To our knowledge no prospective longitudinal study has followed an adult refugee cohort for more than 10 years. We report findings from the third interview phase of a longitudinal prospective community cohort study of Vietnamese refugees settled in Norway. They were included in the study upon their arrival in Norway in 1982 (T 1) and followed up in 1985 (T 2) Reference Hauff1 . The earlier findings, of stable and high levels of mental health problems after 3 years in exile, Reference Hauff and Vaglum2 are consistent with other subsequent short-term follow-up studies among refugees. Reference Mollica, Caridad and Massagli3–Reference Silove and Ekblad5 The aims of the study reported here were to investigate the long-term course and outcome of these individuals' mental status, and to identify which early resettlement factors were relevant to predicting levels of psychological distress over 20 years later.
Method
Design and procedures
The design of the study was similar to that of the two earlier studies of this cohort. Reference Hauff1 An interview administered in the respondents' home (by A.B.G. and A.B.V.) included a self-report questionnaire available in Vietnamese and Norwegian, and a structured face-to-face interview in Vietnamese. The study was approved by the regional committee for medical research ethics and the Norwegian Social Science Data Services. Written information about the study was provided in Vietnamese and Norwegian.
Sample
All Vietnamese refugees aged 15 years or older who arrived in south-east Norway from transit camps in south-east Asia during an 8-month period in 1982 were invited to take part in the first study (T 1). Norwegian merchant vessels had rescued the refugees by chance from the South China Sea, and these people were offered resettlement in Norway. Thus the original cohort was a relatively unselected sample from this wave of Vietnamese ‘boat people’. In the current study (T 3; 2005–6) we sought to interview all surviving members of the cohort remaining in Norway. We were able to collect data from 80 respondents; 24 others had died or moved to another country (Fig. 1). Hence the T 3 sample represented 57% of the original cohort and 74% of those eligible for inclusion.

Fig. 1 Flow diagram of inclusion and attrition.
The Norwegian normative sample, used for comparison of the Symptom Checklist–90–Revised (SCL–90–R) results, consisted of 466 men and 507 women over 19 years old who were representative of the adult population in Norway. Reference Vassend, Lian and Andersen6
Assessments
Sociodemographic variables
Included in the self-report questionnaire at T 3 were marital status, family reunion, presence of family in Norway, social network including Vietnamese and Norwegian friends, religious affiliation, level of education, current work status and economic support.
Symptoms
Psychological distress was rated with the same measure used in 1982 and 1985: the SCL–90–R. Reference Derogatis7 This instrument is considered valid and reliable, and has been used in several studies of refugee mental health, both in its original form, Reference Ghazinour, Richter and Eisemann8,Reference Araya, Chotai, Komproe and de Jong9 and as the shorter 25-item Hopkins Symptom Checklist (HSCL–25). Reference Thapa and Hauff10,Reference Hermansson11 The Global Severity Index (GSI) represents the mean score of all 90 items of the SCL–90–R, with a score of 1 or more used to identify a probable psychiatric ‘case’. Reference Vassend, Lian and Andersen6 As self-report measures may be oversensitive in identifying true cases, Reference Silove, Manicavasagar, Mollica, Thai, Khiek and Lavelle12 we refer to those scoring at least 1 as reaching threshold score.
Trauma exposure
The analyses reported here included information gathered at T 1 and T 2. An additive index combining the factors of having been wounded in the war, having been incarcerated in prison or a concentration camp for a year or more, and having been in great danger before the escape represented the variable ‘extreme traumatic stress’ before the escape (minimum score 0, maximum 3).
Statistical analysis
Univariate analyses included chi-squared tests, Mann–Whitney tests, t-tests and Pearson correlations. Changes in SCL–90–R scores over time were assessed by linear mixed effects models (R version 2.9.7 for Windows, R package ‘nlme’, R Foundation for Statistical Computing, see www.r-project.org), Reference Pinheiro and Bates13 adjusting for relevant T 1 variables. The relationships between SCL–90–R scores at T 3 and baseline (T 1/T 2) variables were investigated by two types of multiple linear regression analyses. First, we generated a model identical to the one published for T 2 data, Reference Hauff and Vaglum2 except that the outcome was the SCL–90–R GSI score at T 3 (independent variables measured at T 1 – or, if not assessed at T 1, at T 2 – were age, gender, years of education in Vietnam, an additive score of extreme traumatic stress, close confidante upon arrival, high-impact negative life events during the first 2 years in Norway, and separation from close family at T 2). Second, for a more comprehensive model predicting GSI at T 3, we included some pre-specified baseline variables from T 1 and T 2 together with two indices of mental health status prior to T 3, namely the GSI score at T 1 and a change measure (GSI at T 2 minus GSI at T 1, with a positive value indicating worsening of symptoms from T 1 to T 2). The significance level was set at 0.05. When adjusting for multiple comparisons the Benjamini–Hochberg procedure was used. Reference Benjamini and Hochberg14 All analyses used SPSS version 15 for Windows and R (see above).
Results
Sociodemographic variables
The sample at T 3 consisted of 12 women and 68 men, with a mean age of 47.5 years (s.d. = 6.8, range 38–70), the respondent group being younger and comprising more men than women compared with the attrition group (further details are given in online Table DS1).
Psychological distress
All but one of the 80 respondents completed the SCL–90–R at T 3 (the exception was a person with psychosis). There was no significant gender difference in mean GSI scores at T 3 (women 0.48 v. men 0.49). The mean GSI decreased significantly from 0.81 at T 1 to 0.49 at T 3 (difference: s.d. = 0.55, 95% CI 0.29–0.44, P<0.001).
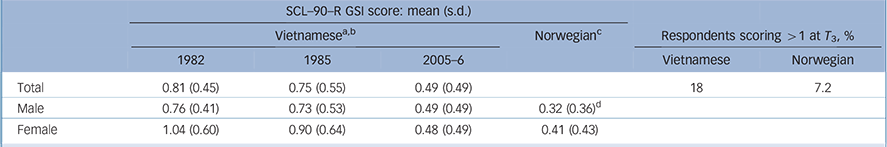
Table 1 shows the GSI mean scores at the three time points compared with the Norwegian normative sample (for subscale scores see online Table DS2). From arrival to follow-up at T 3 there were significant decreases in both the GSI and the means for all subscales of the SCL–90–R (online Table DS3), with the exception of somatisation and anger/hostility. Eighteen per cent of respondents (n = 14) reached threshold scores at T 3 (GSI = 1.00), more than twice the percentage of Norwegians (7.2%). For the Vietnamese cohort there was no significant difference between GSI rates at T 3 and those recorded at T 2 (25%, n = 20) and T 1 (26%, n = 20).
Table 1 Global Severity Index scores for the study cohort (n = 79) at the three assessment points compared with the Norwegian normative sample
| SCL—90—R GSI score: mean (s.d.) | ||||||
|---|---|---|---|---|---|---|
| Vietnamesea,b | Norwegianc | Respondents scoring > 1 at T 3, % | ||||
| 1982 | 1985 | 2005-6 | Vietnamese | Norwegian | ||
| Total | 0.81 (0.45) | 0.75 (0.55) | 0.49 (0.49) | 18 | 7.2 | |
| Male | 0.76 (0.41) | 0.73 (0.53) | 0.49 (0.49) | 0.32 (0.36)d | ||
| Female | 1.04 (0.60) | 0.90 (0.64) | 0.48 (0.49) | 0.41 (0.43) | ||
Prediction of psychological distress at T 3
In the first regression analysis using T 1/T 2 predictors and GSI at T 3, the model being similar to the one published earlier, Reference Hauff and Vaglum2 the included predictors explained 13% of the variance of GSI but no single predictor was associated significantly with the index of distress at T 3. In the second regression, a greater GSI score at T 1 and the change score (the difference in GSI scores between T 2 and T 1) were both significant predictors of a higher GSI at T 3 (Table 2).
Table 2 Multiple regression analysis for Global Severity Index scores at T 3 (n = 79)

| Variables from T 1/T 2 | Regression coefficient | P | 95% CI | R 2 |
|---|---|---|---|---|
| Age at inclusion | -0.001 | 0.86 | -0.02 to 0.01 | 0.008 |
| Gendera | 0.11 | 0.44 | -0.18 to 0.40 | 0.009 |
| Vietnamese contactb | 0.14 | 0.19 | -0.07 to 0.34 | 0.049 |
| Norwegian contactc | 0.09 | 0.54 | -0.20 to 0.37 | 0.062 |
| Healthd | -0.003 | 0.98 | -0.23 to 0.22 | 0.10 |
| GSI score at T 1 | 0.48 | <0.001 | 0.23 to 0.73 | 0.16 |
| GSI difference (T 2 - T 1)e | 0.41 | 0.001 | 0.19 to 0.63 | 0.31 |
Discussion
Our results suggest a complex picture. The mental health of the cohort as a whole had improved significantly since the refugees' arrival in Norway, but the mean scores on the SCL–90–R remained higher than for native Norwegians. Almost a fifth of the cohort, more than twice the percentage of Norwegians had psychological distress scores above threshold on the SCL–90–R, suggesting that the Vietnamese remained a vulnerable group. These findings are broadly consistent with those of Steel et al in suggesting that the majority of Vietnamese had achieved reductions in most symptom domains over time, but a minority remained highly symptomatic. Reference Steel, Silove, Phan and Bauman15
Implications for the treatment of refugees
Our findings may help to clarify the trajectory of symptoms among refugees over a prolonged period of resettlement. In stable resettlement environments, refugee populations tend to manifest high levels of distress over the earlier years, as indicated by the results for T 1 and T 2. This is consistent with other studies, Reference Lie4 and supports the notion that a combination of recent trauma and resettlement/acculturation challenges continue to act as stressors during this time. Nevertheless, the T 3 data indicate that at a population level, and in the context of a stable resettlement environment, Reference Schweitzer, Melville, Steel and Lacherez16,Reference Porter and Haslam17 most refugees have the capacity for symptom improvement over the longer term, although levels of distress may remain higher than among the host population. Symptom improvement during the first 3 years, signified in this study by a reduction in GSI between T 1 and T 2, may therefore represent an important predictor of a positive long-term prognosis, in this instance after 23 years.
Prediction of outcomes: implications for early assessment and intervention
A minority of study participants remained psychologically impaired over many years. Trauma might have been a factor initiating some of these reactions, but in the longer term, as indicated, a key predictive index appeared to be the level and trajectory of psychological symptoms during the period of early resettlement. This supports the potential value of serial screening programmes for refugees, a procedure that could be followed by comprehensive assessment of the identified at-risk group to detect those with clinical disorders in need of treatment. Hence, early intervention may be relevant not only to overcome immediate distress but also to avert risk of psychological difficulties in later years. Still, the predictive capacity of the regression analysis was modest, suggesting that other unmeasured post-migration experiences and/or personal vulnerabilities might have a role in perpetuating psychological symptoms over time, Reference Marshall, Schell, Elliott, Berthold and Chun18 or in initiating new disorders during the ensuing two decades.
Limitations
Despite of the strengths of the study, in particular its prospective longitudinal design, important limitations need consideration. Attrition is evident in most refugee studies, Reference Lie4 and compared with the attrition group, included respondents were younger and more often male than female. This, together with the small original sample and the special characteristics of Norwegian society, may limit the generalisability of the findings to other refugee populations. In addition, gender-specific comparisons could not be undertaken because the relevant information was not available for the Norwegian normative data-set.
The follow-up study did not include a clinical diagnostic interview, which limits comparisons with other studies of refugees. Reference Roth, Ekblad and Agren19,Reference Hinton, Chau, Nguyen, Nguyen, Pham and Quinn20 Although a study among Vietnamese refugees has shown reasonable concordance between a clinical interview (the Structured Clinical Interview for DSM–IV Axis I disorders) and the HSCL–25, Reference Smith Fawzi, Murphy, Pham, Lin, Poole and Mollica21 a comparable study among Cambodians indicated that a clinical interview yielded a more conservative prevalence rate. Reference Silove, Manicavasagar, Mollica, Thai, Khiek and Lavelle12 A recent meta-analysis of the entire refugee mental health field showed a regular pattern in which questionnaires (often derived from the Symptom Checklist) on average returned a 10–13% higher prevalence than interviews when other methodological factors (sample size, approach to sampling) were taken into account. Reference Steel, Chey, Silove, Marnane, Bryant and van Ommeren22 These observations caution against inferring that all Vietnamese who scored above threshold in our study could definitely be assigned to the ‘cases’ group. Further examination would be needed (and warranted) to specify accurately those in need of treatment.
We acknowledge the risk of reduced semantic equivalence arising from the use of an early version of the Vietnamese translation of the SCL–90–R, Reference Flaherty, Gaviria, Pathak, Mitchell, Wintrob and Richman23 but we considered it important to use the same translation for longitudinal comparisons. Other studies among Vietnamese have used a culturally specific measure of mental health, the Phan Vietnamese Psychiatric Scale (PVPS), in conjunction with an international instrument. Reference Phan, Steel and Silove24 This approach increased the overall rates of detected mental health disorders, suggesting the possibility that cases may be overlooked when Western-derived instruments such as the SCL–90–R are used alone.
Clinical implications
Although self-reported psychological distress among Vietnamese refugees decreased significantly over time, even after 23 years of resettlement a greater proportion of this cohort reached threshold SCL–90–R scores compared with the native Norwegian group. Therefore, this population should still be considered to be at increased risk of mental health problems, justifying special attention from psychiatric services. The longitudinal data support the importance of screening refugees in the early years of resettlement, since elevated levels of psychiatric symptoms during that period appear to indicate long-term risk.
Funding
The study was supported by grants from the Western Norway Regional Health Authority, the Centre for Child and Adolescent Mental Health, University of Bergen, the Legacy of Sommer, Lundbeck Pharma AS, the Meltzers Høyskolefond, Stavanger University Hospital and Oslo University Hospital, Ullevål Department of Psychiatry.






eLetters
No eLetters have been published for this article.