3 results
Social media influence on Eating Disorders since COVID-19 pandemic: a pilot study
- F. Micanti, G. Spennato, R. Claudio, E. Amoroso, M. D’Ambrosio, V. M. Saia, A. Barone, M. Tadic, D. Galletta, M. Vannini
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S218
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies show a negative impact of mass media contents on adolescents’ mental health, especially on perceived body uneasiness. COVID-19 lockdown determined an increased use of social networks (SN). Psychiatrists highlighted an increase in Eating Disorders’ (ED) diagnoses.
ObjectivesThe aim of this study is to assess the pattern of SN use in patients with ED using a self-administered questionnaire.
Methods30 patients with clinical diagnosis of ED (Anorexia nervosa, Bulimia nervosa or Binge eating disorder) admitted to the ED unit, underwent clinical assessment, and filed a questionnaire on SN use. The questionnaire assesses time spent on SN, weight-control apps use, exposure to fitness- or food-related contents and to ED-promoting contents, distractibility, weight changes and feeling of body uneasiness.
ResultsMean age was 20.63 (SD 4.71), mean BMI 20.24 (SD 5.27); 93.3% (28) of patients were females. Eating behaviours were divided into restrictive type (66.7%, 20) or binge/bulimic (33.3%, 10). 16.7% (5) of patients reported self-injury behaviours. In 46.7% (14) of cases, the onset of the ED occurred during COVID-19 pandemic; the remaining 53.3% (16) experienced a relapse of a previous ED during this period. 66.7% (20) of subjects reported an increased use of social media and fitness apps. 90% (27) experienced weight changes during the pandemic, with 76.7% (23) seeking nutritional or psychological interventions. 53.3% (16) perceived an increase in body- or food-related contents on their SN feeds, with 50% declaring of knowing the meaning of the terms pro-ana and pro-mia.
Table 1 displays reported answers to the questionnaire. Table 2 shows mean age of patients according to self-injury behaviours and to the onset time of ED.
Table 1. Questionnaire subscales (n) Rarely occurred % (n) Often occurred % (n) Increase of time spent on SNs (30) 33.3% (10) 66.7% (20) Distractibility (30) 70% (21) 30% (9) Self-injury contents (30) 96.7% (1) 3.3% (29) Body uneasiness (30) 26.7% (8) 73.3% (22) Pro-ana/pro-mia contents influence (15) 53.3% (8) 46.7% (7) Body- and food-related contents influence (30) 20% (6) 80% (24) Table 2. Eating disorders features (n) Mean age (SD) Self-injury – Yes (5) 18.20 (1.92) p<0.05 Self-injury – No (25) 21.12 (4.97) Onset during Covid-19 pandemic (14) 18.29 (1.82) p<0.01 Worsening during Covid-19 pandemic (16) 22.69 (5.51) ConclusionsED onset during the COVID-19 pandemic and self-injury behaviours appear as pivotal characteristics of younger patients, displaying a greater severity of the disorder in our clinical experience. With a more consistent number of patients, it would be possible to correlate SN use and body- and food-related contents to the onset and the severity of ED, focusing on pandemic periods.
Disclosure of InterestNone Declared
The relationship between alexithymia and Nyght Eating Syndrome
- F. Micanti, E. Amoroso, M. Vannini, C. Ricci, G. Spennato, M. D’Ambrosio, M. Billeci, H. Lamberti
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S421-S422
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
NES is characterized by daytime anorexia, sleep difficulties with nocturnal food intake, resulting in obesity (Stunkard et al. Am J of Med. 1955; 19 78-86). Alexithymia refers to the impairment in recognizing and describing feelings. The impairment in distinguishing emotions from body sensations may lead patients to confuse emotional arousal with physical hunger (Sifneos et al. Mod. trends psychosom. med. 1976; 3 430-439). This mechanism could lead to nocturnal food intake. Alexithymia was firstly described in BED and was related to BED severity.
ObjectivesTo our knowledge no studies have investigated the relationship between alexithymia and NES. The aim of the present study was to assess alexithymia in patients with NES, to improve surgical and nutritional outcomes.
Methods110 patients with clinical diagnosis of NES admitted to the Eating Disorder Unit, between 2013 and 2022 underwent psychiatric assessment for bariatric surgery. Clinical assessment consisted of clinical interview and the following psychometric rating scales: 20-item Toronto Alexithymia Scale; Eating Disorder Inventory 2, specifically the Interoceptive Awareness subscale; Barratt Impulsiveness Scale; Binge Eating Scale.
ResultsThe mean BES score was 24.14(SD 8.23), computed on 107 patients, of which 16 (14.5%) had no or minimal binge eating problems and 91 (82.7%) had moderate-severe binge eating problems. The mean TAS total score was 55.11(12.92), computed on 103 patients. 42 patients had a TAS-20 total score ≤50 and were categorized as non-alexithymic, and 61 had a TAS-20 total score >50 and were categorized as alexithymic. Simple linear regression was used to test if TAS-20 total score significantly predicted EDI-IA in the whole sample (97 patients). The overall regression was statistically significant (R2=0.27, F(1,96)=35.46, p< .001) and TAS total score significantly predicted EDI-IA score (β=0.519, p<.001). In the alexithymic group, the regression was statistically significant (R2=0.305, F(1,57)=25.07, p< .001) and TAS total score significantly predicted EDI-IA score (β=0.553, p<.001).
Whole sample Alexithymic Non-alexithymic p Female (%) 79(71.8) N=110 48(64.9) N=62 26(35.1) N=42 .087 Age mean(SD) 36.41(12.6) N=110 34.65(12.7) N=62 38.48(11.31) N=42 .11 BMI mean(SD) 44.05(7.61) N=106 43.97(7.9) N=60 43.82(7.38) N=40 .92 TAS mean(SD) 55.11(12.92) N=103 64.05(7.06) N=61 42.12(7.13) N=42 <.001* BIS mean(SD) 67.58(10.35) N=98 70.07(9.93) N=59 63.26 (9.85) N=35 .002* BES mean(SD) 24.14(8.23) N=107 25.7(6.89) N=62 21(9.25) N=40 .004* EDI-IA mean(SD) 8.95(6.44) N=103 10.82(7) N=60 6.05(4.44) N=39 .000* * significant difference between alexithymic and non-alexithymic groups according to independent sample t-test.
Image:
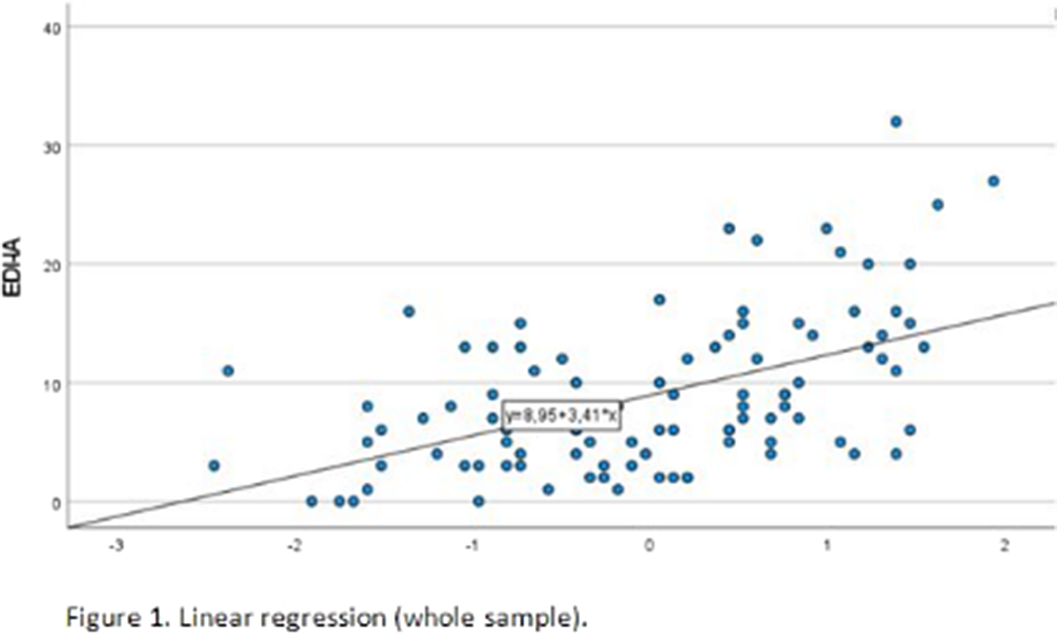
Image 2:
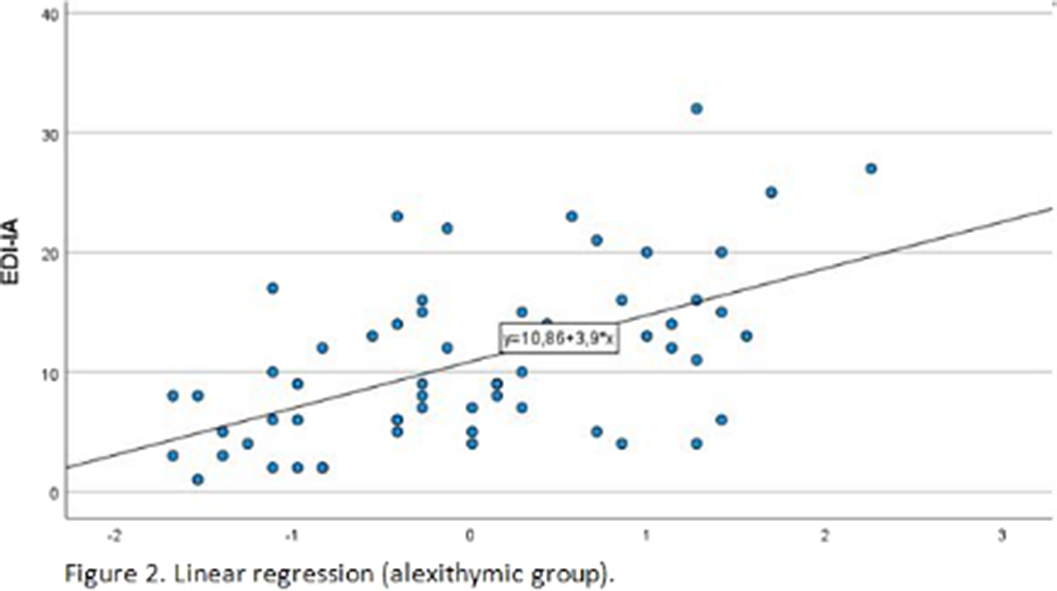 Conclusions
ConclusionsIn patients with NES, alexithymia significantly predicts poor interoceptive awareness, thus explaining excessive nocturnal food intake.
Disclosure of InterestNone Declared
EPA-1116 - Obesity Affects Cognitive Performances Even in the Absence of Obvious Psychopathological Alterations. A Comparison with Schizophrenia Subjects and Non-Affected Controls
- R. Balletta, C. Cucciniello, M. Formato, G. Pecoraro, S. Orlando, G. Mazzola, C. Avagliano, G. Fico, A. De Bartolomeis, F. Micanti, F. Iasevoli
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Obesity has been associated with cognitive impairment. However, it is not clear whether cognitive impairment may depend on concomitant psychopathology, since several psychiatric conditions, e.g. schizophrenia, include cognitive deficits among their manifestations.
Objectives:To assess cognitive performances and psychopathology in obese patients, and to compare cognitive alterations in obese patients with those in schizophrenics and controls.
Aims:To compare cognitive performances in obese patients to normal percentiles. To provide an analysis of correlation with specific psychopathological domains. To evaluate whether cognitive performances in very obese patients were different from those in schizophrenia patients and non-affected controls.
Methods:88 obese patients were included. Exclusion criteria were: axis I and II diagnosis; severe medical, neurological, or endocrinology conditions. Patients underwent an extensive battery of cognitive tests and completed the Toronto Alexithymia Scale (TAS-20), the Barratt Impulsiveness Scale (BIS-11), the Beck Depression Inventory (BDI), the State-Trait Anxiety Inventory (STAI). In the second part of the study, very obese patients (BMI>40; n=16) were compared for cognitive performances to schizophrenia patients (n=16) and non-affected controls (n=17).
Results:Obese patients performed at low percentiles (<15) on the Problem Solving and the Social Cognition tasks. Mean scores on psychopathology rating scales did not reach abnormal values. No correlation was found with psychopathology. When compared to schizophrenics, no significant differences were found in performances on spatial working memory.
Discussion:Obese patients show cognitive alterations even in the absence of abnormal psychopathology. Very obese patients share cognitive alterations with schizophrenia patients, which may imply common neurobiological basis.





