Recent investigation of ‘duration of untreated psychosis’ (DUP) has demonstrated that although individuals generally receive treatment within 6 months of symptom onset, others remain untreated in the community for 1-2 years (e.g. Reference McGlashanMcGlashan, 1999; Reference Barnes, Hutton and ChapmanBarnes et al, 2000; Reference Ho, Andreasen and FlaumHo et al, 2000). Understanding the psychological and service impediments to early diagnosis is a prerequisite for attempts to reduce these potentially deleterious treatment delays (Reference Lincoln, McGorry, McGorry and JacksonLincoln & McGorry, 1999). The first stage of help-seeking — ‘the decision to seek care’ — is particularly prone to delays (Reference Jones, Bebbington and FoersterJones et al, 1993; Reference McGorry, Edwards and MihalopoulosMcGorry et al, 1996) and may be negatively influenced by intrapersonal factors such as avoidant coping style and pessimistic beliefs about health services. In this study, we seek to determine whether help-seeking behaviour in relation to general health matters is predictive of a patient's readiness to seek help from a general practitioner (GP) during the emergence of a mental health problem.
METHOD
Clients from two urban mental health services were screened for participation in the study. All participants met the diagnosis for schizophrenia and related disorders (ICD—10: F20, F22, F23, F25; World Health Organization, 1992) and were in the early stages of treatment.
Measures
Duration of untreated psychosis
The DUP was operationalised as the time interval between the onset of psychotic symptoms and onset of treatment. A semi-structured interview following the model of Beiser et al (Reference Beiser, Erickson and Fleming1993) was conducted with the participant and carer to obtain information about the onset and development of symptoms and the early stages of treatment. Additional information was extracted from the participant's psychiatric records in order to verify dates about the onset of symptoms and treatment. Definitions of DUP have differed in previous studies. In the present study, DUP was calculated according to a stringent protocol adapted from criteria developed by Larsen et al (Reference Larsen, Johannessen and Opjordsmoen1998). They report good test—retest reliability (intraclass correlation, r=0.96, P<0.01). Eighteen cases were selected at random from the sample and rated independently by two assessors, rounding to whole weeks. The average intraclass correlation was unity, which indicates an excellent degree of consistency between the raters.
Miller Behavioral Style Scale
The Miller Behavioral Style Scale (MBSS; Reference MillerMiller, 1987) has been used widely in various health settings to assess individual coping styles on the basis of self-reported preferences for information and distraction in anxiety-provoking situations. The MBSS consists of four hypothetical stress-evoking scenes of an uncontrollable nature (e.g. a possible aeroplane disaster, potential job redundancy). These scenes are intended to be similar in context to a threatening health situation/hospital visit (Miller & Magnan, 1983). Participants are asked to choose one or more items from a total of eight statements that represent their preferred way of responding to each situation presented. Four of the statements correspond to information-seeking (‘monitoring’) and four relate to information-avoiding (‘blunting’); consequently each sub-scale consists of 16 items. Two scores can be obtained for each participant: (a) a total ‘monitoring’ score; and (b) a total ‘blunting’ score.
Reliability analyses show the MBSS sub-scales to be stable over a 4-month period (monitoring: r (98)=0.72, P<0.01; blunting: r (98)=0.75; P<0.01) Miller & Mischel, 1986: cited in Reference MillerMiller, 1987).
Multi-dimensional Health Locus of Control scale
The Multi-dimensional Health Locus of Control (MHLC) scale (Reference Wallston, Wallston and De VellisWallston et al, 1978) measures the extent to which an individual believes that the locus of control for health is: (a) internal, that is, as a result of their own behaviour (IHLC); (b) under the control of ‘powerful others’, that is health professionals (PHLC); and (c) determined by external factors such as chance or fate (CHLC). This self-report questionnaire comprises six items for each scale. The instructions of the MHLC questionnaire were amended to inform participants that the words ‘ill’ and ‘illness’ referred to general health problems.
The MHLC scale is the most widely used measure of health locus of control (Reference Norman, Bennett, Conner and NormanNorman & Bennett, 1995). This questionnaire has been designed for use with adults and is applied to both clinical and nonclinical populations. Two equivalent forms with matching items were found to have acceptable alpha reliabilities for each scale ranging from 0.67 to 0.77. In the original study, the authors reported adequate construct validity and an indication of predictive validity (Reference Wallston, Wallston and De VellisWallston et al, 1978). Form A was used in this study, as the factor structure and reliability of this version has been generally confirmed as satisfactory (Reference Hartke and KunceHartke & Kunce, 1982; Reference Marshall, Collins and CrooksMarshall et al, 1990).
Past health help-seeking behaviour
To obtain an objective measure of how often the participant sought help from a GP, the frequency of contact from 16 years of age (early ‘adulthood’) to the onset of psychosis was assessed from GP medical records. As well as the date of the visit, information about the presenting symptoms/complaint, GP's diagnosis and intervention was noted.
Different types of appointments (e.g. health checks, missed appointments, follow-up appointments) were coded and divided into simple categories to reflect the nature of the consultation (see Reference Atkinson and CoffeyAtkinson & Coffey, 1996); each appointment was then classified according to this protocol. The frequency of visits to the GP for health problems (‘general GP attendance’) was derived by aggregating all appointments attended by the participant. Interrater reliability was calculated for eight randomly selected cases. The average intraclass correlation was r=0.99 (P<0.01), indicating very high reliability.
Data analysis
Data were analysed using SPSS 10.0.0 for Windows. DUP was divided into three pre-defined categories based on the time intervals described by Carbone et al (Reference Carbone, Harrigan and McGorry1999): brief DUP (1 month or less); moderate DUP (greater than 1 month but less than/equal to 6 months); long DUP (greater than 6 months). The analysis of variance (ANOVA) was the main analytical technique.
RESULTS
Sample
Forty-eight participants were contacted, six (12.5%) refused. Demographic and clinical characteristics of the participants are shown in Table 1.
Table 1 Demographic and clinical characteristics of the participants (n=42)
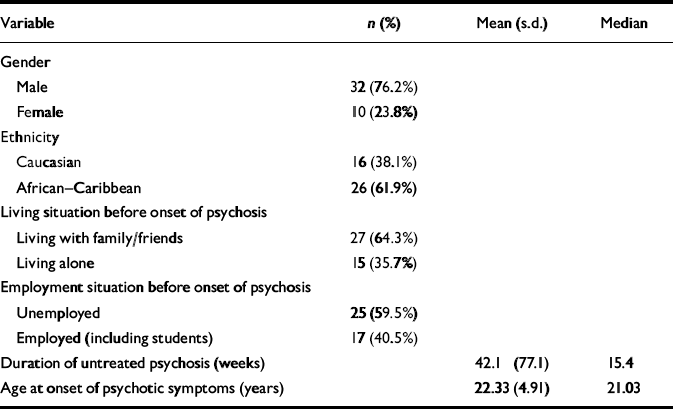
| Variable | n (%) | Mean (s.d.) | Median |
|---|---|---|---|
| Gender | |||
| Male | 32 (76.2%) | ||
| Female | 10 (23.8%) | ||
| Ethnicity | |||
| Caucasian | 16 (38.1%) | ||
| African—Caribbean | 26 (61.9%) | ||
| Living situation before onset of psychosis | |||
| Living with family/friends | 27 (64.3%) | ||
| Living alone | 15 (35.7%) | ||
| Employment situation before onset of psychosis | |||
| Unemployed | 25 (59.5%) | ||
| Employed (including students) | 17 (40.5%) | ||
| Duration of untreated psychosis (weeks) | 42.1 (77.1) | 15.4 | |
| Age at onset of psychotic symptoms (years) | 22.33 (4.91) | 21.03 |
Duration of untreated psychosis
The DUP had a median of 15.4 weeks. The distribution of this sample was positively skewed, because of a number of outliers with extremely long DUPs (one-sample Kolmogorov—Smirnov (K—S) Z=1.901, P<0.01). The median represents a more meaningful measure of central tendency in this case. A total of 12 (28.6%) had brief DUP (≤1 month); 17 (40.5%) had moderate DUP and 13 (30.9%) long DUP.
GP attendance
Four participants were excluded from this part of the analysis: two had experienced an onset of psychosis before the age of 16 years, one had incomplete GP medical records and another withdrew consent for this section of the study. Participants' consultations with a GP were recorded for a specific period (from age 16 to onset of psychosis). The mean for this period was 6.6 (s.d.=4.5) years and the distribution was normal (one-sample K—S Z=1.19, P=0.11, NS). There was a significant difference between the DUP groups regarding their mean frequency of general GP attendance (see Table 2; F 2,35=5.57, P<0.01).
Table 2 Duration of untreated psychosis (DUP) category and general practitioner (GP) attendance

| Brief DUP ≤ 1 month n=12 | Moderate DUP > 1 month, ≤ 6 months n=16 | Long DUP > 6 months n=10 | Total n=38 | |
|---|---|---|---|---|
| GPs attendances per year (mean, s.d.) | 4.25 (2.10) | 2.66 (2.59) | 1.55 (1.78) | 2.69 (2.36) |
Post hoc analysis using Fisher's least significant difference (LSD) test showed that the brief DUP group had higher GP attendance than the long DUP group (mean difference 2.70, p<0.01). No differences were found between mean attendance for the moderate and long DUP groups. Thus, the results indicate that participants who consulted their GP more frequently in the 6 years before the onset of psychosis were more likely to have a shorter DUP.
Miller Behavioral Style Scale
As distributions of ‘monitoring’ and ‘blunting’ sub-scale scores were found to be normal, one-way ANOVA was computed to test the hypothesis of a difference between DUP groups with regard to coping style. For the ‘blunting’ sub-scale there was a significant effect of DUP (F 2,37=3.77, P<0.05) (see Table 3). Post hoc analysis applying Fisher's LSD indicated that the difference was between the brief and moderate DUP groups (mean difference was 2.96, P<0.05) and the brief and long DUP groups (mean difference was 2.75, P<0.05). For the monitoring sub-scale no significant differences were found (F 2,37=0.2, NS). A one-tail correlation between DUP (transformed to the natural logarithm in order to achieve normality) and monitoring was also non-significant (Pearson's r=0.12, P=0.22, NS).
Table 3 Duration of untreated psychosis (DUP) category and coping style on the Miller Behavioral Style Scale (MBSS)

| MBSS sub-scale | Brief DUP ≤ 1 month n=12 | Moderate DUP > 1 month, ≤ 6 months n=16 | Long DUP > 6 months n=12 | Total n=40 |
|---|---|---|---|---|
| ‘Monitoring’ (mean, s.d.) | 10.42 (3.60) | 11.00 (4.03) | 11.17 (4.35) | 10.88 (3.92) |
| ‘Blunting’ (mean, s.d.) | 3.17 (2.33) | 6.13 (3.70) | 5.92 (2.61) | 5.18 (3.24) |
A one-tailed correlation between DUP and ‘blunting’ was positive, but failed to reach significance at the 5% level (Pearson's r=0.22, P=0.01, NS). In other words, only patients with a brief DUP (compared with patients in the moderate and long DUP groups) were significantly less likely to display a blunting coping style.
Multi-dimensional Health Locus of Control scale
Two participants were excluded from this section because of missing data. Scores on the MHLC indicate how strongly the individual believes in each dimension of control; the higher the score the stronger the belief. Analysis using a one-sample K-S Z test indicated that all sub-scales were distributed normally. No differences were found between the DUP groups on any of the MHLC sub-scales: internal HLC, F 2,37=1.0, NS; chance HLC, F 2,37=0.7, NS; and ‘powerful others’ HLC, F 2,37=1.5, NS. Comparing the mean scores of the present sample for each sub-scale with normative data from other samples (Table 4), it can be seen that the early psychosis sample had a lower internal HLC mean score and higher chance and ‘powerful others’ HLC mean scores compared with other samples.
Table 4 Mean scores on the Multi-dimensional Health Locus of Control (MHLC) scale for early psychosis sample with comparative samples1

| Sample | n | Internal HLC (s.d.) | Chance HLC (s.d.) | ‘Powerful other’ HLC (s.d.) |
|---|---|---|---|---|
| First-episode psychosis | 40 | 24.58 (5.13) | 20.78 (5.60) | 24.75 (5.68) |
| Chronic patients2 | 609 | 25.78 | 17.64 | 22.54 |
| College students2 | 749 | 26.68 | 16.72 | 17.87 |
| Healthy adults2 | 1287 | 25.55 | 16.21 | 19.16 |
| Persons engaged in preventive health behaviours2 | 720 | 27.38 | 15.52 | 18.44 |
One-tail correlations between DUP (transformed to the natural logarithm in order to achieve normality) and each MHLC sub-scale were found to be non-significant (IHLC Pearson's r=0.16, P=0.16, NS; CHLC Pearson's r=-0.16, P=0.16, NS; PHLC Pearson's r=0.11, P=0.24, NS).
GP attendance and health coping style
Further analysis revealed a significant negative correlation between general GP attendance and scores on the MBSS ‘blunting’ sub-scale (Pearson's r=-0.40, P=0.02, n=37), suggesting that participants who visit their GP less frequently are more likely to endorse a ‘blunting’ style on the MBSS. This relationship confirms previous observations of the validity of Miller's ‘blunting/monitoring’ concept and supports the validity of the link between DUP and ‘blunting’.
DISCUSSION
Health behaviour and ‘blunting’ coping style
These findings support our hypotheses that those with a long DUP are more likely to use avoidance as a general coping strategy when faced with health threat and are less likely to have visited their GP on a regular basis over a long period of time (6 years). This is consistent with studies indicating that employment of a ‘blunting’ coping style is associated with protracted delay in treatment-seeking and more severe symptoms (both psychological and physical) upon presentation to services (Reference Steptoe and VogeleSteptoe & Vogele, 1992; Reference Davey, Tallis and HodgsonDavey et al, 1993); similarly, first-episode studies have found that a longer DUP is related to more severe symptoms on first admission to psychiatric services (Reference Larsen, McGlashan and MoeLarsen et al, 1996; Reference Verdoux, Bergey and AssensVerdoux et al, 1998; Reference Browne, Clarke and GervinBrowne et al, 2000; Reference Drake, Haley and AkhtarDrake et al, 2000).
It has been found that ‘blunters’ experience less anxiety when faced with an unavoidable stressor and cope better in situations where they can avoid threatening information (Reference Miller and ManganMiller & Mangan, 1983; Reference MillerMiller, 1987). Thus, perhaps, a ‘blunting’ coping style might reduce distress caused by psychotic symptoms, enabling the individual to cope adequately for longer periods compared with ‘low blunters’. Lending partial support to this theory, Drake et al (Reference Drake, Haley and Akhtar2000) found that long DUP was linked to poor insight and preserved coping skills; similarly Birchwood et al (Reference Birchwood, Iqbal and Chadwick2000a ) found that high insight was linked to a raised likelihood of post-psychotic depression. It is difficult to establish, however, whether those with short DUP contact their GP more because they are ‘monitors’ or simply because they have more physical illness; nevertheless the outcome is the same, i.e. greater GP contact. We argue that this greater contact, for whatever reason, increases the propensity of clients to seek help through primary care when they experience distress. In a future communication, we will present data on the timing of GP contact and the nature of the presenting symptoms.
The aggregate figure for GP contacts is a blunt instrument and may include contacts for ‘prodromal’ as well as ‘true’ (physical) illness symptoms. Following this argument through, it would be expected that a greater number of contacts would be a sign of a long or intense prodrome. However, long prodrome is associated with a long DUP (Reference Beiser, Erickson and FlemingBeiser et al, 1993): the very opposite of that observed here (i.e. more contacts linked with short DUP). We conclude, therefore, that the link we have observed reflects the impact of help-seeking behaviour for health concerns per se and is not an artefact of prodromal psychosis.
‘Monitoring’ coping style
Research has indicated that individuals with a ‘monitoring’ coping style are more likely to detect physical symptoms, demand more tests and information and seek help for relatively trivial problems, leading to early detection and treatment (Reference MillerMiller, 1987; Reference Miller, Brody and SummertonMiller et al, 1988; Reference Steptoe and VogeleSteptoe & Vogele, 1992). However, although the ‘blunting’ scale was found to be significant, the monitoring sub-scale showed no relationship to DUP. An explanation for this finding may be the way ‘high monitors’ perceive psychotic symptoms. ‘High monitors’ have been reported to overestimate the potential severity, likelihood and unpredictability of threatening events (Reference Davey, Tallis and HodgsonDavey et al, 1993; Reference Miller, Rodoletz and SchroederMiller et al, 1996). Furthermore, they experience higher levels of worry and distress in medically threatening situations, which may interfere with effective problem-solving behaviour and result in denial and disengagement (Reference Miller, Sarason, Sarason and PierceMiller, 1996; Reference Miller, Rodoletz and SchroederMiller et al, 1996). Thus, predicting behaviour based on the ‘monitoring’ coping style is a complex issue and is related to how the threat is perceived.
Duration of untreated psychosis
The low refusal rate to participate in our study mitigates the likelihood of sample bias. DUP is similar to other studies (e.g. Reference Carbone, Harrigan and McGorryCarbone et al, 1999; Reference Barnes, Hutton and ChapmanBarnes et al, 2000; Reference Drake, Haley and AkhtarDrake et al, 2000) and is comparable with other similar studies. By its very nature, DUP is difficult to calculate as it relies on a respondent's memory, and can only ever be a ‘best estimate’. Previous studies have differed widely in their operational definitions and procedures and thus their accuracy of this time interval is variable (Reference Norman and MallaNorman & Malla, 2001). In the present study, a stringent protocol was adhered to, including use of multiple sources in order to increase the accuracy of DUP and inter-rater reliability was found to be excellent.
The role of GPs
General practitioners have been identified as an important contact in the pathway to care of a young person with first-episode psychosis. GP involvement has been associated with more desirable pathways, including decreased likelihood of police involvement and compulsory admissions (Reference Cole, Leavey and KingCole et al, 1995; Reference Lincoln, Harrigan and McGorryLincoln et al, 1998; Reference Burnett, Mallett and BhugraBurnett et al, 1999). These findings support the finding of many previous studies (Reference Cole, Leavey and KingCole et al, 1995; Reference Burnett, Mallett and BhugraBurnett et al, 1999) that contact with primary care is a key factor in reducing DUP, distress and access to sustained treatment. These data reinforce previous suggestions that ‘normal’ psychological factors are at play in this process (i.e. help-seeking behaviour for health concerns), in addition to those such as shame, which may be specific to a major mental illness (Reference Birchwood, Spencer and McGovernBirchwood et al, 2000b ). We are about to embark on a large-scale replication of these findings and to explore help-seeking behaviour in other family members.
CLINICAL IMPLICATIONS
-
▪ Increasing the ability of general practitioners (GPs) to recognise early signs during the prodromal and psychotic stage of the disorder may contribute to a reduction in untreated psychosis.
-
▪ Intrapersonal variables such as denial and avoidance appear to be common responses to the onset of psychotic symptoms.
-
▪ Increase in public awareness (particularly for people in regular contact with young adults) of psychosis and the benefits of prompt treatment may help ‘avoidant’ young people experiencing a first-episode of psychosis to receive treatment with less delay.
LIMITATIONS
-
▪ The relatively small sample size limited the statistical power of the tests performed.
-
▪ Although measures were chosen to be suitable for use retrospectively, with the exception of GP data, they may be affected by retrospective bias.
-
▪ Although the role of a ‘significant other’ has been shown to be influential in pathways to care, the contributions of participants' relatives or friends could not be examined within this study.







eLetters
No eLetters have been published for this article.