4 results
Are there any differences in clinical and biochemical variables between bipolar patients with or without lifetime psychotic symptoms?
- C. M. Esposito, A. Ceresa, M. Di Paolo, T. Surace, L. Moioli, F. Legnani, G. Nosari, V. Ciappolino, A. M. Auxilia, M. Cappellazzi, I. Tagliabue, L. Cirella, E. Capuzzi, A. Caldiroli, A. Dekanalis, M. Clerici, M. Buoli
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S505-S506
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar Disorder (BD) is a frequent psychiatric disorder, which can be associated with high disability. Psychotic symptoms occur in more than half of bipolar patients and are associated with an unfavorable course of the disorder (Chakrabarti et al. World J Psychiatry 2022; 12(9) 1204-1232).
ObjectivesThe aim of this study is therefore to identify clinical and biological markers able to discriminate between BD patients with (BD-PS) and without lifetime psychotic symptoms (BD-NPS) to facilitate early diagnosis and to implement a target clinical management of these patients.
MethodsWe recruited 665 patients consecutively hospitalized for BD at Fondazione IRCCS Policlinico (Milan) and at San Gerardo Hospital (Monza). Data were obtained through a screening of the clinical charts and blood analyses conducted during the hospitalization. Patients were assessed by psychometric scales. The two groups (BD-PS and BD-NPS) were compared by t tests for quantitative variables and χ2 tests for qualitative ones. Variables that resulted to be significant in univariate analyses were inserted in binary logistic models with the presence of psychotic symptoms as dependent variable.
ResultsAmong the total sample, 64.5% of patients were affected by BD-PS while 35.5% by BD-NPS. The final binary logistic regression model showed that, compared to patients with BD-NPS, those with BD-PS had a longer duration of hospitalization (p=0.007) and were more frequently hospitalized for a manic episode (p=0.001). In addition, subjects with BD-PS had a lower score on the current Global Assessment of Functioning (GAF) (t = 3.157; p = 0.002) and were more frequently males (χ² = 4.061; p = 0.044; OR = 1.399). With regard to biological variables, patients with BD-PS, compared to the counterpart, had a higher Neutrophile to Lymphocyte Ratio (NLR) (t = 2.776; p = 0.006), lower levels of Gamma-Glutamyl Transferase (γGT) (t = 2.249; p = 0.026), higher total bilirubin (t = 2.348; p = 0.019) and creatine phosphokinase (CPK) (t=2.807; p = 0.005), lower total cholesterol (t = 2.369; p = 0.018) and triglycerides (t = 2.554; p = 0.013).
ConclusionsOur data appear to be in line with the literature, especially with respect to the occurrence of psychotic symptoms mainly in manic episodes and their association with greater clinical severity, longer hospitalization and worse outcome (Altamura et al. Aust N Z J Psychiatry 2019; 53(8) 772-781). From a biological point of view, it seems important to emphasize that patients with lifetime psychotic symptoms presented a higher NLR, revealing more prominent low-grade inflammation in these patients than the counterpart. These data confirm the possibility of using NLR as biomarker of severity in bipolar patients, as proposed previously by other authors (Kulacaoglu et al. Nord J Psychiatry 2022). Future multi-center study have to confirm the results of the present study.
Disclosure of InterestNone Declared
Clinical and biochemical parameters associated with substance-induced psychotic disorder: which differences between alcohol, cannabis and psychostimulants
- G. Nosari, A. Ceresa, M. Di Paolo, C. M. Esposito, V. Ciappolino, A. Calabrese, F. Legnani, A. M. Auxilia, M. Capellazzi, I. Tagliabue, L. Cirella, E. Capuzzi, A. Caldiroli, A. Dakanalis, M. Clerici, M. Buoli
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S514-S515
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
According to DSM V, substance-induced psychotic disorder is a mental health condition in which the onset of psychotic symptoms can be traced to the use of a psychotropic substance. The pathogenesis of this disease is still poorly understood; current literature traces its causes back to genetic predisposition and early traumatic events (i.e. child abuse).
ObjectivesThe present study aims to identify specific clinical features and biochemical markers which could be addressed as predictors for the long-term prognosis of this disease. Moreover, we aim to identify specific correlations between the clinical phenotype and the underlying substance abuse, in order to allow the early start of a tailored treatment.
MethodsBetween 2020 and 2022 we recruited 218 patients referring to the Policlinico Hospital in Milan and the San Gerardo Hospital in Monza, Italy. All the patients were diagnosed with substance induced psychotic disorder: 31 reported alcohol abuse (14,2%), 71 psichostimulants (32,6%), 116 cannabis, (53,2%). For each patients, we collected demographic data, medical records and a comprehensive psychometric assessment (GAF, PANSS, BPRS, Modified Sad Person Scale-MOAS). Furthermore, we collected a blood sample for dosing Na+, K+, Na+/K+, hemogram with formula and platelets, glucose , urea, creatinine, uric acid, transaminases, γGT, bilirubin, plasma proteins, albumin, LDH, CPK, PCHE, cholesterol, HDL, LDL, Tg, TSH.
ResultsChi squared test (χ²) has been used to compare qualitative variables between the 3 subgrous (alcohol-, psychostimulants- and cannabis-induced psychotic syndromes) (fig.1). One way ANOVA test has been used to compare quantitative variables between the same 3 subgroups (fig.2). After removing one of the subgropus (alcohol-induced psychotic symptoms), the same analysis have been repeated. Significant variables have been included in a binary logistic regression model in order to confirm their validity as predictors for cannabis- and psychostimulants-induced psychotic disorders (fig 3). Finally we performed Omnibus test and Hosmer-Lemeshow test in order to verify the validity of these regression models.
Image:
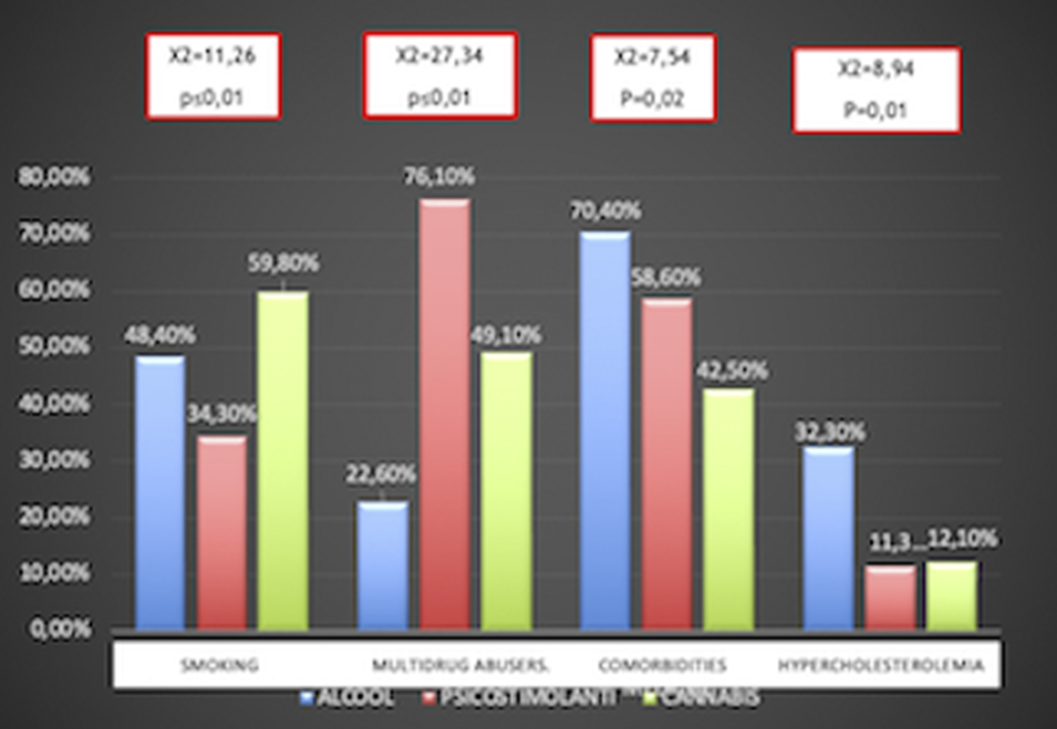
Image 2:
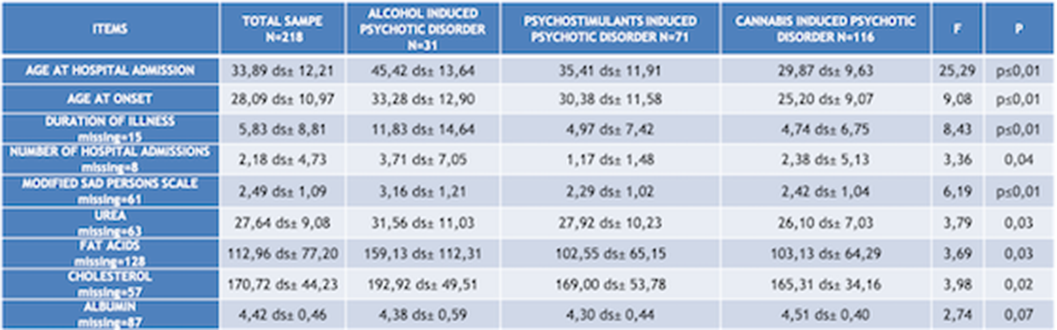
Image 3:
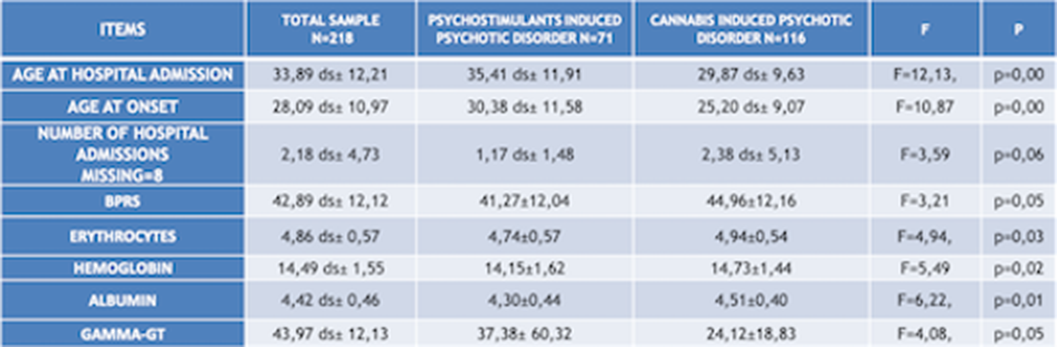 Conclusions
ConclusionsFor each considered subgroups, we indentified the following features. Alcohol induced psychotic syndrome: higher age of onset and age of hospital admission, higher cholesterol and hurea levels, , high comorbidity with medical conditions anxiety/depression, low social functioning, higher suicidal risk;, higher hospitalization rate. Cannabis induced psychotic syndrome: higher hemoglobin and albumin levels, more severe psychiatric symtoms (BPRS), higher smoking rates. Psychostimulants induced psychotic syndrome: higher multi-drug abuse risk. We could assume that according to this consideration the treatment protocols for each of these subgroups should be tailored according to their specific features.
Disclosure of InterestNone Declared
Unequal access and unmet need: neurotic disorders and the use of primary care services
- P. E. BEBBINGTON, H. MELTZER, T. S. BRUGHA, M. FARRELL, R. JENKINS, C. CERESA, G. LEWIS
-
- Journal:
- Psychological Medicine / Volume 30 / Issue 6 / November 2000
- Published online by Cambridge University Press:
- 16 November 2000, pp. 1359-1367
-
- Article
- Export citation
-
Background. In this paper we use data from the National Survey of Psychiatric Morbidity to examine how many people with neurotic disorders receive professional evaluation, and how this is affected by clinical and sociodemographic differences. We hypothesized that psychiatric symptoms and attendant dysfunctions would both have an effect on contacting, and that key demographic variables would not.
Method. The household component of the British National Surveys of Psychiatric Morbidity was based on a random sample of > 10000 subjects. Psychiatric symptoms and ICD-10 diagnosis were established by lay interviewers using the CIS-R. Social dysfunction was tapped by asking about difficulties in performing seven types of everyday activity. We examined symptom score, ADL deficit score and demographic variables in relation to contact with primary care physicians for psychiatric symptoms.
Results. The major determinant of contacting a primary care physician was severity, mainly due to the level of psychiatric symptoms, but with an independent contribution from social dysfunction. There were also significant contributions from sex, marital status, age, employment status and whether the subject had a physical condition as well.
Conclusions. The major influence on whether people seek the help of their family doctors for mental health problems is the severity of disorder. Although there are some social inequalities in access to family doctors, these are less important. The most salient finding from our study is that even people suffering from high levels of psychiatric symptoms very often do not have contact with professionals who might help them.
Neurotic disorders and the receipt of psychiatric treatment
- P. E. BEBBINGTON, T. S. BRUGHA, H. MELTZER, R. JENKINS, C. CERESA, M. FARRELL, G. LEWIS
-
- Journal:
- Psychological Medicine / Volume 30 / Issue 6 / November 2000
- Published online by Cambridge University Press:
- 16 November 2000, pp. 1369-1376
-
- Article
- Export citation
-
Background. Access to psychiatric treatment by people with neurotic disorders in the general population is likely to be affected both by the severity of disorder and by sociodemographic differences.
Method. In the household component of the National Surveys of Psychiatric Morbidity > 10000 subjects in Great Britain with psychiatric symptoms were interviewed using the CIS-R. They were also asked about difficulties experienced in performing seven types of everyday activity. All subjects classed as having an ICD-10 disorder were questioned about their experience of treatment with antidepressants, hypnotics, and counselling or psychotherapy.
Results. Less than 14% of people with current neurotic disorders were receiving treatment for them. Within the previous year, only a third had made contact with their primary care physician for their mental problem: of these < 30% were receiving treatment. Overall, 9% of people with disorders were given medication and 8% counselling or psychotherapy. A diagnosis of depressive episode was that most associated with antidepressant medication. Treatment access was affected by employment status, marital status, and age, but the major determinant was symptom severity. Neither sex nor social class influenced which people received treatment.
Conclusions. People with psychiatric disorders seldom receive treatment, even when they have consulted their primary care physician about them. In many cases, this must represent unmet needs with a strong claim on health resources. There are also inequalities in the receipt of treatment, although the major influence is the severity of disorder.






