The Wernicke-Korsakoff syndrome is a serious neuropsychiatric consequence of dietary deficiency, most commonly caused by heavy alcohol consumption. Wernicke's encephalopathy is classically a disorder of acute onset characterised by nystagmus, abducent and conjugate gaze palsies, ataxia of gait, and a global confusional state, occurring together or in various combinations. It is due to deficiency of the B vitamin thiamine (vitamin B1), and was first described by Carl Wernicke in 1881. Sergei Korsakoff gave the first comprehensive account of the amnestic syndrome now known as Korsakoff psychosis in 1887. He described a range of features including delirium, but the disorder came to be characterised by recent memory loss with confabulation but with relative preservation of other intellectual functions. Wernicke-Korsakoff syndrome is now considered to be a unitary disorder comprising acute Wernicke's encephalopathy which proceeds in some people to Korsakoff psychosis. Reference Victor, Adams, Collins and Davis Company1,Reference Thomson, Cook, Guerrini, Sheedy, Harper and Marshall2
A complicating factor in the assessment of Wernicke's encephalopathy is that in up to 90% of patients the pathology may not be associated with the classical clinical triad of confusion, nystagmus and ataxia. Reference Harper, Giles and Finlay-Jones3 The full triad of symptoms is recognised in just 0.05% of all those admitted to hospital, whereas the whole population prevalence of Wernicke-Korsakoff syndrome based on post-mortem studies in Western countries has been estimated at 1-2%. Reference Torvik4,Reference Harper, Fornes, Duyckaerts, Lecomte and Hauw5 Post-mortem studies of over 25 000 patients in general hospitals from various countries have demonstrated typical lesions of Wernicke's encephalopathy in 1.4% of patients examined, and in those misusing alcohol this figure is as high as 35%. Reference Torvik4-Reference Thomson and Marshall7 Therefore, it has been suggested that a presumptive diagnosis of Wernicke's encephalopathy should be made for any patient with a history of alcohol misuse who may be at risk. This includes anyone showing evidence of ophthalmoplegia, ataxia, acute confusion, memory disturbance, unexplained hypotension, hypothermia, coma or unconsciousness. Reference Cook8 Operational criteria for the diagnosis have been proposed, Reference Caine, Halliday, Kril and Harper9 and although they are not yet widely used, they help in distinguishing the problem from other potentially coexisting conditions such as alcohol withdrawal or hepatic encephalopathy.
Untreated, Wernicke's encephalopathy leads to death in up to 20% of cases Reference Harper, Giles and Finlay-Jones3,Reference Harper10 or Korsakoff psychosis in 85% of the survivors. Up to 25% of the latter require long-term institutionalisation. Reference Victor, Adams, Collins and Davis Company1 Furthermore, the incidence of Korsakoff psychosis has been reported to be rising in some parts of the UK. Reference Ramayya and Jauhar11 For the reasons mentioned earlier, it is probable that Wernicke's encephalopathy is largely underdiagnosed, and so any published incidence and prevalence figures are likely to be a considerable underestimate. Prolonged heavy consumption of alcohol leads to thiamine deficiency by several mechanisms, including the replacement of vitamin-containing foods by alcohol, impaired absorption of thiamine from the gut, impairment of storage by the liver, decreased phosphorylation to thiamine pyrophosphate and excessive requirements for the metabolism of alcohol. Reference Butterworth, Kril and Harper12
A new service for working age adults with cognitive impairment was set up in Birmingham in late 2002, and soon received a series of referrals for patients with alcohol dependence and Wernicke-Korsakoff syndrome. These patients had mostly been treated on acute medical or surgical wards, where the diagnosis had been made but the treatment administered was inadequate in either duration or intensity. We wished to improve levels of knowledge about the syndrome among medical and surgical colleagues, and improve the quality of treatment.
Method
The study took place within the University Hospitals Birmingham National Health Service Foundation Trust, which provides adult services to more than half a million people in Birmingham and specialist services to the wider West Midlands region. As Wernicke-Korsakoff syndrome is commonly missed in routine practice it would have been difficult to assess the prevalence of the condition in all admissions to the Trust's two hospitals, so instead the focus was on patients who had been prescribed a thiamine-containing medicine. These individuals could be readily located using the pharmacy computer system. The project was registered as a clinical audit with the University Hospitals Birmingham audit department.
A data collection form was developed to record potential risk factors for Wernicke-Korsakoff syndrome, using best practice recommendations (summarised in Fig. 1). Reference Cook8,13 An initial audit in May 2003 included all cases identified through computerised pharmacy records where treatment with thiamine or thiamine-containing preparations was prescribed over a period of 6 months (November 2002-April 2003). The case notes were obtained and reviewed, and the risk factors for Wernicke-Korsakoff syndrome and the thiamine treatment regime prescribed were recorded on the form. Treatment was compared with local prescribing guidelines (Fig. 1), themselves based on national recommendations. 13
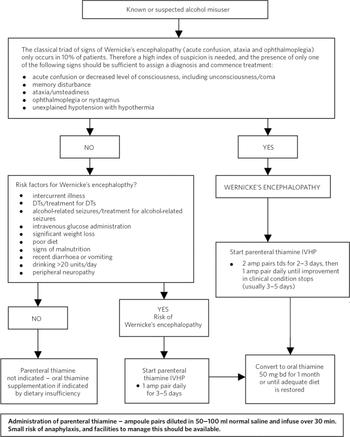
Fig. 1 Treatment flowchart based on local prescribing guidelines DTS, delirium tremens; IVHP, intravenous high potency; tds, three times a day; bd, twice per day; amp, ampoule.
Between May 2003 and April 2004, an intervention was implemented through the hospital pharmacy service to improve the prophylaxis and treatment of Wernicke-Korsakoff syndrome. Each time a thiamine-containing drug was prescribed on the wards the pharmacist gave the prescribing doctor or their team information about best practice in prescribing for the syndrome. Where possible this was done verbally, but in all cases the treatment flowchart (Fig. 1) was attached to the prescription chart. A re-audit was then carried out again exactly a year after the initial audit period (November 2003-April 2004), and the results were compared.
All data were analysed using SPSS version 15.0 for Windows, and differences in continuous variables between the treatment groups were compared by means of independent t-tests for normally distributed continuous variables, Mann-Whitney U-tests for non-normally distributed continuous variables, and χ2-tests for categorical variables; P < 0.05 was considered significant.
Results
Pre-intervention period (November 2002-April 2003)
A total of 201 individuals had received a prescription of either oral or parenteral thiamine. Of these, 148 sets of case notes were obtained and scrutinised (75%). Four cases involved patients with no history of alcohol problems and an alternative cause for thiamine deficiency (e.g. malnutrition secondary to carcinoma), and these individuals were excluded. In the remaining 144 cases, the prescription for thiamine was assumed to be due to alcohol-related deficiency. As shown in Table 1, the majority of the cases were men admitted to hospital as an acute case for non-surgical reasons. Although the routine recording of alcohol consumption and its associated problems was variable, a total of 125 individuals (87%) had a history of alcohol misuse recorded in the case notes.
Table 1 Comparison of cases from two audit periods, pre-intervention and post-intervention

| Pre-intervention N = 144 | Post-intervention N = 195 | Significance | |
|---|---|---|---|
| Audit sample | |||
| Mean age, years (range) | 54.9 (27–93) | 54.1 (20–95) | ns |
| Men, n (%) | 112 (78) | 148 (76) | n |
| Emergency/A&E admissions, n (%) | 116 (84) | 156 (89) | ns |
| Under care of physicians, n (%) | 124 (87) | 157 (81) | ns |
| Under care of surgeons, n (%) | 20 (13) | 38 (19) | ns |
| History of alcohol misuse recorded, n (%) | 125 (87) | 159 (82) | ns |
| Current alcohol consumption recorded, n (%) | 101 (70) | 89 (46) | χ2 = 20.18, d.f. = 1, P < 0.001 |
| Median daily alcohol consumption, units | 14 (n = 101) | 11 (n = 89) | ns |
| Prescribed a benzodiazepine detoxification regime, n (%) | 76 (54) | 88 (47) | ns |
| Thiamine on admission, n (%) | 48 (33) | 53 (27) | ns |
| Risk factors for Wernicke–Korsakoff syndrome recorded in initial assessment, n (%) | |||
| Acute confusion | 48 (33) | 73 (37) | ns |
| Memory disturbance | 28 (19) | 41 (21) | ns |
| Ocular abnormalities | 14 (10) | 10 (5) | ns |
| Ataxia | 21 (15) | 15 (8) | χ2 = 4.14, d.f. = 1, P = 0.04 |
| Unexplained hypotension or hypothermia | 16 (11) | 25 (13) | ns |
| Treatment and prophylaxis, n (%) | |||
| At least one of the risk factors present, therefore needed treatment | 70 (49) | 100 (51) | ns |
| Got adequate treatment | 1 (1) | 10 (5) | χ2 = 5.19, d.f. = 1, P = 0.03 |
| Risk factors present that suggested the need for prophylaxis | 33 (23) | 69 (35) | χ2 = 6.12, d.f. = 1, P = 0.01 |
| Got adequate prophylaxis | 21 (15) | 16 (8) | ns |
| Treatment not required | 41 (28) | 26 (13) | χ2 = 1.19, d.f. = 1, P = 0.001 |
| Route of administration of thiamine, n (%) | |||
| Oral | 87 (60) | 144 (74) | χ2 = 8.47, d.f. = 2, P = 0.02 |
| Intramuscular | 4 (3) | 1 (1) | |
| Intravenous | 53 (37) | 50 (26) | |
| Mean dose of thiamine prescribed on day 1 of treatment, mg | |||
| Oral | 166 | 150 | ns |
| Parenteral | 504 | 697 | U = 1067, P = 0.04 |
In each case the notes were scrutinised for any mention of the five broad sets of features of Wernicke's encephalopathy on initial assessment. Approximately half of the patients had at least one feature and therefore required active treatment for the disorder (the most common was acute confusion/reduced level of consciousness). If none of these features was present, the case notes were examined for risk factors for Wernicke's encephalopathy (Fig. 1). If any of these factors was present, the patient was recorded as requiring prophylaxis with parenteral thiamine.
The next step was to examine the thiamine treatment regime in each patient. Of the 144 individuals, 87 (60%) received thiamine orally, 4 (3%) intramuscularly, and 53 (37%) intravenously. The mean dose was 307 mg per day (s.d. = 266.2, range 0-1500). When considered according to the best practice flowchart, 70 patients required active treatment but only 1 received the recommended regime. A further 33 patients had risk factors for Wernicke's encephalopathy and required prophylactic treatment, but only 21 received it as recommended. Of the 70 patients who required full treatment, 17 merely received a continuation of the dose of oral thiamine that they were taking before admission, and this was also the case for 12 of the 33 patients requiring prophylaxis.
Post-intervention period (November 2003-April 2004)
A total of 263 individuals had received a prescription of either oral or parenteral thiamine in the second time period of the audit cycle, and 200 sets of case notes were examined (76%). Five cases involved patients with no evidence of alcohol problems, and these were excluded from the analysis, leaving 195 in total. There were no statistical differences between the pre- and post-intervention samples in terms of mean age, the proportion of men, the number of emergency admissions and the balance between medical and surgical cases (Table 1). A history of alcohol misuse was also recorded in a similar proportion of notes, but a significantly lower proportion of post-intervention sample had details of current alcohol consumption.
Just over half of the individuals had at least one feature of Wernicke's encephalopathy (acute confusion/reduced level of consciousness was again the most common one), and therefore required active treatment for the disorder. The only significant difference between the samples pre- and post-intervention was a lower rate of ataxia in the post-intervention group. The re-audit showed a small but significantly higher number of cases where patients received adequate treatment for Wernicke's encephalopathy (1 v. 10, χ2 = 5.19, d.f. = 1, P = 0.03). Although the number of patients that required prophylactic treatment with thiamine was higher post-intervention, fewer got adequate prophylactic treatment. The proportion of individuals receiving thiamine intramuscularly or intravenously was lower after the intervention (27%) than before (40%) (χ2 = 6.88, d.f. = 1, P = 0.009), and the mean dose of thiamine prescribed on day 1 also fell. However, there was a significant increase in the prescribed dose of parenteral thiamine as opposed to oral. Of the 100 individuals requiring full treatment, 23 merely had their admission dose of thiamine continued, as did 22 of the 69 individuals judged as requiring prophylaxis.
Discussion
These results suggest that treatment for Wernicke's encephalopathy was rarely in line with expert guidelines in an acute medical setting. All the patients whose case notes were reviewed in this audit (a total of 339 in two audit stages) had a history of alcohol misuse and were prescribed thiamine in hospital, most likely in the form of an oral preparation at a dose of 50-100 mg per day. Symptoms suggestive of Wernicke's encephalopathy were present in approximately half of the cases, and yet only 3% received optimum levels of treatment suggested by expert guidelines. Reference Cook, Hallwood and Thomson6 A further 30% of patients had clinical features suggesting that they were at risk of developing Wernicke's encephalopathy, but only a third of these received thiamine replacement therapy as recommended in the guidelines (i.e. in a parenteral form). Reference Thomson and Marshall7 A third were taking oral thiamine at the point of admission to hospital, and this was continued in over half of these patients despite clinical features suggesting that a different approach was necessary. As we assessed symptoms of Wernicke's encaphalopathy by looking at the case notes, it is possible that these figures underestimate the size of the problem. However, it should be noted that although the guidelines were taken from the best evidence available at the time of the study, this was not based on randomised controlled trials Reference Day, Bentham, Callaghan, Kuruvilla and George14 and so may have been contested by some prescribing doctors.
The pharmacy-led intervention to improve levels of awareness of Wernicke's encephalopathy and its treatment was associated with an increase in the number of patients with likely Wernicke's encephalopathy who were adequately treated. However, at the same time the number of patients prescribed prophylactic treatment decreased. Furthermore, there is no way of determining whether the increased level of prescribing in a small subset of individuals had any positive benefits in terms of improved long-term outcome. The size effect was lower than in a similar study conducted with patients undergoing alcohol detoxification in Edinburgh, Reference McIntosh, Kippen, Hutcheson and McIntosh15 but that sample was selected on the basis of starting an alcohol detoxification rather than being in need of thiamine.
This study is in keeping with other research in acute medical settings that suggests doctors need regular reminders of the importance of taking an alcohol history in all cases, Reference Shepherd, London and Alexander16 and the need to be alert to the possibility of Wernicke-Korsakoff syndrome in chronic heavy drinkers. These two factors are likely to interact: if significant alcohol-related neurotoxicity has occurred by the time of admission to hospital, the outcomes may be limited irrespective of an adequate prescription of thiamine. Reference Thomson and Marshall17 Reasons for inadequate treatment of Wernicke-Korsakoff syndrome have been well documented, and may be based on poor levels of knowledge about the condition. In particular there appeared to be a fundamental misunderstanding about the limited effectiveness of oral preparations of thiamine in individuals with a history of heavy alcohol consumption. Reference Thomson18 There may also continue to be concern over the risks of anaphylaxis associated with parenteral thiamine, despite evidence to suggest that the risks are lower than with other commonly used parenteral medications (e.g. penicillin). Reference Thomson and Cook19 The long-term personal and economic implications of developing Korsakoff psychosis far outweigh these concerns, and the simple, cheap treatment for Wernicke-Korsakoff syndrome is likely to be extremely cost-effective in the longer term.
These results suggest that all acute hospitals should have clear policy on managing alcohol-related problems in general and the prevention and management of Wernicke-Korsakoff syndrome in particular. Although the syndrome is rare in absolute terms, in those with alcohol misuse or dependence the number of cases is not insignificant and the consequences of not treating a patient correctly could be lifelong. Therefore policies alone are not enough and a system for regular education of both junior doctors and more experienced clinicians in the assessment and management of Wernicke-Korsakoff syndrome is important. Reference Shepherd, London and Alexander16 Hospital pharmacy service can have a key role in the monitoring of prescribing guidelines in this area. With the development of electronic prescribing systems, it should be possible to provide a warning message when thiamine is prescribed, alerting the prescriber to best practice guidelines. However, further work is required to clarify the optimum dosing schedule for treatment and prophylaxis of Wernicke-Korsakoff syndrome.





eLetters
No eLetters have been published for this article.