The Reform Law 180, approved in Italy in 1978, had - and still has - great national and international significance for its dramatic consequences on both clinical and health organisational aspects of psychiatry: the law, in short, had the great effect of bringing psychiatry back to medicine, to the community and to the general hospital. This was the starting point of other relevant events, one of which was the establishment of the specialty of consultation–liaison psychiatry in Italy (Reference Cazzullo, Comazzi and GuaraldiCazzullo et al, 1984). Since then, consultation–liaison psychiatry has gradually developed worldwide and in Italy as a super-specialised branch of psychiatry, able to put into practice - to operationalise - the great psychosomatic tradition in its three interrelated strands of clinical, teaching and research activities. The report that follows is strongly influenced by this historical background.
CLINICAL WORK PERFORMED
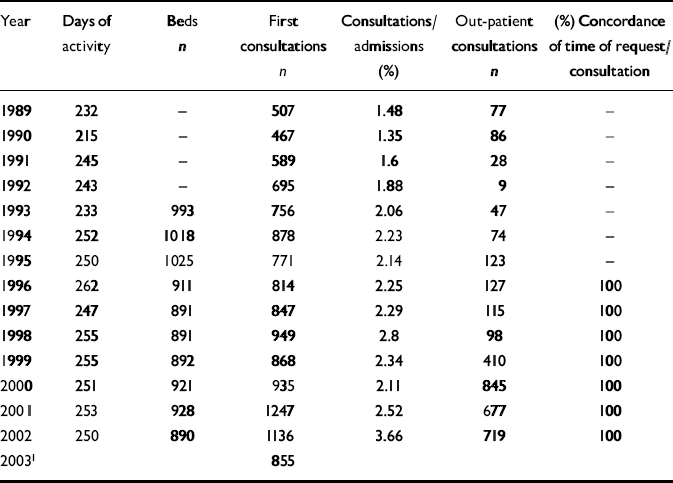
Founded in 1989, the Consultation–Liaison Psychiatry service of Modena University Hospital is one of the services of that hospital's psychiatric department, which also includes a psychiatric ward (for both voluntary and compulsorily admitted patients), a day hospital, an out-patient clinic and a rehabilitation unit. With its consultation–liaison activities and out-patient clinic, the Modena service now provides about 1200 first consultations a year, corresponding to around 3% of all patients admitted to non-psychiatric hospital departments in the same period - twice the European average of 1.4% (Reference Huyse, Herzog and LoboHuyse et al, 2001a ; Table 1). The workforce comprises one full-time and one half-time consultation–liaison psychiatry consultants, four or five psychiatry residents, two consultant psychiatrists who are also PhD students and a clinical psychologist.
Table 1 Modena University Hospital Consultation-Liaison Psychiatry Service: activity data
| Year | Days of activity | Beds n | First consultations n | Consultations/admissions (%) | Out-patient consultations n | (%) Concordance of time of request/consultation |
|---|---|---|---|---|---|---|
| 1989 | 232 | - | 507 | 1.48 | 77 | - |
| 1990 | 215 | - | 467 | 1.35 | 86 | - |
| 1991 | 245 | - | 589 | 1.6 | 28 | - |
| 1992 | 243 | - | 695 | 1.88 | 9 | - |
| 1993 | 233 | 993 | 756 | 2.06 | 47 | - |
| 1994 | 252 | 1018 | 878 | 2.23 | 74 | - |
| 1995 | 250 | 1025 | 771 | 2.14 | 123 | - |
| 1996 | 262 | 911 | 814 | 2.25 | 127 | 100 |
| 1997 | 247 | 891 | 847 | 2.29 | 115 | 100 |
| 1998 | 255 | 891 | 949 | 2.8 | 98 | 100 |
| 1999 | 255 | 892 | 868 | 2.34 | 410 | 100 |
| 2000 | 251 | 921 | 935 | 2.11 | 845 | 100 |
| 2001 | 253 | 928 | 1247 | 2.52 | 677 | 100 |
| 2002 | 250 | 890 | 1136 | 3.66 | 719 | 100 |
| 20031 | 855 |
PREVIOUS RESEARCH
In the work previously addressed by the team, three main streams of research are recognisable. The first is that originating from the intense involvement of the team in the three EU-funded multicentre projects and promoted by the European Consultation–Liaison Workgroup (ECLW) since the beginning of the 1990s (Reference Herzog, Huyse, Cardoso and BaertHerzog et al, 1995; Huyse et al, Reference Huyse, Herzog and Malt1996, Reference Huyse, Herzog and Lobo2000a ,Reference Huyse, Herzog and Lobo b , Reference Huyse, Herzog and Lobo2001a ; Reference Lobo, Huyse and HerzogLobo et al, 1996; Reference Malt, Huyse and HerzogMalt et al, 1996). Further national projects sprang from that experience (Reference Gala, Rigatelli and de BertoliniGala et al, 1999; Reference Grassi, Gritti and RigatelliGrassi et al, 2000). This involvement had numerous direct and indirect outcomes, particularly the increasing improvement in clinical and organisational standards: for example, the regular use of structured forms for psychiatric referral and back-referral, and of computerised databases, and better definitions of procedures of intervention, specifically for common or critical clinical situations, such as delirium and self-harm. The obvious next step was the involvement in quality assurance work: from 1994 to 1997, the team took part in a multi-centre quality assurance study (Reference Herzog, Huyse, Cardoso and BaertHerzog et al, 1995); meanwhile, work began on the accreditation–certification scheme, culminating in International Organization for Standardization ISO 9000 certification of the whole University of Modena psychiatry department in 2002.
A further emanation of the initial ECLW projects is the development of INTERMED, a screening instrument designed to predict complexity of care, acknowledged as the operationalisation of the Engel biopsychosocial paradigm (Reference De Jonge, Huyse and Slaetsde Jonge et al, 2001; Reference Huyse, Lyons and StiefelHuyse et al, 2001b ).
A second research stream is that dealing with organisational issues in consultation–liaison psychiatry. Two examples are an analysis of what happens to patients referred to a consultation–liaison service following their discharge from hospital (Reference Rigatelli, Casolari and MassariRigatelli et al, 2001), and a description of the teaching programme promoted by the consultation–liaison psychiatry service in Modena University Hospital (Reference Rigatelli, Ferrari and UguzzoniRigatelli et al, 2000).
The third is less epidemiological and more speculative in nature, involving collaboration with specialists from other medical disciplines. These projects address the ‘boundaries of medicine’ - syndromes of difficult biological definition such as vertigo (Reference Monzani, Casolari and GuidettiMonzani et al, 2001), obstetric and gynaecological or andrological disorders (Reference Pescatori, Silingardi and GaleazziPescatori et al, 2000; Reference Rigatelli, Galeazzi and PalmieriRigatelli et al, 2002) and, previously, ulcerative colitis (Reference RigatelliRigatelli, 1981).
NEW INITIATIVES
Work is in progress in all of the three areas described above. As a contribution to the operationalisation of psychosomatic constructs, a recent study on interrater reliability of the Diagnostic Criteria for use in Psychosomatic Research, first conceived by Fava et al (Reference Fava, Freyberger and Bech1995), is shortly to be published in Psychosomatics (Reference Galeazzi, Ferrari and MackinnonGaleazzi et al, 2004).
The Modena Consultation–Liaison Psychiatry service is one of thirty centres involved in the second national multicentre inquiry into consultation–liaison psychiatry activity in Italy, recently conducted by the Società Italiana di Psichiatria di Consultazione (Italian Society of Consultation Psychiatry; www.sipc.it), which collected data on more than 10 000 patients referred to a consultation–liaison psychiatry service. In another analysis of service management and organisation, the team has conducted a study on levels of satisfaction among the Modena University Hospital ward physicians, surgeons and head nurses about the quality of consultation–liaison activities.
Increasing interest is being focused on consultation–liaison psychiatry in the setting of primary care or general medicine outside the hospital. This is still a pioneer field in Italy. A study is in progress to characterise features of frequent attenders at primary care clinics, and possibly to identify higher rates of psychic distress in these patients compared with normal attenders.
The recent opening of an active transplant unit at Modena University Hospital and the consequent increase in psychiatric referrals, both arising from pre-transplant assessment procedures and after surgery, were the stimulus to initiating research in this area, including psychopathological evaluation, evaluation of psychosocial and familial variables, and investigation of adaptive and compliance abilities.




eLetters
No eLetters have been published for this article.