3 results
Expectations in the treatment of delusional disorder: A case report
- A. Fuentes Merlos, C. Arroyo del Val, E. X. González Vivero, L. Núñez Cantos, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S965
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 43 year-old woman that, following the sudden death of his brother in 2015, begins with symptoms of anxiety, irritability and emotional instability, with a tendency to social isolation. Thereafter, she starts the development of persecutory delusions focused on the work and family environment that evolve into inappropriate behaviors to the point of abandoning her professional life.
Objectives(1) We will carry out a complete review about persecutory delusions and its relationship with affective disorders, based on the severity of our patient’s case.
(2) We will study the different lines of treatment in delusional disorder (DD) and its course and prognosis in relation to the intervention performed.
MethodsA review of the patient’s history will be conducted, taking into account her biography, clinical evolution and response to the treatments received.
Likewise, a bibliographic review of the available scientific literature in relation to DD treatment strategies will be carried out.
Results(1) DD is more common in middle-aged women. People who tend to be socially isolated are more likely to develop DD.
(2) Acute onset, in young women with identifiable precipitating factors, suggests a better prognosis.
(3) In the long term, 50% of patients recover and a further 20% experience some improvement.
(4) The combination of antipsychotic medications and psychological therapies such as cognitive behavioral therapy (CBT) is fundamental in the management of DD patients.
ConclusionsThe prognosis for patients with DD varies depending on various factors, including the type and severity of the delusional ideas, and their own life circumstances. It is often possible to eliminate the behavioral alterations derived from the DD, allowing the patient to function normally. However, delusions often persist and become encapsulated.
Disclosure of InterestNone Declared
Cyclothymia, bipolar disorder and multiple sclerosis: A case report
- M. D. P. Paz Otero, E. Lozano Bori, J. Sánchez Rodríguez, S. Puyal González, M. Fernández Fariña, F. Mayor Sanabria, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S703-S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 49-year-old woman who was diagnosed with multiple sclerosis at the age of 19 and suffers from an affective disorder that has been evolving for years. This condition, for which she has been followed by psychiatry and psychology for more than ten years, consists of alternating periods of hypomania lasting weeks and phases in which frank depressive symptomatology predominates, with no phases of euthymia in between and with a predominance of severe deterioration of her functionality at both poles.
Objectives(1) We will review the term cyclothymia and explore the concept of “cyclothymic temperament” advocated by some authors, in order to be able to understand the dimension of the present case and reformulate its approach.
(2) The relationship between multiple sclerosis and bipolar spectrum disorders will be covered, reviewing the current knowledge in this regard and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, taking into account her life history, the complementary tests performed as well as the multiple therapeutic approaches tried over the last few years.
Likewise, a bibliographic review of the available scientific literature will be carried out in relation to the diagnosis of cyclothymia or bipolar disorder type II, the controversial term “cyclothymic temperament”, and the relationship that these diagnoses have with the diagnosis of Multiple Sclerosis.
Results(1) Our patient could fit into what many authors define as a cyclothymic temperament, fulfilling, in certain episodes, the criteria that the manuals propose for bipolar disorder type II.
(2) 2.1 The prevalence of bipolar affective disorder in MS is approximately twice as high as in the general population (rates of 0.3-2.4%). 2.2 Patients with MS have higher scores in cyclothymic and hyperthymic temperament than the control group. 2.3 Certain drugs generally used in BD also seem to have a beneficial effect on MS.
Image:
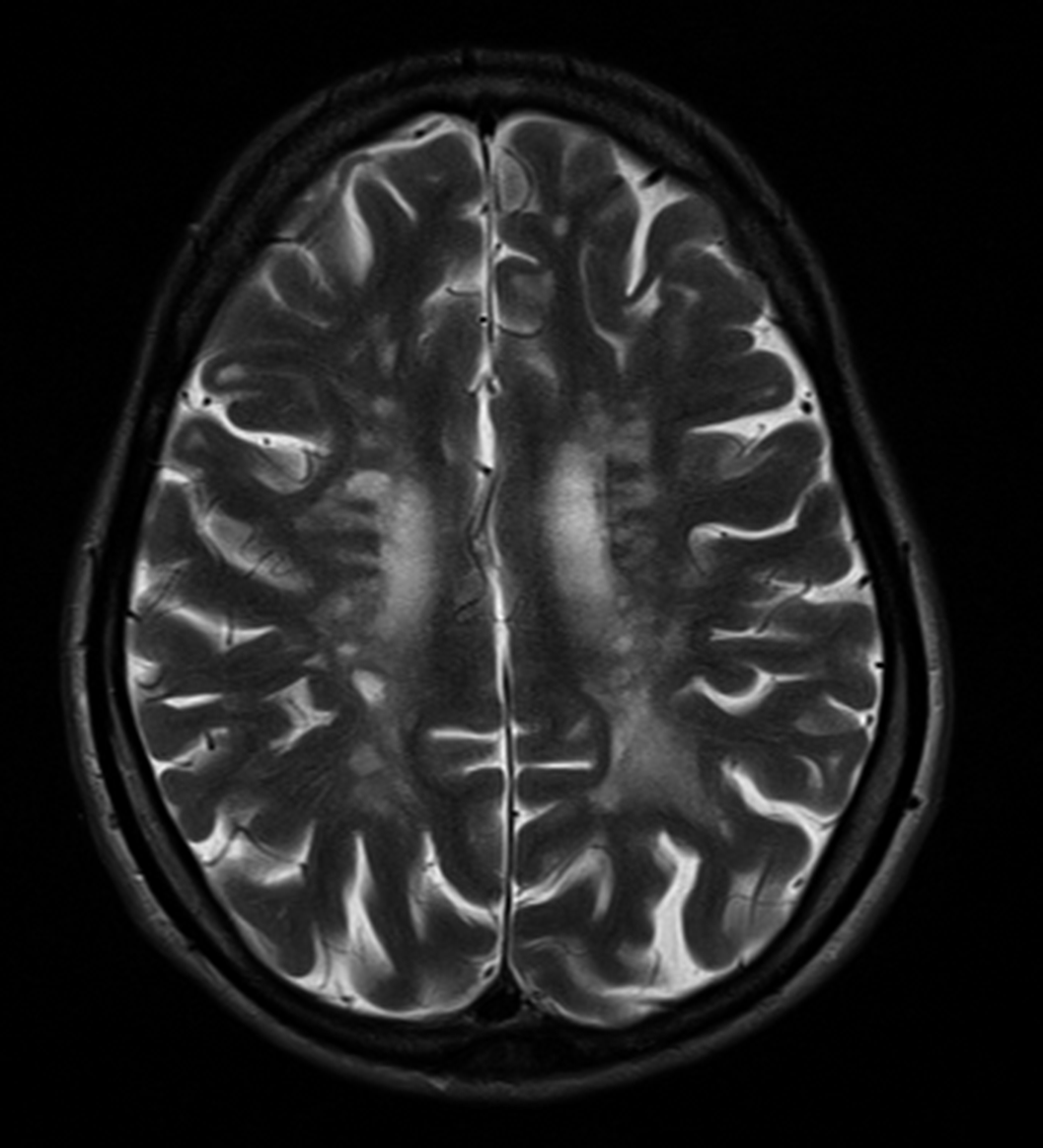
Image 2:
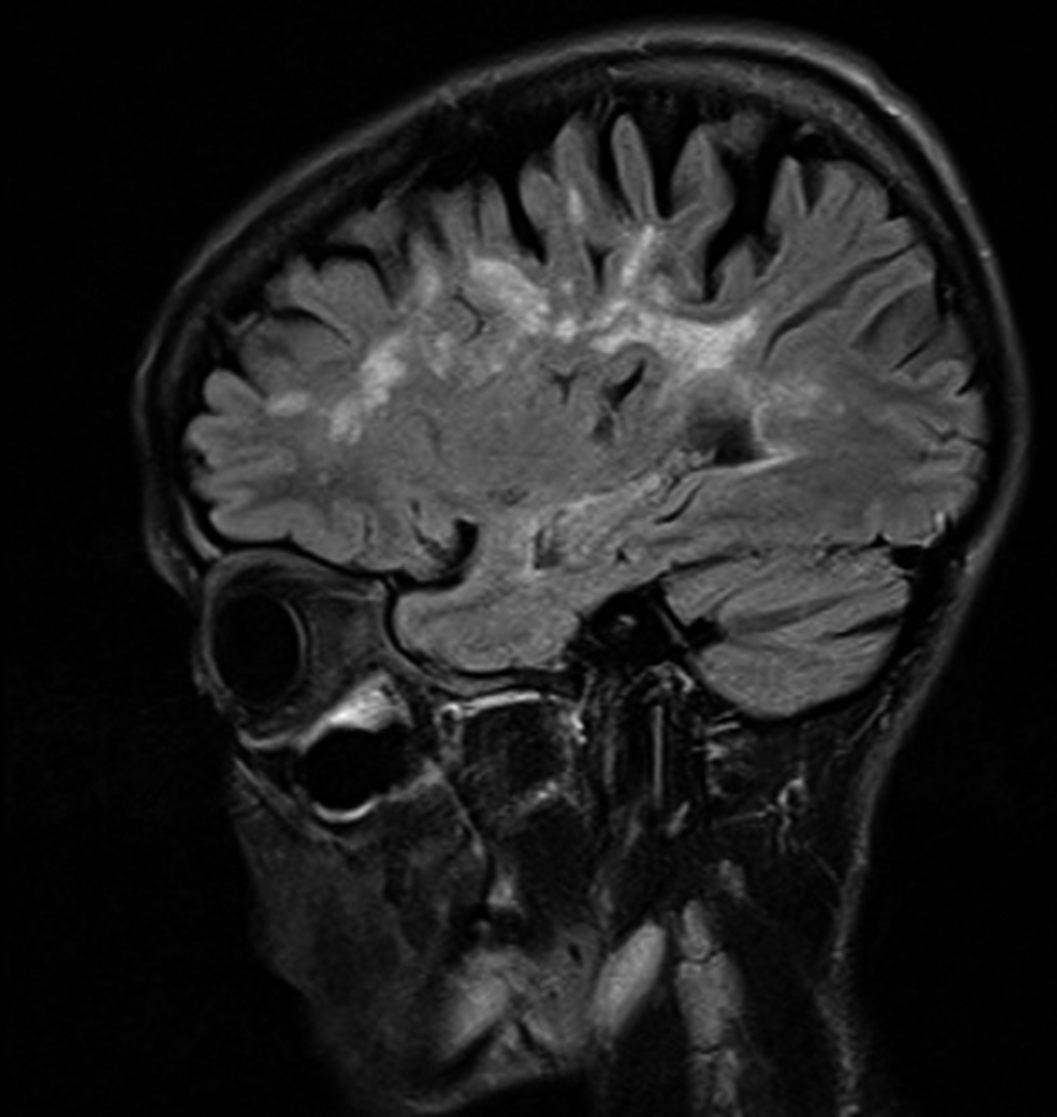 Conclusions
ConclusionsThe reformulation of the concept of cyclothymia would allow us to recognize in our patient a basic temperament of long evolution that would be the substrate on which different factors have subsequently influenced, such as antidepressant drugs or multiple sclerosis. In addition, it is necessary to know the association between BD and MS, in order to be able to offer an adequate treatment, contemplating some pharmacological options such as Lithium or some Atypical Antipsychotics, given the beneficial effect both for the affective disorder and for the neurological process.
Disclosure of InterestNone Declared
Psychiatric comorbidity in epilepsy and difficulties in treatment: A case report
- M. Fernández Fariña, F. Mayor Sanabria, C. Regueiro Martín-Albo, M.E. Expósito Durán, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S462
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 36-year-old male with depressive states, impulsive traits and fits of anger (including episodes of self and heteroagressiveness) since early childhood, in the context of traumatic family history and the beginning of an epileptic disease. These symptoms have been maintained over the years, in addition to other variable and recurrent symptoms, such as severe anxiety, somatizations or serious depressive symptoms.
ObjectivesTo highlight the possible influence of epilepsy in the course of mental illnesses, especially depression, as well as the increased difficulty in management.
MethodsWe collected the complete medical history of a patient with an important history of mental health in addition to epileptic disease since childhood and we carried out a review of the comorbidity between these diseases and their treatment.
ResultsThe epileptic disease of our patient may have influenced the behavioural alterations and the depressive symptoms since childhood, as well as the personality traits with aggressiveness and impulsiveness. There is an added difficulty in treating this case given the possible interactions between antiepileptic and antidepressant medications.
ConclusionsThis case highlights the importance of taking into account the influence of this comorbidity on the prognosis of patients. Knowing the interactions and side effects of drugs is essential for good clinical management.
DisclosureNo significant relationships.





