7 results
Unsupervised neurobiology-driven stratification of clinical heterogeneity in depression
- F. Colombo, F. Calesella, B. Bravi, L. Fortaner-Uyà, C. Monopoli, E. Maggioni, E. Tassi, R. Zanardi, F. Attanasio, I. Bollettini, S. Poletti, F. Benedetti, B. Vai
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S614
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the main obstacles in providing effective treatments for major depressive disorder (MDD) is clinical heterogeneity, whose neurobiological correlates are not clearly defined. A biologically meaningful stratification of depressed patients is needed to promote tailored diagnostic procedures.
ObjectivesUsing structural data, we performed an unsupervised clustering to define clinically meaningful clusters of depressed patients.
MethodsT1-weighted and diffusion tensor images were obtained from 102 MDD patients. In 64 patients, clinical symptoms, number of stressful life events, severity and exposure to adverse childhood experiences were evaluated using the Beck Depression Inventory (BDI), Schedule of Recent Experiences (SRE), Risky Family Questionnaire (RFQ), and Childhood Trauma Questionnaire (CTQ). Clustering analyses were performed with extracted tract-based fractional anisotropy (TBSS, FSL), cortical thickness, surface area, and regional measures of grey matter volumes (CAT12). Gaussian mixture model was implemented for clustering, considering Support Vector Machine (SVM) as classifier. A 10x2 repeated cross-validation with grid search was performed for hyperparameters tuning and clusters’ stability. The optimal number of clusters was determined by normalized stability, Akaike and Bayesian information criterion. Analyses were adjusted for total intracranial volume, age, and sex. The clinical relevance of the identified clusters was assessed through MANOVA, considering domains of clinical scales as dependent variables and clusters’ labels as fixed factors. Discriminant analysis was subsequently performed to assess the discriminative power of these variables.
ResultsCross-validated clustering approach identified 2 highly stable clusters (normalized stability=0.316, AIC=-80292.48, BIC=351329.16). MANOVA showed a significant between-clusters difference in clinical scales scores (p=0.038). Discriminant analysis distinguished the two clusters with an accuracy of 78.1%, with BDI behavioural and CTQ minimisation/denial domains showing the highest discriminant values (0.325 and 0.313).
ConclusionsOur results defined two biologically informed clusters of MDD patients associated with childhood trauma and specific clinical profiles, which may assist in targeting effective interventions and treatments.
Disclosure of InterestNone Declared
Structural neuroimaging differentiates between depressed bipolar disorder and major depressive disorder patients: a machine learning study
- F. Calesella, F. Colombo, B. Bravi, L. Fortaner-Uyà, C. Monopoli, E. Tassi, E. Maggioni, I. Bollettini, S. Poletti, F. Benedetti, B. Vai
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S614-S615
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depression is the predominant mood alteration in bipolar disorder (BD), leading to overlapping symptomatology with major depressive disorder (MDD). Consequently, in clinical assessment, almost 60% of BD patients are misdiagnosed as affected by MDD. This calls for the creation of a framework for the differentiation of BD and MDD patients based on reliable biomarkers. Since machine learning (ML) enables to make predictions at the single-subject level, it appears to be particularly suitable for this task.
ObjectivesWe implemented a ML pipeline for the differentiation between depressed BD and MDD patients based on structural neuroimaging features.
MethodsDiffusion tensor imaging (DTI) and T1-weighted magnetic resonance imaging (MRI) data were acquired for 282 depressed BD (n=180) and MDD (n=102) patients. Axial (AD), radial (RD), mean (MD) diffusivity, and fractional anisotropy (FA) maps were extracted from DTI images, and voxel-based morphometry (VBM) measures were obtained from T1-weighted images. Each feature was entered separately into a 5-fold nested cross-validated ML pipeline differentiating between BD and MDD patients, comprising: confound regression for nuisance variables removal (i.e., age and sex), feature standardization, principal component analysis, and an elastic-net penalized regression. The models underwent 5000 random permutations as a test for significance, and the McNemar’s test was used to assess whether there was any significant difference between the models (significance threshold was set to p<0.05).
ResultsThe performance of the models and the results of the permutation tests are summarized in Table 1. McNemar’s test showed that the AD-, RD-, MD-, and FA-based models did not differ between each other and were significantly different from the VBM.
Table 1. Models’ performance and p-value at 5000 permutation test. Feature Overall accuracy MDD specifictiy BD sensitivity p-value VBM 0.61 0.38 0.74 0.058 AD 0.78 0.65 0.86 <0.001 FA 0.79 0.61 0.89 <0.001 MD 0.79 0.63 0.88 <0.001 RD 0.79 0.63 0.88 <0.001 ConclusionsIn conclusion, our models differentiated between BD and MDD patients at the single-subject level with good accuracy using structural MRI data. Notably, the models based on white matter integrity measures relying on true information, rather than chance.
Disclosure of InterestNone Declared
Inflammatory signature of post-COVID-19 depression
- M. Palladini, M. G. Mazza, V. Aggio, S. Spadini, F. Calesella, S. Poletti, P. Rovere-Querini, F. Benedetti
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S123-S124
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Persisting and disabling depressive symptomatology represent a prominent feature of the post-acute COVID-19 syndrome. Sars-CoV-2-induced immune system dysregulation mainly result in a cytokine storm. Once in the brain, inflammatory mediators negatively affect neurotransmission, microglia activation, and oxidative stress, possibly disrupting critical brain neurocircuits which underpin depressive symptoms. So far, only inflammatory markers based on leukocyte counts have been linked to depressive outcome in COVID survivors. However, an accurate immune profile of post-COVID depression has yet to be elucidated.
ObjectivesIdentify inflammatory mediators that predict post-COVID depression among a panel of cytokines, chemokines, and growth factors, with a machine learning routine.
Methods88 COVID age- and sex-matched survivors’ (age 52.01 ± 9.32) were screened for depressive symptomatology one month after the virus clearance through the Beck Depression Inventory (BDI-13), with 12.5% of the individuals scoring in the clinical range (BDI-13 ≥ 9). Immune assay was performed through Luminex system on blood sampling obtained in the same context. We entered 42 analytes into an elastic net penalized regression model predicting presence of clinical depression, applied within a 5-fold nested cross-validation machine learning routine running in MATLAB. Significance of predictors was evaluated according to variable inclusion probability (VIP), as returned by 5000 bootstraps. Socio-demographics, previous psychiatric history, hospitalization, time after discharge were used as covariates.
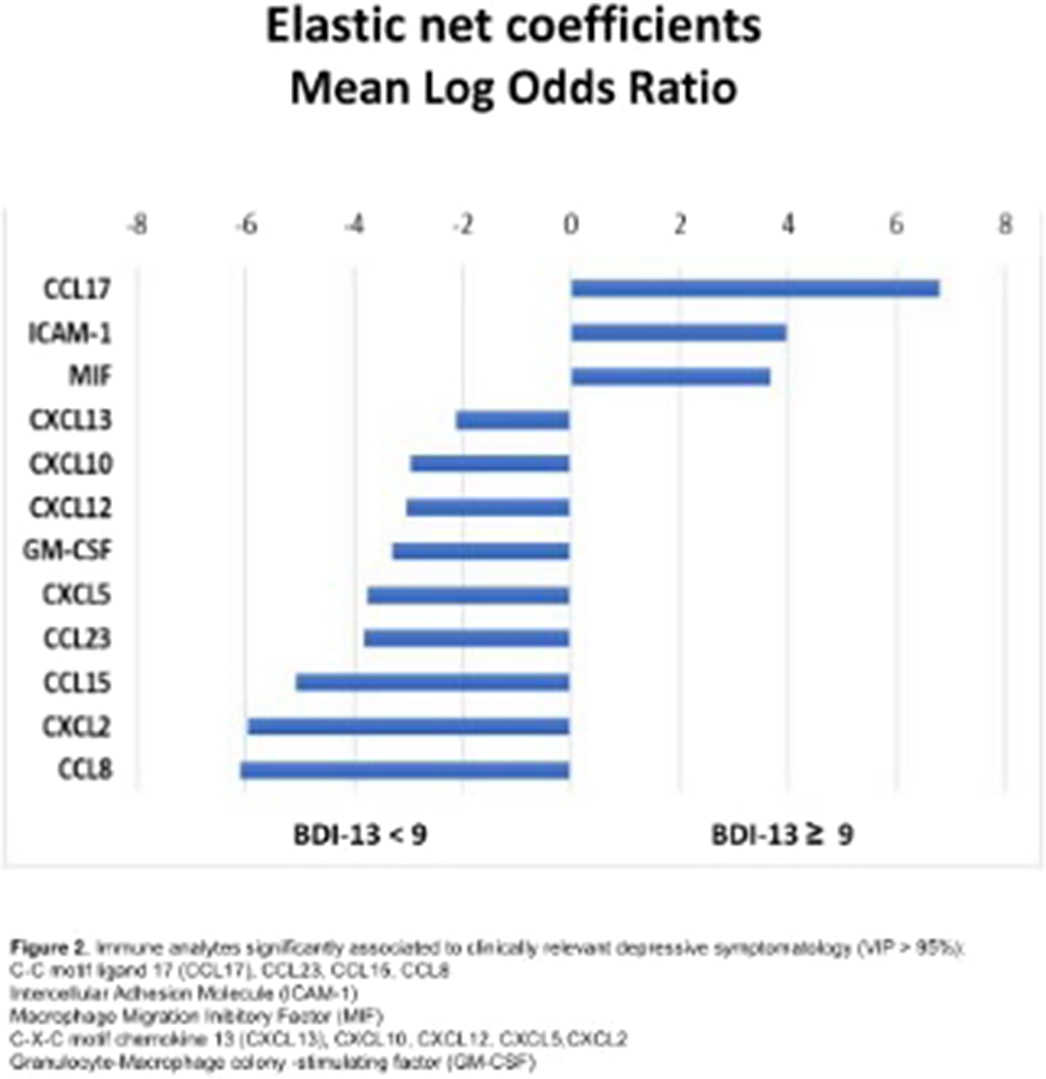
ResultsThe model reached a balance accuracy of 73% and AUC of 77%, correctly identifying 73% of people suffering from clinically relevant depressive symptoms (Figure1). Depressive symptomatology was predicted by high levels of CCL17, ICAM-1, MIF, whereas CXCL13, CXCL12, CXCL10, CXCL5, CXCL2, CCL23, CCL15, CCL8, GM-CSF showed a protective effect (Figure2).
Image:
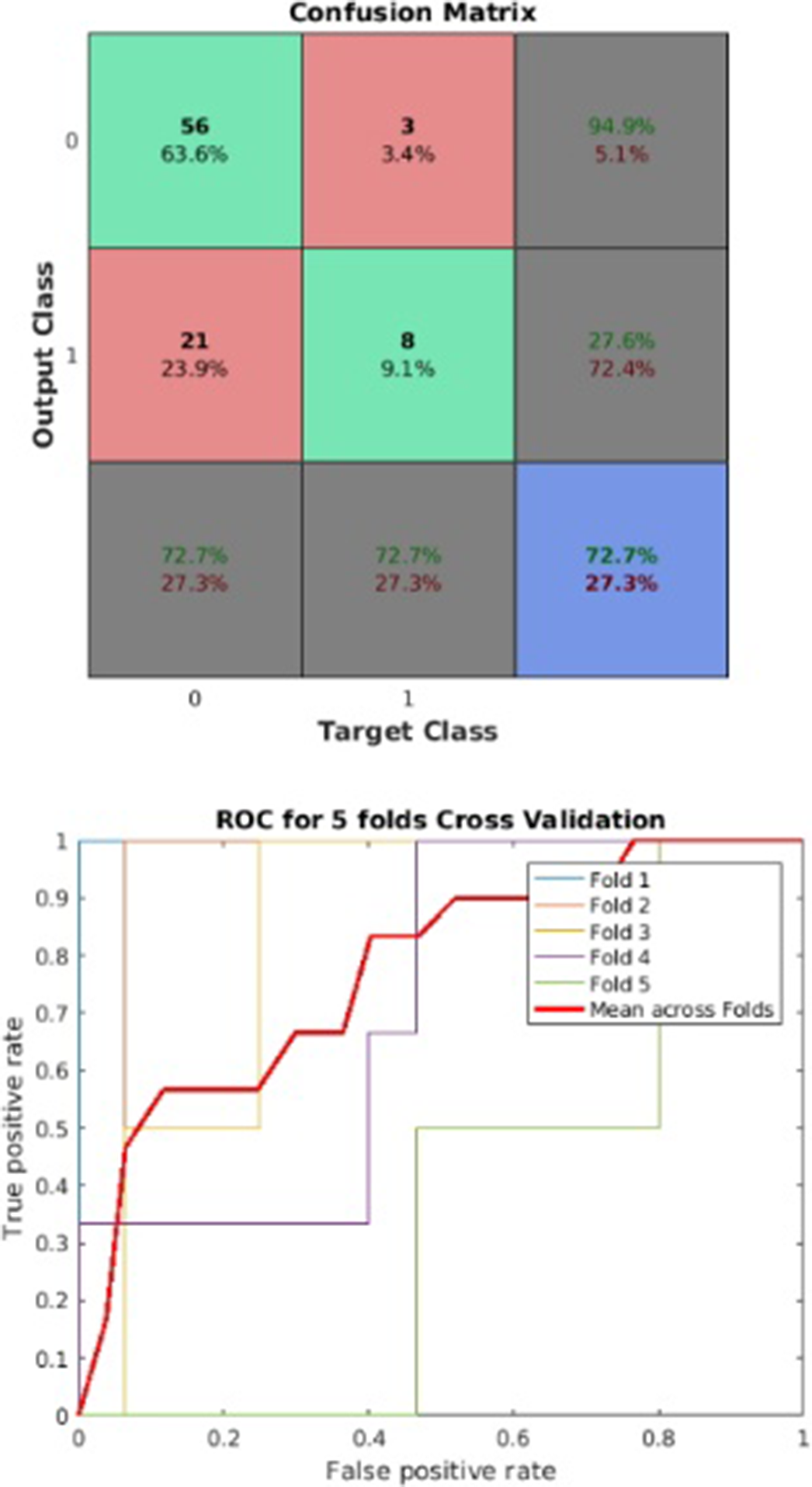
Image 2:
 Conclusions
ConclusionsThis is the first study highlighting a putative inflammatory signature of post-COVID depression. Consistently to the immune profile of Major Depressive disorder, upregulation of innate immunity mediators seems to foster depressive symptoms in the aftermath of COVID. Interestingly, recruiters of B and T cells promoting a physiological adaptive response to viral infection also mitigate its psychiatric sequelae. Understanding the biological basis of post-COVID depression could pave the way for personalized treatments capable of reducing its add-on burden.
Disclosure of InterestNone Declared
Identifying a predictive model of cognitive impairment in bipolar disorder patients: a machine learning study
- C. Monopoli, L. Fortaner-Uyà, F. Calesella, F. Colombo, B. Bravi, E. Maggioni, E. Tassi, I. Bollettini, S. Poletti, F. Benedetti, B. Vai
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S612
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar patients (BP) frequently have cognitive deficits, that impact on prognosis and quality of life. Finding biomarkers for this condition is essential to improve patients’ healthcare. Given the association between cognitive dysfunctions and structural brain abnormalities, we used a machine learning approach to identify patients with cognitive deficits.
ObjectivesThe aim of this study was to assess if structural neuroimaging data could identify patients with cognitive impairments in several domains using a machine learning framework.
MethodsDiffusion tensor imaging and T1-weighted images of 150 BP were acquired and both grey matter voxel-based morphometry (VBM) and tract-based white matter fractional anisotropy (FA) measures were extracted. Support vector machine (SVM) models were trained through a 10-fold nested cross-validation with subsampling. VBM and FA maps were entered separately and in combination as input features to discriminate BP with and without deficits in six cognitive domains, assessed through the Brief Assessment of Cognition in Schizophrenia.
ResultsThe best classification performance for each cognitive domain is illustrated in Table 1. FA was the most relevant neuroimaging modality for the prediction of verbal memory, verbal fluency, and executive functions deficits, whereas VBM was more predictive for working memory and motor speed domains.
Table 1. Performance of best classification models. Input feature Balance Accuracy (%) Specificity (%) Sensitivity (%) Verbal Memory FA 60.17 51.31 43 Verbal Fluency FA 57.67 62 53.33 Executive functions FA 60 63.33 56.67 Working Memory VBM 56.50 56 57 Motor speed VBM 53.50 47.67 59.33 Attention and processing speed VBM + FA 58.33 49.17 67.5 ConclusionsOverall, the tested SVM models showed a good predictive performance. Although only partially, our results suggest that different structural neuroimaging data can predict cognitive deficits in BP with accuracy higher than chance level. Unexpectedly, only for the attention and processing speed domain the best model was obtained combining the structural features. Future research may promote data fusion methods to develop better predictive models.
Disclosure of InterestNone Declared
Predicting Suicide Attempts among Major Depressive Disorder Patients with Structural Neuroimaging: A Machine Learning Approach
- L. Fortaner-Uyà, C. Monopoli, F. Calesella, F. Colombo, B. Bravi, E. Maggioni, E. Tassi, S. Poletti, I. Bollettini, F. Benedetti, B. Vai
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1111-S1112
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Every year at least one million people die by suicide, with major depressive disorder (MDD) being one of the major causes of suicide deaths. Current suicide risk assessments rely on subjective information, are time consuming, low predictive, and poorly reliable. Thus, finding objective biomarkers of suicidality is crucial to move clinical practice towards a precision psychiatry framework, enhancing suicide risk detection and prevention for MDD.
ObjectivesThe present study aimed at applying machine learning (ML) algorithms on both grey matter and white-matter voxel-wise data to discriminate MDD suicide attempters (SA) from non-attempters (nSA).
Methods91 currently depressed MDD patients (24 SA, 67 nSA) underwent a structural MRI session. T1-weighted images and diffusion tensor imaging scans were respectively pre-processed using Computational Atlas Toolbox 12 (CAT12) and spatial tract-based statistics (TBSS) on FSL, to obtain both voxel-based morphometry (VBM) and fractional anisotropy (FA) measures. Three classification models were built, entering whole-brain VBM and FA maps alone into a Support Vector Machine (SVM) and combining both modalities into a Multiple Kernel Learning (MKL) algorithm. All models were trained through a 5-fold nested cross-validation with subsampling to calculate reliable estimates of balanced accuracy, specificity, sensitivity, and area under the receiver operator curve (AUC).
ResultsModels’ performances are summarized in Table 1.
Table 1. Models’ performances.
Input features Algorithm Specificity Sensitivity Balanced accuracy AUC VBM SVM 55.00% 50.00% 52.50% 0.55 FA SVM 72.00% 54.00% 63.00% 0.62 VBM and FA MKL 68.00% 54.00% 61.00% 0.58 Abbreviations: AUC, area under the receiver operator curve; FA, fractional anisotropy; VBM, voxel-based morphometry.
ConclusionsOverall, although overcoming the random classification accuracy (i.e., 50%), performances of all models classifying SA and nSA MDD patients were moderate, possibly due to the imbalanced numerosity of classes, with SVM on FA reaching the highest accuracy. Thus, future studies may enlarge the sample and add different features (e.g., functional neuroimaging data) to develop an objective and reliable predictive model to assess and hence prevent suicide risk among MDD patients.
Disclosure of InterestNone Declared
The different effect of adverse childhood experiences on Theory of Mind brain networks in schizophrenia and healthy controls
- A. Pelucchi, F. Calesella, M. Bechi, R. Cavallaro, S. Poletti, B. Vai, F. Benedetti
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S373-S374
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Deficit in Theory of Mind (ToM) is a core feature of schizophrenia (SZ), while adverse childhood experiences (ACEs) can contribute to worsen ToM abilities through their effect on brain functioning, structure and connectivity.
ObjectivesHere, we investigated the effects of ACEs on brain functional connectivity (FC) during an affective and cognitive ToM task (AToM, CToM) in healthy control (HC) and SZ, and whether FC can predict the performance at the ToM task and patients’ symptoms severity.
MethodsThe sample included 26 HC and 33 SZ. In an fMRI session, participants performed a ToM task targeting affective and cognitive domains. Whole-brain FC patterns of local correlation (LC) and multivariate pattern analysis (MVPA) were extracted. The significant MVPA clusters were used as seeds in further seed-based connectivity analyses. Second-level analyses were modelled to investigate the interaction between ACEs, the diagnosis, and the task, corrected for age, sex, and equivalent doses of chlorpromazine (p<0.05 FWE). FC values significantly affected by ACEs (Risky Family Questionnaire) were entered in a cross-validated LASSO regression predicting symptoms severity (Positive and Negative Syndrome Scale, PANSS) and task performance measures (accuracy and response time).
ResultsIn AToM, LC showed significant different effects of ACE between HC and SZ in frontal pole, caudate and cerebellum. MVPA showed significant widespread interaction in cortico-limbic regions, including prefrontal cortex, precuneus, insula, parahippocampus, cingulate cortex, temporal pole, thalamus, and cerebellum in AToM and CToM. SBC analyses found significant target regions in the frontal pole, cerebellum, pre and postcentral gyrus, precuneus, lateral occipital cortex, angular gyrus, and paracingulate gyrus. LASSO regression predicted PANSS score (R2=0.49) and AToM response latency time (R2=0.37).
ConclusionsOur findings highlighted a widespread different effect of ACEs on brain FC in ToM networks in HC and SZ. Notably, the FC in these regions is predictive of behavioral ToM performance and clinical outcomes.
Disclosure of InterestNone Declared
Predicting unipolar and bipolar depression using inflammatory markers, neuroimaging and neuropsychological data: a machine learning study
- L. Raffaelli, F. Colombo, F. Calesella, L. Fortaner-Uya, I. Bollettini, C. Lorenzi, E. Maggioni, E. Tassi, S. Poletti, R. Zanardi, F. Attanasio, F. Benedetti, B. Vai
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S621
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
About 60% of bipolar disorder (BD) cases are initially misdiagnosed as major depressive disorder (MDD), preventing BD patients from receiving appropriate treatment. An urgency exists to identify reliable biomarkers for improving differential diagnosis (DD). Machine learning methods may help translate current knowledge on biomarkers of mood disorders into clinical practice by providing individual-level classification. No study so far has combined biological data with clinical data to provide a multifactorial predictive model for DD.
ObjectivesDefine a predictive algorithm for BD and MDD by integrating structural neuroimaging and inflammatory data with neuropsychological measures (NM). Two different algorithms were compared: multiple kernel learning (MKL) and elastic net regularized logistic regression (EN).
MethodsIn a sample of 141 subjects (70 MDD; 71 BD), two different models were implemented for each algorithm: 1) structural neuroimaging measures only (i.e. voxel-based morphometry (VBM), white matter fractional anisotropy (FA), and mean diffusivity (MD)); 2) VBM, FA, and MD combined with NM. In a subsample of 71 subjects (36 BD; 38 MDD), two similar models were implemented: 1) VBM, FA, and, MD combined with only NM; 2) VBM, FA, and MD combined with NM and peripheral inflammatory markers. Finally, the best model was selected for comparison with healthy controls (HC).
ResultsOverall, the EN model based on all the modalities achieved the highest accuracy (AUC = 90.2%), outperforming MKL (AUC=85%). EN correctly classified BD and MDD with a diagnostic accuracy of 78.3%, sensitivity of 75%, and specificity of 81.6%. The most significant predictors of BD (variable inclusion probability (VIP) > 80%) were the parahippocampal cingulate, interleukin 9, chemokine CCL5, posterior thalamic radiation, and internal capsule, whereas MDD was best predicted by chemokine CCL23, the anterior cerebellum, and the sagittal stratum. In contrast, NM did not help to differentiate between MDD and BD. However, they help to distinguish patients from HC. Psychomotor coordination and speed of information processing discriminated between MDD and HC (VIP>90%), whereas fluency, working memory, and executive functions differentiated between BD and HC (VIP>80%).
ConclusionsIn summary, BD was predicted by a strong proinflammatory profile, whereas MDD was identified by structural neuroimaging data. A multimodal approach offers additional instruments to improve personalized diagnosis in clinical practice and enhance the ability to make DD.
Disclosure of InterestNone Declared





