11 results
Depressive disorder comorbid with problematic alcohol use
- H. Berrada, H. Chebli, F. Azraf, F. El Omari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S661-S662
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Alcohol use disorder is a real public health problem in the world, it consists of a pathological mode of consumption which is characterized by a loss of control and craving. Depressive disorder and alcohol use disorder are among the most frequent mental pathologies and are often associated.
The links between these two disorders can be of several types: Alcohol Induced Depressive Disorders, Primary Depressive Disorders and Secondary Alcohol Dependence. They can also have two-way relationships or be favored by common factors.
ObjectivesThe objective of our work is to analyze the causal links between alcohol use disorder and depression.
Methodsprovide an update via two clinical vignettes and a review of the literature the relationship between alcohol use disorder and depression
ResultsThe causal relationships between alcohol dependence and psychiatric disorders can be of several types which are not mutually exclusive: primary alcohol dependence, secondary psychiatric disorders, induced by alcohol. This is the case for the majority of depressive disorders encountered in alcohol-dependent patients; primary psychiatric disorders and secondary alcohol dependence; alcohol dependence and anxiety and/or depressive disorders are favored by common factors, in particular personality disorders, encountered in approximately 40% of alcohol-dependent patients. Whatever the direction of causation, alcohol dependence and psychiatric disorders worsen each other over time.Depression and alcohol use disorder are among the most frequent mental pathologies and are often associated.The optimal management of patients with dual diagnosis is so-called “integrated” management, simultaneously combining alcohol and psychiatric therapeutic approaches.
ConclusionsAlcohol consumption impairs the prognosis of depression, increases the risk of suicide, impairs social functioning and increases recourse to the healthcare system.The optimal management of patients with dual diagnosis is so-called “integrated” management. Psychotherapeutic (individual and systemic), drug and psychosocial approaches would be necessary to maximize therapeutic success.
Disclosure of InterestNone Declared
Could we predict an episode of delirium tremens? Case report
- A. Tounsi, Z. Bencharfa, F. Azraf, M. Sabir, F. Elomari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S656-S657
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Delirium tremens is one of the most serious complications associated with alcohol withdrawal. It affects a percentage of 5 to 20% of users and is not related to the duration of consumption nor to the quantities taken. An early diagnosis will facilitate a quick treatment without putting at risk the vital prognosis.
ObjectivesOur objective is to identify the different indicators mentioned in the existing literature and to compare these to the clinical and paraclinical data of our patients
MethodsWe present through clinical vignettes, the cases of two patients hospitalized in our department of addictology for a cure of alcohol withdrawal and who presented an episode of delirium tremens.
Resultseveral clinical and paraclinical parameters have been linked to statistically significant differences in the published reports related to this subject. Thrombocytopenia remains the common element between the different publications and was the case in our two patients.
Clinically, the presence of a previous episode of delirium or seizure during withdrawal , as well as tachycardia (>100 bpm) and low number of quit attempts were significantly related to the occurrence of delirium tremens. The majority of the predictors identified were paraclinical and included: hyponatremia, hypokalemia, elevated ALT and homocyctein levels, low pyridoxine levels, and the presence of structural brain damage.
Conclusionsthe literature on predictors of delirium tremens remains poor. more studies are needed to confirm the data already mentioned
Disclosure of InterestNone Declared
Correlates of aggressive behavior in the moroccan context
- A. Tounsi, Z. Bencharfa, F. Azraf, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S284
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Violence among the mentally ill population has long been a subject of stigma, and controversy. Clinicians’ ability to assess the violent potential is still limited.
ObjectivesThe objective of this work is to identify the positively correlated indicators of aggressive behavior in patients admitted to hospital emergency departments.
MethodsIt is a retrospective and descriptive paper based on the records of patients admitted to the emergency department of Arrazi University Psychiatric Hospital in Salé during a one-month period.
The psychiatric diagnosis was formulated using the DSM-5 diagnostic criteria and Violent behavior was assessed using the Modified Overt Aggression Scale (MOAS). The existence of aggressive behavior was defined by a MOAS score ≥3.
We used SPSS 15 to analyse results
ResultsSixty-five case files were selected during the study month. The average age was 35.3 (19;64).
The mean of our sample MOAS aggression scale score was 31.5 [0; 79] and 90% of patients had a score ≥ 3 (image 1)
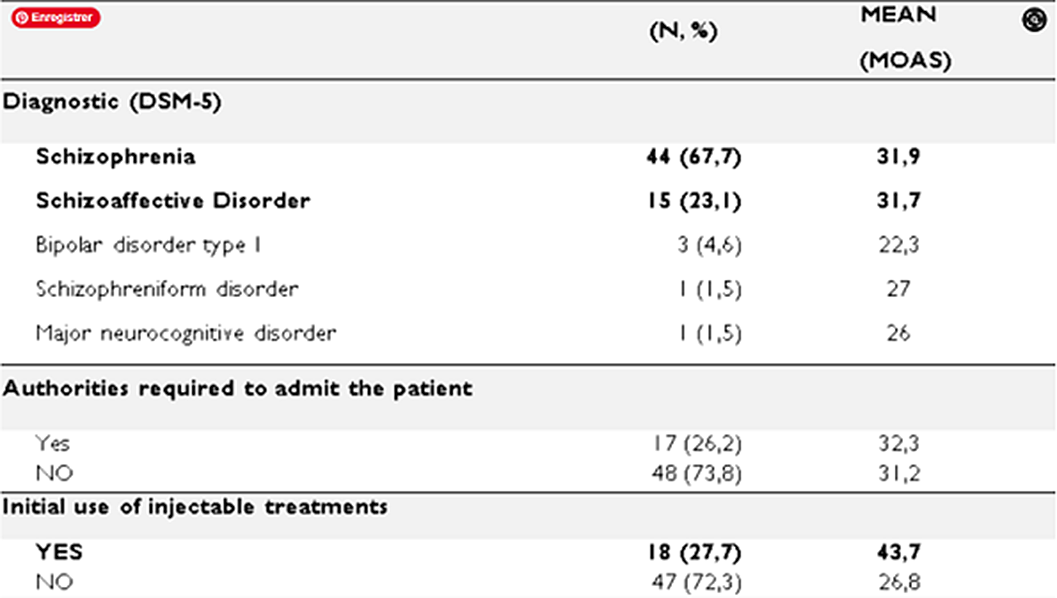
Among the 65 admissions, heteroaggressive risk was the most frequent reason for hospitalization (N=53), followed by psychomotor excitement. IMAGE 2
Statistical analysis revealed a significant association between high MOAS scores and substance use, history of suicide attempt, educational level and socioeconomic level
Image:
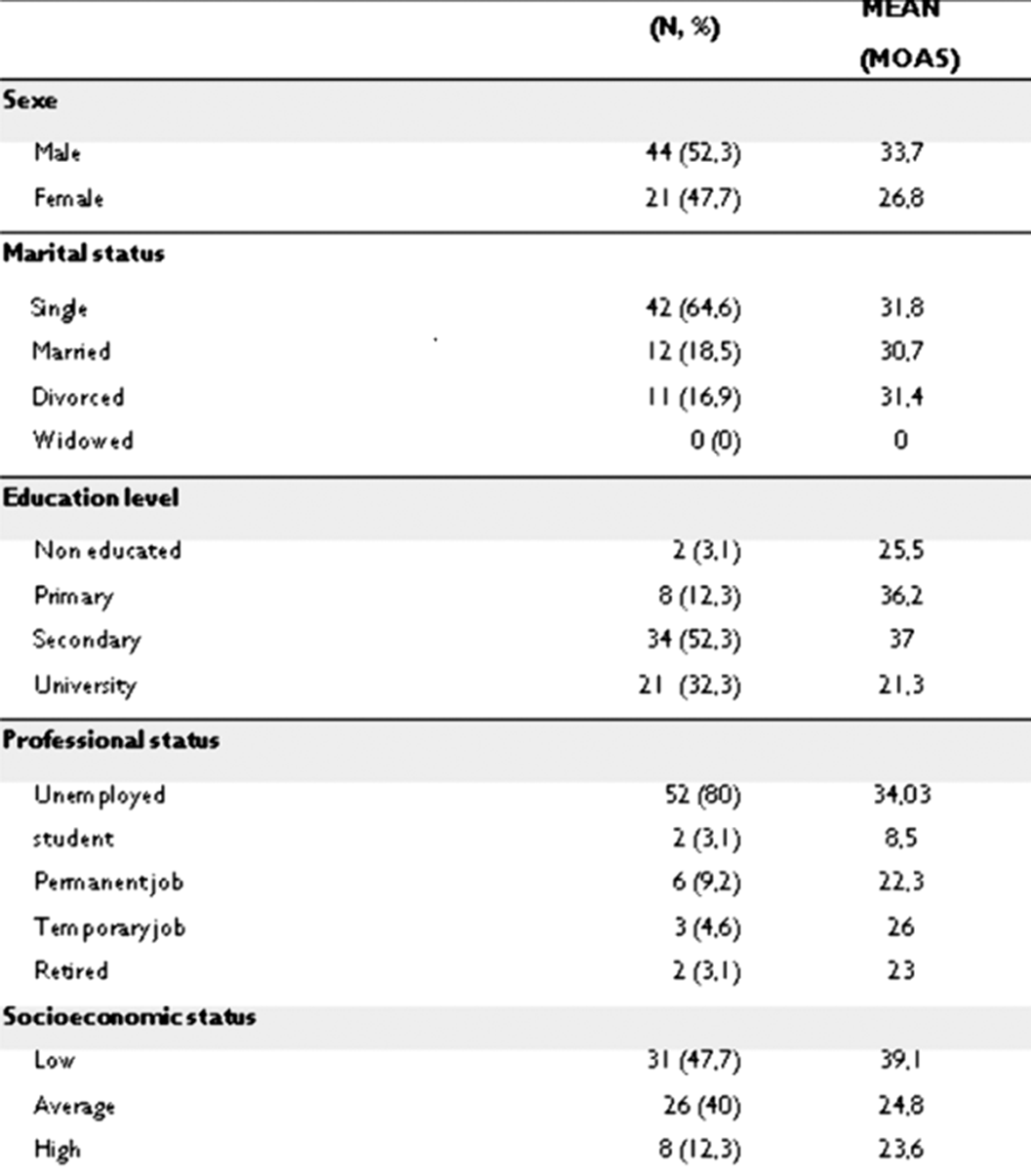
Image 2:
 Conclusions
ConclusionsIn the current research, the prevalence of aggressive behavior was high among these patients, which may be due to the conditions of psychiatric hospitalization in our region, which is often reserved for the most serious and dangerous patients.
Disclosure of InterestNone Declared
Methadone in pain management: About a case and a review of the literature
- F. Azraf, H. Berrada, M. Sabir, F. El Omari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S964
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Methadone has been available for about half a century. It is traditionally known for its role in the withdrawal and maintenance of patients addicted to heroin or other opioids.
A large body of evidence has identified a number of advantages of methadone over other opioids in the treatment of pain, including its agonist action at μ- and δ-opioid receptors, its N-methyl-D-aspartate (NMDA) antagonist activity, and the ability to inhibit monoamine reuptake, hence its interest in the treatment of cancer pain and, more recently, neuropathic pain and non-cancer pain.
Methadone proves to be a treatment adapted to the management of complex painful situations, resistant to other opioids. It sometimes makes it possible to postpone an invasive act, sedation for refractory symptoms while maintaining the patient’s autonomy. Its use in many countries and feedback from our colleagues agree with our observations. It is an effective molecule as an analgesic on different types of pain, including post-surgical pain, cancer-related pain or nociceptive pain
Objectivesexplain the role of methadone in the treatment of chronic and acute pain.
MethodsWe will explain through a clinical case the role of methadone in the treatment of chronic and acute pain. The patient was a 35-year-old nurse, married with 3 children, with problematic use of codeine and morphine for chronic pain due to endometriosis. She was put on 20mg/d of methadone with good clinical improvement.
ResultsWe reported the clinical case of a patient followed for endometriosis and that she presents with acute and chronic pain during and outside of menstruation. The patient was treated with (Danazol) and analgesics to manage her pain. She was initially put on level 1 analgesics: paracetamol and NSAIDs, then on level 2 analgesics, in particular codeine at a rate of 200 mg/day, without any improvement. Faced with this state, the patient was put on morphine with a gradual increase in doses on her own initiative up to 30mg/d. The patient tried to stop her morphine consumption on several occasions without succeeding. The patient was put on methadone to treat both her pain and her addiction to morphine, methadone significantly reduced her pain within a few days.
ConclusionsMethadone proves to be a treatment adapted to the management of complex painful situations, resistant to other opioids. It sometimes makes it possible to postpone an invasive act, sedation for refractory symptoms while maintaining the patient’s autonomy. Its use in many countries and feedback from our colleagues agree with our observations. It is an effective molecule as an analgesic on different types of pain, including post-surgical pain, cancer-related pain or nociceptive pain.
Disclosure of InterestNone Declared
Inhalant use and psychosis: EXPERIENCE of a moroccan addiction departement
- A. Tounsi, F. Azraf, N. El Moussaoui, M. Sabir, F. Elomari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S656
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Inhalants are volatile psychoactive compounds whose effect varies from disorientation, excitement, euphoria to hallucinations. Different opinions have been raised concerning the relationship between inhalant use and psychosis and several publications have studied the incidence of psychotic disorders in the context of inhalant use. These studies concluded that using inhalants was independently associated with the development of psychosis
Objectivesour aim is to determine the demographic and psychiatric profile of inhalant users previously hospitalized in our department
MethodsThis is a retrospective descriptive study carried out by analyzing hospitalization records in the addictology department of the psychiatric university hospital Ar-Razi in Salé over a period of one year (from August 2020 to August 2021). The diagnoses are established according to the DSM 5 diagnostic criteria.
ResultsSeventeen patients, inhalant users, were recruited after chart review, including 5 women and 11 men (68.7 %). The average age was 24.7 years (16; 41). The majority of the patients were single (81.2%), 62.5 % had a secondary education and 62.5 % were unemployed.
The psychiatric evaluation showed that 87% of these patients had a history of incarceration, 50% had a diagnosis of schizophrenia, 12.5% had bipolar disorder and 14.2% had a cluster B personality disorder (DSM 5).
The average age of onset of the addictive disorder in this population was 14.4 years and the entire sample was polyaddictive.
ConclusionsMore than half of our sample had psychosis associated with their inhalant use disorder. these results are consistent with literature data.
Disclosure of InterestNone Declared
ADDICTION AND THE EVOLUTION AND COMPLIANCE OF SCHIZOPHRENIC PATIENTS
- F. Azraf, H. Chebli, F. El Omari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1054-S1055
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a chronic illness, affecting approximately 1% of the general population. The more chronic a treatment is, the poorer the quality of adherence. In fact, approximately 60% of patients with schizophrenia are incompletely or non-adherent within one year of the first episode. Poor adherence has consequences in terms of clinical status, quality of life and psychosocial functioning due to associated relapses. One of the main factors of poor compliance is the use of addictive substances. Half of schizophrenic patients have, or have had, an addictive comorbidity during their life. Moreover, schizophrenic patients with addictive comorbidity have a more severe symptomatology and have more associated physical, psychological and social problems, representing a challenge in the management
ObjectivesThe objective of our work is to evaluate the impact of addictive comorbidity on medication adherence and relapse.
MethodsThis is a cross-sectional study, carried out in patients with schizophrenia hospitalized or followed in ambulatory consultation, at the psychiatric hospital Ar-razi of Salé. The data collection (sociodemographic, clinical and therapeutic) is carried out by a questionnaire established for this purpose. The use of substances is evaluated according to the DSM-V criteria
ResultsA total of 110 schizophrenic patients were followed or hospitalized, of which 61.8% had a substance use disorder. The average age of onset of substance use was 18 years. The duration of substance use ranged from 1 to 11 years and up to 49 years for tobacco and cannabis. 72% of the addicts tried to stop their use alone or in outpatient settings, only 17% in inpatient settings. The average duration of abstinence was 11 months and ranged from 1 to 18 years. 81% reported remission of the disease after abstinence. The hospitalization rate was 88.2% for addicts versus 85% for non-addicts. The number of hospitalizations was 180 for addicts versus 78 for non-addicts. The cumulative duration of hospitalization is 208 months against 96 months for addicts. The duration of remission is 5 months for addicts and 24 months for non-addicts. 71% of non-addicts patients have well observed their treatment against 57% of addicts
ConclusionsThe weight of co-morbid addictions represents between 1/5 and 1/3 of the factors at stake in the compliance and the risk of relapse of patients suffering from schizophrenia. The development of specific care strategies for a global management of addiction and schizophrenia should be a priority.
Disclosure of InterestNone Declared
Profile of forensic patients hospitalized in psychiatry
- F. Azraf, H. Berrada, S. Belbachir, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S536
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The question of violence and dangerousness is a central subject in psychiatry, since it is a source of stigmatization for many patients and represents a major element of medical, legal and social care. Violence being defined as: "the deliberate use or threat of deliberate use of physical force or power against oneself, against another person or against a group or community, which results in or is very likely to lead to trauma, death, moral damage, maldevelopment or deficiency”. The violent character of the mentally ill was among the precursors to the discussion around the first therapeutic measures for the mentally ill. A better knowledge of the risk factors for the passage to a violent act in mental disorders is therefore necessary for the development of therapeutic and preventive strategies.
ObjectivesThe objective of our work is to determine the socio-demographic, clinical and criminological characteristics of forensic patients and to seek the predictive factors of violence in these patients.
MethodsThis is a retrospective study spread over 10 years on a series of forensic patients who were hospitalized at the Ar-razi psychiatric hospital in Salé (Morocco). The collection of data was carried out from clinical observations, psychiatric expertise and an exploitation sheet.
ResultsNumerous studies have defined subgroups of patients at risk. Factors such as positive symptoms, poor treatment compliance, and comorbidities such as substance use disorders or antisocial personality traits have been described as predictive of violence.
ConclusionsThe prevention of medico-legal acts must take into consideration these associated factors, in particular early management of the disorders, improvement of therapeutic observance and family care.
Disclosure of InterestNone Declared
Psychiatric disorders in women hospitalized at the arrazi psychiatric hospital
- H. Berrada, F. Azraf, A. Tounsi, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S952
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women get hospitalized for various serious mental disorders that are gender specific, half of them married with children, the other half single\divorced women stigmatized and marginalized in our society.
ObjectivesThe aim of this study is to describe mentally ill women admitted into the psychiatric hospital, socio demographically and clinically, highlighting differences, specificities and multiple roles distress deviate with the course of disorder.
MethodsThis is a prospective cross-sectional study involving 50 patients admitted to Ar-razi Psychiatric Hospital
ResultsThe average age is 39years, 41% of them are single, with a low educational level (primary school). 77% of our women are from the urban region, 59% are jobless. 19% of patients in our study have positive family history, 65% of them suffered from schizophrenia. 65% of patients are admitted for schizophrenia, followed by bipolar I disorder 22%, MDD is only represented by 10%. 25% of inpatients deal with a toxic habit, 18,5% abuse nicotine and only one woman have tried quitting. Suicide attempts are closely linked to major depressive episodes of MDD and BID, in patients were already under a combination of antidepressants and anxiolytics for at least 3 months. Psychotic features are observed in most of admitted disorders, 80% in BIP and 64% in MDD. According to HAMILTON-DEPRESSION 62,9% of women are admitted for a severe depressive episode, 30% present anxiety comorbidity and a history of CBT sessions months prior hospitalization.
ConclusionsShading the light into admitted women in psychiatry and deciphering specific demographic, clinical and therapeutic features may improve the global care system and women’s adherence to treatment and follow up.
Disclosure of InterestNone Declared
Caesarean section and post traumatic stress disorder
- H. Chebli, M. Chtibi, F. Azraf, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S977
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Childbirth can be a very painful experience, especially vaginally. It can have many complications. The obstetrical complications of caesarean section are well studied but its psychological complications are little mentioned. Most women recover quickly after giving birth, but others seem to have more difficulty. Researchers have attempted to identify perinatal risk factors for the development of post-traumatic stress disorder in parturients and caesarean section seems to be one of the predictors.
ObjectivesThe objective of our study is to detect post traumatic stress disorder in women after vaginal delivery.
MethodsThis is a cross-sectional descriptive study conducted among women from the general population who have given birth vaginally. The information was collected using a questionnaire distributed on social networks. Symptom severity was quantified using the PTSD checklist for DSM-V (PCL-5).PCL-5 is a 20-item self-assessment that measures the 20 DSM-5 symptoms of PTSD. She rates each symptom from 0 (not at all) to 4 (extremely). The score varies from 0 to 80. A threshold of 33 allows screening for post-traumatic stress disorder.
Results61 women took part in this study, 81.5% of whom gave birth vaginally between the ages of 20 and 30.70.3% of the participants gave birth vaginally once, 44.4% twice and 7.3% of the women in our sample had a caesarean three times.Regarding the indication of the high way in our sample: the narrowing of the pelvis and fetal distress were in 22.2%. Exceeding term was in 18.5% of cases.In our sample, 59.3% of the women had planned their vaginal delivery and 40.7% had given birth urgently.Regarding the results of the PCL-5 scale (PTSD checklist for DSM-V), the score varies between 0 and 48 with a median score equal to 12. 3.7% of the participants had a score greater than 33.
ConclusionsPost-traumatic stress disorder can accompany childbirth, especially when it is high and in an emergency. Postpartum post traumatic stress disorder affects the mother-child relationship and can be complicated by depressive disorder. Medical monitoring of pregnancy, good medical and family support for the parturient and preparation for childbirth are necessary to better start the maternity experience.
Disclosure of InterestNone Declared
Schizophrenia: the announcement of the diagnosis
- F. Azraf, M. Chtibi, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1055
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For many years, the question of the announcement of the diagnosis in psychiatry has been controversial. It is the starting point of a management allowing access to psychoeducation and to the patient’s recovery. In the case of schizophrenia, the cognitive impairment and the stigmatizing nature of the pathology jeopardize the announcement of the diagnosis. However, recommendations and legislation emphasize the need to inform the patient about his or her pathology. In Morocco, the law n° 131-13 of February 19, 2015 relating to the practice of medicine has made information about the diagnosis to patients an obligation for doctors and a right for patients
ObjectivesThe interest of our work is to try to evaluate the current state of this practice, its ethics and its representations among psychiatrists.
MethodsThis is a descriptive study on the announcement of the diagnosis of schizophrenia in a population of psychiatrists. The data collection was carried out by a questionnaire including: Socio-demographic and professional data, opinion on practice and training concerning diagnostic announcement in psychiatry, physicians’ representations concerning announcement: frequency, opinion on the importance of this practice.
Results31 participants responded to our questionnaire. More than 9 out of 10 participants would not benefit from training on diagnostic announcement. Only 22.6% of physicians reported being very or somewhat familiar with medical information laws and their content regarding the regulation of diagnostic announcement. All participants considered schizophrenia to be the most difficult pathology to announce, followed by personality disorders and bipolar disorder. 74.2 of the participants considered it “rather” or “completely” essential to inform the patient of his or her psychiatric diagnosis. 77.4% of the participants considered it necessary to announce the diagnosis of schizophrenia and 80.7 often or systematically announce this diagnosis. Three situations considered appropriate to announce a diagnosis of schizophrenia: 74.2% announce it in general when the patient or the family asks for information about the diagnosis, 42% advise the patient when he/she mentions schizophrenia on his/her own. The patient’s functional inability to understand the diagnosis (77.4%) and the fear of negative clinical and therapeutic repercussions (41.9 and 38.7 respectively) were reported to deter physicians from making the announcement. More than half of the participants (64.5%) thought that the announcement of the diagnosis improved therapeutic compliance. Conversely, 35.5% considered that the announcement had no impact on therapeutic compliance.
ConclusionsThe announcement of the diagnosis of schizophrenia remains today a complex and evolving subject. Even if great progress has been made to inform patients as well as possible, practices remain disparate from one doctor to another and this information is not well traced.
Disclosure of InterestNone Declared
Misuse of psychotropic medications among hospitalized patients
- F. Azraf, A. Tounsi, M. Sabir, F. El Omari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S660
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotropic drugs are sometimes taken outside of any medical context and can be diverted or even trafficked. This phenomenon affects more adolescents and young adults, more specifically those who are already struggling with other consumption problems. This vulnerable population is thus exposed to several negative health and social repercussions.
ObjectivesThe objective of our work is to determine the sociodemographic characteristics of the patients, the main drugs used, the dose, the route of administration, the mode of obtaining the drug and the intentionality of the use.
MethodsIt is a retrospective study spread over 1 year on a series of patients who were hospitalized in the service of addictology at the psychiatric hospital Ar-razi of Salé. The data collection was carried out from the medical files and an exploitation form.
ResultsA total of 141 patients were hospitalized during this period of which 53 37.5 had a diverted use of medication. Our sample is characterized by a predominance of female patients (90%) with a median age of 33 years. The most misused drugs were benzodiazepines (85.7%), analgesics (11.7%), hypnotics (9.4%) and antihistamines (1.9%). Misuse is related to exceeding doses (up to 40 times the maximum dose of the AMM) and duration of treatment, to use or obtaining drugs without a prescription 79.2 , to the route of administration and to drug addiction. 11.3 of patients were dependent on a single drug; 88.7% of patients had a co-addiction: tobacco 86.8%, cannabis 77.3%, alcohol 58.5%, cocaine 34.5%, solvents 15 , heroin 1.8% or a history of addiction. Hospitalization was only related to drug misuse in 11.3% of cases. The effects sought: anxiolysis 58.5%, euphoria 30.2%, analgesic 5.7%, disinhibition 3.8%, increased performance 1.9%
ConclusionsThe misuse of psychotropic drugs is a well-known public health problem. However, this phenomenon remains unknown and neglected in Morocco.
Disclosure of InterestNone Declared





