Post-traumatic stress disorder (PTSD), codified in DSM—III in 1980 (American Psychiatric Association, 1980), has become the subject of a debate about its nature and origins. Although it has only recently been defined, many have argued that PTSD has always existed and went unrecognised by contemporaries (Reference Gersons and CarlierGersons & Carlier, 1992). Shay (Reference Shay1991) suggested that elements of the disorder could be identified in Homer's Iliad. Samuel Pepys, who lived through the plague and Great Fire of London, is said to have recorded the features of PTSD in his diary (Reference DalyDaly, 1983), while the symptoms reported in a family trapped in the Bergemoletto avalanche have been frequently quoted as evidence for the disorder's existence in the mid-18th century (Reference Parry-Jones and Parry-JonesParry-Jones & Parry-Jones, 1994). Dean argued that the symptoms of PTSD, including flashbacks, can be identified in the accounts of veterans of the American Civil War (Reference DeanDean, 1997). Trimble concluded that ‘this relatively common human problem has been known for many hundreds of years, although under different names’ (Reference Trimble and FigleyTrimble, 1985: p. 5).
In contrast, Young argued that PTSD is a culture-derived diagnosis and can only have existed in the late 20th century:
“The disorder is not timeless.... Rather, it is glued together by the practices, technologies, and narratives with which it is diagnosed, studied, treated and represented and by the various interests, institutions, and moral arguments that mobilised these efforts and resources” (Reference YoungYoung, 1995: p. 5).
Mumford's analysis of the Iliad showed that the heart alone (and not the head or the abdominal organs) was associated with emotional distress (Reference MumfordMumford, 1996). In the Hebrew Bible too, he found that the heart was interpreted as the seat of the emotions, will and intellect (Reference MumfordMumford, 1992); this is a significantly different somatic vocabulary from that of today and the one reflected by PTSD. Bracken argued that because PTSD should be seen as ‘the product not of trauma in itself but of trauma and culture acting together’ it cannot be a timeless phenomenon, and that earlier responses to extreme stress, such as shellshock, are not the same (Reference BrackenBracken, 2001: p. 742).
Using historical medical files of soldiers who served in the Boer War and in the First and Second World Wars, we have attempted to test the hypothesis that the symptom clustering associated with PTSD existed before psychiatrists recognised it as a formal disorder.
METHOD
Subjects
War pension files were used as the primary source because they contained detailed medical and military reports. Throughout the period under investigation soldiers were assessed for a pension by a board of at least two doctors and then re-examined annually until their condition had stabilised or remitted. Military physicians gave way to civilians during the First World War, when the volume of claims rose exponentially. Although the assessment procedure did not change greatly, the criteria were revised. Initially, awards were based on a veteran's ability to earn a living wage rather than the nature of his disability. From December 1916 they were granted according to a standardised schedule of injury in which (for example) the loss of two or more limbs entitled a man to a 100% award. Since no standardised checklist of symptoms was provided, doctors were instructed to categorise shellshock as a severe injury if the patient was thought likely to recover, and as a very severe injury if the condition was chronic.
Because we sought to test the incidence of flashbacks in populations at risk and because there was no equivalent diagnostic label for earlier wars, we identified post-combat disorders that typified particular conflicts, such as shellshock for the First World War and ‘disordered action of the heart’ for the Boer War. Indeed, some have argued that these presentations are simply PTSD by another name (Reference Joseph, Williams and YuleJoseph et al, 1997). Individual files contained medical notes that covered the serviceman's history from enlistment until his demise or the termination of the award. Pensioners were required to attend regular medical boards to assess their disability and specialist opinions were sought. As a result, symptoms were often recorded on an annual basis for 5-10 years after discharge from the armed forces. The long-term nature of the notes allowed cases to be excluded if a serviceman was found to be suffering from an organic disorder or a major mental illness. The investigation was restricted to members of the British Army. A total of 1856 cases were included (Table 1), drawn from seven conflicts and representing ten diagnoses (Reference Jones, Hodgins Vermaas and McCartneyJones et al, 2002).
Table 1 The database: total number of cases classified according to conflict and diagnosis

| Conflict and diagnosis | Number of service personnel |
|---|---|
| Victorian campaigns (1854-1895) | |
| Palpitation | 19 |
| Debility | 9 |
| Boer War (1899-1902) | |
| Disordered action of the heart | 200 |
| Rheumatism | 200 |
| First World War (1914-1918) | |
| Servicemen | |
| Disordered action of the heart | 200 |
| Neurasthenia | 200 |
| Gassed | 167 |
| Nurses | |
| Disordered action of the heart | 24 |
| Neurasthenia | 49 |
| Second World War (1939-1945) | |
| Effort syndrome | 67 |
| Psychoneurosis | 200 |
| Dyspepsia | 100 |
| Malaya (1948-1960) and Korea (1951-1953) | |
| Effort syndrome | 1 |
| Psychoneurosis | 15 |
| Dyspepsia | 5 |
| Persian Gulf War (1991) | |
| Gulf-related illness | 400 |
| Total | 1856 |
Boer War
Two hundred cases of disordered action of the heart and 200 cases of rheumatism (without objective signs) were randomly selected from the pension files of the Royal Hospital, Chelsea, London. Consecutive files were extracted in proportion to their alphabetical distribution by surname. Both of these post-combat disorders were a major cause of invalidity from the forces. Contemporaries believed that disordered action of the heart was caused by lengthy marching in equipment, which constricted blood flow to and from the heart, whereas rheumatism was considered to be the product of fever and exposure to wet conditions.
First World War
Two hundred cases of disordered action of the heart and 200 cases of shellshock (reclassified as neurasthenia in 1917), together with 167 servicemen who had been gassed without permanent organic injury, were selected using a random number generator from all surviving First World War pension files. These case notes, held at the Public Record Office (PRO), were a representative 2% sample based on London and south-east England. Every pension for disordered action of the heart or neurasthenia awarded to a nurse was also included.
Second World War
Three diagnostic groups were chosen: effort syndrome (for comparison with the Boer War and First World War samples of disordered action of the heart), psychoneurosis (for comparison with neurasthenia) and non-ulcer dyspepsia. War pension files for this conflict were stored at two sites according to a number of criteria. We surveyed the entire holding to discover its characteristics and then randomly extracted 200 cases of psychoneurosis to obtain a representative sample. Effort syndrome, in contrast, had become a discredited term and all cases found were included. The focus of health concerns in the UK switched from the heart in the First World War to the stomach in the Second World War. To reflect this important change in medical priorities, 100 cases of non-ulcer dyspepsia were included.
Malaya and Korea
Considerable problems were encountered in finding awards for psychoneurosis, effort syndrome and dyspepsia from Korea and Malaya, in part because troops deployed there represented a small proportion of the UK's armed forces. All cases were included.
Persian Gulf War
Although pensions have been granted to veterans of the Persian Gulf War, we were not given permission to consult these files. Nevertheless, it was important to study a group whose health might have been damaged by active service. The Ministry of Defence granted access to anonymous case records from the Gulf Veterans' Medical Assessment Programme (MAP). From their database of 2162 army personnel, a sample of 400 Gulf War veterans was selected using a random number generator. A definite diagnosis of PTSD had been made for 369 (12.3%) of the first 3000 cases who attended the MAP, although this figure understates the true incidence as many early presentations had not been referred for a psychiatric opinion (Reference Lee, Gabriel and BoltonLee et al, 2002).
Symptomatology
A standardised form was employed to collect 94 possible symptoms, which included 11 of the main signs of PTSD (see Table 4). In addition, the observations of clinicians and patients were recorded, together with details of each soldier's military career.
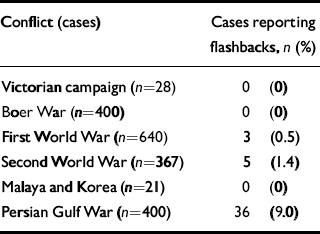
Table 2 The incidence of flashbacks in post-combat syndromes
| Conflict (cases) | Cases reporting flashbacks, n (%) | |
|---|---|---|
| Victorian campaign (n=28) | 0 | (0) |
| Boer War (n=400) | 0 | (0) |
| First World War (n=640) | 3 | (0.5) |
| Second World War (n=367) | 5 | (1.4) |
| Malaya and Korea (n=21) | 0 | (0) |
| Persian Gulf War (n=400) | 36 | (9.0) |
Table 3 Veterans of the Persian Gulf War reporting flashbacks compared with veterans of other conflicts

| Gulf War veterans reporting flashbacks (9%) compared with: | Difference in proportions reporting flashbacks (%) | 95% CI |
|---|---|---|
| Victorian campaign veterans (0%) | 9.0 | 6-12 |
| Boer War veterans (0%) | 9.0 | 6-12 |
| First World War veterans (0.5%) | 8.5 | 6-11 |
| Second World War veterans (1.4%) | 7.6 | 5-11 |
| Korea/Malaya veterans (0%) | 9.0 | 6-12 |
Table 4 Post-traumatic stress disorder symptom checklist for the First and Second World War veterans who reported flashbacks

| Case no. and diagnosis | Flashbacks | Recurrent dreams | Anxiety | Poor memory | Sleep difficulty | Irritability | Concentration difficulty | Startle response | Loss of interest | Detachment | Avoidance |
|---|---|---|---|---|---|---|---|---|---|---|---|
| First World War | |||||||||||
| 1 Neurasthenia | + | + | + | + | + | + | + | + | + | + | |
| 2 Neurasthenia | + | + | + | + | + | + | + | + | + | + | + |
| 3 Neurasthenia | + | + | + | + | + | + | + | + | |||
| Second World War | |||||||||||
| 4 Psychoneurosis | + | + | + | + | + | + | + | + | + | ||
| 5 Psychoneurosis | + | + | + | + | + | + | + | + | |||
| 6 Battle hysteria | + | + | + | + | + | + | + | ||||
| 7 Psychoneurosis | + | + | + | + | + | + | + | ||||
| 8 Anxiety state | + | + | + | + | + |
Flashbacks
Flashbacks, a form of dissociative state, are defined as involuntary, vivid images that occur in a waking state (Reference FrankelFrankel, 1994). Although the term itself was not mentioned in the first diagnostic checklist for PTSD published in DSM—III in 1980, the phenomenon was outlined:
‘Re-experiencing of the trauma as evidenced by at least one of the following: (a) recurrent and intrusive recollections of the event, (b) recurrent dreams of the event and (c) sudden acting or feeling as if the traumatic event were reoccurring, because of an association with an environmental or ideational stimulus’ (American Psychiatric Association, 1980: p. 238).
In 1987, DSM—III—R included the term ‘flashback’ as a synonym for some aspects of these experiences (American Psychiatric Association, 1987). One of the criteria for PTSD was defined as follows:
‘Sudden acting or feeling as if the traumatic event were recurring (includes a sense of reliving the experience, illusions, hallucinations, and dissociative [flashback] episodes, even those that occur upon awakening or when intoxicated)’ (American Psychiatric Association, 1987: p. 250).
Other symptoms of PTSD such as difficulty in sleeping, nightmares and poor concentration can be found in other disorders (e.g. depression), reflecting the high level of comorbidity. Although the term had originally been introduced to describe visual imagery related to hallucinogens (Reference Sierra and BerriosSierra & Berrios, 1999), the flashback as a diagnostic tool is largely limited to PTSD.
Generally, it has been argued that PTSD is the product of indelible traumatic memory, the ability of which to capture events with cinematic and photographic accuracy results in the presence of flashbacks (Reference YoungYoung, 2002). This memory is considered abnormal because of its unchanging nature. This model stands in sharp contrast to earlier explanations offered by Freud, Rivers and others for the traumatic neuroses. Freud argued that certain experiences, which are neither salient nor meaningful when they occur, acquire an emotional potency or importance by an additional piece of information. Belatedly, a normal recollection of an event becomes transformed into a disturbing and highly significant memory.
The hypothesis has been put forward that the sensory form taken by intrusive memories relates to the nature of the trauma — people who witnessed traumatic events would have a high proportion of visual intrusions (Reference Ehlers, Hackmann and SteilEhlers et al, 2002). Accordingly, we expected to find reports of flashbacks in the medical records of soldiers who had observed the horrific sights of warfare. Because the term ‘flashback’ did not exist during the First and Second World Wars, we were forced to re-evaluate contemporary descriptions. Visual hallucinations reported in individuals who were not psychotic were included. For example, Driver Thomas Hughes, a regular in the Royal Artillery, went overseas as part of the British Expeditionary Force in August 1914 and managed to survive until August 1918, when he was admitted to a hospital in Gateshead with shellshock. On discharge from the army he suffered from vertigo, night starts, claustrophobia, tremors, headaches, poor sleep and weakness, and was described as irritable and depressed. He had frequent war dreams and experienced ‘visual and auditory hallucinations’ during the latter part of 1919, a year after active service in France, but had no delusions and was described as ‘rational and reasonable, though apathetic’ (Anon., 1929). In November 1920, when he had lost all interest ‘in anything or anybody’, Hughes reported seeing ‘things at night, e.g. faces and somebody standing in the room’, which occurred in a context of awakening. This phenomenon was accompanied by a fear that ‘someone might finish him, knock him down or something’. His vivid visual recollections of war appear to have ended after out-patient psychotherapy in November 1921. Similarly, a First World War veteran, who had been treated for shellshock at Craiglockhart, was described in 1927 as having ‘hypnagogic hallucinations of a man with a gaping throat’ (Anon., 1928), and was rated as experiencing flashbacks.
In contrast, a soldier who was described as ‘always thinking of the past’ with a memory ‘too good for past events’ (Anon., 1923) did not meet our criteria, as these appeared to be ideas and images under the veteran's rational control. Where there was doubt we rated the phenomenology as present. For instance, one infantryman undergoing treatment in a Ministry of Pensions psychotherapy clinic from April 1922 to May 1923 was reported as experiencing ‘frequent revival of war experiences’ in a context of disturbing war dreams, impaired memory and concentration (Anon., 1924). Because he appeared to be reliving episodes from his active service in France, these phenomena were included.
RESULTS
Analysis of the 1856 cases revealed that flashbacks were virtually non-existent before the First World War and were still rare during the Second World War (Table 2). Although not a common phenomenon today, their incidence is significantly higher than in previous conflicts (χ2=98.47, d.f.=5, P<0.001). The proportion of veterans experiencing flashbacks after the Gulf War was also compared with the percentage found in ex-servicemen from earlier conflicts, and the difference in each case was found to be significant (Table 3).
All three First World War veterans and all five Second World War servicemen had seen combat and therefore almost certainly met the exposure criterion for PTSD. To discover whether these cases would fulfil the diagnostic requirements, the veterans' other symptoms were recorded (Table 4). Although anxiety, difficulty in sleeping and poor concentration were common, other features such as social avoidance and startle response were not often identified. Three of the eight cases (cases 3, 6 and 8) did not meet DSM—IV criteria (American Psychiatric Association, 1994) in so far as there was insufficient evidence of persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness. Case 8 had a number of somatic symptoms, including headache, tremor, rapid breathing, chest pain and dyspepsia, and had been diagnosed as suffering from effort syndrome. Similarly, case 6 experienced chest pain, shortness of breath, palpitations and abdominal pains, and had been admitted to a military hospital with a diagnosis of battle hysteria.
DISCUSSION
Incidence
In recent decades PTSD has become the most prevalent post-combat psychiatric diagnosis. The National Vietnam Veterans Readjustment Study, involving a representative sample of 3000 subjects, estimated that 15% of male Vietnam veterans had PTSD 15 years after completing their service (Reference Kulka, Schlenger and FairbankKulka et al, 1990). A study conducted 1 year after the Lebanon War of 1982 showed that 16% of a random sample of Israel Defence Force personnel had PTSD (Reference Solomon, Weisenbery and SchwarzwaldSolomon et al, 1987). A 6-year follow-up of Israeli combat stress casualties revealed that 41% had the symptoms of PTSD (Reference SolomonSolomon, 2001). O'Brien & Hughes (Reference O'Brien and Hughes1991) found a prevalence of 22% in a sample of 64 UK servicemen who had fought in the Falklands conflict, although the authors subsequently expressed caution about the significance of the symptoms reported. It was hypothesised that if PTSD has always existed, veterans of earlier wars would also exhibit symptoms of the disorders, as many had been exposed to prolonged and intense stress.
Although we did find cases from the First and Second World Wars which would meet today's criteria for PTSD, their incidence was significantly lower than for the Gulf conflict. Previous historical investigations have relied on single case studies to make the point that PTSD is a timeless disorder. However, such studies lack a denominator and are instead based on an active search through historical literature for descriptions that resemble modern formulations of PTSD, while presumably discarding presentations that appear different.
Issues of evidence
It could be argued that our negative findings are simply the result of a failure on the part of servicemen to report symptoms or the failure of doctors to ask about them. Although physicians might have occasionally discounted symptoms because they were not part of a recognised syndrome, as diagnosticians they were often forced to rely on observation. The repeated nature of the assessment procedure and the requirement to document symptoms suggest that underreporting by doctors was not a major cause of the low incidence. Equally, it was in the veteran's interest to relate distressing symptomatology to improve his chances of being awarded or sustaining a war pension, while the intrusive and disturbing nature of flashbacks might have prompted their description. It is possible, however, that some servicemen were reluctant to describe the phenomenon because they feared being diagnosed as mad or malingering.
Flashbacks do not seem to have been described in other ways. Although visual hallucinations and other perceptual abnormalities were widely recorded for psychotic states, they were rarely reported for historic, post-combat syndromes.
In two respects the flashback percentages for the First and Second World Wars and the Gulf conflict may overstate the true incidence. We relied on self-report (the benefit of the doubt being given to the veteran) and in some cases there had been no examination by a psychiatric specialist. It is also possible that, with growing familiarity, the term ‘flashback’ is increasingly being used to describe a broadening group of symptoms, including ruminations and eidetic memories.
Our results support the hypothesis that the symptoms of intrusion and avoidance, which lie at the heart of the DSM concept of PTSD, also occur relatively infrequently in earlier forms of traumatic stress disorders. Somatic symptoms appear much more often in presentations of post-trauma illness from the 19th and early 20th centuries.
Flashbacks and culture
Why, then, did the flashback — a core symptom of PTSD — become more common in the latter part of the 20th century? Shorter has argued that the nature of medically unexplained syndromes has itself changed, with a shift from apparently neurological symptoms such as paralyses, tremors and fits to more ill-defined and subjective symptoms such as fatigue, pain and depression (Reference ShorterShorter, 1986). The flashback itself is a visual device practised in the cinema to introduce immediate dramatic tension. Several authors have argued that there is a direct association between the flashback and films (Reference Blank, Sonnenberg, Blank and TalbottBlank, 1985). Leys wrote:
‘the term flashback implies the cinematic possibility of literally reproducing or cutting back to a scene from the past and hence expresses the idea that the trauma victim's experiences are exact “reruns” or “replays” of the traumatic incident’ (Reference LeysLeys, 2000: p. 241).
Yet films were an integral part of popular culture during the First and Second World Wars, when flashbacks appear to have been much rarer than today. Involuntary visual images may be tied more closely to the mass production of affordable television sets in the 1950s and 1960s and the subsequent introduction of video recorders. This hypothesis is supported by the intrusive nature of the flashback. People make a conscious choice to go to the cinema and travel to a designated building to view exciting or disturbing pictures. The experience is ritualised and contained. In contrast, television in the home can be a source of sudden and disturbing imagery in a familiar and apparently safe situation. It is possible that the introduction of colour pictures also intensified the image by making it more realistic. Indeed, some patients describe flashbacks as being like the playback of a vivid video recording.
We have been unable to study the incidence of flashbacks in Vietnam veterans because UK troops were not deployed to that conflict. Given that PTSD was at one time called ‘post-Vietnam syndrome’, it is possible that the significant increase in the incidence of flashbacks took place during the 1960s. Films about the war, such as The Deer Hunter, sometimes cut scenes of warfare into civilian episodes in a dramatic and abrupt manner. Whether these reflected the veteran's flashback experience or, alternatively, served as a cultural influence shaping the form of PTSD is impossible to say, but the flashback has become a frequent cinematic device in films about the Vietnam War.
Universal phenomenon
Basing his hypothesis on the model of an animal's response to inescapable shock or stress, Bessel van der Kolk has attempted to explain traumatic memory in neurobiological terms. Traumatic experiences, he argues, are encoded in the brain in a manner akin to skills, habits and reflex actions, such that they are preserved with a timeless accuracy, which, in turn, accounts for the long-term effects of PTSD. Both flashbacks and traumatic nightmares are processed not by the mediated or ‘declarative’ memory system but as ‘subcortically based emotional memories’ (Reference Van der KolkVan der Kolk, 1994). By distinguishing these events from normal narrative memory, this approach implies that all participants in war are alike in so far as they will have suffered from objective cerebral changes in ways that tend to eliminate the issue of moral meaning. Leys has criticised this school as accepting the ‘waxing and waning of interest in trauma in the course of more than a century’, while presenting PTSD as a ‘timeless diagnosis, the culmination of a lineage that is seen to run from the past to the present in an interrupted yet ultimately continuous way’ (Reference LeysLeys, 2000: p. 3).
Evolving responses to trauma
Our data provide empirical support for Young's seminal observations of PTSD in its current manifestation as a contemporary culture-bound syndrome whose expression has been influenced by powerful undercurrents, including technological advances in broadcasting traumatic events and a wider appreciation of psychological processes. Although cases undoubtedly existed during the First and Second World Wars that would meet today's criteria, their incidence was significantly lower. It is possible that the rarity of flashbacks during those conflicts was because servicemen tended to express the stress of battle in somatic terms. Shellshock, for example, was often depicted by contemporaries in terms of contractures, tics, movement disorders and paresis. Our findings imply that the psychopathology of trauma is not static and that culture has an impact on the expression of distressing memories. There is no single way for human beings to respond to the terrifying events of war, and the concept of a ‘universal trauma reaction’ appears flawed. We suggest that PTSD is one more phase in the continually evolving picture of human reaction to adversity (Reference YoungYoung, 1995).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Some characteristics of post-traumatic stress disorder, notably flashbacks, appear to be culturally influenced.
-
▪ The psychopathology of trauma is not static and distressing memories are not conveyed in a universal manner across time.
-
▪ The emphasis on somatic symptoms in trauma-related disorders appears to have lessened in the post-Vietnam period, whereas neuropsychiatric symptoms have become more prominent.
LIMITATIONS
-
▪ Because flashback is a modern term we were forced to re-evaluate historical descriptions.
-
▪ We were reliant on the self-report of symptoms by veterans who had been awarded war pensions.
-
▪ The destruction of some war pension files relating to the Boer War and the First World War forced a reliance on random samples, which may not be totally representative.
Acknowledgements
The authors thank Professor Anke Ehlers, Professor Edward Shorter, Dr Stuart Turner and Professor Allan Young for their valuable comments on an earlier draft of this paper. We are grateful to Professor Harry Lee for allowing us access to anonymised MAP data. Thanks are also due to Vasilis Nikolaou for his help with the statistical analysis. The study was funded by the US Army Research and Material Command under grant number DMD17-98-1-8009. E.J. was supported by a grant from the US Department of Defense.







eLetters
No eLetters have been published for this article.