19 results
How cultural factors along with mental health diagnoses influence the treatment of a stroke patient with no previous mental health history: a case report
- P. Setién Preciados, E. Arroyo Sánchez, A. Sanz Giancola, I. Romero Gerechter, M. Martín Velasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S822-S823
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental health awareness campaigns in the past few years have vastly improved how medical professionals treat mental health patients. However, prejudices and ignorance still interfere in medical practice. In this context, with the case presented we can see that even in presumed mental health diagnoses along with cultural factors (race, language…), the best medical assistance is not ensured.
ObjectivesReview how different intersectional factors can determine the treatment patients receive at hospitals.
MethodsPresentation of a patient’s case and review of existing literature, in regards to the influence of race, language barriers and mental health diagnoses when attending patients.
ResultsThe patient is presumed to suffer from a mental health condition after a battery of initial tests with inconclusive results do not demonstrate an organic origin. Instead of continuing with the medical study, the patient is disregarded as psychiatric even though his profile doesn´t fit beforehand of a fictitious or conversion disorder. The fact that there are also cultural factors in play (race and language) probably unconsciously influence how the medical team treats this patient’s case. Cultural social factors persistently present as barriers in clinical practice.
ConclusionsRace, language barriers and mental health diagnoses as well as other intersectional factors do have a great impact in the treatment patients receive. There is yet a lot to do when it comes to educating health professionals if we want to offer the best medical assistance.
Disclosure of InterestNone Declared
Suicide behaviour after hospitalisation and related factors: a case report.
- P. Setién Preciados, A. Sanz Giancola, E. Arroyo Sánchez, M. Martín Velasco, I. Romero Gerechter
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1115
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a global epidemic, with the World Health Organization (WHO) estimating that there are roughly 800,000 suicides annually, accounting for 1.4% of all deaths, and making suicide the 18th leading cause of death in 2016 (World Health Organization. There is a pressing need to better understand factors that contribute to suicide risk. One important domain for suicide prevention is inpatient psychiatric treatment, as many patients are admitted precisely in order to reduce their risk of suicide. Although inpatient psychiatric treatment is often used for suicide risk prevention the risk of suicide after inpatient treatment remains high. Patients who have been recently discharged have a greater risk of suicide than non-hospitalised mentally ill people.
ObjectivesReview suicidal risk after hospitalisations and the factors that may have an influence on it.
MethodsPresentation of a patient’s case and review of existing literature, in regards to the rate of suicide after a patient is released from psychiatric hospitalisation and the factors that surround it.
ResultsThe patient in question is admitted into a psychiatric ward with a diagnosis of severe psychotic depression, after a suicide attempt trying to dissect his arms’ blood vessels. Health professionals at the hospital attend to his needs and the patient sees improvement. Not long after his release, there is a second hospital admission, which doesn’t have the same result and after his release he successfully ends his life. What comes to mind with these sorts of patients is: what kind of help would they have needed? Why hospital admission was not enough? And which factors and profile of patient is more prone to develop suicide behaviour?
ConclusionsAdmissions at psychiatric wards always have to be thought of as a beneficial resource for patients. There are some cases in which patients do not get the help they need by being hospitalised, increasing the risk of comitting suicide. A lot more studies will have to be carried out to understand what variables play a part in this. Meanwhile an improvement in outpatient care to support patients after hospital release is crucial.
Disclosure of InterestNone Declared
New-Onset Bipolar Disorder in Late Life: a case report and review of literature
- A. Sanz Giancola, E. Arroyo Sánchez, P. Setién Preciados, M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S691
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The elderly represents the fastest growing group of the population. It is fair to assume that the portion of old age patients suffering from bipolar disorder will grow in a similar manner. Elderly patients represent approximately 25% of the bipolar population. Summarizing, 5–10% of patients were 50 years of age when they experienced their first manic episode, constituting the subgroup of late onset bipolar disorder (LOBD).
ObjectivesThe purpose of this case report and literature review is to emphasise the importance of LOBD in old population and to highlight its still sparse-knowledge.
MethodsDescriptive case study and review of literature (Arnold,I. et al. Old Age Bipolar Disorder—Epidemiology, Aetiology and Treatment. Medicina 2021,57,587; Baldessarini et al. Onset-age of bipolar disorders at six international sites. J Affect Disord 2010;121(1-2):143-6).
ResultsA 60-year-old woman is brought to the emergency department for evaluation by her family. Over the past 7 days, the patient has become increasingly irritable and argumentative, is sleeping less, is talking faster than usual and has begun to express paranoid concerns about her students “stealing my exam”. The patient is a university professor.
In the assessment interview she is hyperverbal, expansive, and grandiose. The family has also just recently discovered that she has spent a large sum of money on the Internet.
She has no history of psychiatric contact or substance use disorders; however, she has a family history of severe depression.
In the absence of any plausible non-psychiatric condition that could mimic or induce mania, the working diagnosis is bipolar I disorder, most recent episode (MRE) manic with psychotic features.
Image:
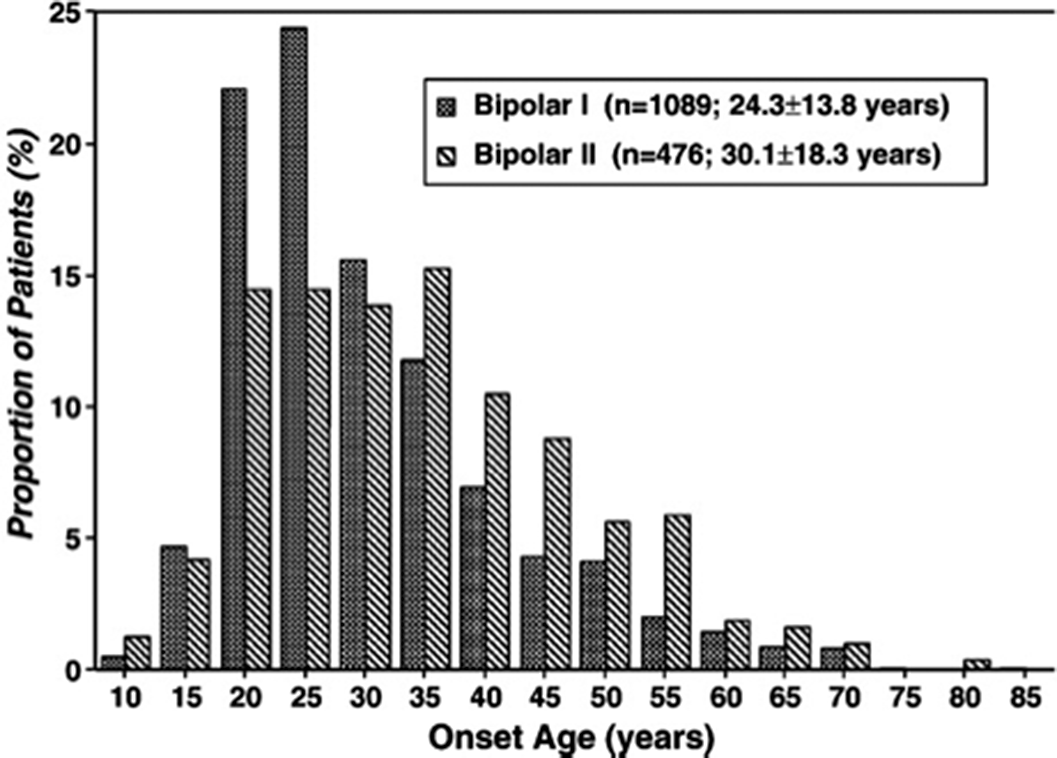
Image 2:
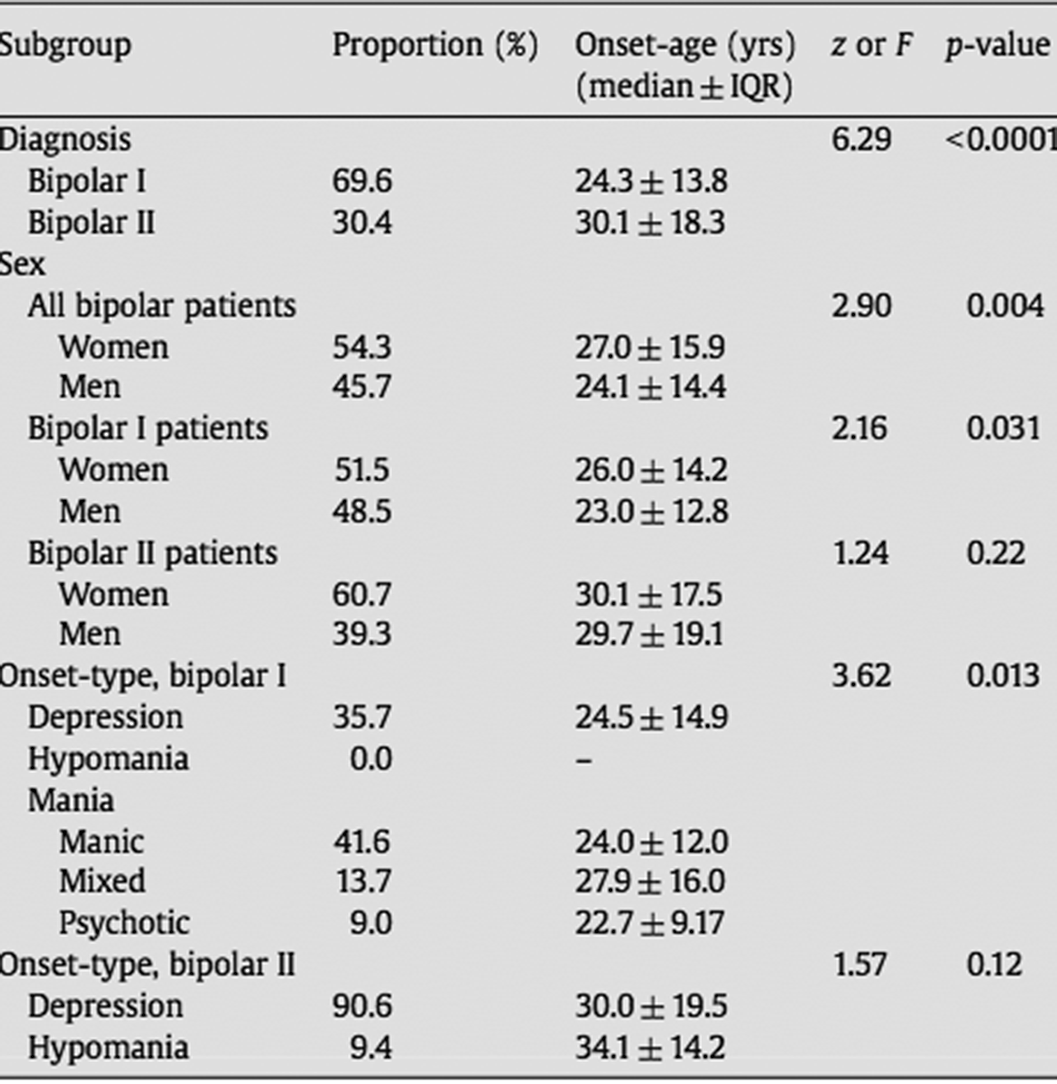 Conclusions
ConclusionsThe share of older age bipolar disorder will grow constantly in the next decades and further research on this neglected patient group is urgently required.
Disclosure of InterestNone Declared
Lithium management in pregnant patients with bipolar disorder
- I. Romero Gerechter, M. Martín Velasco, A. Sanz Giancola, E. Arroyo Sánchez, C. Díaz Mayoral, P. Setien Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women with bipolar disorder often ask their treating clinician for information about family planning, as they are concerned about the impact of their illness on offspring. Pregnancy places additional stress on patients, and physiological changes are particularly acute during postpartum. On the other hand, the risk of abnormalities and teratogenicity from psychotropic drugs is significant. The decision wether resuming or discontinuating lithium is discussed.
ObjectivesWe present a theoretical review on the topic.
MethodsA bibliographic review is presented.
ResultsThe choice to continue medication during pregnancy balances the risks of an untreated illness with the risks of medication exposure. Abrupt discontinuation of psychotropic medications is associated with an increased risk for illness recurrence. Women with BD who discontinue their medications before or during pregnancy have a 71% risk of recurrence with new episodes occurring most frequently in the first trimester. Recurrent illness during pregnancy is associated with a 66% increase in the risk of postpartum episodes. Untreated or under-treated BD during pregnancy is associated with poor birth outcomes independent of pharmacotherapy exposure, including preterm birth, low birth-weight, intrauterine growth retardation, small for gestational age, fetal distress, and adverse neurodeve- lopmental outcomes. Women with untreated BD also have behavioral risk factors such as decreased compliance with prenatal care, poor nutrition, and high-risk behaviors. Impaired capacity to function may result in loss of employment, health care benefits, and social support. The biological and psychosocial risks of a BD episode are the justification for the risk of medication exposure.
Fetal exposure to lithium has been associated with an increased risk for cardiac abnormalities. The risk for Ebstein’s anomaly with first trimester exposure is 1 (0.1%) to 2 in 1000 (0.2%), but the absolute risk remains low. Folate supplementation with 5 mg reduces the risk and severity of congenital heart disease. Lithium toxicity causes lethargy, hypotonia, tachycardia, coma, cyanosis, and chronic twitching in the newborn.
Strategies to minimize fetal exposure and maintain efficacy include using the lowest effective dose, prescribing lithium twice daily to avoid high peak serum concentrations, and regular monitoring of lithium serum concentrations. The effective serum concentration must be established before pregnancy. If a therapeutic concentration has not been established, the lithium dose is titrated to a concentration within the therapeutic range. Breast feeding is discouraged in women taking lithium because of the high rate of transmission to the infant.
ConclusionsTreatment decisions for pregnant women with mood disorders must weigh the potential for increased risks of lithium during pregnancy, especially during the first trimester, against its effectiveness at reducing relapse.
Disclosure of InterestNone Declared
Clozapine use in drug induced psychosis in Parkinson´s disease: a case report and review of literature.
- A. Sanz Giancola, P. Setién Preciados, E. Arroyo Sánchez, I. Romero Gerecther, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The occurrence of psychotic symptoms induced by dopaminergic drugs marks a new phase in the course of Parkinson’s disease (PD). The term drug induced psychosis may be used when other significant psychiatric diseases are excluded in patients with no history of psychosis. The prevalence of dopaminomimetic psychosis varies from 5% to 20%. Therefore, knowledge of the psychopharmacological management of this condition is essential.
ObjectivesThe purpose of this case report and literature review is to to learn the psychopharmacological management of this not uncommon medical complication.
MethodsDescriptive case study and review of literature
ResultsWe present the case of a 71-year-old man with a medical history of Parkinson’s disease with partial response to treatment with high doses of levodopa and carbidopa.
He was brought to the emergency department by his family due to the presence of behavioural alterations at home.
The patient reported seeing men in foam trying to harm his family. In a disjointed way in his speech, he links this idea with the delusional belief that he is being watched by electronic devices placed throughout the house. In a variegated manner he links this with a coelotypical type of discourse, however the delusional ideation remains unstructured throughout.
With no previous personal or family history of mental health and ruling out underlying organic conditions, a diagnosis of psychosis secondary to pharmacological treatment for Parkinson’s disease is presumed.
Considering the risks and benefits, it was decided to maintain the anti-Parkinson’s dose in order to avoid worsening the patient’s motor function. Therefore, after reviewing the literature, the best option was to introduce clozapine at low doses, up to 50 mg at night, with the respective analytical control. After a week’s admission, the patient began to improve psychopathologically, achieving an ad integrum resolution of the psychotic symptoms.
ConclusionsDespite the availability of other antipsychotic treatments such as quetiapine or the more recent pimavanserin, clozapine remains the treatment of choice for drug-induced psychosis in Parkinson’s disease.
Disclosure of InterestNone Declared
Psychotic denial of pregnancy: case report and narrative literature review.
- M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral, E. Arroyo Sánchez, A. Sanz Giancola, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the phenomenon where a woman fails to recognize or accept her pregnancy at >20 weeks gestational age. It associates with increased morbidity and mortality of mother and child, and can be classified as non-psychotic or psychotic. There is fewer medical literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data regarding incidence nor approved interventions or treatment.
ObjectivesTo describe this unfamiliar entity in order to be able to perform a proper diagnosis and thus prevent possible negative outcomes.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, with an advanced pregnancy, who was admitted to a Psychiatry in-patient unit due to psychotic symptoms such as mistrust and delusions. She showed scarce collaboration during assessment and did not give any plausible information about her identity. Her birthplace and prior medical records were therefore unknown. Apparently, she had no family nor social support network. Despite the obvious signs, she did not recognize being pregnant and showed great irritability when asked; her responses ranged from claiming she was suffering from a gastric tumor and making delusional attributions of symptoms clearly related to the pregnancy to partially acknowledging her state but refusing to answer any questions on the matter. Blood work showed no significant abnormalities and obstetric ultrasound revealed a low risk 35 weeks pregnancy.
With an estimated prevalence of 1:475 in general population, denial of pregnancy is not as rare as it may seem. The psychotic variant, however, is rather uncommon. Typically, women with psychotic pregnancy denial have prior history of major mental illness, most frequently schizophrenia, and suffer from extreme psychosocial vulnerability. They usually present previous or anticipated child custody loss, which hampers the process of developing antenatal attachment behaviours. Psychotic denial does not associate with concealing, since these women are mentally detached from the gestation and tend to create delusional explanations to their pregnancy symptoms. Not all of them show complete denial, some being able to acknowledge it, though mostly in an inconsistent way. These patients often fail to seek prenatal care or are noncompliant, they are at greater risk of drug exposure, and some are unable to recognize symptoms of labour, all of which increases the rate of negative outcomes for mother and baby, including neonaticide.
ConclusionsPsychotic denial is a rare diagnosis which should be properly assessed due to its clinical implications and the need to prevent potential negative outcomes for mother and baby.
Disclosure of InterestNone Declared
Application of family therapy in a case of anorexia nervosa
- C. Díaz Mayoral, I. Romero Gerechter, E. Arroyo Sánchez, M. Martín Velasco, A. Sanz Giancola, M. Martín de Argila
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S848
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is a behavioral mental disorder, characterized by body dysmorphia, an intense fear of gaining weight and behaviors that interfere with this, in addition to a restriction of food intake, associated usually with medical complications, even a considerable risk of death.
Several psychotherapeutic approaches have been used along last decades. Until relatively recently, parents have been recognized as part of the problem, but nowadays we involve them into the therapeutic process through family therapy based on a systemic approach, recommended in current published clinical guidelines and research findings, with consistent evidence, as the first-line treatment of patients with anorexia nervosa.
ObjectivesA case of a patient with anorexia nervosa, is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsA 24-yeard-old female was hospitalized for renutrition due to a significant weight loss and multiple physical symptoms. After 4 months without progress, the patient was transferred to the psychiatric ward.
Once there, physical stabilisation was achieved with family therapy and pharmacological treatment, based on progressive administration of Clomipramine, previously assessed by Cardiology, which improved rumination and obsessive behaviour. We conduct daily individual and weekly family interviews, working on family dynamics, emotional regulation strategies and more adaptive ways of communication. Likewise, several lines of action were found in the systemic work: peripheral father; maternal over-involvement; fraternal rivalry; difficulties of interaction between all of them, derived from “the role of the sick person” and intra-family communication around the illness. Finally, showed effectiveness in terms of an improvement in interpersonal relationships, greater assertiveness and an optimistic attitude with an active search for coping strategies.
ConclusionsHistorically, parents have been recognized by a causal factor in the pathogenesis of this disorder. Nevertheless, the abolition of the emphasis on family responsibility, motivated by a philosophic and evidence-based, has allowed us to see them as an essential resource in aiding the patient in the improvement process. This parental involvement has resulted in a relevant reduction in morbidity, as well as a significant decrease treatment attrition rates. It has been noted a re-establishment in other individual and family factors such as self-esteem, quality of life, and some aspects of the experiences of caregiving, and behavioral symptoms have been resolved.
Disclosure of InterestNone Declared
Mania induced after corticosteroid treatment: a case report
- E. Arroyo Sánchez, A. Sanz- Giancola, P. Setién Preciados, I. Romero Gerechter, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S697
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are drugs widely used in clinical practice for their anti-inflammatory and immunosuppressive properties. Despite their beneficial effects, a high association of these drugs with neuropsychiatric adverse effects such as psychosis, mania, depression, delirium or increased risk of suicide, among others, has been observed. We present the case of 54-year-old man who started treatment with hydroaltesone 20 mg/8h after undergoing surgery for a pituitary macroadenoma who began with maniform clinic.
ObjectivesTo know the prevalence, risk factors and treatment of mania as a side effect of corticosteroid drugs.
MethodsPresentation of the case and review of the available literature on the risk of developing mania after corticosteroid treatment.
ResultsSeveral studies confirm that the incidence of psychiatric adverse effects after the use of corticosteroids is around 6% if we refer to severe reactions; 28% moderate reactions; and 72% if we consider milder reactions. The direct relationship between these drugs and affective symptoms ranges in rates between 1-50% of cases, the most frequent being depression and mania. The risk of mania after treatment with corticosteroids is 4-5 times higher than if we compare it with a group of population not exposed to these drugs. There is a dose-response relationship, increasing the risk from a daily dose of 40 mg/day, with an average duration of symptoms of around 21 days. Female sex seems to be a risk factor in relation to the fact that diseases requiring this type of treatment are more common in this gender. As first-line treatment for mania secondary to corticosteroids, a decrease in treatment dose or its interruption, whenever possible, is proposed. Adjuvant treatment may be required, with atypical antipsychotics being the first choice.
ConclusionsCorticosteroid therapy has a direct dose-response relationship with the presence of psychiatric adverse effects such as mania. Dose and sex have been studied as possible adverse effects. Therefore, the pharmacological treatment of choice consists of a reduction in the dose of corticosteroids administered or withdrawal, if possible, and may be combined with an atypical antipsychotic such as olanzapine, quetiapine or risperidone. Re-evaluation is recommended until complete resolution of the clinical picture and then antipsychotic treatment can be progressively withdrawn.
Disclosure of InterestNone Declared
Psychotic symptoms in eating disorders: a case report
- E. Arroyo Sánchez, P. Setién Preciados, A. Sanz- Giancola
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S848-S849
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic symptoms and eating disorders can occur in the same person, sometimes at the same time. This comorbidity is not well studied despite the difficulties of management at both clinical and pharmacological levels that it may entail. We present the case of a 35-year.old female patient with anorexia nervosa with years of evolution, currently admitted to a center specializing in Eating Disorders, who comes to the emergency department with psychotic symptoms.
ObjectivesTo know the prevalence of comorbidity of psychotic symptoms in people with eating disorders, as well as possible risk factors, severity and management of them.
MethodsPresentation of a case and review of the available literature on the presence of symptoms of the psychotic sphere in persons diagnosed with eating disorders.
ResultsThe literature reflects data of a prevalence of 10-15% of patients with eating disorders presenting psychotic symptoms. The presence of psychotic symptoms is not directly related to a greater severity of the eating disorder. Some genetic associations have been found, as well as alterations at the physiological, cognitive and brain structure level that coincide in both pathologies. In some cases, an improvement in eating behavior has been observed when the psychotic symptomatology is resolved. In the case of patients with bulimia nervosa, a higher number of psychotic symptomatology has been observed, such as paranoid ideations, which some studies relate to a greater emotional capacity and histrionic expressiveness of this patient profile.
ConclusionsThe comorbidity of psychotic symptoms and eating disorders is relatively frequent and makes us face challenges in the diagnosis, as well as in the management of these patients. This comorbidity is especially important in patients with bulimia nervosa. Future research is necessary to know a more exact management of these pathologies.
Disclosure of InterestNone Declared
Hysteria in neurology: a diagnostic approach to conversive disorder
- A. Sanz Giancola, I. Cuevas Iñiguez, C. Alvarez Garcia, M.D.C. Molina Liétor, M. Blanco Prieto
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S395
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Conversion disorder (a term that describes what was previously called hysteria) refers to motor or sensory symptoms, or both, that resemble a neurological disease, but that do not originate from or cannot be explained by a known physical disease.
ObjectivesTo find reliable tools that can guide the difficult diagnosis of conversion disorder.
MethodsBibliographic review
ResultsThe exact prevalence of the disorder is unknown. It is estimated that approximately 5% of referrals to neurology are for this disorder. Approximately one third of patients referred to the neurologist have symptoms that cannot be explained by an organic disease. Involuntary movements are the most common motor manifestations of the conversive syndrome, being tremor one of the most frequent manifestations. The first differential diagnosis of conversion disorder is neurological disease. It is currently not necessary for the diagnosis to assess whether or not the symptoms are produced intentionally, as the assessment of conscious intentionality is unreliable. The neurological examination is the fundamental tool for the diagnostic approach, being even more enlightening than the complementary tests. Hoover’s sign, Babinski’s combined leg flexion, plantar flexion of the ankle, tremor and its distraction and synchronisation manoeuvres, as well as the clinical differences between epileptic seizures and non-epileptic seizures of psychogenic origin, are some of the reliable tools for a correct diagnosis.
ConclusionsThe diagnosis of the disease should be one of exclusion. There must be clinical data showing clear evidence of incompatibility with a neurological disease and conversion symptoms do not correspond to known physiological mechanisms and anatomical pathways.
DisclosureNo significant relationships.
Proposal of a therapeutic algorithm for the psychopharmacological management of treatment-resistant depression
- A. Sanz Giancola, M.D.C. Molina Liétor, I. Cuevas Iñiguez, C. Alvarez Garcia, M. Blanco Prieto
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S567
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The lack of a standardised definition for the concept of TRD and an adequate criteria for therapeutic response make difficult the management of patients with MDD who do not achieve remission with one or more courses of treatment. All classifications suggested to define TRD are arbitrary, partially evidence-based, subordinated to the pharmacological findings of the time in which they are written and with serious inconsistencies, making it difficult to construct a universal and enduring diagnostic system.
ObjectivesConsidering that the most important goal in treating a patient with Major Depressive Disorder (MDD) should be remission and return to previous functionality, the search for a standardised, evidence-based classification system will allow timely and effective interventions leading to the reduction of this devastating condition.
MethodsBibliographic review
ResultsThe proposed therapeutic algorithm arises from the combination of several fundamental principles for the management of treatment-resistant depression: the different classification systems of the concept, as well as the concepts of response, relapse, recurrence and remission; the scientific evidence found in the current literature, routine clinical practice, knowledge of switching and augmentation strategies, the new pharmacological targets and neurobiological hypothesis discovered, without forgetting finally the different clinical profiles of depressive symptomatology and the specific indications of each antidepressant.
ConclusionsResistant depression is difficult to treat successfully and is not a uniform entity. Recently there has been a move to characterise treatment-resistant depression as ‘difficult-to-treat’ depression on the basis that the former description implies that depression treatments are normally effective and that non-response is therefore somehow abnormal.
DisclosureNo significant relationships.
Functional Neurological Disorder: a multidisciplinary approach
- C. Alvarez Garcia, A. Gomez Martín, M.D.C. Molina Liétor, I. Cuevas Iñiguez, A. Sanz Giancola
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S396
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Functional neurological disorders (FNDs), also known as “conversion disorder”, consist in the appearance of neurological symptoms that do not correspond to any medical condition and produces an impairment in social, occupational and other areas in the patient’s life. This disorder can represent up to 30% of neurologist’s consultation. We introduce the case of a 23-year-old man who attended the emergency services due to fainting and was finally diagnosed with FND.
ObjectivesTo summarize the difficulties of making a diagnosis of FND and the importance of a multidisciplinary approach.
MethodsA narrative review through the presentation of a case.
ResultsThe patient presented many absence seizures during his stay in the hospital. These episodes were characterized by non-reactivity, dysarthria, tremors, tachycardia and hyperventilation. The neurological examination and imaging tests didn’t show any pathological findings. During the psychiatric interview he revealed he had lived a severe conflict with his brothers the previous week and he was being excluded within his family. Furthermore he didn’t have any social support besides his mother in the city he was living, leading this situation to an incrementation of anxiety. Due to the absence of any abnormalities in the examination and recent psychological conflict that was affecting him, FND diagnose was made.
ConclusionsVery frequently the absence of a clear psychological trigger and the presence of neurological alterations can hinder the study of the patient. This makes necessary a multidisciplinary approach and the knowledge of signs that can help to carry out an accurate diagnosis.
DisclosureNo significant relationships.
Hysteria: history of a conceptual and clinical pathomorphosis
- A. Sanz Giancola, C. Alvarez Garcia
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S545-S546
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Transhistorical psychiatry defends that a psychic alteration can be interpreted as a cultural, historical and personal construction, subject to incessant variations.
ObjectivesA journey through the history of the disorder and the successive pathomorphoses it has undergone could provide us with a better understanding of it and explain the reason for the epidemiological trend towards a decrease in its diagnosis; and bring us closer to a universal definition of the phenomenon.
MethodsBibliographic review
ResultsThe word hysteria and all its subsequent meanings, not only contain a particular conception of the pathology, but also reflect its different forms of presentation in specific periods of time. Hysteria is presented as a voluble material that can take on any form: from the wandering womb theory of classical Greece to the demonic possessions of the Middle Ages; from the neurological degeneration of Charcot (1825-1893) to the conversion and dissociation of Freud (1856-1939). With the entry of the 20th century, its dramatic clinic has been progressively overshadowed by somatoform disorders and emerging functional somatic syndromes. Today, it is practically unrecognisable and very difficult to diagnose, to the point of having disappeared as a term from the official classifications of our time.
ConclusionsHysteria is an entity that has not always been the same, neither in its conception nor in its manifestations. Depending on the socio-cultural context in which it is framed, it will be interpreted and expressed in different ways.
DisclosureNo significant relationships.
Dealing with Posttraumatic Nightmares
- C. Alvarez Garcia, L. Nocete Navarro, A. Sanz Giancola
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S674
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Posttraumatic nightmares are one of the most frequent symptoms in posttraumatic stress disorder. Prevalence can be up to 96%. These nightmares evoke the experienced traumatic event, causing a negative impact. Besides, they are and independent risk for suicide. There are different pharmacological and non-pharmacological options for PTN, despite is no optimal treatment.
ObjectivesTo analyse the different treatment options for PTN.
MethodsThis was a narrative literature review.
ResultsThe two main treatments for PTN nowadays are the Imagery Rehearsal Therapy (IRT) and prazosin. IRT is a cognitive-behavioral intervention, that helps the patient to change the content of the nightmare to a “happier ending”. Prazosin is an alpha-adrenergic receptor antagonist that blocks the stress response in the central nervous system receptors. Although it was a promising drug, significant differences compared to placebo have not been found. There is growing data that suggests nabilone, a synthetic cannabinoid, could be helpful in PTN treatment. A clinical trial made in Canada revealed that 72% of patients experienced a complete disappearance or at least an important reduction of PTN.
ConclusionsPTN is a very common and distressing symptom in patients presenting PTSD. Nevertheless, there is no treatment with enough evidence for this pathology. On this account, it is fundamental to do more research in order to find and suitable treatment that can improve the quality of life of these patients.
DisclosureNo significant relationships.
Griefing reaction and social networks
- M.D.C. Molina Liétor, M. Martín, I. Cuevas Iñiguez, I. Romero Gerechter, A. Sanz Giancola
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S577
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Grief is a normal and not necessarily pathological psychological process that occurs after the loss of a family member or loved one with its psycho-affective consequences, external manifestations and rituals. Although mourning processes can be associated with losses of different types (employment, housing, baseline situation, housing), we will refer to mourning for the loss of a loved one. For some people, social networks facilitate the expression of feelings and experiences of grief, connecting with the emotional support of other friends and loved ones. However, the presence of accounts belonging to these deceased persons, the persistence of photos and memories that periodically appear on the screen without the person being able to choose them, can make it difficult to process the mourning.
ObjectivesThe aim of this paper is to consider the beneficial and detrimental factors of social media during a grieving reaction after the loss of a loved one.
MethodsFor the preparation of this work, a bibliographic review on the subject has been carried out. Likewise, the clinical information provided by patients during our evaluations has provided critical views on what has been published in this regard.
ResultsSupport through social networks can help to feel more affectionate, but there are other harmful factors that must be taken into account: permanence of photos, appearance of memories and reminder of the deceased person’s birthday.
ConclusionsSocial networks can have favorable but also detrimental factors in the elaboration of a grief and should be considered in the psychiatric exploration and intervention.
DisclosureNo significant relationships.
Image testing in psychiatrics: a bibliografic review
- M.D.C. Molina Liétor, I. Cuevas Iñiguez, A. Sanz Giancola, C. Alvarez Garcia
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychoradiology is a term that describes a growing interest in relating psychiatry and radiological images, proposing a radiological approach in the management of major psychiatric illnesses. This includes the diagnosis, the planning of the treatment and the study of the clinical course.
ObjectivesThe objective of this communication is to review the current status of the importance and indications of neuroimaging tests in psychiatry.
MethodsA literature review has been carried out to review this issue.
ResultsIn schizophrenia, longitudinal studies have been carried out that compare the anatomical structures between a first psychotic episode and in a chronic state, locating regional changes that progress as the disease does. Anatomical alterations have also been detected among patients with a predominance of positive symptoms or negative symptoms. Although more and more studies demonstrate a certain common genetic and radiological basis between bipolar disorder and schizophrenia, imaging techniques can also show specific findings that differentiate one pathology from the other. The neuroimaging tests used in psychiatry are: • Brain CT, recommended when a first psychotic episode is suspected. • MRI: recommended in processes of cognitive deterioration, to evaluate white matter and for pregnant patients. It is also recommended to evaluate injuries that could have a poor prognosis with the application of electroconvulsive therapy. • Functional tests (PET and SPECT) are often used to screen some types of dementia such as Alzheimer’s or for research.
ConclusionsNew advances and knowledge in psychiatry and radiology must be integrated for better clinical practice.
DisclosureNo significant relationships.
Ischemic colitis induced by psychotropics drugs: a case report
- C. Alvarez Garcia, A. Sanz Giancola, L. Nocete Navarro
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S710
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Ischemic colitis (IC) is a rare condition due to hypoperfusion in the large intestine. Usually the etiology is unidentified, but many drugs are known to induce it because of their anticholinergic effects. We present the case of a 63-year-old woman, with the diagnosis of histrionic personality disorder, in treatment with quetiapine and venlafaxine. She attended the hospital due to diffuse abdominal pain, diarrhea and hematochezia in the last two days. An abdominal CT scan is made, showing parietal thickening and submucosal edema in the colon, without any tumoral findings, suggesting IC.
ObjectivesTo point up the correlation between IC and the intake of psychotropic drugs.
MethodsWe conducted a narrative review of the literature through the presentation of a case. Articles were selected based on their clinical relevance.
ResultsThere are reported cases of IC related to antipsychotics, but any drug with anticholinergic effects can potentially cause it. Anticholinergics reduce intestinal motility, leading to colonic ileus and dilatation. Both quetiapine and venlafaxine, taken by the patient, have these effects. Common obstructive and non-obstructive processes are excluded due to the absence of any other pathological signs. For these reasons, the diagnosis of IC secondary to treatment with quetiapine and venlafaxine is made.
ConclusionsMany psychotropic drugs can produce IC owing to their anticholinergic effects, being this chance increased when taken simultaneously with other drugs with same effects. IC is a rare but fatal side effect, which makes it important to consider it in the differential diagnosis in patients in treatment with psychotropics who suffer from gastrointestinal symptoms.
DisclosureNo significant relationships.
The overlap between complex posttraumatic stress disorder and borderline personality disorder
- C. Álvarez García, L. Nocete Navarro, M.D.C. Molina Lietor, I. Cuevas Iñiguez, A. Sanz Giancola
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S754
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Research has shown the relationship between borderline personality disorder (BPD) and complex posttraumatic stress disorder (cPTSD), pointing out the overlapping nature and expression of both conditions. In order to understand their differences and similarities, we present a case of a 22-years-old patient with a history of repeated sexual trauma throughout all her adolescence, whose diagnose was changed from BPD to cPTSD after she was admitted in an acute inpatient mental health unit.
ObjectivesTo gather the similarities between borderline personality disorder and complex posttraumatic stress disorder.
MethodsA narrative review of the literature through the presentation of a case. Articles were chosen based on its clinical relevance.
ResultscPTSD merges the clinical features and symptoms of PTSD with affect dysregulation, negative self-perception, unstable relationships and somatization, also present in BPD. Furthermore, BPD is known to frequently have a traumatic etiology.
ConclusionsIt is not always simple to draw a clear line between cPTSD and BPD conditions. However, each diagnosis may have a different impact on patient understanding and treatment.
DisclosureNo significant relationships.
Electroconvulsive therapy in the medical comorbidities context: A case report
- A. Sanz Giancola, M.D.C. Molina Lietor, M. Blanco Prieto, N. Freund Llovera, L. Nocete Navarro, I. Cuevas Iñiguez, C. Álvarez García
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S689-S690
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Electroconvulsive therapy (ECT) is today one of the main treatments available and used in psychiatry for serious mental illnesses. Eighty years after its introduction, the ECT procedure has evolved to become a safe option based on scientific evidence. Nowadays there are no absolute contraindications for ECT, regardless of the type of population and clinical situation.
ObjectivesTo illustrate the electroconvulsive therapy in medical comorbidities context with a case report.
MethodsDescriptive case study.
ResultsWe present a 66 years old patient who suffers from a psychiatric decompensation with a diagnosis of major depressive disorder with psychotic symptoms. Due to her cardiological history (prolongation of the QT interval of possible psycopharmacological origin and a 2:1 AV block, that required the implantation of a definitive pacemaker) and partial response to psychotropic medication, the initiation of electroconvulsive therapy is proposed as the best alternative. The pacemaker was previously studied by cardiology for a very complete analysis before the procedure. It was recommended to convert it to fixed rate pacing by using a magnet. To do this, we placed it over the pacemaker during the technique. While waiting for a clinical improvement, no incidence has been produced during the sessions.
ConclusionsECT should not be postponed as a last resort. Numerous studies conclude that ECT is globally the treatment of choice (70-85% response) in severe depressive conditions, over and above antidepressant drugs. The incidence of relevant cardiac complications on ECT is relatively rare (0.9%). Regarding the use of pacemakers, electroconvulsive therapy represents an effective and safe option for the patient.
DisclosureNo significant relationships.





