213 results
New-Onset Bipolar Disorder in Late Life: a case report and review of literature
- A. Sanz Giancola, E. Arroyo Sánchez, P. Setién Preciados, M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S691
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The elderly represents the fastest growing group of the population. It is fair to assume that the portion of old age patients suffering from bipolar disorder will grow in a similar manner. Elderly patients represent approximately 25% of the bipolar population. Summarizing, 5–10% of patients were 50 years of age when they experienced their first manic episode, constituting the subgroup of late onset bipolar disorder (LOBD).
ObjectivesThe purpose of this case report and literature review is to emphasise the importance of LOBD in old population and to highlight its still sparse-knowledge.
MethodsDescriptive case study and review of literature (Arnold,I. et al. Old Age Bipolar Disorder—Epidemiology, Aetiology and Treatment. Medicina 2021,57,587; Baldessarini et al. Onset-age of bipolar disorders at six international sites. J Affect Disord 2010;121(1-2):143-6).
ResultsA 60-year-old woman is brought to the emergency department for evaluation by her family. Over the past 7 days, the patient has become increasingly irritable and argumentative, is sleeping less, is talking faster than usual and has begun to express paranoid concerns about her students “stealing my exam”. The patient is a university professor.
In the assessment interview she is hyperverbal, expansive, and grandiose. The family has also just recently discovered that she has spent a large sum of money on the Internet.
She has no history of psychiatric contact or substance use disorders; however, she has a family history of severe depression.
In the absence of any plausible non-psychiatric condition that could mimic or induce mania, the working diagnosis is bipolar I disorder, most recent episode (MRE) manic with psychotic features.
Image:
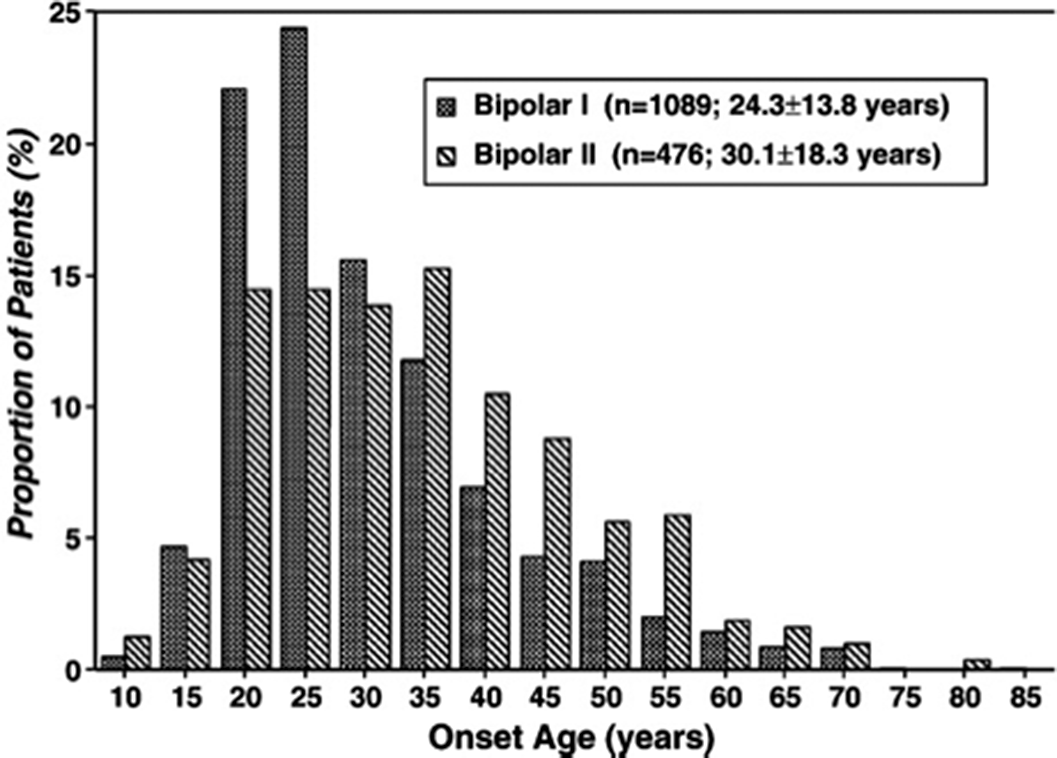
Image 2:
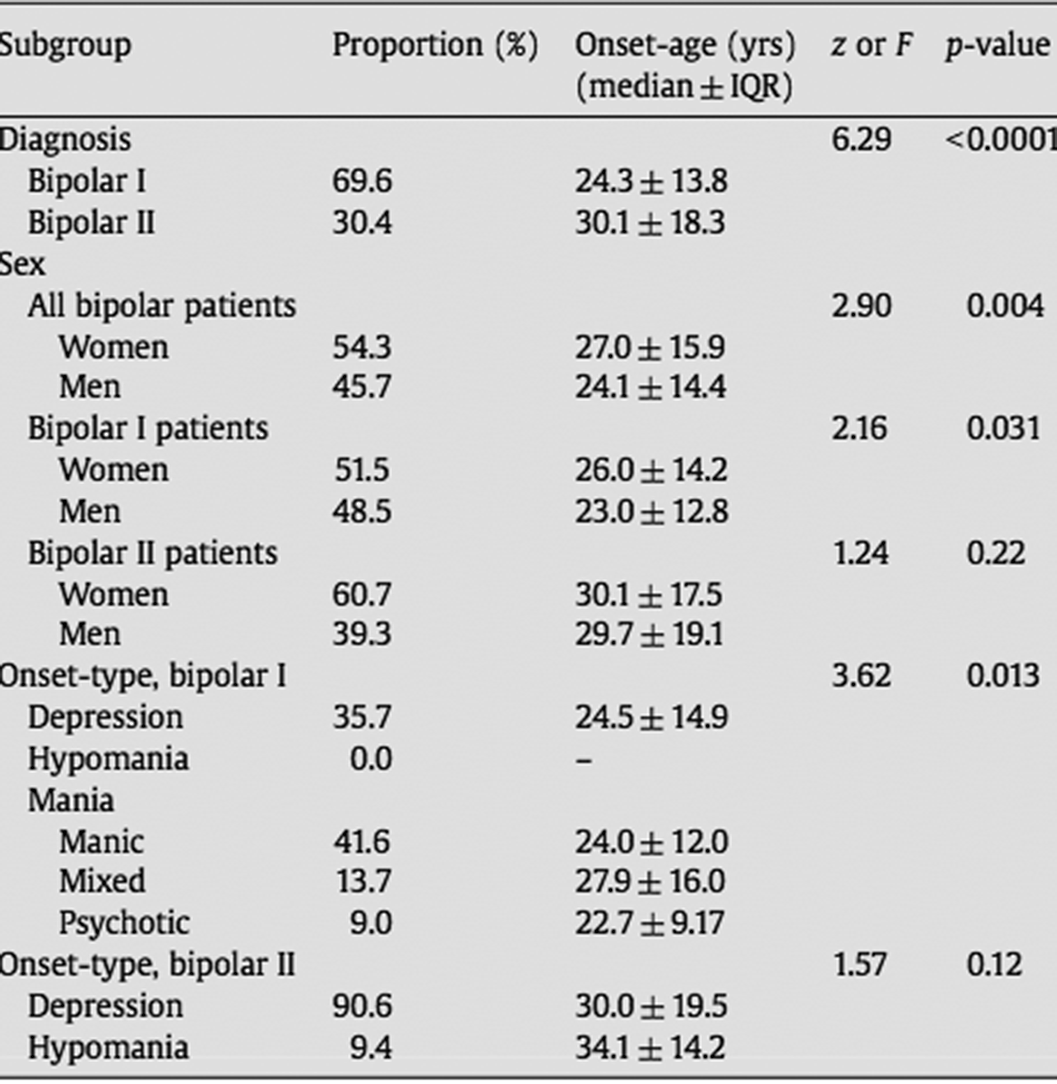 Conclusions
ConclusionsThe share of older age bipolar disorder will grow constantly in the next decades and further research on this neglected patient group is urgently required.
Disclosure of InterestNone Declared
Lithium management in pregnant patients with bipolar disorder
- I. Romero Gerechter, M. Martín Velasco, A. Sanz Giancola, E. Arroyo Sánchez, C. Díaz Mayoral, P. Setien Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women with bipolar disorder often ask their treating clinician for information about family planning, as they are concerned about the impact of their illness on offspring. Pregnancy places additional stress on patients, and physiological changes are particularly acute during postpartum. On the other hand, the risk of abnormalities and teratogenicity from psychotropic drugs is significant. The decision wether resuming or discontinuating lithium is discussed.
ObjectivesWe present a theoretical review on the topic.
MethodsA bibliographic review is presented.
ResultsThe choice to continue medication during pregnancy balances the risks of an untreated illness with the risks of medication exposure. Abrupt discontinuation of psychotropic medications is associated with an increased risk for illness recurrence. Women with BD who discontinue their medications before or during pregnancy have a 71% risk of recurrence with new episodes occurring most frequently in the first trimester. Recurrent illness during pregnancy is associated with a 66% increase in the risk of postpartum episodes. Untreated or under-treated BD during pregnancy is associated with poor birth outcomes independent of pharmacotherapy exposure, including preterm birth, low birth-weight, intrauterine growth retardation, small for gestational age, fetal distress, and adverse neurodeve- lopmental outcomes. Women with untreated BD also have behavioral risk factors such as decreased compliance with prenatal care, poor nutrition, and high-risk behaviors. Impaired capacity to function may result in loss of employment, health care benefits, and social support. The biological and psychosocial risks of a BD episode are the justification for the risk of medication exposure.
Fetal exposure to lithium has been associated with an increased risk for cardiac abnormalities. The risk for Ebstein’s anomaly with first trimester exposure is 1 (0.1%) to 2 in 1000 (0.2%), but the absolute risk remains low. Folate supplementation with 5 mg reduces the risk and severity of congenital heart disease. Lithium toxicity causes lethargy, hypotonia, tachycardia, coma, cyanosis, and chronic twitching in the newborn.
Strategies to minimize fetal exposure and maintain efficacy include using the lowest effective dose, prescribing lithium twice daily to avoid high peak serum concentrations, and regular monitoring of lithium serum concentrations. The effective serum concentration must be established before pregnancy. If a therapeutic concentration has not been established, the lithium dose is titrated to a concentration within the therapeutic range. Breast feeding is discouraged in women taking lithium because of the high rate of transmission to the infant.
ConclusionsTreatment decisions for pregnant women with mood disorders must weigh the potential for increased risks of lithium during pregnancy, especially during the first trimester, against its effectiveness at reducing relapse.
Disclosure of InterestNone Declared
Clozapine use in drug induced psychosis in Parkinson´s disease: a case report and review of literature.
- A. Sanz Giancola, P. Setién Preciados, E. Arroyo Sánchez, I. Romero Gerecther, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The occurrence of psychotic symptoms induced by dopaminergic drugs marks a new phase in the course of Parkinson’s disease (PD). The term drug induced psychosis may be used when other significant psychiatric diseases are excluded in patients with no history of psychosis. The prevalence of dopaminomimetic psychosis varies from 5% to 20%. Therefore, knowledge of the psychopharmacological management of this condition is essential.
ObjectivesThe purpose of this case report and literature review is to to learn the psychopharmacological management of this not uncommon medical complication.
MethodsDescriptive case study and review of literature
ResultsWe present the case of a 71-year-old man with a medical history of Parkinson’s disease with partial response to treatment with high doses of levodopa and carbidopa.
He was brought to the emergency department by his family due to the presence of behavioural alterations at home.
The patient reported seeing men in foam trying to harm his family. In a disjointed way in his speech, he links this idea with the delusional belief that he is being watched by electronic devices placed throughout the house. In a variegated manner he links this with a coelotypical type of discourse, however the delusional ideation remains unstructured throughout.
With no previous personal or family history of mental health and ruling out underlying organic conditions, a diagnosis of psychosis secondary to pharmacological treatment for Parkinson’s disease is presumed.
Considering the risks and benefits, it was decided to maintain the anti-Parkinson’s dose in order to avoid worsening the patient’s motor function. Therefore, after reviewing the literature, the best option was to introduce clozapine at low doses, up to 50 mg at night, with the respective analytical control. After a week’s admission, the patient began to improve psychopathologically, achieving an ad integrum resolution of the psychotic symptoms.
ConclusionsDespite the availability of other antipsychotic treatments such as quetiapine or the more recent pimavanserin, clozapine remains the treatment of choice for drug-induced psychosis in Parkinson’s disease.
Disclosure of InterestNone Declared
PSYCHOTIC DISORDER DUE TO PSYCHOSOCIAL STRESS EPISODE. REVIEW OF A CASE.
- A. Gonzalez-Mota, I. M. Peso-Navarro, C. Garcia-Cerdan, C. Munaiz-Cosio, M. Ligero-Argudo, C. Martin-Gomez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1040-S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic disorder is defined as a loss of contact with reality. Those who suffer from it perceive an altered reality, assuming it to be true.This feeling of unreality generates nervousness, anguish, hypervigilance and even social and emotional isolation.
We present the case of a 18-year-old woman who attended the Emergency Department accompanied by the director of her college due to behavioral alterations. The patient reports that since she has moved to Salamanca to study,she has the feeling that her father has hired spies, one of them being her classmate, being able to hear sounds and voices, which she defines as motivating her to go on with her life. She reports that she is in a lower mood in this context and that there have been some days when she has not been able to attend class.
ObjectivesThe objectives are to study the severity of the psychotic disorder in a young patient subjected to an episode of stress and to observe the reaction of the patient when it has been properly treated.
MethodsWe carry out a review of the clinical history of a 18-year-old female patient with psychotic disorder, admitted to the Psychiatric Brief Hospitalization Unit (PBHU) in Salamanca.
ResultsThe patient was treated with Risperidone 2mg/24h. After a few days in the PBHU, total disappearance of the psychotic symptoms was observed and the patient is completely self-critical. Once she was discharged, it was decided that she should return home with her parents for several months and continue treatment with Aripiprazole and Sertraline.
ConclusionsOccasionaly, there are ethical dilemmas about beginning to treat young patients with psychotic ideas derived from external situations. Optimal treatment including drugs, psychotherapy and family support are essential. According to the scientific literature,a greater involvement in diagnosis,treatment and follow-up is recommended in patients with psychotic symptomatology derived from stress.
Disclosure of InterestNone Declared
Acute mutism in a young female. A case report of a 20-year-old female who presents a 3-month mutism
- A. Gonzalez-Mota, A. Gonzalez-Gil, C. Martin-Gomez, J. A. Benito-Sanchez, I. M. Peso-Navarro, L. Fernandez-Alonso
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 20-year-old female presents with a progressive 3-month mutism, hyporexia (20kg weight loss), abulia, anhedonia, apathy, social isolation,seeking company of her parents even at night, bradypsychia, sialorrhea, psychomotor slowdown and hypomimia. She is hospitalized in the Psychiatric Brief Hospitalization Unit (PBHU).Her parents relate the beginning of this symptomatology to a breakup and gender violence,which the patient confirms during the interview by eye/cephalic movements and single words jotted down.
ObjectivesThe objective of this study is to describe the evolution of the patient during her hospitalization in the PBHU of Salamanca and to look into the available bibliography about mutism related to stress and sialorrhea.
MethodsWe carried out a follow-up of the hospitalization of the patient and a structured search in PubMed with the keywords “mutism”,“sialorrhea” and “stress” in the last 10 years in English,Spanish and French.
ResultsFew or no articles where found.Therefore, the articles about mutism and stress were analyzed, which focused mostly in selective mutism. Regarding fear,the response to cope with the threat(fight, flight, freeze) is mediated by the autonomic system. The “Polyvagal Theory” speaks about the vagus nerve participating in emotion regulation (social communication and mobilization). Dissociation, in this context,has adaptive and defensive purposes and its threshold can be reduced by repeated stress situations.Long-term alteration of the autonomic nervous system has been described in selective mutism.This malfunction can be related to an elevated production of saliva due to the activation of the parasympathetic in the salivary glands, causing sialorrhea in our patient.
The patient began treatment with sertraline 100mg and risperidone 2mg with the aim of its antidepressive and major tranquilizer effects, she also began individual and family psychotherapy, we assured her sleep and intakes and she began to progressively recover her speech and mobility,identifying a possible trigger for the symptomatology: a physical beating of gender violence after her breakup.
ConclusionsDissociation and “freeze” response can be a maladaptative mechanism to fear.The malfunction of the autonomic nervous system can explain the disconnection,poor gaze,low facial and body expression and inability to speak.
Disclosure of InterestNone Declared
Moria or Mania? Manic symptoms as the clinical manifestation of glioblastoma recurrence: a case report
- F. Mayor Sanabria, M. E. Expósito Durán, M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. Paz Otero, I. Alberdi Páramo, B. Rodado León
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S520
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Up to 50% of patients with brain tumors experience psychiatric symptoms, and rates up to 80% have been reported in malignant neoplasms such as glioblastoma multiforme (GBM). Still, clinical presentation as mania-like syndromes is a rare phenomenon, mainly occurring when frontal structures are compromised.
We present the case of a 42-year-old woman who was admitted to our hospital due to manic symptoms coinciding with a recurrence of a bifrontal GBM, for which she underwent surgery 5 months prior.
Objectives1) To describe the clinical particularities of this case, focusing on the differential diagnosis.
2) To review the association between manic symptoms and frontal dysfunction caused by brain tumors, with special interest on GBM.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, we reviewed the available literature in relation to manic symptoms related to brain tumors.
ResultsThe patient’s GBM recurrence presented with late onset symptoms of mania, including euphoric mood, increased spending, ideas of grandiosity and hyper-religiosity. She had no previous psychiatric history but, interestingly, she had an extensive affective burden in her family, with 4 consummated suicides. However, she also presented other clinical signs, such as disorientation, perseveration, mild memory impairment and stereotyped motor behaviors, that pointed to relevant frontal lobe dysfunction, suggesting Moria as a possible contribution for the symptoms described.
Manic symptoms in the context of brain tumors appear in 7-15% of patients with psychiatric symptoms, usually associated with right frontal dysfunction (75% of cases). Bifrontal affectation, such as this patient, is only described in 6% of cases. Although fast growing, malignant tumors have been associated with higher rates of psychiatric symptoms, no correlation has been described between these and brain tumor histology.
Conclusions- The presence of atypical manic symptoms, such as those presented in this case, should raise clinical concern for secondary mania.
- Moria shares similarities with mania, including mood elevation, tendency to hilarity or hyper-sexuality, that may hinder diagnosis of patients with frontal dysfunction.
- This case outlines the difficulties in making a differential diagnosis in patient with both manic and neurological signs, and highlights the implication of frontal structures in the development of manic symptoms.
Disclosure of InterestNone Declared
Psychotic denial of pregnancy: case report and narrative literature review.
- M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral, E. Arroyo Sánchez, A. Sanz Giancola, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the phenomenon where a woman fails to recognize or accept her pregnancy at >20 weeks gestational age. It associates with increased morbidity and mortality of mother and child, and can be classified as non-psychotic or psychotic. There is fewer medical literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data regarding incidence nor approved interventions or treatment.
ObjectivesTo describe this unfamiliar entity in order to be able to perform a proper diagnosis and thus prevent possible negative outcomes.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, with an advanced pregnancy, who was admitted to a Psychiatry in-patient unit due to psychotic symptoms such as mistrust and delusions. She showed scarce collaboration during assessment and did not give any plausible information about her identity. Her birthplace and prior medical records were therefore unknown. Apparently, she had no family nor social support network. Despite the obvious signs, she did not recognize being pregnant and showed great irritability when asked; her responses ranged from claiming she was suffering from a gastric tumor and making delusional attributions of symptoms clearly related to the pregnancy to partially acknowledging her state but refusing to answer any questions on the matter. Blood work showed no significant abnormalities and obstetric ultrasound revealed a low risk 35 weeks pregnancy.
With an estimated prevalence of 1:475 in general population, denial of pregnancy is not as rare as it may seem. The psychotic variant, however, is rather uncommon. Typically, women with psychotic pregnancy denial have prior history of major mental illness, most frequently schizophrenia, and suffer from extreme psychosocial vulnerability. They usually present previous or anticipated child custody loss, which hampers the process of developing antenatal attachment behaviours. Psychotic denial does not associate with concealing, since these women are mentally detached from the gestation and tend to create delusional explanations to their pregnancy symptoms. Not all of them show complete denial, some being able to acknowledge it, though mostly in an inconsistent way. These patients often fail to seek prenatal care or are noncompliant, they are at greater risk of drug exposure, and some are unable to recognize symptoms of labour, all of which increases the rate of negative outcomes for mother and baby, including neonaticide.
ConclusionsPsychotic denial is a rare diagnosis which should be properly assessed due to its clinical implications and the need to prevent potential negative outcomes for mother and baby.
Disclosure of InterestNone Declared
Application of family therapy in a case of anorexia nervosa
- C. Díaz Mayoral, I. Romero Gerechter, E. Arroyo Sánchez, M. Martín Velasco, A. Sanz Giancola, M. Martín de Argila
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S848
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is a behavioral mental disorder, characterized by body dysmorphia, an intense fear of gaining weight and behaviors that interfere with this, in addition to a restriction of food intake, associated usually with medical complications, even a considerable risk of death.
Several psychotherapeutic approaches have been used along last decades. Until relatively recently, parents have been recognized as part of the problem, but nowadays we involve them into the therapeutic process through family therapy based on a systemic approach, recommended in current published clinical guidelines and research findings, with consistent evidence, as the first-line treatment of patients with anorexia nervosa.
ObjectivesA case of a patient with anorexia nervosa, is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsA 24-yeard-old female was hospitalized for renutrition due to a significant weight loss and multiple physical symptoms. After 4 months without progress, the patient was transferred to the psychiatric ward.
Once there, physical stabilisation was achieved with family therapy and pharmacological treatment, based on progressive administration of Clomipramine, previously assessed by Cardiology, which improved rumination and obsessive behaviour. We conduct daily individual and weekly family interviews, working on family dynamics, emotional regulation strategies and more adaptive ways of communication. Likewise, several lines of action were found in the systemic work: peripheral father; maternal over-involvement; fraternal rivalry; difficulties of interaction between all of them, derived from “the role of the sick person” and intra-family communication around the illness. Finally, showed effectiveness in terms of an improvement in interpersonal relationships, greater assertiveness and an optimistic attitude with an active search for coping strategies.
ConclusionsHistorically, parents have been recognized by a causal factor in the pathogenesis of this disorder. Nevertheless, the abolition of the emphasis on family responsibility, motivated by a philosophic and evidence-based, has allowed us to see them as an essential resource in aiding the patient in the improvement process. This parental involvement has resulted in a relevant reduction in morbidity, as well as a significant decrease treatment attrition rates. It has been noted a re-establishment in other individual and family factors such as self-esteem, quality of life, and some aspects of the experiences of caregiving, and behavioral symptoms have been resolved.
Disclosure of InterestNone Declared
The role of immune disfunction in schizophrenia pathogenesis
- I. Azevedo Silva, B. Martins, V. Melo, J. Cardão, A. Matos, C. Agostinho
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1060-S1061
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the last years there has been increasing evidence that inflammation and autoimmunity may play a role in the pathogenesis of schizophrenia.
Although the brain has been considered an immune-privileged site, we understand now that infections and inflammation interfere with the blood-brain barrier, making the brain vulnerable to antibodies, cytokines and infectious agents.
ObjectivesTo understand the role of immune disfunction in schizophrenia pathogenesis, as well as the potential role of immunotherapy in its treatment.
MethodsWe performed a narrative review of the evidence, using the following terms and their combinations “schizophrenia”, “autoimmunity” and “monoclonal antibodies”.
ResultsIt is widely known that prenatal, perinatal and childhood exposure to infections, nutritional deficits and other environmental insults, acting on a background of genetic vulnerability, may lead to schizophrenia. In such cases, we can observe potent and enduring inflammatory responses, such as cytokines dysregulations.
State markers, including IL-1β, IL-6 and TGF-β have increased levels during exacerbation of symptoms and stabilized levels when antipsychotics are administrated. Trait markers, such as IL-12, IFN-γ and TNF-α have systematically increased levels in acutely and chronically ill patients, even during clinical stability.
Moreover, patients with schizophrenia have been showing abnormalities of the blood-brain barrier, signs of central nervous system inflammation and elevated autoantibody levels and reactivity.
Several autoimmune diseases are associated with schizophrenia, such as celiac disease, Graves’ disease and psoriasis. On the other hand, it is known since the 1950’s that schizophrenia has a negative association with rheumatoid arthritis.
There are case reports of people with psychosis that were treated with immunosuppressive agents (for concurrent autoimmune diseases) that showed improvement in their psychotic symptoms.
NSAIDs, immunomodulators and several monoclonal antibodies have been tested as potential treatments for schizophrenia. The results were conflicting but promising. It is suggested that not every patient with schizophrenia may benefit from these treatments. Ideally, treatment targeting the immune system should be provided in earlier phases of disease, such as in prodromal psychosis and first episode psychosis, because these are related to irreversible grey matter loss which causes cognitive decline.
ConclusionsImmune dysregulation may have an important etiological role in schizophrenia.
Hence, specific therapeutic approaches targeting the immune system may lead to new ways of treating and even preventing psychotic disorders.
Further investigation is necessary in order to provide more information on how aberrant antibody and cytokine production interferes with neuronal function and how it is expressed at the clinical level.
Disclosure of InterestNone Declared
Visual hallucinosis and Linezolid use: A case report.
- M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. E. Expósito Durán, F. Mayor Sanabria, Í. Alberdi Páramo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1012
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 78-year-old man with multiple somatic pathologies and associated depressive symptoms, under treatment with Citalopram 10mg, who was admitted due to cholangitis secondary to biliary prosthetic obstruction.
Empirical antibiotic treatment with Meropenem and Linezolid was started, along with an increase in the dose of Citalopram to 20mg due to mood worsening. The patient begins with symptoms consisting of complex and polymorphic visual hallucinosis, without any affective or behavioral repercussions. He does not present another semiology of the psychotic sphere.
ObjectivesTo highlight the importance of knowing the different interactions and adverse effects of drugs for good clinical management.
MethodsWe collected the complete medical history of our patient and we carried out a review of the interactions and adverse effects described with the antibiotic drug Linezolid.
ResultsAs the onset of hallucinations was temporarily correlated with the use of medications, drug-induced hallucinations were suspected, resolving completely after 2 days after withdrawal of Linezolid treatment.
Linezolid is a nonselective inhibitor of MAO A and B, preventing the destruction of monoamine neurotransmitters like serotonin, dopamine, or norepinephrine. It has dopaminergic properties that may enhance the central nervous system effects of anticholinergics and co-prescription with serotonergic drugs increases the risk of serotonin syndrome.
ConclusionsThis case highlights the importance of taking into account drug interactions and adverse effects to reduce the risk of drug induced symptoms and optimize their management.
The increase in resistance to antibiotic treatment allows us to anticipate that the use of Linezolid will increase in the coming years, and it is important to know its mechanism of action given the interactions with psychotropic drugs that we use in our usual clinical practice
Disclosure of InterestNone Declared
Correlation between BDNF levels and folic acid levels at baseline in drug-naïve First Episode Psychosis
- A. Toll, D. Bergé, I. Canosa, M. Martín - Subero, T. Legido, C. Fernandez - Hinchado, V. Perez - Sola, A. Mané
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S184-S185
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a severe and common psychiatric disorder characterized by disturbed brain development. Brain-derived neurotrophic factor (BDNF) mediates differentiation and survival of neurons as well as synaptic plasticity during the brain development. Several studies have shown decreased serum levels of BDNF in chronic, first episode, and drug naïve schizophrenia patients. Folate provides the substrate for intracellular methylation reactions that are essential to normal brain development and function. Abnormal folate metabolism has been implicated in schizophrenia. For example, reduced maternal folate intake associated with an increased risk for schizophrenia. Also, low blood levels of folate have been reported in patients with schizophrenia, and are associated with clinical manifestation especially in the negative symptom domain.
ObjectivesWith this study, we want to know how BDNF levels at baseline in drug-naïve FEP are associated with folic acid.
MethodsFifty drug-naïve FEP treated between April 2013 and July 2017 at the ETEP Program at Hospital del Mar were included. Inclusion criteria were: 1) age 18-35 years; 2) DSM-IV-TR criteria for brief psychotic disorder, schizophreniform disorder, schizophrenia or unspecified psychosis; 3) no previous history of severe neurological medical conditions or severe traumatic brain injury; 4) presumed IQ level > 80, and 5) no substance abuse or dependence disorders except for cannabis and/or nicotine use. All patients underwent an assessment at baseline including sociodemographic and clinical variables. Fasting blood samples were obtained before administering any medication at baseline and used to determine folic acid and BDNF levels.
ResultsIn our drug-naïve FEP sample, folic acid levels showed a significative positive correlation with BDNF levels at baseline (r = 0.584; p = 0.003). Moreover, we did a lineal regression model that showed that the baseline variables that better predict BDNF levels were folic acid levels, and cannabis use.
ConclusionsOur results are consistent with the findings from some of previous studies that also shows that lower folic acid levels are associated with lower BNDF levels at baseline in drug-naïve FEP. Folate deficiency is associated with cerebrovascular and neurological diseases, and mood disorders. The importance of folate in the nervous system was initially demonstrated in studies that established a greatly increased risk of neurodevelopmental disorders in the offspring of folate-deficient pregnant women. In the adult, epidemiological studies have linked lack of folate to neurodegenerative and neuropsychiatric diseases. However, the mechanisms by which chronic folate deficiency adversely affects CNS function are incompletely understood. Some studies in animals models have hypothesized that folate deficiency in animals could be associated with pyramidal cell loss and reduced hippocampal BDNF.
Disclosure of InterestNone Declared
Mania induced after corticosteroid treatment: a case report
- E. Arroyo Sánchez, A. Sanz- Giancola, P. Setién Preciados, I. Romero Gerechter, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S697
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are drugs widely used in clinical practice for their anti-inflammatory and immunosuppressive properties. Despite their beneficial effects, a high association of these drugs with neuropsychiatric adverse effects such as psychosis, mania, depression, delirium or increased risk of suicide, among others, has been observed. We present the case of 54-year-old man who started treatment with hydroaltesone 20 mg/8h after undergoing surgery for a pituitary macroadenoma who began with maniform clinic.
ObjectivesTo know the prevalence, risk factors and treatment of mania as a side effect of corticosteroid drugs.
MethodsPresentation of the case and review of the available literature on the risk of developing mania after corticosteroid treatment.
ResultsSeveral studies confirm that the incidence of psychiatric adverse effects after the use of corticosteroids is around 6% if we refer to severe reactions; 28% moderate reactions; and 72% if we consider milder reactions. The direct relationship between these drugs and affective symptoms ranges in rates between 1-50% of cases, the most frequent being depression and mania. The risk of mania after treatment with corticosteroids is 4-5 times higher than if we compare it with a group of population not exposed to these drugs. There is a dose-response relationship, increasing the risk from a daily dose of 40 mg/day, with an average duration of symptoms of around 21 days. Female sex seems to be a risk factor in relation to the fact that diseases requiring this type of treatment are more common in this gender. As first-line treatment for mania secondary to corticosteroids, a decrease in treatment dose or its interruption, whenever possible, is proposed. Adjuvant treatment may be required, with atypical antipsychotics being the first choice.
ConclusionsCorticosteroid therapy has a direct dose-response relationship with the presence of psychiatric adverse effects such as mania. Dose and sex have been studied as possible adverse effects. Therefore, the pharmacological treatment of choice consists of a reduction in the dose of corticosteroids administered or withdrawal, if possible, and may be combined with an atypical antipsychotic such as olanzapine, quetiapine or risperidone. Re-evaluation is recommended until complete resolution of the clinical picture and then antipsychotic treatment can be progressively withdrawn.
Disclosure of InterestNone Declared
Clozapine in first episode psychosis – the experience of a Portuguese center
- I. Soares Da Costa, F. Santos Martins, C. Silveira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S438
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Antipsychotics are the standard in the treatment of first psychotic episodes. Although the majority of patients respond to the established treatment, it is currently known that there is a subgroup of patients whose response is not satisfactory. In this group, the subsequent response to a new antipsychotic is generally poor. Clozapine is an antipsychotic with a unique profile, with demonstrated efficacy and approval in the treatment of treatment-resistant schizophrenia. Its role in the first psychotic episodes remains unclear and its use is, to say the least, controversial.
ObjectivesThis work aims to analyze and evaluate the use of clozapine in patients with a first psychotic episode, taking into account the experience of a Portuguese Hospital Center.
MethodsWe carried out a retrospective study, including all patients admitted to the inpatient clinic of adults with a first psychotic episode, in the Department of Psychiatry of Centro Hospitalar Universitário of São João, in Oporto, between 2007 and 2020. Clinical and socio-demographic data were collected.We performed a retrospective analysis of patients who, at discharge, were medicated with clozapine, proceeding to a descriptive analysis.
ResultsIn this case series, we intended to describe the cases of patients in whom the use of clozapine in the first psychotic episode was initiated. All patients were discharged with the diagnosis of Schizophrenia. Prior to the introduction of clozapine, patients were treated with other antipsychotics, normally two. Patients taking clozapine were younger and had a longer duration of untreated psychosis. They had also longer length of hospital stay. The pattern of prescribing antipsychotics in the first and subsequent episodes has generally been extensively studied. However, the use of clozapine in the first episodes remains unclear.In the literature, and despite clozapine being considered one of the most effective antipsychotics, there is a high prevalence of polypharmacy and a significant delay in its use in the first episodes.Notwithstanding the unfavorable metabolic and hematological profile of clozapine, compared to other antipsychotics, in terms of hospitalization, mortality and discontinuation rates for all causes, it demonstrates a pattern of superiority.
ConclusionsThe superiority in effectiveness of clozapine is well established, despite its underutilization and frequent delay in its introduction.The clinicians attitude remains a significant barrier to the commencement of clozapine, although it is important to define and characterize better potential groups of eligible patients. Education resources for clinicians as well as services specifically dedicated to early identification and management of eligible patients would be beneficial.
Disclosure of InterestNone Declared
Formal Caregivers in Intellectual Disability Facilities
- B. Martins, I. A. Silva, J. Cardão, A. H. de Matos, C. Agostinho
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S892-S893
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Caring for individuals with intellectual disabilities is a passionate, but challenging profession. Whether working in residential homes or in occupational facilities, its staff deals with the ordinary issues of teamwork, but also with these clients behavioral comorbidities. It often includes self-harming and aggression towards others – namely towards the staff itself. This is particularly relevant since a high turnover of staff implies the loss of people who are familiar with the needs and specificities of those clients. The quality of care provided may also be affected.
ObjectivesTo investigate whether, or not, formal caregivers are at greater risk of occupational health issues, and what their main determinants are.
MethodsResearch in Medline for intellectual disability caregivers. Only the relevant articles, published in English, were considered.
ResultsAmong formal caregivers of people with intellectual disabilities, job dissatisfaction and job strain were found to be especially relevant and were associated to the following variables:
• Younger workers or those with less professional experience
• Personality and individual maladaptive coping strategies
• Poor organizational support
• Conflicting, ambiguous, or overloaded professional roles
• Unclear work tasks
The incidence of Burnout Syndrome was also described as relevant among these workers and was associated not only to aggression towards the worker, but also to the fear of aggression.
ConclusionsCaring for people with intellectual disabilities, in a residential or in an occupational context, implies heavy emotional and physical demands and a high prevalence of job dissatisfaction, Job Strain and Burnout Syndrome. In addition to the high risks to the quality of life and health of caregivers, there are consequences for the quality of the care that is provided. For this reason, guaranteeing proper work conditions should be considered part of the Social Institutions main goals. Yet, we lack specific, controlled studies that properly evaluate what measures could indeed help institutions to prevent occupational (and mental) health distress among their staff.
Disclosure of InterestNone Declared
Effectiveness and Tolerability of Intranasal Esketamine in Treatment-Resistant Depression: Report of Two Clinical Cases
- A. Mercado-Rodríguez, C. Martín Requena, A. Cano Baena, I. Zorrilla Martínez, A. González-Pinto Arrillaga, L. Mar-Barrutia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S824
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is a mental health disorder characterised by persistently low mood; anhedonia; feelings of worthlessness and guilt; altered appetite, weight and sleep and suicidal ideation. About one-third of patients do not respond to available antidepressants (AD). Treatment-resistant depression (TRD) is a clinical term used to define a lack of response to two or more AD in patients with MDD that do not respond to other lines of treatment either. TRD is associated with an increased risk of relapse, hospitalisation and suicide. Esketamine is a non-competitive NMDAR antagonist that acts as an antidepressant by modulating glutamatergic neurotransmission, disturbed in MDD patients. It has recently been approved by the European Commission as a fast-acting nasal spray therapy for depression and suicidal ideation after showing effectiveness in TRD patients (Papakostas et al. JCP 2020; 81 4).
ObjectivesThe aim of this study is to determine the effectiveness, safety and tolerability of intranasal esketamine in two TRD-diagnosed patients and to assess their clinical evolution.
MethodsA prospective study was conducted describing the evolution of two TRD patients treated with intranasal esketamine. We used The Hamilton Depression Rating Scale (HDRS) to quantify the severity of their symptoms and assess their recovery over time, analyzing the score change from baseline to endpoint as a primary outcome of the study. We also applied the Addensbrooke Cognitive Examination (ACE-III) as a tool to establish their cognitive condition before therapy and its evolution. Changes in dosage during treatment, adverse effects, time required for onset of action, clinical outcomes and other variables were also measured.
ResultsIntranasal esketamine was administered twice a week during the first 4-week induction phase and weekly during the following 6-month maintenance phase. Dosage of antidepressant was determined depending on each patient’s age and clinical evolution, being 56 mg the initial dose for case 1 (57 years old) and 28 mg for case 2 (71 years old). This antidepressant was effective in both patients in a fast-acting way, with the onset of action occuring within the first two weeks. During the course of treatment, the HDRS score significantly decreased, associated with improvement and remission of depressive symptoms. Cognitive performance got better in both cases. None of the patients discontinued treatment due to adverse effects or lack of efficacy.
ConclusionsOur data suggest that intranasal esketamine therapy is a good alternative in TRD patients, being effective, fast-acting and well-tolerated, with a manageable safety profile. Clinical stability was also observed in the medium-term follow-up after the end of treatment. This presents esketamine as a promising therapeutic and effective strategy in MDD patients who are either treatment-resistant or acutely suicidal.
Disclosure of InterestNone Declared
Mega-analysis of association between obesity and cortical morphology in bipolar disorders: ENIGMA study in 2832 participants
- Sean R. McWhinney, Christoph Abé, Martin Alda, Francesco Benedetti, Erlend Bøen, Caterina del Mar Bonnin, Tiana Borgers, Katharina Brosch, Erick J. Canales-Rodríguez, Dara M. Cannon, Udo Dannlowski, Ana M. Diaz-Zuluaga, Lorielle M.F. Dietze, Torbjørn Elvsåshagen, Lisa T. Eyler, Janice M. Fullerton, Jose M. Goikolea, Janik Goltermann, Dominik Grotegerd, Bartholomeus C. M. Haarman, Tim Hahn, Fleur M. Howells, Martin Ingvar, Neda Jahanshad, Tilo T. J. Kircher, Axel Krug, Rayus T. Kuplicki, Mikael Landén, Hannah Lemke, Benny Liberg, Carlos Lopez-Jaramillo, Ulrik F. Malt, Fiona M. Martyn, Elena Mazza, Colm McDonald, Genevieve McPhilemy, Sandra Meier, Susanne Meinert, Tina Meller, Elisa M. T. Melloni, Philip B. Mitchell, Leila Nabulsi, Igor Nenadic, Nils Opel, Roel A. Ophoff, Bronwyn J. Overs, Julia-Katharina Pfarr, Julian A. Pineda-Zapata, Edith Pomarol-Clotet, Joaquim Raduà, Jonathan Repple, Maike Richter, Kai G. Ringwald, Gloria Roberts, Alex Ross, Raymond Salvador, Jonathan Savitz, Simon Schmitt, Peter R. Schofield, Kang Sim, Dan J. Stein, Frederike Stein, Henk S. Temmingh, Katharina Thiel, Sophia I. Thomopoulos, Neeltje E. M. van Haren, Cristian Vargas, Eduard Vieta, Annabel Vreeker, Lena Waltemate, Lakshmi N. Yatham, Christopher R. K. Ching, Ole A. Andreassen, Paul M. Thompson, Tomas Hajek, for the ENIGMA Bipolar Disorder Working Group
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 14 / October 2023
- Published online by Cambridge University Press:
- 27 February 2023, pp. 6743-6753
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Obesity is highly prevalent and disabling, especially in individuals with severe mental illness including bipolar disorders (BD). The brain is a target organ for both obesity and BD. Yet, we do not understand how cortical brain alterations in BD and obesity interact.
Methods:We obtained body mass index (BMI) and MRI-derived regional cortical thickness, surface area from 1231 BD and 1601 control individuals from 13 countries within the ENIGMA-BD Working Group. We jointly modeled the statistical effects of BD and BMI on brain structure using mixed effects and tested for interaction and mediation. We also investigated the impact of medications on the BMI-related associations.
Results:BMI and BD additively impacted the structure of many of the same brain regions. Both BMI and BD were negatively associated with cortical thickness, but not surface area. In most regions the number of jointly used psychiatric medication classes remained associated with lower cortical thickness when controlling for BMI. In a single region, fusiform gyrus, about a third of the negative association between number of jointly used psychiatric medications and cortical thickness was mediated by association between the number of medications and higher BMI.
Conclusions:We confirmed consistent associations between higher BMI and lower cortical thickness, but not surface area, across the cerebral mantle, in regions which were also associated with BD. Higher BMI in people with BD indicated more pronounced brain alterations. BMI is important for understanding the neuroanatomical changes in BD and the effects of psychiatric medications on the brain.
The Evolutionary Map of the Universe Pilot Survey – ADDENDUM
- Ray P. Norris, Joshua Marvil, J. D. Collier, Anna D. Kapińska, Andrew N. O’Brien, L. Rudnick, Heinz Andernach, Jacobo Asorey, Michael J. I. Brown, Marcus Brüggen, Evan Crawford, Jayanne English, Syed Faisal ur Rahman, Miroslav D. Filipović, Yjan Gordon, Gülay Gürkan, Catherine Hale, Andrew M. Hopkins, Minh T. Huynh, Kim HyeongHan, M. James Jee, Bärbel S. Koribalski, Emil Lenc, Kieran Luken, David Parkinson, Isabella Prandoni, Wasim Raja, Thomas H. Reiprich, Christopher J. Riseley, Stanislav S. Shabala, Jaimie R. Sheil, Tessa Vernstrom, Matthew T. Whiting, James R. Allison, C. S. Anderson, Lewis Ball, Martin Bell, John Bunton, T. J. Galvin, Neeraj Gupta, Aidan Hotan, Colin Jacka, Peter J. Macgregor, Elizabeth K. Mahony, Umberto Maio, Vanessa Moss, M. Pandey-Pommier, Maxim A. Voronkov
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 39 / 2022
- Published online by Cambridge University Press:
- 02 November 2022, e055
-
- Article
- Export citation
Significant early and long-term improvement of neuropsychiatry symptomatology in HCV-infected patients after viral eradication with DAA
- R. Martin-Santos, C. Bartrés, L. Nacar, R. Navinés, M. Cavero, S. Lens, S. Rodriguez-Tajes, J.C. Pariante, I. Horrillo, E. Muñoz-Moreno, N. Bargallo, L. Capuron, J. Meana, X. Forns, Z. Mariño
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S238-S239
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Chronic Hepatitis C infection is considered a systemic disease with extrahepatic manifestations, mainly neuropsychiatric symptoms, which is associated with a chronic low-grade inflammatory state. Hepatitis C virus (HCV) eradication is currently achieved in >98% of cases with oral direct-acting antivirals (DAA).
ObjectivesTo study potential clinical neuropsychiatric changes (mood, cognition, sleep, gastrointestinal, sickness, and motion) in HCV-infected patients after HCV eradication with DAA.
MethodsDesign: Cohort study. Subjects: 37 HCV-infected patients, aged<55 years old, with non-advanced liver disease receiving DAA; free of current mental disorder. 24 healthy controls were included at baseline. Assessment: -Baseline (BL) (socio-demographic and clinical variables, MINI-DSM-IV, and Neurotoxicity Scale (NRS), (mood, cognitive, sleep, gastrointestinal, sickness and motor dimensions). Follow-up: End-of-treatment, 12weeks-after and 48weeks-after DAA: NRS. Analysis: Descriptive and bivariate non-parametrical analysis.
ResultsNRS total score and dimensions where different between cases and controls (.000) at baseline. NRS total score (.000) and mood (.000), cognition (.000), sleep (.002), gastrointestinal (.017), and sickness (.003), except motor dimension score (.130) showed significant longitudinal improvement.
ConclusionsHCV-infected patients with mild liver disease presented significantly worse scores for neurotoxicity symptomatology in all dimensions compared to healthy individuals. After HCV eradication with DAA, both at short and long follow-up a significant improvement of the NRS total score and each of the dimensions (except motor) were observed. However, they did not reach the values of healthy individuals, suggesting a not complete neuropsychiatric restoration in the period studied. Grant: ICIII-FIS:PI17/02297.(One way to make Europe) (RMS) and Gilead Fellowship-GLD17/00273 (ZM); and the support of SGR17/1798 (RMS)
DisclosureNo significant relationships.
Is Praecox Feeling at risk of extinction?
- A. Duarte, C. Laginhas, A. Lourenço, I. Simões, P. Martins
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S218-S219
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Praecox feeling (PF) is a characteristic feeling of bizarreness or unease that a psychiatrist experiences when facing a patient with schizophrenia. This term, proposed by Rumke in 1941, was considered an important feature of a schizophrenia diagnosis. However, since the movement toward operational diagnostic methods in the late 1970s, it has fallen out of use.
ObjectivesThis work aims to discuss the role of Praecox Feeling in the clinical approach to schizophrenia diagnosis.
MethodsPubMed database was searched using combinations of the terms “praecox”, combined with “feeling” and “schizophrenia”.
ResultsPF is sometimes experienced silently before the patient participates verbally. An experienced and attentive clinician can intuitively feels changes in the body posture, facial expression, the tone of the voice, motor behavior, and attitude that could look insignificant, but as a whole they present the patient as “definitely un-understandable.” Although there is lacking evidence to sustain the rehabilitation of the PF as a reliable and valid clinical criterion consistent with the operational approach, a broader scientific approach is called for. PF should not be trivialized, as is sometimes the case, into a quick diagnosis but could be a real determinant of medical decision.
ConclusionsEven though there may not be sufficient evidence to consider it valid clinical diagnostic criteria, it still appears to play an important role in the clinical decision-making process and should not be underestimated or stigmatized. This concept is not completely subjective and does rely on objective information, such as the patient’s behaviour and body language.
DisclosureNo significant relationships.
Functional Neurological Disorder: a multidisciplinary approach
- C. Alvarez Garcia, A. Gomez Martín, M.D.C. Molina Liétor, I. Cuevas Iñiguez, A. Sanz Giancola
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S396
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Functional neurological disorders (FNDs), also known as “conversion disorder”, consist in the appearance of neurological symptoms that do not correspond to any medical condition and produces an impairment in social, occupational and other areas in the patient’s life. This disorder can represent up to 30% of neurologist’s consultation. We introduce the case of a 23-year-old man who attended the emergency services due to fainting and was finally diagnosed with FND.
ObjectivesTo summarize the difficulties of making a diagnosis of FND and the importance of a multidisciplinary approach.
MethodsA narrative review through the presentation of a case.
ResultsThe patient presented many absence seizures during his stay in the hospital. These episodes were characterized by non-reactivity, dysarthria, tremors, tachycardia and hyperventilation. The neurological examination and imaging tests didn’t show any pathological findings. During the psychiatric interview he revealed he had lived a severe conflict with his brothers the previous week and he was being excluded within his family. Furthermore he didn’t have any social support besides his mother in the city he was living, leading this situation to an incrementation of anxiety. Due to the absence of any abnormalities in the examination and recent psychological conflict that was affecting him, FND diagnose was made.
ConclusionsVery frequently the absence of a clear psychological trigger and the presence of neurological alterations can hinder the study of the patient. This makes necessary a multidisciplinary approach and the knowledge of signs that can help to carry out an accurate diagnosis.
DisclosureNo significant relationships.





