.33–6.92, P=0.008) and immersion (OR=1.94, 95% CI 1.12–3.36, P=0.019), relative to the ‘undiagnosed’ group. The at-risk mental state group was also more likely to report cognitive control (OR=7.18, 95% CI 3.08–16.73, P<0.001) and reappraisal responses (OR=3.10, 95% CI 1.32–7.30, P=0.010) relative to the undiagnosed group. Therefore, in accordance with the prediction, different patterns of response were reported by the undiagnosed group compared with the clinical groups.
DISCUSSION
The AANEX was validated through the successful differentiation of groups of individuals with and without a need for care on the basis of a number of variables. The findings also elucidated some of the factors associated with the development of clinically relevant psychotic symptoms from anomalous experiences associated with psychosis. These data may therefore have implications for early intervention strategies aiming both at identifying individuals genuinely at risk of developing clinical need and averting this risk. The AANEX is not intended to be used to predict transition to psychosis. However, the data it yields are certainly informative with regard to the range of forms of psychotic experience and those forms which have greater or lesser likelihood of association with a need for care. Further studies could assess the specificity and sensitivity of the instrument in predicting need for care while bearing in mind that other contextual factors may also have an impact on this.
The results predominantly met the predictions suggested to indicate good construct validity. Out of the 20 variables to which the five predictions pertained, the clinical and non-clinical groups were differentiated in the predicted direction on 15 variables.
The undiagnosed group of participants was characterised by significantly different styles of appraisal, response and context to those in the clinical groups, as predicted by cognitive models of psychosis (Reference Garety, Kuipers and FowlerGarety et al, 2001). Overall the undiagnosed participants reported appraising their experiences as relatively more positive and benign, with a more positive and less negative emotional response. Interestingly, on average this group did not report any less arousal in relation to their experiences than the clinical groups, suggesting that the reduced distress did not reflect a lack of emotional engagement with the anomalies. Another finding that may be related to the reduced distress in this group was the higher level of perceived controllability of the anomalies. However, even in this group, the mean rating for controllability was only just above ‘minimal’.
The undiagnosed participants were also less likely to report avoidant responses or to employ cognitive control strategies than both the clinical groups. Although they were less likely than the diagnosed group to act on the basis of their experiences (the ‘immersion’ category), they were also less likely to reappraise their experiences than at-risk mental state participants, suggesting that they had found a way of appraising their experiences that was (subjectively) coherent and adaptive.
The undiagnosed participants were also much less likely than the diagnosed group to form a ‘paranoid’ appraisal, such as thinking that other people or agencies were causing the experiences, and were more likely to think that the experiences were caused by something psychological. However, the results did not suggest that an externalising appraisal per se marked the defining decision leading to clinically relevant psychotic symptoms: the undiagnosed participants also reported externalising appraisals such as those falling in the ‘supernatural’ category.
Moreover, the results suggest that the preponderance of externalising appraisals in the diagnosed group was secondary to differences in the sorts of anomalies predominating at the time points under discussion, compared with the undiagnosed group, suggesting that certain types of anomaly tend to elicit external appraisals. Similarly, the finding that the excess of ‘spiritual’ appraisals in the undiagnosed group was accounted for by the inclusion of the state component scores suggests that certain experiences, more common in the response sets of the undiagnosed group, tended to elicit ‘spiritual’ appraisals. As suggested by Garety et al (Reference Garety, Kuipers and Fowler2001), and demonstrated by differences in appraisal when holding the effects of type of anomaly constant, appraisals are relevant to transition from anomalous experience to clinically relevant symptom; however, the relationship appears more complex than simply turning on an externalising decision.
Overall, and taking into account variance in the kinds of experiences being described, the undiagnosed group was much more likely to consider that their experiences were part of the spectrum of normal human experience. This may reflect another characteristic of the group: the higher perceived levels of understanding of their experiences among their social group. In relation to early intervention strategies, these findings suggest that normalising approaches towards anomalies reported by those seeking help may be invaluable. Moreover, facilitating access to ‘experts by experience’, people who have had the same experiences and coped with them, could be a useful strategy for supporting the normalising approach.
Limitations
There are some limitations to the generalisability of these preliminary findings, because of the nature of the undiagnosed sample. Relative to the clinical groups, the undiagnosed participants were more likely to come from White ethnic backgrounds (although there were more non-British people), which may be relevant to their styles of response and appraisal, as well as their social context. They also differed significantly from the diagnosed group in terms of estimated IQ. Although this may not affect appraisal processes per se, it might represent an additional factor influencing the development of need for care: the undiagnosed group had higher than average IQ, which might possibly act as a protective factor through allowing more sophisticated appraisals and responses. However, it is not known whether this is characteristic of all those in the general population with at least occasional experiences of any first-rank symptom.
Furthermore, although the number and types of anomalies occurring at each time point were controlled for, the frequency or severity of any particular type was not. It is likely that variance in frequency has an impact on appraisals and response. Nevertheless, the undiagnosed group was selected on the basis of reporting comparable anomalous experiences to the clinical groups, and individuals reporting only infrequent experiences were not included.
Implications
Overall, the initial results suggest that the AANEX has the potential to elicit information that may clarify the nature of the continuum of psychotic and psychotic-like experiences, and the complex and multifactorial development of distress and need for care relative to these experiences. The interview may allow this clarification by assessing a range of components of experience considered to vary across the continuum, such as types and frequency of anomalous experience, interpretations, and emotional and contextual factors. In relation to this, it has demonstrated utility as a clinical tool for differentiating anomalous experiences from their appraisals, thereby improving understanding of the person's subjective experience and how they might benefit from psychological interventions.
The majority of the interview schedule was found to have good levels of reliability, indicating that the dimensions assessed and scoring schemes are robust, despite the complexity of the material being elicited. The small number of items that required amendment have been refined on the basis of the data gathered in this study, aiming for clearer, more unidimensional definition.
The form and process of the interview was acceptable to participants from both clinical and non-clinical populations, and sensitive to the differing ways in which psychotic-like experiences may be interpreted. These characteristics differentiate the AANEX from existing symptom rating scales that assess only pre-specified ‘clinical’ forms of anomalous experiences (e.g. the Scale for Assessment of Positive Symptoms (Reference AndreasenAndreasen, 1984) or the Positive and Negative Syndrome Scale; Reference Kay, Fiszbein and OplerKay et al, 1987), and also from other scales suitable for populations without psychosis that do not assess relevant context, appraisal and response variables (e.g. the CAARMS (Reference YungYung, 2000) or WMAPE (Reference Kwapil, Chapman and ChapmanKwapil et al, 1999)). The flexible structure of the AANEX facilitates its use for either detailed investigations of individuals' experiences or briefer assessments that may be repeated at several time points (e.g. pre- and post-intervention or during a follow-up period). The brief form of the AANEX is currently being piloted as a repeated assessment during a follow-up of clients of OASIS with at-risk mental state.
APPENDIX

| These items were included in the inventory. The 19 anomalies contributing to state component scores are in bold. | |
| Number | Anomaly |
| A1 | Thought transmission |
| A2 | Receptivity |
| A3 | Thought withdrawal |
| A4 | Controlled actions |
| A5 | Passivity (other) |
| A6 | Reference experiences |
| A7 | Activity experiences |
| A8 | Loud thoughts |
| A9 | Voices/auditory hallucinations |
| B1 | Depersonalisation |
| B2 | Derealisation |
| B3 | Visual anomalies (global) |
| B4 | Visual anomalies (hallucinations) |
| B5 | Auditory anomalies |
| B6 | Oversensitivity |
| B7 | Somatic anomalies |
| B8a | Lost automatic skills |
| B8b | Dividing attention deficit |
| B9a | Receptive language disturbance |
| B9b | Concretism |
| B10 | Olfactory anomalies |
| C1a | Distractability |
| C1b | Thought interference |
| C1c | Thought blockage |
| C1d | Captivation/fixation |
| C2 | Time distortion |
| C3 | Disorientation |
| C4 | ‘Insight’ experiences |
| C5 | Thought pressure |
| C6 | ‘Mission’ experiences |
| D1 | ‘Spiritual’ elation |
| D2 | Monitored |
| D3 | Doom |
| D4 | Mixed emotions |
| D5 | Emotional reactivity |
| D6 | Loss of emotions |
| E1 | Precognition |
| E2 | Out of body experiences |
| F1 | Loss of boundary |
| F2 | Subjective isolation |






eLetters
No eLetters have been published for this article.