12 results
Correlates of aggressive behavior in the moroccan context
- A. Tounsi, Z. Bencharfa, F. Azraf, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S284
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Violence among the mentally ill population has long been a subject of stigma, and controversy. Clinicians’ ability to assess the violent potential is still limited.
ObjectivesThe objective of this work is to identify the positively correlated indicators of aggressive behavior in patients admitted to hospital emergency departments.
MethodsIt is a retrospective and descriptive paper based on the records of patients admitted to the emergency department of Arrazi University Psychiatric Hospital in Salé during a one-month period.
The psychiatric diagnosis was formulated using the DSM-5 diagnostic criteria and Violent behavior was assessed using the Modified Overt Aggression Scale (MOAS). The existence of aggressive behavior was defined by a MOAS score ≥3.
We used SPSS 15 to analyse results
ResultsSixty-five case files were selected during the study month. The average age was 35.3 (19;64).
The mean of our sample MOAS aggression scale score was 31.5 [0; 79] and 90% of patients had a score ≥ 3 (image 1)
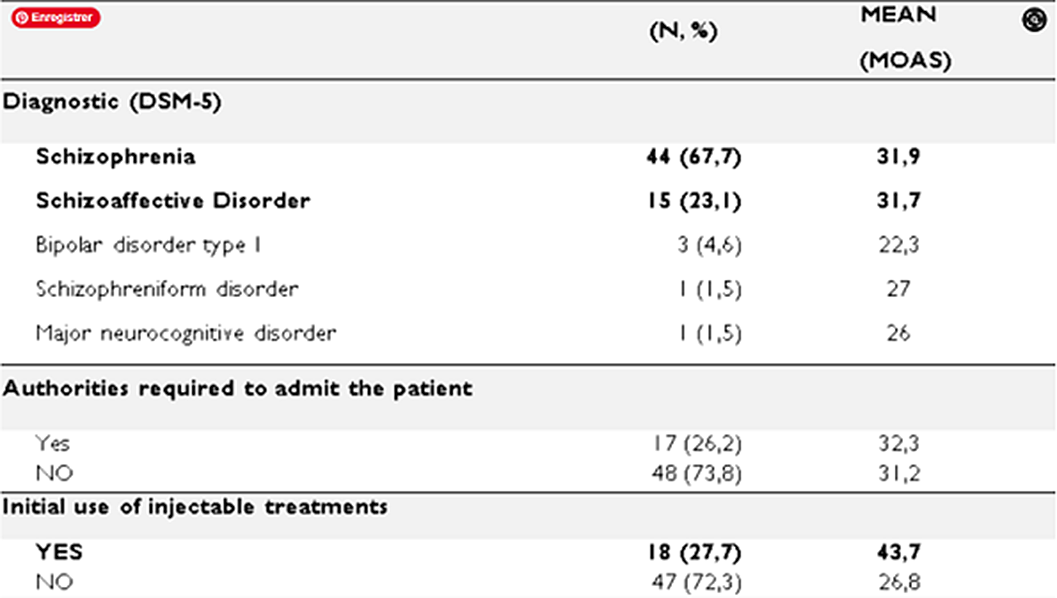
Among the 65 admissions, heteroaggressive risk was the most frequent reason for hospitalization (N=53), followed by psychomotor excitement. IMAGE 2
Statistical analysis revealed a significant association between high MOAS scores and substance use, history of suicide attempt, educational level and socioeconomic level
Image:
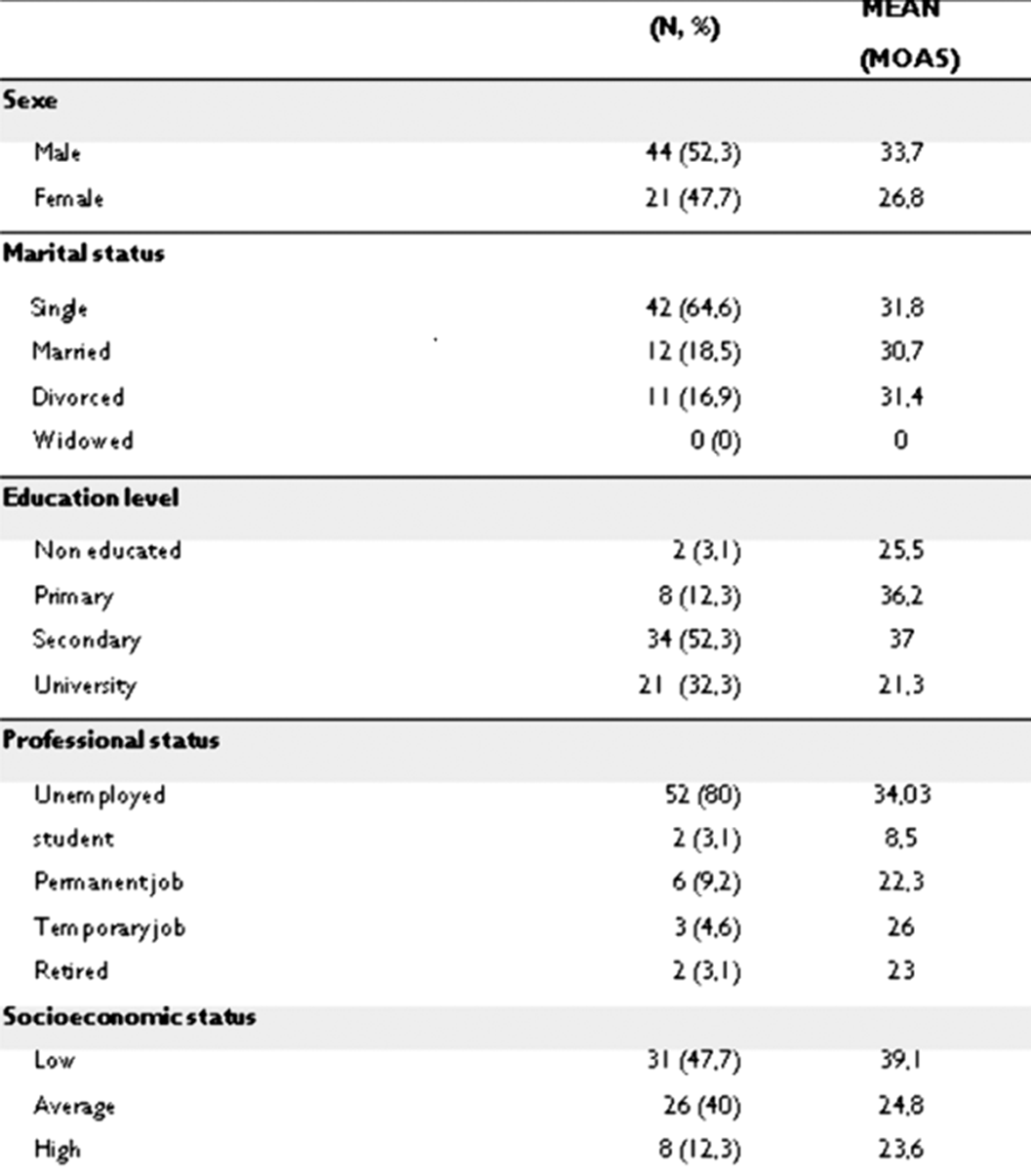
Image 2:
 Conclusions
ConclusionsIn the current research, the prevalence of aggressive behavior was high among these patients, which may be due to the conditions of psychiatric hospitalization in our region, which is often reserved for the most serious and dangerous patients.
Disclosure of InterestNone Declared
Hair loss due to Quetiapine usage : a case report
- A. Rhaouti, H. Boukidi, A. khallouk, F. Laboudi, O. Abderrazak
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S826
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hair loss is a common clinical complaint, resulting from a wide variety of causes, a variety of medications prescribed to treat mental diseases may contribute to hair loss.
ObjectivesAs far as we know, no previously published reports of alopecia associated with quetiapine were identified in Morocco.
Through this work we will try to expose the first case having this undesirable effect in our context, next to the rare cases in the literature.
MethodsThis article describes the experience of a 37-year-old male developing diffuse alopecia associated with use of quetiapin and recovering after cessation of the medicament is presented, besides presenting some rare cases that were found and described in other studies.
ResultsAmong these psychotropic agents, this side effect is most often reported with the use of valproic acid and lithium It has been also reported with the atypical antipsychotic medicines olanzapine and risperidone, but only rare cases were reported in relation to quetiapine, In this paper, a 37-year-old male patient developing diffuse alopecia associated with use of quetiapine and recovering after cessation of the medicament is presented.
ConclusionsThe results of this study are the first known in morocco, establishing a relationship between hair loss and the use of quetiapine will be taken in consideration while prescriping this medicine. These results confirm the relatively new idea of the impact of quetiapine on hair loss, unlike older studies which suggested good tolerance of this molecule.
Disclosure of InterestNone Declared
Relatives experience in moroccan psychiatric emergency
- A. Tounsi, B. Zineb, H. Chebli, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S862-S863
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In terms of care, family has a major role to play in the evolution of psychiatric illness.
Our aim in this work is to determine the family experience during the hospitalization of their sibling in the emergency room of the psychiatric university hospital Ar-Razi in Salé.
ObjectivesOur aim in this work is to determine the family experience during the hospitalization of their sibling in the emergency room of the psychiatric university hospital Ar-Razi in Salé.
MethodsOur work was carried out with families of patients admitted to the emergency department of the psychiatric university hospital Ar-Razi in Salé.
The data collection was carried out with the help of a questionnaire including several items.
ResultsSixty-five family members were included in this study. Their relatives hospitalized in the psychiatric emergency department were male in 70% of cases with an average age of 32.4 years.
- In 76% of the cases, the family member interviewed was the one who requested hospitalization;
- 55% of those interviewed were parents.
The analysis of relatives’ feelings during the hospitalization showed:
- Feelings of guilt were related to feelings of fear of exclusion and worries.
- Feelings of fear and exclusion were mostly expressed by mothers of patients hospitalized for the first time
At the end of the hospitalisation, 90% expressed relief, and 85% of family members were satisfied with their relative’s stay in the psychiatric emergency department.
ConclusionsRecognizing families as units of care and understanding their situation and experiences facilitates the post-hospitalization care process. A well-informed family about mental illness and the types of therapeutic treatments available helps optimize the treatment.
Disclosure of InterestNone Declared
Psychiatric disorders in women hospitalized at the arrazi psychiatric hospital
- H. Berrada, F. Azraf, A. Tounsi, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S952
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women get hospitalized for various serious mental disorders that are gender specific, half of them married with children, the other half single\divorced women stigmatized and marginalized in our society.
ObjectivesThe aim of this study is to describe mentally ill women admitted into the psychiatric hospital, socio demographically and clinically, highlighting differences, specificities and multiple roles distress deviate with the course of disorder.
MethodsThis is a prospective cross-sectional study involving 50 patients admitted to Ar-razi Psychiatric Hospital
ResultsThe average age is 39years, 41% of them are single, with a low educational level (primary school). 77% of our women are from the urban region, 59% are jobless. 19% of patients in our study have positive family history, 65% of them suffered from schizophrenia. 65% of patients are admitted for schizophrenia, followed by bipolar I disorder 22%, MDD is only represented by 10%. 25% of inpatients deal with a toxic habit, 18,5% abuse nicotine and only one woman have tried quitting. Suicide attempts are closely linked to major depressive episodes of MDD and BID, in patients were already under a combination of antidepressants and anxiolytics for at least 3 months. Psychotic features are observed in most of admitted disorders, 80% in BIP and 64% in MDD. According to HAMILTON-DEPRESSION 62,9% of women are admitted for a severe depressive episode, 30% present anxiety comorbidity and a history of CBT sessions months prior hospitalization.
ConclusionsShading the light into admitted women in psychiatry and deciphering specific demographic, clinical and therapeutic features may improve the global care system and women’s adherence to treatment and follow up.
Disclosure of InterestNone Declared
Representations of long-acting antipsychotics in patients at the Arrazi hospital in Salé Morocco
- H. Chebli, A. Tounsi, H. Berrada, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S265
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since the appearance of long-acting antipsychotics (LAPAs) and given the high frequency of non-adherence to treatment in psychotic disorders, LAPAs have recognized a resurgence of interest in the psychiatric literature. These long-acting drugs may pose ethical issues (e.g. limitation of freedom).
ObjectivesThe present study aims to determine the representations of long-acting antipsychotics in patients followed at Arrazi Hospital in Salé.
MethodsDescriptive study carried out with patients hospitalized at the Arrazi hospital in Salé and those followed in consultation who are on APAP or who have already used it. The collection of information is done using an exploitation sheet
ResultsAPAPs have been used for less than 5 years by 53.8% of patients84.6% of participants do not use APAP bychoice, in 79.2% of cases it was the doctor’s decision and in 20.8% of cases it was the family’s choiceMonotherapytreatment was the most cited benefit by our patients (76.9%)The route of administration of APAP by intramuscular injection is the problem encountered in 57.7% of our patients, while11.5% of patients find no inconvenience for the use of these psychotropics.
ConclusionsNegative beliefs associated with the treatment contribute to a very large part to the lack of compliance, onthe contrary, long-acting antipsychotics may be better accepted by patients when taking into account the patients’ beliefsand preferences in the development of the treatment. therapeutic project
Disclosure of InterestNone Declared
Caesarean section and post traumatic stress disorder
- H. Chebli, M. Chtibi, F. Azraf, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S977
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Childbirth can be a very painful experience, especially vaginally. It can have many complications. The obstetrical complications of caesarean section are well studied but its psychological complications are little mentioned. Most women recover quickly after giving birth, but others seem to have more difficulty. Researchers have attempted to identify perinatal risk factors for the development of post-traumatic stress disorder in parturients and caesarean section seems to be one of the predictors.
ObjectivesThe objective of our study is to detect post traumatic stress disorder in women after vaginal delivery.
MethodsThis is a cross-sectional descriptive study conducted among women from the general population who have given birth vaginally. The information was collected using a questionnaire distributed on social networks. Symptom severity was quantified using the PTSD checklist for DSM-V (PCL-5).PCL-5 is a 20-item self-assessment that measures the 20 DSM-5 symptoms of PTSD. She rates each symptom from 0 (not at all) to 4 (extremely). The score varies from 0 to 80. A threshold of 33 allows screening for post-traumatic stress disorder.
Results61 women took part in this study, 81.5% of whom gave birth vaginally between the ages of 20 and 30.70.3% of the participants gave birth vaginally once, 44.4% twice and 7.3% of the women in our sample had a caesarean three times.Regarding the indication of the high way in our sample: the narrowing of the pelvis and fetal distress were in 22.2%. Exceeding term was in 18.5% of cases.In our sample, 59.3% of the women had planned their vaginal delivery and 40.7% had given birth urgently.Regarding the results of the PCL-5 scale (PTSD checklist for DSM-V), the score varies between 0 and 48 with a median score equal to 12. 3.7% of the participants had a score greater than 33.
ConclusionsPost-traumatic stress disorder can accompany childbirth, especially when it is high and in an emergency. Postpartum post traumatic stress disorder affects the mother-child relationship and can be complicated by depressive disorder. Medical monitoring of pregnancy, good medical and family support for the parturient and preparation for childbirth are necessary to better start the maternity experience.
Disclosure of InterestNone Declared
Comorbid anxiety has schizophrenia diagnosis and management modality
- A. Korchi, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S679-S680
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a chronic psychiatric disorder with disorganization progressive and important affecting several spheres: thought, affectivity, cognition and social life of the subject. It is a serious mental disorder with a prevalence of nearly 1%.
Men would present more premorbid difficulties, but the overall prevalence of symptoms of schizophrenia is similar in both sexes.
When it comes to comorbidity, men and women are vulnerable to somewhat different health issues.
Anxiety symptoms are one of the main symptoms in patients with schizophrenia, but the effect of anxiety symptoms on patients is easily overlooked.
About 40% have persistent anxiety symptoms in patients with schizophrenia, and whether they are accompanied depressive symptoms, the symptoms may have a greater impact on the patients. We need to help patients avoid suicide when the symptoms depression appear.
Hallucinations auditory, anxiety symptoms and depressive symptoms may exist simultaneously in patients with schizophrenia.
Most studies focus on studying the relationship between auditory hallucinatory symptoms and depressive symptoms in patients with schizophrenia, the relationship between auditory hallucinatory symptoms and anxiety symptoms, or the relationship between anxiety symptoms and symptoms depressive
ObjectivesThe objective of this study is to resolve important questions concerning the interaction of anxiety and schizophrenia in patients followed in psychiatry at Arrazi Hospital .
MethodsDescriptive and analytical cross-sectional study, conducted over a period from May 2022 to October 2022 in patients consulted in Arrazi de Salé, using a questionnaire grouping together the sociodemographic characteristics, the risks and the advantages of antipsychotics, medical comorbidities and the mobilization of psychosocial support, and thus the BPRS Anxiety Rating Scale.
ResultsOf the 42 patients who completed the study, 18 were female and 24 were male 60% were single. The average age was 36.63 years, 60% have secondary education, 25% primary, and 15% university level, 30% have a family history of schizophrenia.
32 were taking an atypical antipsychotic, 10 were taking classic neuroleptics.
Most schizophrenics encountered in psychiatry are stabilized on antipsychotic treatment, and those who have an anxious comorbidity are still too often underestimated , put on the account of the positive symptoms and the negative symptoms of schizophrenia, it is insufficiently diagnosed and treated.
The effect of anxiety symptoms on patients is easily overlooked.
It should be kept in mind that anxiety in schizophrenia requires special attention when discussing and prescribing antipsychotic medications.
ConclusionsOptimal interventions for patients with comorbid schizophrenia and anxiety differ by quality of life.
At all consultations, preventive strategies should consider mindful interviews and the risks and benefits of treatment for schizophrenia and comorbidities.
Disclosure of InterestNone Declared
Schizophrenia: the announcement of the diagnosis
- F. Azraf, M. Chtibi, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1055
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For many years, the question of the announcement of the diagnosis in psychiatry has been controversial. It is the starting point of a management allowing access to psychoeducation and to the patient’s recovery. In the case of schizophrenia, the cognitive impairment and the stigmatizing nature of the pathology jeopardize the announcement of the diagnosis. However, recommendations and legislation emphasize the need to inform the patient about his or her pathology. In Morocco, the law n° 131-13 of February 19, 2015 relating to the practice of medicine has made information about the diagnosis to patients an obligation for doctors and a right for patients
ObjectivesThe interest of our work is to try to evaluate the current state of this practice, its ethics and its representations among psychiatrists.
MethodsThis is a descriptive study on the announcement of the diagnosis of schizophrenia in a population of psychiatrists. The data collection was carried out by a questionnaire including: Socio-demographic and professional data, opinion on practice and training concerning diagnostic announcement in psychiatry, physicians’ representations concerning announcement: frequency, opinion on the importance of this practice.
Results31 participants responded to our questionnaire. More than 9 out of 10 participants would not benefit from training on diagnostic announcement. Only 22.6% of physicians reported being very or somewhat familiar with medical information laws and their content regarding the regulation of diagnostic announcement. All participants considered schizophrenia to be the most difficult pathology to announce, followed by personality disorders and bipolar disorder. 74.2 of the participants considered it “rather” or “completely” essential to inform the patient of his or her psychiatric diagnosis. 77.4% of the participants considered it necessary to announce the diagnosis of schizophrenia and 80.7 often or systematically announce this diagnosis. Three situations considered appropriate to announce a diagnosis of schizophrenia: 74.2% announce it in general when the patient or the family asks for information about the diagnosis, 42% advise the patient when he/she mentions schizophrenia on his/her own. The patient’s functional inability to understand the diagnosis (77.4%) and the fear of negative clinical and therapeutic repercussions (41.9 and 38.7 respectively) were reported to deter physicians from making the announcement. More than half of the participants (64.5%) thought that the announcement of the diagnosis improved therapeutic compliance. Conversely, 35.5% considered that the announcement had no impact on therapeutic compliance.
ConclusionsThe announcement of the diagnosis of schizophrenia remains today a complex and evolving subject. Even if great progress has been made to inform patients as well as possible, practices remain disparate from one doctor to another and this information is not well traced.
Disclosure of InterestNone Declared
Post-traumatic stress disorder and restraint in patients followed at Arrazi Hospital
- L. Azizi, O. Seyar, N. Baabouchi, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S979
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Post-traumatic stress disorder (PTSD) is characterized by intense, unpleasant, and dysfunctional reactions that appear after an overwhelming traumatic event. A life-threatening or serious injury event can cause lasting and intense suffering.
Hospitalization without consent, the use of isolation techniques, restraint or the obligation to take treatment are situations that can be perceived as traumatic.
ObjectivesOur goal is: The search for the existence of psycho-pathological links and vulnerabilities between the state of post-traumatic stress and physical restraint. Consideration of the traumatic event in the development of appropriate care strategies.
Our goal is:The search for the existence of psycho-pathological links and vulnerabilities between the state of post-traumatic stress and physical restraint.Consideration of the traumatic event in the development of appropriate care strategies.
MethodsTo meet this objective, we carried out a descriptive study which identified 200 cases collected in the psychiatric emergency department of the Arrazi Hospital in Salé from 2017 to 2021. An exploitation sheet was drawn up and the study was carried out using Meta-chart and Visuel-chart software.
ResultsAt the end of this work we found: The average age is 35 years +/- the sex ratio is equal to 1.42. 80% are single while 10% are divorced. Regarding professional activity, 70% are unemployed. 10% of patients have a level of education above the baccalaureate.
As for the history, 60% of the cases studied have a personal psycho-addictive history. 34.6% of the cases studied have a medical-surgical history.
The psychiatric pathologies that were found are: 10% suffer from depressive disorder, 80% have psychosis, 10% have attempted suicide.
ConclusionsDuring an acute episode, patients may be exposed to coercive treatments. Hospitalization without consent, the use of isolation techniques, restraint or the obligation to take treatment are all factors that can be perceived as traumatic. For example, patients recently exposed to a first psychotic episode confirmed the traumatic character of the psychotic episode itself, of the treatment or of both.
Disclosure of InterestNone Declared
Cannabis and society: families’ perceptions of cannabis consumption
- H. Chebli, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S661
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cannabis is an illicit substance whose use is very common among the patients we see daily in hospitals. Its use is not simply a “recreational” desire, but above all an attempt at self-medication in order to manage emotions that have become too painful. However, even if cannabis reduces the symptomatology in the moment, it worsens most psychiatric pathologies.
ObjectivesThe purpose of this study is to assess the experiences of cannabis users’ families.
MethodsThe survey was carried out among the families of patients hospitalized at the Arrazi Hospital in Salé and those followed in consultation and who use cannabis. The collection of information is done with the help of an exploitation form.
Results34.6% of the participating families put bad company as the cause of consumption, followed by family problems, psychiatric problems come in 3rd position with a percentage of 19.2%. Cannabis use is considered as a disease in 52.8% of the families participating in the study. 58.5% of the families distinguish between good and bad cannabis use and define bad use by the use of large quantities of cannabis in 34.2% of the cases. The majority of the participating families (86.8%) saw cannabis as aggravating their loved one’s mental illness.
ConclusionsThe understanding of the perceptions of the families towards the use of cannabis by their close relatives as well as the correction of the false perceptions will help to establish better prevention programs and better patient care especially with the family therapy which showed its utility in the management of the patients having disorders related to the use of cannabis.
Disclosure of InterestNone Declared
Eating disorder and suicide attempt
- A. Chaara, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S581-S582
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The quantification of suicidal risk in specific populations is important for the adoption of prevention and risk reduction measures. This risk remains very high in patients with eating disorders compared to the general population.
ObjectivesThe present study evaluates the prevalence of suicide among patients with eating disorders all seeking different suicidal risk factors in these patients.
MethodsA retrospective study of medical records of all patients with eating disorders, diagnosed according to DSM 5 criteria, at Arrazi hospital of Salé for the past 14 years, by assessing the prevalence of suicide attempts and care.
ResultsIn our work, all patients are female, 17 years old on average, 18 patients out of 20 have anorexia nervosa, 4 of them have had bouts of bulimia, and only one patient was admitted for management of bulimia nervosa alone. The mean age of onset was 15 years with addictive comorbidity in 5 patients.
Thirteen patients had comorbid depressive disorder, one patient was schizophrenic and six patients had borderline personality disorder.
12 patients have made suicide attempts, planned especially in a depressive environment.
ConclusionsPreventive management of suicidal risk must be taken in order to improve the prognosis in this category of patients.
DisclosureNo significant relationships.
Hospitalization in Psychiatry: Patients’ experiences at Arrazi Psychiatric Hospital in Morocco
- A. Chaara, F. Laboudi, A. Ouanass
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S599
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hospitalization in psychiatry is marked by the use of care without consent.
We therefore proposed to study from this perspective the feelings and opinions of patients on such an experience.
ObjectivesThe objective of this work is to explore the experiences of patients and their perception of the effects of this hospitalization, through 3 fundamental ethical principles: Autonomy, beneficence and non-maleficence.
MethodsThis study will be conducted at Arrazi Psychitaric Hospital, in patients at the end of their stay, via a questionnaire.
ResultsA total of 122 patients attended the study. A very large proportion of patients were satisfied with the premises, space planning, and had knowledge of a structured planning of the organization of care. A senior doctor was identified by 95% of them. Eighty five per cent were free to move around in the hospital.
The information on the care offered was perceived by 83.7%. The rates are lower with respect to clear explanations received on the disease, the effects of drugs and the type of hospitalization.
Regarding the feelings experienced during the stay, 83% of people who spoke mentioned a painful experience. The feelings that prevailed were a feeling of helplessness, fear, worthlessness. On the other hand, a majority of patients expressed that the hospitalization had protective effects towards themselves and towards others, but that it wasn’t justified.
ConclusionsThese results suggest that autonomy and beneficence are respected. Therefore, an attention should be paid to various information given during the stay.
DisclosureNo significant relationships.





