3 results
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
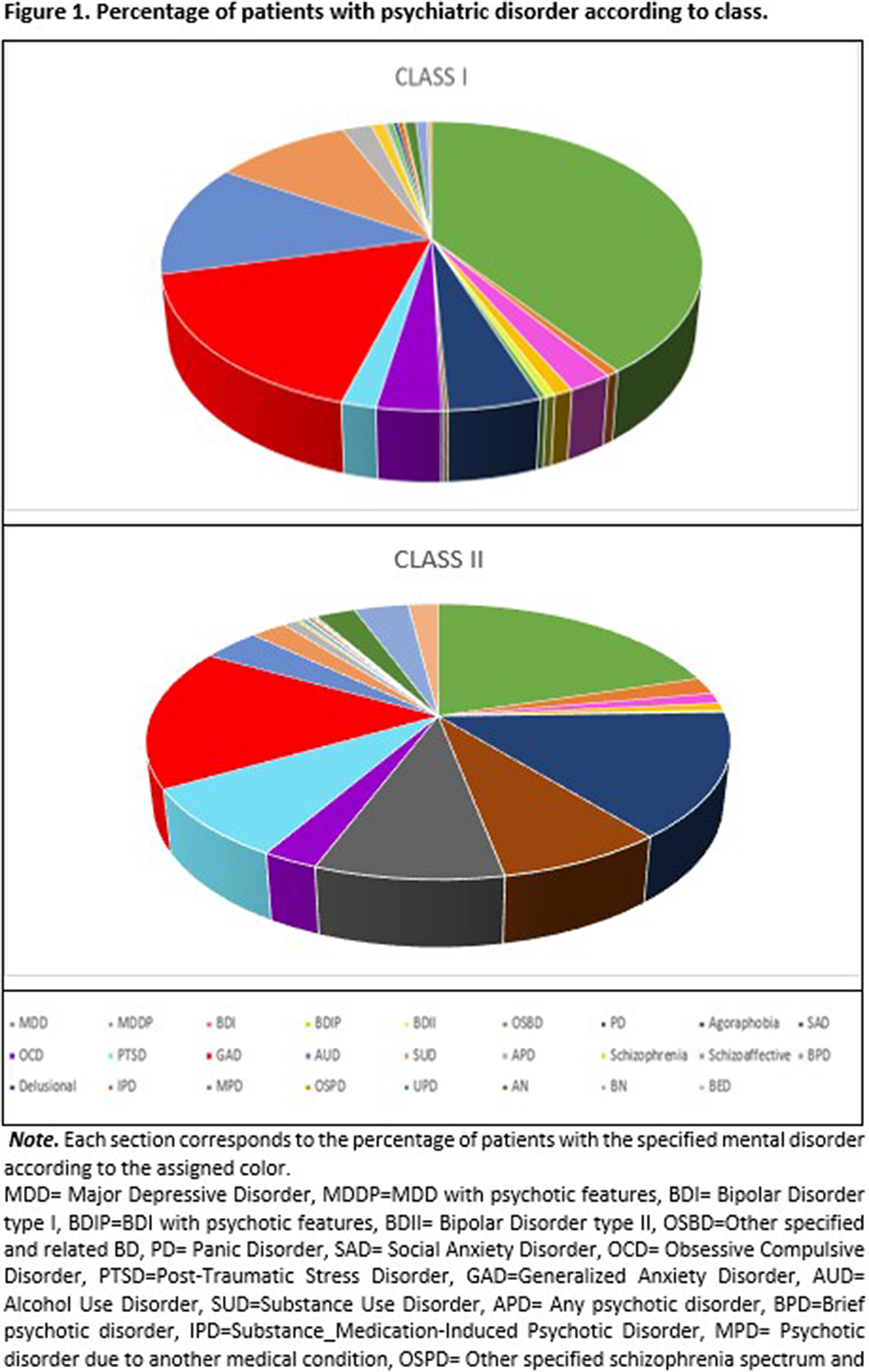 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
Study of mentalizing ability in borderline personality disorder: relationship with impulsivity
- A. Galvez-Merlin, P. de la Higuera-Gonzalez, J. M. Lopez-Villatoro, A. de la Torre-Luque, M. Diaz-Marsa, J. L. Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S114
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Borderline personality disorder (BPD) is a severe mental disorder characterized by affective, behavioral and relational instability, along with interpersonal hypersensitivity and unstable affective relationships (APA 2013). Poor interpersonal functioning could be associated with critical deficits in the ability to mentalize in these patients, together with high levels of impulsivity. Although most studies have described hypermentalization deficits among BPD patients (Bora Psychol Med 2021;51 2541-2551), existing literature is still scarce on this aspect, as well as its relationship with the impulsive behavior.
Objectives1) to assess specific mentalizing deficits in BPD compared to healthy controls in a complex ecological mentalization task; 2) evaluate the relationship between mentalization and impulsivity in BPD.
Methods63 patients diagnosed with borderline personality disorder and 31 control subjects were studied using the Movie for the Assessment of Social Cognition -MASC- (Dziobeck et al. J Autism Dev Disord 2006; 36 623-636) and the Barratt Impulsivity Scale -BIS-11- (Patton et al. J Clin Psychol 1995; 51 768-774), as well as other sociodemographic and clinical factors. The clinical research study was approved by the Clinical Research Ethics Committee of the Hospital Clínico San Carlos (Madrid, Spain).
ResultsThe results showed significant differences in the scores related to correct mentalization, hypomentalization, and non-mentalizing responses between patients and controls, with BPD patients showing worse performance. A significant negative relationship was also observed between impulsivity scores and correct mentalizing responses in BPD patients.
ConclusionsThe results showed a deficit in the ability to mentalize in BPD patients, compared to control subjects, characterized by a hypomentalization and an absence of mentalization. Likewise, this deficit in mentalization ability was related to greater impulsive behavior in patients. These results would be consistent with the hyperarousal hypothesis in BPD, which would reduce inhibitory control, causing mentalization deficits (Euler et al. J Pers Disord. 2021; 35 177-193). Future studies will try to associate specific impulsive behaviors associated with the characteristics of hypomentalization and absence of mentalization observed in our results.
Disclosure of InterestNone Declared
Assessment of Theory of Mind in Psychopathology: a Scoping Review
- P. de la Higuera-Gonzalez, A. Galvez-Merlin, E. Rodríguez-Toscano, J. Andreo-Jover, T. Lopez-Soto, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1001-S1002
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Theory of Mind (ToM) is defined as the cognitive ability that infers other’s mental states (Premack & Woodruff. J Behav Brain Sci 1978; 1 515-526).The interest in the study of ToM distinguishing its affective and cognitive components has been growing. Its study in psychopathology has been evolved from its original studies in autism spectrum disorders (ASD), schizophrenia (SCZ) and, borderline personality disorder (BPD), to other mental disorders like major depressive disorder (MDD), bipolar disorder (BP), anorexia nervosa (AN) and social anxiety disorder (SAD).
Objectives1) review the most commonly used instruments for ToM assessment; 2) to compile the evidence on ToM deficits across mental disorders. For both objectives, target disorders are previously mentioned.
MethodsThe search was carried out on the PubMed, PsycInfo and Scopus databases, using the terms “Theory of mind”, “Mentalization” and the previously mentioned mental disorders and pertinent thesaurus. Articles in English, published since 2010 were considered. A 2-step strategy (first, article screening and full reading) was followed to select articles of interest.
ResultsReading the Mind in the Eyes (Baron-Cohen et al., J Child Psychol Psychiatry 2001; 42 241-251) and Movie for the Assessment of Social Cognition (Dziobeck et al. J Autism Dev Disord 2006; 36 623-636) were the most commonly used tasks to assess ToM. Regarding mental disorders, studies showed deficits in cognitive and affective ToM skills in ASD, SCZ, BPD, MDD and BP. Hypomentalization was mainly observed in ASD and MDD, while BPD and SCZ were featured by errors associated with hypermentalization. Studies in AN and SAD are scarce, but they mainly highlight a cognitive ToM deficit, with hypomentalization in AN and hypermentalization in ASD. In all of them, depressive symptomatology seems to be a critical moderator of ToM performance.
ConclusionsAlthough ToM impairments are well described for some mental disorders, more research is needed to reach solid conclusions for others. The use of different and heterogeneous ToM assessment instruments can strongly influence the results of studies. The study of ToM is essential to gain a better understanding of the diseases and to develop effective treatments targeting specific ToM deficits.
Disclosure of InterestNone Declared




