7 results
The contribution of cannabis use to the increased psychosis risk among minority ethnic groups in Europe
- J. P. Selten, M. Di Forti, D. Quattrone, P. B. Jones, H. E. Jongsma, C. Gayer-Anderson, A. Szöke, P. M. Llorca, C. Arango, M. Bernardo, J. Sanjuan, J. L. Santos, M. Arrojo, I. Tarricone, D. Berardi, A. Lasalvia, S. Tosato, C. la Cascia, E. Velthorst, E. M. A. van der Ven, L. de Haan, B. P. Rutten, J. van Os, J. B. Kirkbride, C. M. Morgan, R. M. Murray, F. Termorshuizen
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 09 May 2024, pp. 1-10
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
We examined whether cannabis use contributes to the increased risk of psychotic disorder for non-western minorities in Europe.
MethodsWe used data from the EU-GEI study (collected at sites in Spain, Italy, France, the United Kingdom, and the Netherlands) on 825 first-episode patients and 1026 controls. We estimated the odds ratio (OR) of psychotic disorder for several groups of migrants compared with the local reference population, without and with adjustment for measures of cannabis use.
ResultsThe OR of psychotic disorder for non-western minorities, adjusted for age, sex, and recruitment area, was 1.80 (95% CI 1.39–2.33). Further adjustment of this OR for frequency of cannabis use had a minimal effect: OR = 1.81 (95% CI 1.38–2.37). The same applied to adjustment for frequency of use of high-potency cannabis. Likewise, adjustments of ORs for most sub-groups of non-western countries had a minimal effect. There were two exceptions. For the Black Caribbean group in London, after adjustment for frequency of use of high-potency cannabis the OR decreased from 2.45 (95% CI 1.25–4.79) to 1.61 (95% CI 0.74–3.51). Similarly, the OR for Surinamese and Dutch Antillean individuals in Amsterdam decreased after adjustment for daily use: from 2.57 (95% CI 1.07–6.15) to 1.67 (95% CI 0.62–4.53).
ConclusionsThe contribution of cannabis use to the excess risk of psychotic disorder for non-western minorities was small. However, some evidence of an effect was found for people of Black Caribbean heritage in London and for those of Surinamese and Dutch Antillean heritage in Amsterdam.
Inequality on the frontline: A multi-country study on gender differences in mental health among healthcare workers during the COVID-19 pandemic
- Diana Czepiel, Clare McCormack, Andréa T.C. da Silva, Dominika Seblova, Maria F. Moro, Alexandra Restrepo-Henao, Adriana M. Martínez, Oyeyemi Afolabi, Lubna Alnasser, Rubén Alvarado, Hiroki Asaoka, Olatunde Ayinde, Arin Balalian, Dinarte Ballester, Josleen A.l. Barathie, Armando Basagoitia, Djordje Basic, María S. Burrone, Mauro G. Carta, Sol Durand-Arias, Mehmet Eskin, Eduardo Fernández-Jiménez, Marcela I. F. Frey, Oye Gureje, Anna Isahakyan, Rodrigo Jaldo, Elie G. Karam, Dorra Khattech, Jutta Lindert, Gonzalo Martínez-Alés, Franco Mascayano, Roberto Mediavilla, Javier A. Narvaez Gonzalez, Aimee Nasser-Karam, Daisuke Nishi, Olusegun Olaopa, Uta Ouali, Victor Puac-Polanco, Dorian E. Ramírez, Jorge Ramírez, Eliut Rivera-Segarra, Bart P.F. Rutten, Julian Santaella-Tenorio, Jaime C. Sapag, Jana Šeblová, María T. S. Soto, Maria Tavares-Cavalcanti, Linda Valeri, Marit Sijbrandij, Ezra S. Susser, Hans W. Hoek, Els van der Ven
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 11 / 2024
- Published online by Cambridge University Press:
- 04 March 2024, e34
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Healthcare workers (HCWs) were at increased risk for mental health problems during the COVID-19 pandemic, with prior data suggesting women may be particularly vulnerable. Our global mental health study aimed to examine factors associated with gender differences in psychological distress and depressive symptoms among HCWs during COVID-19. Across 22 countries in South America, Europe, Asia and Africa, 32,410 HCWs participated in the COVID-19 HEalth caRe wOrkErS (HEROES) study between March 2020 and February 2021. They completed the General Health Questionnaire-12, the Patient Health Questionnaire-9 and questions about pandemic-relevant exposures. Consistently across countries, women reported elevated mental health problems compared to men. Women also reported increased COVID-19-relevant stressors, including insufficient personal protective equipment and less support from colleagues, while men reported increased contact with COVID-19 patients. At the country level, HCWs in countries with higher gender inequality reported less mental health problems. Higher COVID-19 mortality rates were associated with increased psychological distress merely among women. Our findings suggest that among HCWs, women may have been disproportionately exposed to COVID-19-relevant stressors at the individual and country level. This highlights the importance of considering gender in emergency response efforts to safeguard women’s well-being and ensure healthcare system preparedness during future public health crises.
Psychiatric symptoms in people living with HIV: prevalences, interactions and consequences
- E. M. Meeder, M. Blaauw, L. E. van Eekeren, A. Groenendijk, W. A. Vos, Q. de Mast, W. L. Blok, A. Verbon, M. A. Berrevoets, J. van Lunzen, L. Joosten, M. Netea, V. Matzaraki, A. J. van der Ven, A. F. Schellekens
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S519-S520
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
People living with HIV (PLHIV) experience higher levels of mental health issues compared to the general population. Especially depression, anxiety, impulsivity and substance use occur frequently in PLHIV. This is thought to have important consequences for quality of life, sexual risk behaviour and antiretroviral treatment (ART) adherence. Both in PLHIV as well as in the general population, divergent psychiatric symptoms often co-occur, and influence one another.
ObjectivesTo assess the interrelatedness of psychiatric symptoms and their potential consequences in PLHIV.
MethodsData from 1615 outpatient PLHIV using suppressive ART from the 2000HIV study (NCT03994835) were analysed. Participants reported on the severity of substance use (MATE-Q), depression and anxiety (HADS), impulsivity (BIS-11), quality of life (EQ-5D-5L), ART adherence (MASS-8) and sexual risk behaviour. For these variables, prevalence rates and mean scores were calculated. After binarizing the data, an Ising network model was constructed. Using this network, interrelations between psychiatric symptoms were assessed, the centrality of symptoms was estimated and connections with clinical consequences were explored.
ResultsIn our cohort of PLHIV, the increased prevalence of substance use was most pronounced, as shown by a prevalence rate of 28.7% for smoking, 13.6% for cannabis use, 11.1% for heavy alcohol drinking and 9.2% for ecstasy use in the past month. The network analysis revealed that symptoms of depression and anxiety were most strongly interrelated. The depressive symptom “feeling slowed down” was one of the most central symptoms, and was most strongly connected with quality of life. Substance use was associated with a higher occurrence of sexually transmitted diseases, and this relationship was mediated by a higher number of sexual partners. Notably, ART adherence did not display any connections with depression, anxiety, impulsivity or substance use.
Image:
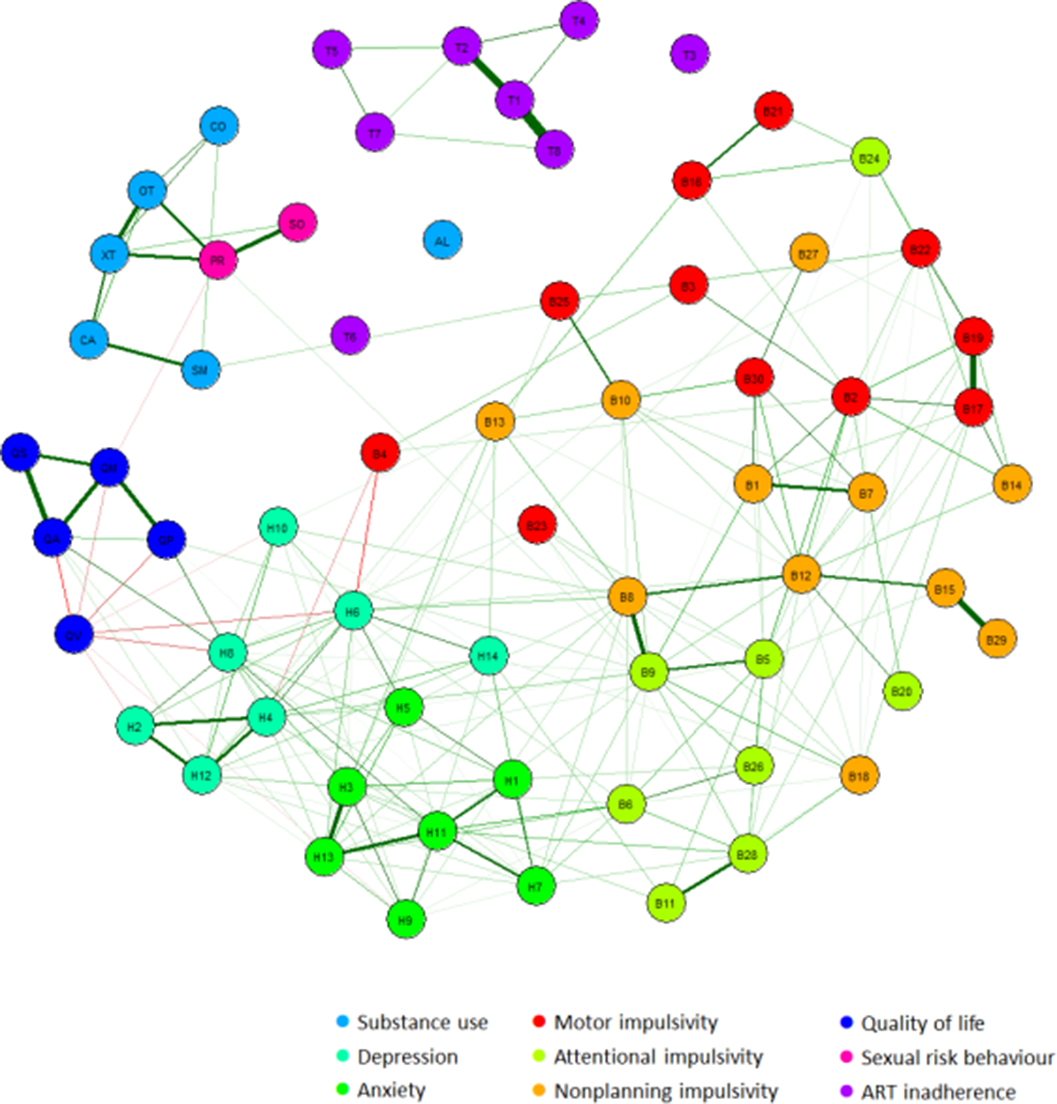 Conclusions
ConclusionsThe high occurrence of substance use and its link with sexual risk behaviour, emphasizes it’s role as a potential target for prevention of HIV transmission. Contrary to general assumption, psychiatric symptoms are not associated with lower levels of ART adherence in our cohort. Treatment of depression in PLHIV might be improved by focussing on the symptom of feeling slowed down, since this symptom was most strongly connected with quality of life.
Disclosure of InterestE. Meeder Grant / Research support from: ViiV Healthcare, M. Blaauw: None Declared, L. van Eekeren: None Declared, A. Groenendijk: None Declared, W. Vos: None Declared, Q. de Mast: None Declared, W. Blok: None Declared, A. Verbon: None Declared, M. Berrevoets: None Declared, J. van Lunzen Employee of: ViiV Healthcare, L. Joosten: None Declared, M. Netea: None Declared, V. Matzaraki: None Declared, A. van der Ven: None Declared, A. Schellekens: None Declared
Child maltreatment, migration and risk of first-episode psychosis: results from the multinational EU-GEI study
- Giuseppe D'Andrea, Jatin Lal, Sarah Tosato, Charlotte Gayer-Anderson, Hannah E. Jongsma, Simona A. Stilo, Els van der Ven, Diego Quattrone, Eva Velthorst, Domenico Berardi, Paulo Rossi Menezes, Celso Arango, Mara Parellada, Antonio Lasalvia, Caterina La Cascia, Laura Ferraro, Daniele La Barbera, Lucia Sideli, Julio Bobes, Miguel Bernardo, Julio Sanjuán, Jose Luis Santos, Manuel Arrojo, Cristina Marta Del-Ben, Giada Tripoli, Pierre-Michel Llorca, Lieuwe de Haan, Jean-Paul Selten, Andrea Tortelli, Andrei Szöke, Roberto Muratori, Bart P. Rutten, Jim van Os, Peter B. Jones, James B. Kirkbride, Robin M. Murray, Marta di Forti, Ilaria Tarricone, Craig Morgan
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 13 / October 2023
- Published online by Cambridge University Press:
- 28 October 2022, pp. 6150-6160
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Child maltreatment (CM) and migrant status are independently associated with psychosis. We examined prevalence of CM by migrant status and tested whether migrant status moderated the association between CM and first-episode psychosis (FEP). We further explored whether differences in CM exposure contributed to variations in the incidence rates of FEP by migrant status.
MethodsWe included FEP patients aged 18–64 years in 14 European sites and recruited controls representative of the local populations. Migrant status was operationalized according to generation (first/further) and region of origin (Western/non-Western countries). The reference population was composed by individuals of host country's ethnicity. CM was assessed with Childhood Trauma Questionnaire. Prevalence ratios of CM were estimated using Poisson regression. We examined the moderation effect of migrant status on the odds of FEP by CM fitting adjusted logistic regressions with interaction terms. Finally, we calculated the population attributable fractions (PAFs) for CM by migrant status.
ResultsWe examined 849 FEP cases and 1142 controls. CM prevalence was higher among migrants, their descendants and migrants of non-Western heritage. Migrant status, classified by generation (likelihood test ratio:χ2 = 11.3, p = 0.004) or by region of origin (likelihood test ratio:χ2 = 11.4, p = 0.003), attenuated the association between CM and FEP. PAFs for CM were higher among all migrant groups compared with the reference populations.
ConclusionsThe higher exposure to CM, despite a smaller effect on the odds of FEP, accounted for a greater proportion of incident FEP cases among migrants. Policies aimed at reducing CM should consider the increased vulnerability of specific subpopulations.
Migration history and risk of psychosis: results from the multinational EU-GEI study
- Ilaria Tarricone, Giuseppe D'Andrea, Hannah E. Jongsma, Sarah Tosato, Charlotte Gayer-Anderson, Simona A. Stilo, Federico Suprani, Conrad Iyegbe, Els van der Ven, Diego Quattrone, Marta di Forti, Eva Velthorst, Paulo Rossi Menezes, Celso Arango, Mara Parellada, Antonio Lasalvia, Caterina La Cascia, Laura Ferraro, Julio Bobes, Miguel Bernardo, Iulio Sanjuán, Jose Luis Santos, Manuel Arrojo, Cristina Marta Del-Ben, Giada Tripoli, Pierre-Michel Llorca, Lieuwe de Haan, Jean-Paul Selten, Andrea Tortelli, Andrei Szöke, Roberto Muratori, Bart P. Rutten, Jim van Os, Peter B. Jones, James B. Kirkbride, Domenico Berardi, Robin M. Murray, Craig Morgan
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 14 / October 2022
- Published online by Cambridge University Press:
- 10 February 2021, pp. 2972-2984
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Psychosis rates are higher among some migrant groups. We hypothesized that psychosis in migrants is associated with cumulative social disadvantage during different phases of migration.
MethodsWe used data from the EUropean Network of National Schizophrenia Networks studying Gene-Environment Interactions (EU-GEI) case–control study. We defined a set of three indicators of social disadvantage for each phase: pre-migration, migration and post-migration. We examined whether social disadvantage in the pre- and post-migration phases, migration adversities, and mismatch between achievements and expectations differed between first-generation migrants with first-episode psychosis and healthy first-generation migrants, and tested whether this accounted for differences in odds of psychosis in multivariable logistic regression models.
ResultsIn total, 249 cases and 219 controls were assessed. Pre-migration (OR 1.61, 95% CI 1.06–2.44, p = 0.027) and post-migration social disadvantages (OR 1.89, 95% CI 1.02–3.51, p = 0.044), along with expectations/achievements mismatch (OR 1.14, 95% CI 1.03–1.26, p = 0.014) were all significantly associated with psychosis. Migration adversities (OR 1.18, 95% CI 0.672–2.06, p = 0.568) were not significantly related to the outcome. Finally, we found a dose–response effect between the number of adversities across all phases and odds of psychosis (⩾6: OR 14.09, 95% CI 2.06–96.47, p = 0.007).
ConclusionsThe cumulative effect of social disadvantages before, during and after migration was associated with increased odds of psychosis in migrants, independently of ethnicity or length of stay in the country of arrival. Public health initiatives that address the social disadvantages that many migrants face during the whole migration process and post-migration psychological support may reduce the excess of psychosis in migrants.
The incidence of psychotic disorders among migrants and minority ethnic groups in Europe: findings from the multinational EU-GEI study
- Fabian Termorshuizen, Els van der Ven, Ilaria Tarricone, Hannah E. Jongsma, Charlotte Gayer-Anderson, Antonio Lasalvia, Sarah Tosato, Diego Quattrone, Caterina La Cascia, Andrei Szöke, Domenico Berardi, Pierre-Michel Llorca, Lieuwe de Haan, Eva Velthorst, Miguel Bernardo, Julio Sanjuán, Manuel Arrojo, Robin M. Murray, Bart P. Rutten, Peter B. Jones, Jim van Os, James B. Kirkbride, Craig Morgan, Jean-Paul Selten
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 7 / May 2022
- Published online by Cambridge University Press:
- 22 September 2020, pp. 1376-1385
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
In Europe, the incidence of psychotic disorder is high in certain migrant and minority ethnic groups (hence: ‘minorities’). However, it is unknown how the incidence pattern for these groups varies within this continent. Our objective was to compare, across sites in France, Italy, Spain, the UK and the Netherlands, the incidence rates for minorities and the incidence rate ratios (IRRs, minorities v. the local reference population).
MethodsThe European Network of National Schizophrenia Networks Studying Gene–Environment Interactions (EU-GEI) study was conducted between 2010 and 2015. We analyzed data on incident cases of non-organic psychosis (International Classification of Diseases, 10th edition, codes F20–F33) from 13 sites.
ResultsThe standardized incidence rates for minorities, combined into one category, varied from 12.2 in Valencia to 82.5 per 100 000 in Paris. These rates were generally high at sites with high rates for the reference population, and low at sites with low rates for the reference population. IRRs for minorities (combined into one category) varied from 0.70 (95% CI 0.32–1.53) in Valencia to 2.47 (95% CI 1.66–3.69) in Paris (test for interaction: p = 0.031). At most sites, IRRs were higher for persons from non-Western countries than for those from Western countries, with the highest IRRs for individuals from sub-Saharan Africa (adjusted IRR = 3.23, 95% CI 2.66–3.93).
ConclusionsIncidence rates vary by region of origin, region of destination and their combination. This suggests that they are strongly influenced by the social context.
Social disadvantage, linguistic distance, ethnic minority status and first-episode psychosis: results from the EU-GEI case–control study
- Hannah E. Jongsma, Charlotte Gayer-Anderson, Ilaria Tarricone, Eva Velthorst, Els van der Ven, Diego Quattrone, Marta di Forti, EU-GEI WP2 Group, Paulo Rossi Menezes, Christina Marta Del-Ben, Celso Arango, Antonio Lasalvia, Domenico Berardi, Caterina La Cascia, Julio Bobes, Miguel Bernardo, Julio Sanjuán, Jose Luis Santos, Manuel Arrojo, Lieuwe de Haan, Andrea Tortelli, Andrei Szöke, Robin M. Murray, Bart P. Rutten, Jim van Os, Craig Morgan, Peter B. Jones, James B. Kirkbride
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 9 / July 2021
- Published online by Cambridge University Press:
- 03 March 2020, pp. 1536-1548
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Ethnic minority groups in Western countries face an increased risk of psychotic disorders. Causes of this long-standing public health inequality remain poorly understood. We investigated whether social disadvantage, linguistic distance and discrimination contributed to these patterns.
MethodsWe used case–control data from the EUropean network of national schizophrenia networks studying Gene-Environment Interactions (EU-GEI) study, carried out in 16 centres in six countries. We recruited 1130 cases and 1497 population-based controls. Our main outcome measure was first-episode ICD-10 psychotic disorder (F20–F33), and exposures were ethnicity (white majority, black, mixed, Asian, North-African, white minority and other), generational status, social disadvantage, linguistic distance and discrimination. Age, sex, paternal age, cannabis use, childhood trauma and parental history of psychosis were included as a priori confounders. Exposures and confounders were added sequentially to multivariable logistic models, following multiple imputation for missing data.
ResultsParticipants from any ethnic minority background had crude excess odds of psychosis [odds ratio (OR) 2.03, 95% confidence interval (CI) 1.69–2.43], which remained after adjustment for confounders (OR 1.61, 95% CI 1.31–1.98). This was progressively attenuated following further adjustment for social disadvantage (OR 1.52, 95% CI 1.22–1.89) and linguistic distance (OR 1.22, 95% CI 0.95–1.57), a pattern mirrored in several specific ethnic groups. Linguistic distance and social disadvantage had stronger effects for first- and later-generation groups, respectively.
ConclusionSocial disadvantage and linguistic distance, two potential markers of sociocultural exclusion, were associated with increased odds of psychotic disorder, and adjusting for these led to equivocal risk between several ethnic minority groups and the white majority.




