4 results
European federation of psychiatric trainees - Exchange Programme - appreciated by trainees in spite of language-related challenges
- F. H. Kraxner, A. Lengvenytė, M. C. Dias
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S320
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Differences in psychiatry training vary substantially across Europe. Such organisations as the European Federation of Psychiatry Trainees (EFPT), the European College of Neuropsychopharmacology, and the European Psychiatry Association, have committed to offer international experiences based on the premise that it could foster international collaboration, aid early career professionals to progress professionally and spark discussion regarding different practices across Europe.
To date, there are no studies that focus on the exchange experience in mental health professionals.
ObjectivesWe present the synthesis of the first seven years answers from 2012 to 2019 to the post-exchange online evaluation form, which trainees had to fill in in order to receive an attendance certificate.
MethodsThe present study analysed the answers of 182 psychiatry trainees or recent graduates who took part in the EFPT exchange program during 2012 and 2019 and filled in the internet-based evaluation form. The inclusion criteria were currently in training or recently finished training as a psychiatrist in Europe and filling in the questionnaire. The exclusion criterion was participation in the EFPT exchange program for the second or subsequent time.
All trainees were systemically asked to complete the online evaluation form after the exchange period. The form includes sociodemographic, training in host country-related, and exchange experience-related questions. Experience measures were evaluated using the 4-point Likert scale. Data was anonymized before the analysis. The study followed the principles of the Declaration of Helsinki.
ResultsFrom the 198 individuals who filled the questionnaire, 182 were involved in final analyses. The majority of participants were females in the second half of their training. The average age was 29 years. The largest number of applicants were from Turkey, whereas the United Kingdom hosted the most participants. One-third of the participants had previous international exchange experience.
Most trainees were exposed to both outpatient and inpatient treatment settings and were involved in educational or research activities. 96.7% of participants indicated that they were satisfied or very satisfied with the experience, 95.6% said that the exchange was useful or very useful, and 98.9% were likely or very likely to recommend exchange to colleagues. A description of trainees and exchange placements is presented in a table (couldn’t be uploaded).
ConclusionsTo our knowledge, this study is the first to assess the experience of psychiatry trainees who went on exchange during their professional training. Vast majority of trainees were satisfied with their exchange, thought it would be useful for their clinical practice and would recommend it to their colleagues. These findings are in line with other studies that examined medical exchange experiences .
Disclosure of InterestNone Declared
Diagnostic and psychopharmacotherapy in the general practictioner practice
- F. H. Kraxner
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S830
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Due to the often long-standing and extensive doctor-patient relationship, family doctors have special access to the mental state of their patients. They are often the first point of contact, and consequently the treatment of depression often begins in the GP’s practice or even takes place entirely there. This requires dedicated knowledge on the part of the general practitioner, especially with regard to diagnostic criteria and treatment.
ObjectivesThe aim of this article is to describe the basic diagnostic process for the general practitioner’s practice, to give advice on the indication and implementation of psychopharmacological interventions, and to present the results. This overview summarises the most relevant connections to the diagnosis, assessment of the severity and psychopharmacotherapy of depression in general practice.
MethodsThe following therapy algorithms and remarks are essentially based on the treatment recommendations of the Swiss Society for Psychiatry and Psychotherapy (SGPP) and the Swiss Society for Anxiety and Depression (SGAD) as well as the German S3 guideline of the German Society for Psychiatry and Psychotherapy, Psychosomatics and Neurology (DGPPN).
ResultsFamily doctors play a central role in the treatment of depressive disorders. They are often the first point of contact for patients with depression and in about 40 percent of cases even the only contact point. The likelihood of developing a depressive episode in the course of a lifetime is 10 to 15 percent globally. Evaluations by the World Health Organisation WHO show that 9 to 23 percent of people with chronic illnesses have depression as a concomitant illness. A cross-sectional epidemiological study in Germany showed that 60 percent of patients in general medical care were not treated with antidepressants and/or psychotherapy in accordance with guidelines. In Switzerland, about half of the antidepressants are currently prescribed by general practitioners. Image 1 shows a detailled overview (in German) of the current medication.
Image:
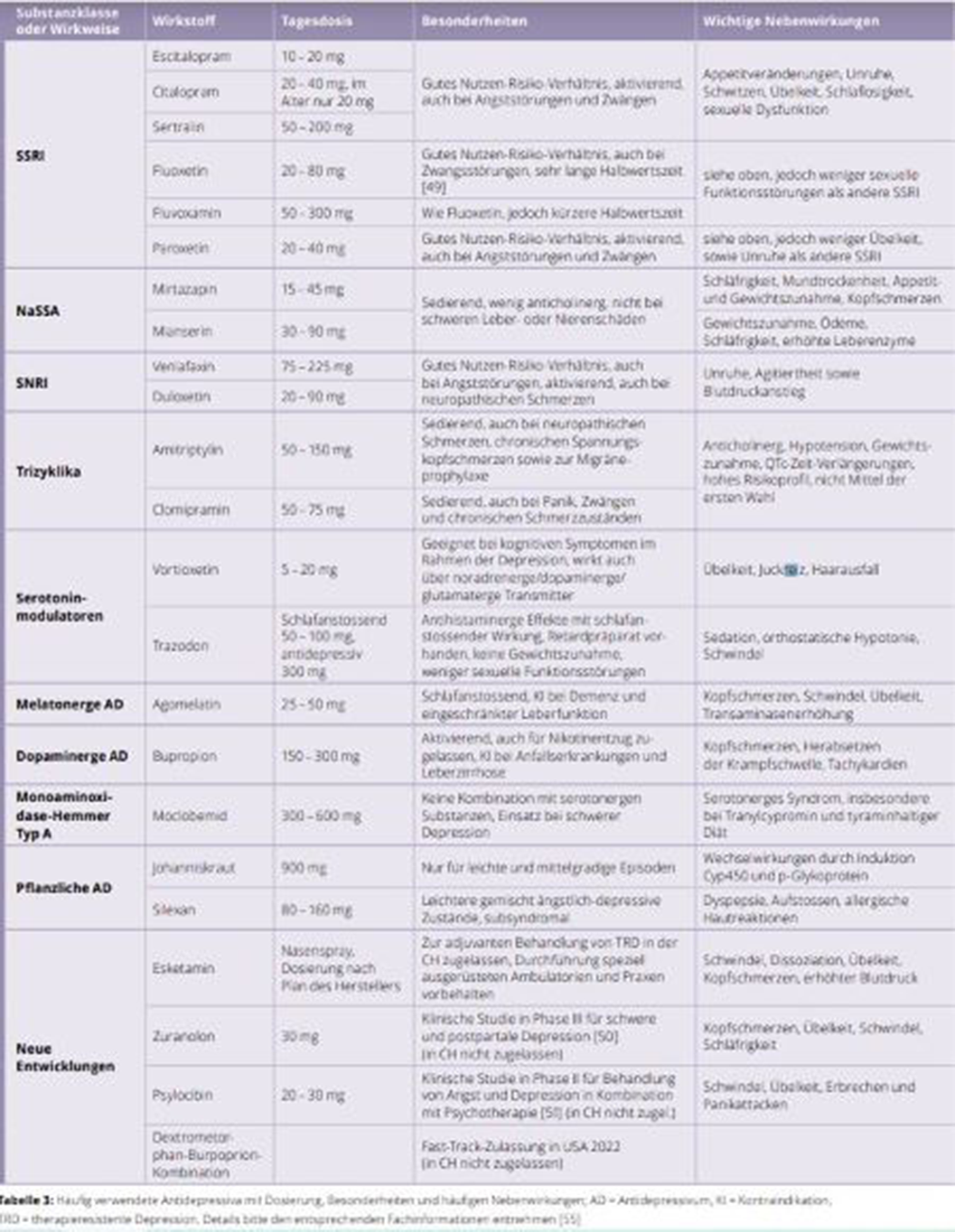 Conclusions
ConclusionsSpecialists in general internal medicine have a central role in recognition and treatment of depressive syndromes. Somatic causes can be ruled out by means of physical examination, laboratory and ECG/EEG/imaging. Mild and moderate depressive episodes can be treated by psychoeducation, counselling and medication. If the symptoms are mild, psychosocial support or psychotherapy alone can be considered. If acute suicidal tendencies or psychotic symptoms are identified, emergency symptoms, emergency admission to a psychiatric hospital should be considered.
The presence of other psychiatric comorbidities, resistance to therapy or complex psychiatric medication necessitate referral to outpatient specialists. Metabolic and cardiovascular side effects and interactions between psychopharmacological and internal medicine must be considered.
Disclosure of InterestNone Declared
Changing trends of suicide mortality from 2011 to 2019: an analysis of 38 European Countries
- G. Fico, A. Gimenez-Palomo, R. Andra Bursan, C. R. Ionescu, F. Kraxner, P. Rolland, S. Gomes-Rodrigues, M. Batković, E. Metaj, S. Tanyeri Kayahan, A. Mamikonyan, P. Paribello, A. K. Sikora, C. M. Platsa, M. Spasic Stojakovic, A. H. Halt, M. Az, N. Ovelian, K. Melamud, M. Janusz, K. Hinkov, C. Gramaglia, J. Beezhold, J. L. Castroman, C. Hanon, D. Eraslan, E. Olie
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S85-S86
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a serious public health problem since it accounts for nearly 900,000 deaths each year worldwide. Globally in 2019, 10.7 persons out of 100,000 died by suicide. Psychiatric disorders are related to an overwhelming proportion of these cases. In the last years, several specific interventions and action plans for suicide prevention have been implemented in a number of European countries.
ObjectivesOur aim was to analyze recent epidemiologic trends of suicide mortality rates in Europe.
MethodsAnnual national statistics of suicide mortality rates derived from Eurostat public databases from 2011 to 2019 were analyzed for 38 European countries. The suicide mortality rate was estimated per year/100,000 population. Linear regression models were used to study temporal trends of suicidal mortality. Analyses were performed using RStudio.
ResultsAvailable data show a statistically significant reduction in suicide mortality rates from 2011 to 2019 in 15 European countries, and a significant increase for Turkey (ES=0.32, SD=0.06, p=0.037) (Fig 1). The greatest significant decrease was reported in Lithuania (ES=-1.42, SD=0.02, p=0.02), followed by Hungary (ES=-1.13, SD=0.11, p=0.0007), Latvia (ES=-0.76, SD=0.11, p=0.007), and Poland (ES=-0.73, SD=0.10, p=0.001). Italy reported the lowest significant reduction in suicide mortality rates (ES=-0.13, SD=0.018, p=0.003). The remaining 16 countries showed no significant changes in suicide mortality trends.
Image:
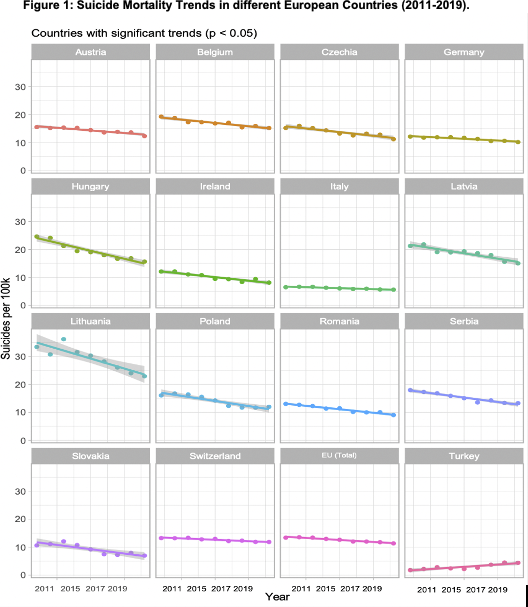 Conclusions
ConclusionsIn the last years, Europe registered an overall reduction in reported suicide rates. However, more recent data (i.e., suicide rates after COVID-19 pandemic, age and sex-related effect on suicide rates) should be analyzed and used to implement future recommendations. Current and future suicide prevention strategies aim to contribute to a greater reduction of suicide rates in the different European countries.
Disclosure of InterestNone Declared
Variable feelings of cohesion, trust, individualism and exclusion and their consequences on Swiss public mental health during the ongoing COVID-19 pandemic
- F. Kraxner
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S538
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The first cases of COVID-19 in Switzerland were related to the Milan cluster in February 2020. Border crossing restrictions were imposed and economic support measures worth 40 billion Swiss francs were announced. By 24th September 2021 Switzerland achieved a fully vaccination rate of 54%, confirmed 836’000 cases and 11’060 deaths.
ObjectivesThe objective was to describe and analyse the mental health of the general Swiss population under the ongoing COVID-19 pandemic and it’s social changes: including a case description, transgenerational influence and psychosocial treatment opportunities
MethodsTo answer the research question, I used deepened internet research, population interviews among different age gropus and colloquies with healthcare providers and federal authorities.
ResultsDifferent psychosocial phenomena lead to the transgenerational influence. Unfortunately, vaccination rate is slowed down by this pandemic’s impacts on public mental health. While during the first wave the positive feelings of cohesion and trust dominated, the mood changed afterwards to anxiousness and reactive individualism. Among all generations the fear of infection was shown to be a general booster of anxiety and distress. In fact, Swiss experts perceive the corona crisis as a catalysator for depression and anxiety disorders.
ConclusionsSpecific psychosocial treatment has to address general and individual vulnerability factors. However, staying in touch with family members, pursuing meaningful activities and being physically active can all help to overcome COVID-19 related mental health issues.
DisclosureNo significant relationships.





