4 results
Treatment of tardive dyskinesias with vitamin E: A case series
- B. Senol, F. N. Akarca, R. N. Ekinci, E. Goka
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1004
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Tardive dyskinesia is usually persistent, irreversible involuntary movement of the tongue, lips, face, trunk and extremities in patients taking long-term dopaminergic antagonist drugs. Although it is mostly associated with the use of neuroleptics, cases of tardive dyskinesia existed before the discovery of these agents. Patients with schizophrenia and other neuropsychiatric disorders are particularly at risk for tardive dyskinesia because they are exposed to neuroleptics and anticholinergic agents for longer periods than healthy individuals. Free radicals are thought to be probably involved in the pathogenesis of tardive dyskinesia. Vitamin E is a fat-soluble antioxidant, and it is thought to be effective in the treatment of antipsychotic-associated tardive dyskinesia, as it has a cytotoxic free radical-binding effect.
ObjectivesIn this poster presentation, it was aimed to evaluate the clinical results of the treatment of tardive dyskinesia with high-dose vitamin E in four inpatients with serious mental illness and long-term antipsychotic use. In addition, the treatment of tardive dyskinesia will be discussed in the light of current literature data.
MethodsIn the case report, there are three patients with schizophrenia and one with mild mental retardation. They were treated with 1600 IU of vitamin E per day. The patients continued their vitamin E treatment for 90 days. The severity of tardive dyskinesia of the patients was measured by Abnormal Involuntary Movement Scale (AIMS).
ResultsAt the end of the 90 day treatment, the AIMS measurements of the subjects decreased 72,7%, 73,3%, 72,2% and 80% respectively.
Image:
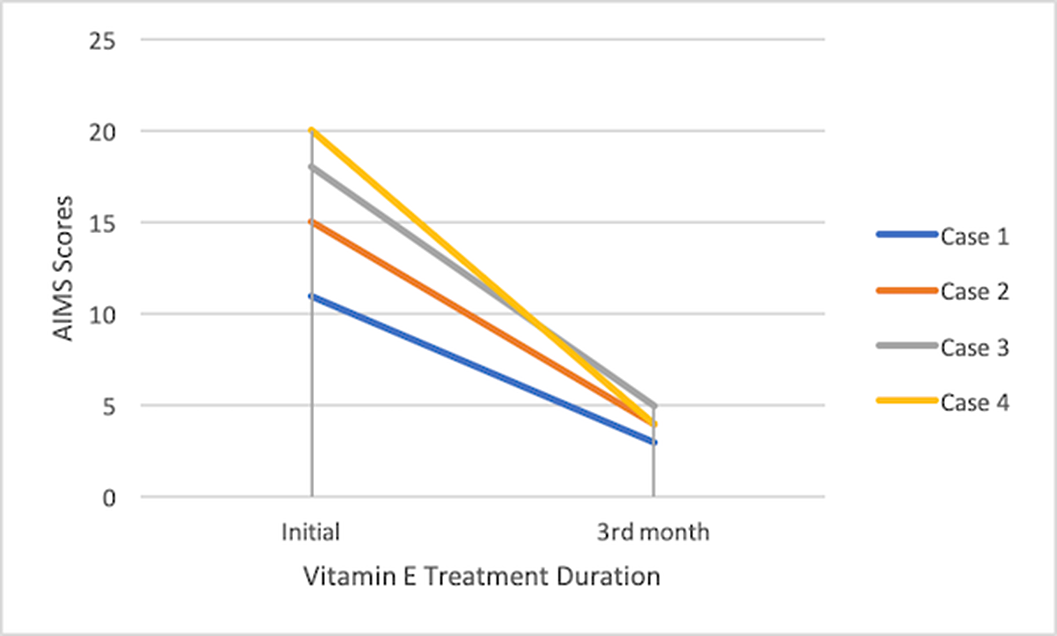 Conclusions
ConclusionsIn our clinic, we observed that patients using long-term typical antipsychotics were prescribed antipsychotics in unindicated situations or in high doses, patients with high risk for tardive dyskinesia were not taken into consideration when planning treatment, and we encountered cases of tardive dyskinesia despite the widespread use of atypical antipsychotic drugs in hospitalized patients. The use of benzodiazepines is restricted especially in elderly individuals due to their side effects and the risk of addiction in long-term use. Although the clinical importance of vitamin E is unknown, it is preferred because it can be used with a low risk of side effects, considering that it can prolong bleeding time. Although the results of a review of tardive dyskinesia treatment do not suggest that vitamin E reliably improves tardive dyskinesia symptoms, our experience shows that patients benefit from vitamin E treatment. In this regard, there is a need for studies that will be conducted with a large sample and compare the effectiveness of vitamin E with the treatments known to be effective in tardive dyskinesia.
Disclosure of InterestNone Declared
Neutrophil gelatinase-associated lipocalin (NGAL) and tumor necrosis factor-α(TNF-α) levels in patients with schizophrenia
- A. Gül Çakıl, H. Kaya, A. Sakallı Nural, I. B. Çakmak, I. T. Okay, E. Göka
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S254
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Although the immune system is thought to contribute to the etiology of schizophrenia, the mechanism has not been clearly elucidated. Clarifying the relationship between them is important in terms of diagnosis, treatment, and prevention approaches.
ObjectivesIn this study, it is aimed to determine whether there is any difference in serum levels of neutrophil gelatinase-associated lipocalin (NGAL) and tumor necrosis factor-alpha (TNF-α) in the group of patients with schizophrenia and healthy volunteers, whether these values are changed by medical treatment, whether there is any relation between these values and the severity of the symptoms of patients with schizophrenia, and whether NGAL can be used as a biomarker in the diagnosis and the follow-up of the schizophrenia.
MethodsA total of 64 patients who were hospitalized in the Psychiatry Clinic of Xxxxxx and diagnosed with schizophrenia and 55 healthy volunteers were included in the study. A sociodemographic information form was given to all participants and TNF-α and NGAL values were measured. Positive and Negative Symptoms Rating Scale (PANSS) were applied to the schizophrenia group on admission and follow-up. TNF-α and NGAL levels were re-measured in the 4th week after the start of antipsychotic treatment.
ResultsAs a result of the present study, it was found that NGAL levels decreased significantly after antipsychotic treatment of schizophrenia patients hospitalized with exacerbation (Figure 1). There was no significant correlation between NGAL and TNF-α levels among schizophrenia and the control group.
Image:
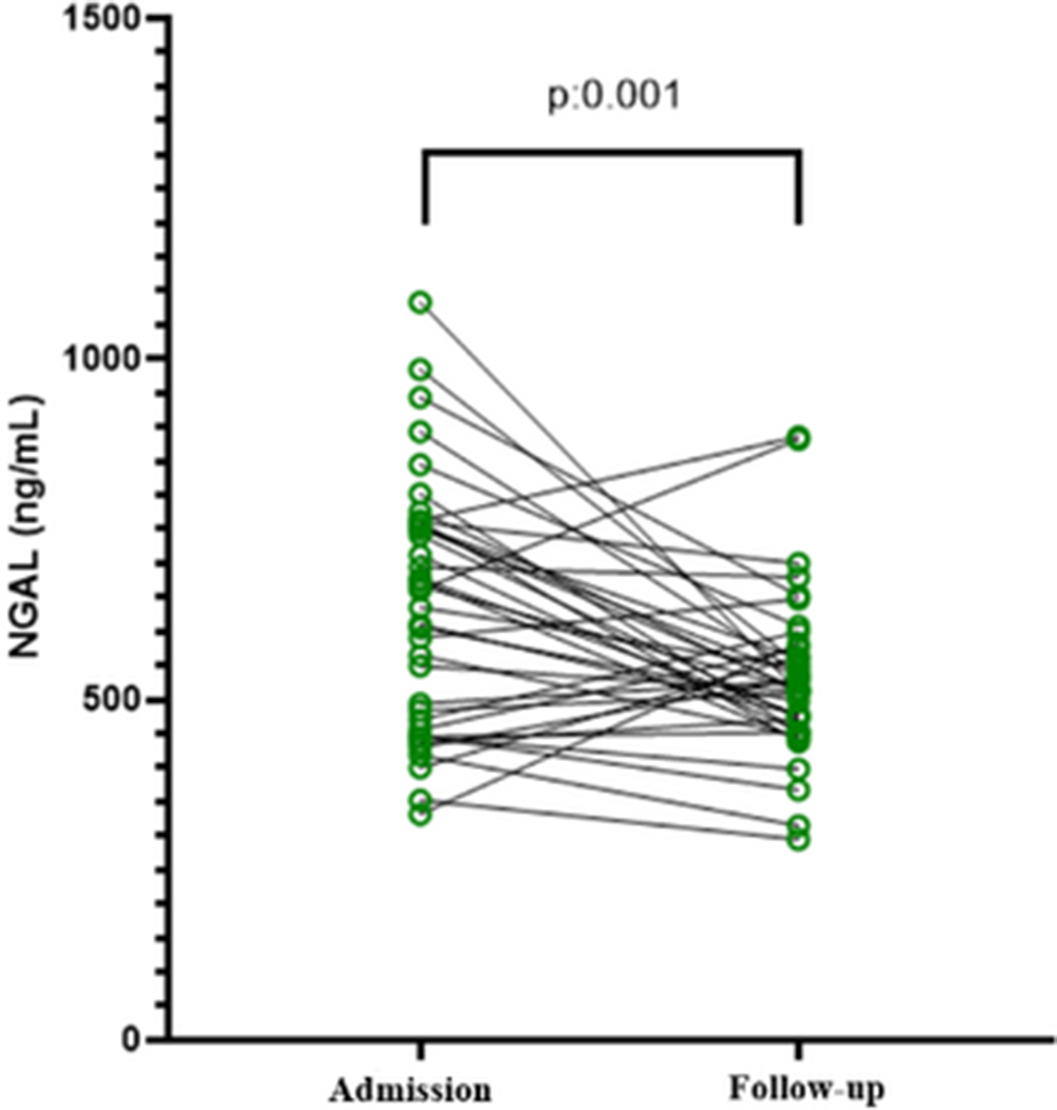 Conclusions
ConclusionsIn psychiatric diseases, especially schizophrenia, there may be differences in immune and inflammatory markers compared to the healthy population. After treatment, the NGAL levels of the patients at follow-up were reduced in comparison with the levels at their admission. It can be thought that NGAL may be related to psychopathology in schizophrenia and antipsychotic treatment. This is the first followup study for NGAL levels in schizophrenia.
Disclosure of InterestA. Gül Çakıl Grant / Research support from: This study funded by the Turkish Republic SBU Scientific Research Projects Coordinatorship. (Project no: 2020/013), H. Kaya: None Declared, A. Sakallı Nural: None Declared, I. Çakmak: None Declared, I. Okay: None Declared, E. Göka: None Declared
Assessment of Serum IL-4, 15d-PGJ2, PPAR Gamma Levels in Patients with Bipolar Disorder
- G. Erzin, Ç. aydemir, R. yüksel, E. tatlıdil, B. Çakır, S. sezer, E. göka
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S75
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Many hypotheses have been proposed about development of bipolar disorder including inflammatory processes due to the external and endogenous factors. There are strong evidences that immunological dysfunction is present in bipolar disorder. In the pathophysiology of bipolar disorder, there are many data that support the inflammatory hypothesis.
ObjectivesIn this study, to clarify the etiology of bipolar disorder, based on the inflammatory process hypothesis, it is aimed to measure and evaluate serum 15d-PGJ2 and PPARγ, anti-inflammatory cytokine IL-4 levels in patients with bipolar disorder.
MethodsThis study was performed at Ankara Numune Training and Research Hospital. Ninety-five patients are included in the study that were in their mania or remission periods and meet the DSM-V criteria for bipolar disorder. Forty-four healthy volunteers are included in the study as well. Serum IL-4, 15d-PGJ2, PPARγ levels are measured in both groups. Young Mania Scale, Hamilton Depression Scale, demographic data form were given to patient group.
ResultsIn our study, 15d-PGJ2, PPARγ levels were found statistically significantly lower in patients with bipolar disorder compared to healthy controls.
ConclusionThere are differences in anti-inflammatory prostaglandin levels in patients with bipolar disorder who are in their mania period when compared to healthy controls and patients in their remission period. This does not show any significance according to smoking and gender. This implies that inflammation markers could be a good candidate to determine trait markers, which will provide an insight for preventing patient from mania period or prognosis after the diagnosis of bipolar disorder.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Single, dual and multiple respiratory virus infections and risk of hospitalization and mortality
- E. A. GOKA, P. J. VALLELY, K. J. MUTTON, P. E. KLAPPER
-
- Journal:
- Epidemiology & Infection / Volume 143 / Issue 1 / January 2015
- Published online by Cambridge University Press:
- 24 February 2014, pp. 37-47
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Respiratory virus infections cause a significant number of hospitalization and deaths globally. This study investigated the association between single and multiple respiratory virus infections and risk of admission to a general ward, intensive care unit or death in patients aged 0–105 years (mean ± s.d. = 24·4 ± 24·1 years), from North West England, that were tested for respiratory virus infections between January 2007 and June 2012. The majority of infections were in children aged ⩽5 years. Dual or multiple infections occurred in 10·4% (1214/11 715) of patients, whereas single infection occurred in 89·6% (10 501/11 715). Rhinovirus was the most common co-infecting virus (occurring in 69·5%; 844/1214 of co-infections). In a multivariate logistic regression model, multiple infections were associated with an increased risk of admission to a general ward [odds ratio (OR) 1·43, 95% confidence interval (CI) 1·2–1·7, P < 0·0001]. On the other hand, patients with respiratory syncytial virus (RSV) and human parainfluenza virus types 1–3 (hPIV1–3), as a single infection, had a higher risk of being admitted to a general ward (OR 1·49, 95% CI 1·28–1·73, P < 0·0001 and OR 1·34, 95% CI 1·003–1·8, P = 0·05, respectively); admitted to an intensive-care unit or dying (OR 1·5, 95% CI 1·20–2·0, P = 0·001 and OR 1·60, 95% CI 1·02–2·40, P = 0·04, respectively). This result emphasizes the importance of RSV, hPIV and mixed infections and calls for research on vaccines, drugs and diagnostic tests targeting these respiratory viruses.





