Late-life depression is a common psychiatric disorder in old age. It often has a poor long-term prognosis, more frequently showing a chronic course and a higher relapse rate compared with depression at younger ages. Reference Mitchell and Subramaniam1 In addition, late-life depression is linked to more medical comorbidity (e.g. cognitive impairment and cardiovascular diseases) and a high risk of mortality. Reference Penninx, Beekman, Bandinelli, Corsi, Bremmer and Hoogendijk2-Reference Baldwin, Gallagley, Gourlay, Jackson and Burns4 A different phenomenology has been suggested for late-life compared with early-life depression. Possible reasons for a different presentation of late-life depression are the overlap of somatic symptoms of depression and physical disease in old age, and sociocultural factors such as the minimal expression of sadness in the current cohort of old people not used to complaining about depressed mood. Reference Baldwin, Jacoby, Oppenheimer, Dening and Thomas5 Also, age-related biological and psychological factors may underlie a different phenomenology of late-life and early-life depression. In three narrative reviews insufficient evidence was found to support a different presentation of depression in older people. Reference Baldwin, Jacoby, Oppenheimer, Dening and Thomas5-Reference Kok7 However, conceptual and methodological limitations of the reviewed studies, and the inherent subjectivity and bias proneness of narrative reviews, might have had a role in this conclusion. Therefore, this meta-analysis of studies examines the phenomenology of depression at the single-item level of the Hamilton Rating Scale for Depression (HRSD), also known as the Hamilton Depression Rating Scale (HDRS) or abbreviated to HAM-D.
Method
A systematic literature search was performed in PubMed, Embase and PsycINFO. The following (key)words were used: depress*, depressive, major depression, dysthymic disorder, geriatric patients, geriatric psychiatry, elder*, elderly, geriatric, aged, old age, old, oldest old, middle aged, adult, adults, early onset, late onset, onset age, age of onset, age at onset, phenomenol*, symptom*, clinical presentation, clinical features, atypical, melanchol* and dimension*. These were combined with the Medical Subject Headings (MeSH) depression, depressive disorder, signs and symptoms and age factors. The search was run on 18 July 2011. No limitation in the search strategy was inserted. Reference lists from all relevant literature were hand-searched for additional relevant articles overlooked by the database search. Titles and abstracts of the articles were screened to identify possible relevant articles. Finally, the full texts of the remaining articles were reviewed (by J.H.) with respect to our inclusion and exclusion criteria. In cases of doubt, articles were discussed in a consensus meeting with three authors (J.H., R.K., R.M.).
Studies were excluded if no comparison was made between old age and younger age regarding the phenomenology of major depression; if studies did not present primary data (e.g. letters, comments and reviews were excluded); and if the study population consisted mainly of participants with bipolar disorder, schizoaffective disorder or dementia. Samples could be drawn from an in-patient, out-patient, primary healthcare or general population. As depression is a heterogeneous disorder irrespective of age, strict diagnostic criteria were used. Participants had to be diagnosed with major depression according to the RDC, ICD-9, ICD-10, DSM-III, DSM-III-R or DSM-IV criteria. The cut-off age for late-life depression had to be defined as being between 50 and 70 years; alternatively, correlation coefficients between age and item scores had to be presented. To increase homogeneity we included only studies in which symptoms of depression were measured using the HAM-D and both age groups were compared at the single-item level for the HAM-D-17, HAM-D-21 or HAM-D-24. Furthermore, the HAM-D is the most commonly used observer-rated and validated instrument for rating depression in both younger and older adults. Reference Bagby, Ryder, Schuller and Marshall8 Where articles reported data on overlapping cohorts, the studies with the largest sample size or with the most complete information were included.
Mean scores and standard deviations as well as frequencies of the 17 items of the HAM-D-17 for all HAM-D scales, mean total HAM-D scores (and standard deviations) and numbers of participants were extracted from the articles. From studies reporting frequencies of high- or low-severity scores on individual HAM-D items as well as presence of the item, the frequency of any presence at all was extracted. Correlations were extracted when articles provided only correlations between age and single-item scores. When only subsets of the 17 HAM-D items were presented, the authors of more recent studies (published after 1995) were contacted and requested to provide missing data. Where mean scores or correlations were presented separately for men and women or for early-onset and late-onset late-life depression, these were transformed into one weighted combined mean score (s.d.) or correlation coefficients using appropriate formulae.
Quality assessment
Quality assessment of observational studies in meta-analyses is not usual and there is no consensus regarding the method used. Reference Mallen, Peat and Croft9,Reference Sanderson, Tatt and Higgins10 In our study the quality of the included studies was assessed by two authors (J.H., E.G.) using a checklist with the following five criteria:
-
(a) both age groups were selected from the same source population;
-
(b) population characteristics and inclusion and exclusion criteria were described;
-
(c) (semi)structured diagnostic instruments were used;
-
(d) difference in overall disease severity between younger and older patients controlled for, or no statistically significant difference in depression severity reported;
-
(e) a complete set of 17 HAM-D items was usable or transformable for meta-analysis.
For two criteria weighting was applied, resulting in quality criteria (a) through (c) being coded as 0 or 1 and criteria (d) and (e) as 0, 1 or 2 points, and these criteria were summed to yield a score ranging from 0 to 8 points. If no information was provided as to whether a specific quality criterion was met, it was coded as 0. The cut-off for high or low quality was defined at a score of 5 or more, based on the 60% cut-off point commonly used in quality assessments. Reference Luppino, de Wit, Bouvy, Stijnen, Cuijpers and Penninx11 Discrepancies between the reviewers were resolved through discussion (J.H., E.G.).
Statistical analysis
Data management, calculation of effect sizes and quantitative data synthesis were performed using the Comprehensive Meta-Analysis software version 2.0.021 for Windows (www.meta-analysis.com). Odds ratios were calculated for each HAM-D-17 item separately and then used for all mean comparisons. A higher odds ratio means that the particular HAM-D item showed higher prevalence rates and/or greater severity in older v. younger patients. Because considerable heterogeneity was expected, all analyses were performed with the random-effects model that reduces the risk of a type 1 error (as fixed models typically result in narrower confidence intervals). To assess heterogeneity between the studies we calculated the I 2, which is an indicator of heterogeneity in percentages, and used a value of 50% or over to indicate meaningful heterogeneity. Reference Higgins, Thompson, Deeks and Altman12 In addition, Q statistics were calculated. A statistically significant Q rejects the null hypothesis of homogeneity and indicates a heterogeneous distribution of effect sizes between studies, meaning that systematic differences, possibly influencing the results, are present. For each HAM-D-17 item two summary estimates were calculated: an estimate based on all studies with usable data (see Fig. 2); and an estimate based on the studies with a quality score of ≥5 points, to estimate the effect of bias and potential confounding. A P-value below 0.01 was considered statistically significant, because of multiple testing for every HAM-D item.
Results
The search yielded 3037 articles, including 2200 in PubMed, 773 in Embase, 53 in PsycINFO and 11 hand-searched articles. Exclusion of duplicates and irrelevant references after a first screening of the titles and abstracts left 129 potentially relevant articles for further evaluation (Fig. 1). Most articles were excluded because they did not report the outcome of interest (65 studies), most comparing the phenomenology of early-onset v. late-onset late-life depression (20 studies) or examining neurocognitive function rather than depressive symptoms in relation to age (14 studies). Of the 23 excluded articles not concerning a diagnosis of major depression, 21 reported on depressive symptoms, one reported on minor depression and one on dysthymic disorder. Finally, 11 articles were included in this meta-analysis comparing early and late-life major depression. Because some articles did not present all individual items of the HAM-D, three sets of authors were contacted. Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13-Reference Shahpesandy16 In one case we received data on the unreported HAM-D items. Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13 In the second case the authors were also asked whether two different articles presented data on the same study population. Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14,Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15 Although our question was not answered we extracted the data, choosing the article with the largest study population. As the HAM-D items ‘weight loss’ and ‘anxiety’ were not presented in this larger study, we extracted these data from the article with the smaller sample size. Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14,Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15 Data from a third article by this group were also included in this meta-analysis because the study population was without doubt a different group. Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17 In the third case, the author was unobtainable for further information concerning not reported or not transformable HAM-D scores and methodological issues. Reference Shahpesandy16 For this latter article, Z scores and P-value statistics were used for the reported HAM-D items.
Late-life v. early-life depression
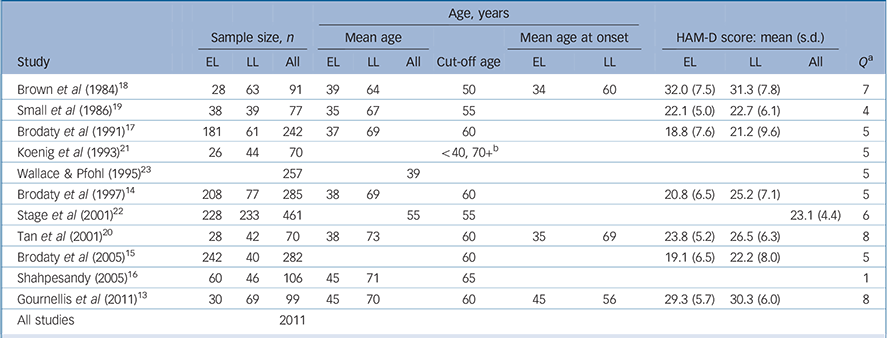
The characteristics of the included studies are shown in online Table DS1 and summarised in Table 1; the total number of

Fig. 1 Flow chart of study selection (HAM-D, Hamilton Rating Scale for Depression).
TABLE 1 Characteristics of the 11 included studies
| Age, years | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Sample size, n | Mean age | Mean age at onset | HAM-D score: mean (s.d.) | ||||||||||
| Study | EL | LL | All | EL | LL | All | Cut-off age | EL | LL | EL | LL | All | Q a |
| Brown et al (1984) Reference Brown, Sweeney, Loutsch, Kocsis and Frances18 | 28 | 63 | 91 | 39 | 64 | 50 | 34 | 60 | 32.0 (7.5) | 31.3 (7.8) | 7 | ||
| Small et al (1986) Reference Small, Komanduri, Gitlin and Jarvik19 | 38 | 39 | 77 | 35 | 67 | 55 | 22.1 (5.0) | 22.7 (6.1) | 4 | ||||
| Brodaty et al (1991) Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17 | 181 | 61 | 242 | 37 | 69 | 60 | 18.8 (7.6) | 21.2 (9.6) | 5 | ||||
| Koenig et al (1993) Reference Koenig, Cohen, Blazer, Krishnan and Sibert21 | 26 | 44 | 70 | <40, 70+ b | 5 | ||||||||
| Wallace & Pfohl (1995) Reference Wallace and Pfohl23 | 257 | 39 | 5 | ||||||||||
| Brodaty et al (1997) Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14 | 208 | 77 | 285 | 38 | 69 | 60 | 20.8 (6.5) | 25.2 (7.1) | 5 | ||||
| Stage et al (2001) Reference Stage, Bech, Kragh-Sorensen, Nair and Katona22 | 228 | 233 | 461 | 55 | 55 | 23.1 (4.4) | 6 | ||||||
| Tan et al (2001) Reference Tan, Ng, Tan, Roy, Brodaty and Parker20 | 28 | 42 | 70 | 38 | 73 | 60 | 35 | 69 | 23.8 (5.2) | 26.5 (6.3) | 8 | ||
| Brodaty et al (2005) Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15 | 242 | 40 | 282 | 60 | 19.1 (6.5) | 22.2 (8.0) | 5 | ||||||
| Shahpesandy (2005) Reference Shahpesandy16 | 60 | 46 | 106 | 45 | 71 | 65 | 1 | ||||||
| Gournellis et al (2011) Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13 | 30 | 69 | 99 | 45 | 70 | 60 | 45 | 56 | 29.3 (5.7) | 30.3 (6.0) | 8 | ||
| All studies | 2011 | ||||||||||||
EL, early-life depression; HAM-D, Hamilton Rating Scale for Depression; LL, late-life depression, NR, not reported.
a Quality assessment score.
b Participants were aged <40 or >70 years.
participants was 2011. On average, older patients had significantly more severe depression (seven studies with standardised difference in means 0.33, 95% CI 0.13-0.52; P = 0.001). Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13-Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15,Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17-Reference Tan, Ng, Tan, Roy, Brodaty and Parker20 However, four studies did not report the overall HAM-D severity scores for older and younger patients. Reference Shahpesandy16,Reference Koenig, Cohen, Blazer, Krishnan and Sibert21-Reference Wallace and Pfohl23 In fact, depression severity was particularly greater in older patients in the three studies by Brodaty et al. Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14,Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15,Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17 Apart from this, another study included a population with psychotic depression only, Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13 in which both age groups were severely affected. Small et al reported only on guilt. Reference Small, Komanduri, Gitlin and Jarvik19 With regard to quality assessment we rated nine articles as being of high quality, Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13-Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15,Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17,Reference Brown, Sweeney, Loutsch, Kocsis and Frances18,Reference Tan, Ng, Tan, Roy, Brodaty and Parker20-Reference Wallace and Pfohl23 and two articles as being of lower quality. Reference Shahpesandy16,Reference Small, Komanduri, Gitlin and Jarvik19

Fig. 2 Forest plot of overall odds ratios (and their 95% confidence intervals as the extremes of the diamonds) comparing early-life and late-life occurrence of every item of the 17-item Hamilton Rating Scale for Depression (HAM-D-17). Darker blue diamonds indicate the items are more prevalent and/or severe in younger patients, and the lighter blue diamonds that the items are more prevalent and/or severe in older patients.
Figure 2 presents the pooled odds ratios for the relation between age and symptoms of depression according to the HAM-D-17. Random effect modelling, with a 95% confidence interval and P<0.01, showed that older people with major depression, compared with younger people, demonstrated more agitation (OR = 1.84, 95% CI 1.39-4.45, P<0.001), general somatic symptoms (OR = 2.01, 95% CI 1.38-2.92, P<0.001), gastrointestinal somatic symptoms (OR = 1.58, 95% CI 1.27-1.97, P<0.001) and hypochondriasis (OR = 3.13, 95% CI 2.24-4.38, P<0.001), but less guilt (OR = 0.52, 95% CI 0.42-0.65, P<0.001) and less loss of sexual interest (OR = 0.51, 95% CI 0.37-0.70, P<0.001) (Fig. 3). A sensitivity analysis of the nine articles of high

Fig. 3 Forest plot for the six statistically significant items of the 17-item Hamilton Rating Scale for Depression (HAM-D-17) for the comparison between early-life and late-life depression (P<0.01).
quality revealed that the significant differences persisted for all six HAM-D-17 items. Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13-Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15,Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17,Reference Brown, Sweeney, Loutsch, Kocsis and Frances18,Reference Tan, Ng, Tan, Roy, Brodaty and Parker20-Reference Wallace and Pfohl23 Another sensitivity analysis excluding studies with more severe depression in older people v. younger people revealed similar results. Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14,Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15,Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17 Again, removing the study with patients with psychotic depression only did not notably affect the sizes of the odds ratios, Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13 although these were no longer significant for loss of sexual interest and general and gastrointestinal somatic symptoms.
Heterogeneity between studies was not significant for the items agitation (Q = 6.44, P = 0.26), gastrointestinal somatic symptoms (Q = 5.17, P = 0.52), guilt (Q = 8.10, P = 0.43) and loss of sexual interest (Q = 10.12; P = 0.12), suggesting a homogeneous distribution of effect sizes between the studies. However, for the items hypochondriasis (Q = 17.90; P = 0.02) and general somatic symptoms (Q = 13.17; P = 0.04) the I value was just above 50%, which has a minor effect as we used random-effect models. No study was identified as a consistent outlier for most of the 17 HAM-D items.
Discussion
The results of this meta-analysis show a partly different phenomenology of late-life depression compared with early-life depression. Older people with major depression demonstrated more agitation, general and gastrointestinal somatic symptoms and hypochondriasis, but less guilt and less loss of sexual interest, compared with younger people with major depression. The difference between the two groups did not reach statistical significance for late insomnia, somatic anxiety and suicidality, which might be due to the small numbers of participants (type 2 error). In general, these results indicate that major depression in older people may have a more somatic presentation, whereas feelings of guilt and loss of sexual function may be symptoms that are more specific for depression at a younger age.
Our results are largely consistent with some earlier studies examining this subject in a different way from comparison at the HAM-D single-item level. For example, older people with major depression were found to be more likely to have somatic symptoms and less likely to have guilt, suicidal and cognitive symptoms. Reference Balsis and Cully24 Another study found that older people were more likely to have agitation and late insomnia, Reference Garvey and Schaffer25 whereas younger people were more likely to have increased appetite, weight gain and decreased libido. Similarly, in a study examining exclusively psychotic depression, Reference Reischies, von Spiess and Stieglitz26 an increase of agitation and a decrease of suicidality and guilt was found in old age compared with younger age. Husain et al used the 30-item Inventory of Depressive Symptomatology - Clinician Rated and found clinically meaningful differences. Reference Husain, Rush, Sackeim, Wisniewski, McClintock and Craven27 In their study older people with non-psychotic major depression had more gastrointestinal symptoms and middle and late insomnia, less irritability and hypersomnia, and were less likely to hold negative cognitions of the self or the future. Others, however, found no difference in the phenomenology of late-life and early-life depression. Reference Musetti, Perugi, Soriani, Rossi, Cassano and Akiskal28-Reference Wesner and Winokur30 For instance, no difference in symptoms of major depression was found in an in-patient psychiatric population using the Duke Depression Evaluation Schedule for the Elderly. Reference Blazer, Bachar and Hughes31 In addition, Corruble et al, Reference Corruble, Gorwood and Falissard32 using the Montgomery-Åsberg Depression Rating Scale, found similar results in a comparison of the phenomenology of major depression at age ≥60 years v. <60 years. In a sensitivity analysis we added the seven items that roughly corresponded to the HAM-D items, which did not lead to different conclusions (data not shown). In three reviews without quantitative data analysis it was argued that no clinically relevant difference was found. Reference Baldwin, Jacoby, Oppenheimer, Dening and Thomas5-Reference Kok7 However, although the studies in these earlier narrative reviews almost overlapped with our studies, some recent articles were not included. Also, these differences in interpretation may relate to the advantages of a meta-analysis over a narrative review that is more prone to subjectivity and bias. Remarkably, in contrast to earlier studies, we did not find differences between older and younger age groups in the HAM-D items loss of insight, work and activity, and psychomotor retardation, which are closely related to the concept of apathy. Reference Hyett, Parker, Proudfoot and Fletcher33-Reference Newmann, Engel and Jensen35 Also, in spite of what has been suggested by others, Reference Baldwin, Jacoby, Oppenheimer, Dening and Thomas5,Reference Gatz and Hurwicz36,Reference Gurland37 no difference was found in depressed mood.
The question arises whether age-related factors modify the presentation of depression or just lead to overlap of somatic symptoms of depression and medical illness, both complicating the diagnosis of late-life depression. For example, not only decrease of sexual desire and sexual function with ageing, but also the lack of a living partner, might explain our finding that older patients had less sexual dysfunction caused by depression compared with younger patients. Reference Bouwman, Jacoby, Oppenheimer, Dening and Thomas38 The expression of more somatic symptoms and less guilt in older patients might be explained by the tendency of the current cohort of older people to express somatic instead of psychological complaints. Reference Wetherell, Petkus, McChesney, Stein, Judd and Rockwell39 Alternatively, it might be that the phenomenology of late-life depression is related to specific risk factors; for instance, in the oldest old people, psychomotor retardation and loss of energy were associated with vascular or neurodegenerative risk factors, whereas symptoms such as thoughts of death, as well as sleep and appetite disturbances, were more strongly related to an inflammatory risk factor. Reference Naarding, Schoevers, Janzing, Jonker, Koudstaal and Beekman40 However, another study on this subject reported conflicting results. Reference Naarding, Tiemeier, Breteler, Schoevers, Jonker and Koudstaal41 Besides, it is difficult to distinguish apathy and cognitive impairment as distinct clinical entities from depression at old age because of overlap of symptoms. Again, it follows that depression may have been overestimated in these studies, suggesting a different phenomenology based on wrong assumptions. Reference Newson, Hek, Luijendijk, Hofman, Witteman and Tiemeier42,Reference Van der Mast, Vinkers, Stek, Bek, Westendorp and Gussekloo43
Several methods have been proposed to resolve the issue of overlap of somatic symptoms of depression and physical illness, complicating the diagnosis of late-life depression. For example, in an inclusive approach all somatic symptoms are included regardless of being primarily due to a medical illness, whereas in an exclusive approach somatic symptoms of depression are excluded and only psychological symptoms are counted for a diagnosis of depression. Next, in an aetiological approach a somatic symptom is only counted if not caused by a medical illness and in a substitutive approach the somatic symptoms are replaced by non-somatic alternatives. Reference Koenig, George, Peterson and Pieper44 Although the HAM-D-17 has been criticised for use in patients with physical illness on the grounds that it includes too many somatic items, the use of this scale is even justified to diagnose post-stroke depression and depression in Parkinson's disease. Reference De Coster, Leentjens, Lodder and Verhey45,Reference Leentjens, Verhey, Lousberg, Spitsbergen and Wilmink46 Moreover, some somatic symptoms were highly sensitive for post-stroke depression. Reference De Coster, Leentjens, Lodder and Verhey45
Strengths and limitations
Our study has some limitations. First, older patients had on average a higher level of severity of depression than the younger patients, which may account for the slightly different phenomenology in older patients. Although statistically significant, these differences in depression severity were small and therefore not regarded as clinically relevant. In addition, sensitivity analysis excluding studies with significantly more severe depression in older people revealed similar results, Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14,Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15,Reference Brodaty, Peters, Boyce, Hickie, Parker and Mitchell17 suggesting that our results are unlikely to be explained by differences in depression severity. Alternatively, overlapping somatic symptoms of depression and comorbid age-related physical disorders may explain the higher scores on depression severity scales in the older population. Second, we could not adjust for comorbid physical disorders in older v. younger people. Lack of this information means that we cannot be certain whether our findings are related to somatic comorbidity. In fact, all but one study included in-patients, and perhaps older patients with a more somatic presentation were admitted to hospital more often than younger depressed patients in order to exclude an underlying somatic illness. In previous studies, however, differences in the phenomenology of major depression persisted after adjustment for somatic comorbidity. Reference Koenig, Cohen, Blazer, Krishnan and Sibert21,Reference Husain, Rush, Sackeim, Wisniewski, McClintock and Craven27 One of these studies was included in our meta-analysis and used an inclusive approach for rating HAM-D items. Reference Koenig, Cohen, Blazer, Krishnan and Sibert21 Third, as studies mainly reported on in-patients it follows that generalisation of our findings to an out-patient or general population is limited. Fourth, a conceptual limitation is the use of strict RDC, DSM and ICD diagnostic criteria for major depression and the HAM-D. Obviously, if distinctive features of late-life depression indeed exist, they would be missed if not included in the HAM-D. Moreover, if depression in older people presents with many symptoms that differ from the DSM or ICD criteria, then these patients might not be diagnosed as having depression and would not have been included in these studies. Finally, this meta-analysis focused on comparing depression at older and younger age, irrespective of age at first onset. It follows that we did not address the question of whether the age at onset of the first depressive episode is related to a specific symptom profile of early- or late-onset late-life depression. However, the studies of Gournellis et al and Brodaty et al compared both early v. late-life depression and early onset v. late onset in late-life depression. Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13-Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15 Gournellis et al found differences related to both age at onset and current age in which the group of older patients with early-onset depression had an in-between position concerning the extent of differences in hypochondrial ideation and gastrointestinal symptoms compared with a group of older patients with late-onset depression and a group of younger patients with early-onset depression. Reference Gournellis, Oulis, Rizos, Chourdaki, Gouzaris and Lykouras13 In the studies by Brodaty et al differences were found related to current age only, but not for age at onset. Reference Brodaty, Luscombe, Parker, Wilhelm, Hickie and Austin14,Reference Brodaty, Cullen, Thompson, Mitchell, Parker and Wilhelm15 Furthermore, as late-life depression probably encompasses patients with recurrent depressive episodes and treatment-refractory depression, it is possible that differences in phenomenology between late-life and early-life depression might be more marked when studies include only patients with first depressive episodes. Ideally, these would be prospective cohort studies because recall bias of age at onset is one of the problems of such studies. Reference Lyness, Pearson, Lebowitz and Kupfer47 However, older patients with recurrent depressive episodes might also have a ‘new onset’ distinctive depressive episode, for example related to (vascular) changes in the ageing brain.
Strengths of this meta-analysis include the thorough search resulting in over 2000 participants from 11 studies, the quality of the review process and the consistent findings across studies with generally low heterogeneity. Moreover, we are not aware of previous meta-analyses examining the relation between age and the phenomenology of major depression.
Clinical implications
In summary, the results of this study suggest only in part a different phenomenology of major depression in older people compared with younger adult patients. These findings are relevant for clinical practice, because we should be aware that major depression in older people may present in a more somatic way. This may help our understanding of the phenomenology of late-life depression related to certain risk factors and age at onset, in order to improve recognition and early detection, and refine prevention and treatment of depression in older people.







eLetters
No eLetters have been published for this article.