3 results
Transcranial magnetic stimulation for catatonia: case series
- G. Mamedova, N. Zakharova
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1019
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Catatonia is diagnosed in 5–43% of patients with various mental disorders, thus actualizing the problem of elaborating therapeutic interventions for catatonia on an outpatient basis. Although the current experience in application of transcranial magnetic stimulation (TMS) in catatonia is limited, it provides promising data on positive effect of dorsolateral prefrontal cortex (DLPFC) stimulation in a series of clinical observations. According to the available data, TMS shows comparable efficacy with electroconvulsive therapy, but unlike it is safe and does not require general anesthesia in intensive care unit.
Objectivesto evaluate the efficacy and safety of TMS in the treatment of catatonia in patients with mental disorders
MethodsFour patients were diagnosed with catatonia as part of schizophrenia spectrum disorders in three cases (P1,4,7) and in one case within the structure of recurrent depression phase (P8). Psychopathological examination includes PANSS, SAS, NSA-4, BFCRS, NCRS, and BACS.
Personalized choice of stimulation protocol was determined by rCBF lateralization in DLPFC reflecting the neuronal activity in that region: 1) P1, P4, and P8 underwent 20 sessions of high-frequency stimulation at the frequency of 20 Hz with the amplitude of 120% MT in the projection of left DLPFC 2) P7 underwent 20 sessions of low-frequency stimulation at the frequency of 1 Hz with the amplitude of 120% MT in the projection of right DLPFC
ResultsSafety evaluation was performed daily during TMS sessions. None of participants reported any adverse events at high compliance.
The efficacy was estimated during by the following criteria: 1) positive clinical response: decline of BFCRS and NCRS scores by 70% from the primary evaluation 2) achievement symptomatic remission (total BFCRS and NCRS score 3 and less).
Positive clinical response was detected in all four patients, however, symptomatic remission was formed only in two of them (P1 and P4) referring to BFCRS.
Evaluation of neurotransmitter concentration: P1, P7, P8 showed a tendency for absolute and relative glutamate concentration values to approach normal. After the TMS course GABA concentration diminished in all cases but P4, in whom the elevation of GABA level was registered.
ConclusionsTMS potentially activates metabolic processes in brain tissues, thus promoting deceleration of pathological mechanisms and potentiating neuroplasticity with procognitive effect, expressed primarily in the increase of processing speed and response to it, as well as in the improvement of working memory. To summarize, the influence of TMS on local brain regions makes it possible to achieve a positive clinical effect in treatment of catatonia.
No strong and unequivocal results were received for the efficacy of TMS in treatment of catatonia. A positive clinical effect was seen, however, insufficient for achieving remission in the majority of subjects.
Disclosure of InterestNone Declared
Decrease in anterior cingulate cortex GABA in schizophrenia at early stage
- A. Manzhurtsev, S. Nevzorova, M. Ublinskiy, L. Mosina, I. Melnikov, G. Mamedova, V. Ushakov, N. Zakharova, M. Shlyapnikov, D. Andreyuk, T. Akhadov
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S609-S610
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is evidence that the concentrations of the main inhibitory neurotransmitter (GABA) may be altered in schizophrenia. The purpose of this study is to find the changes in the GABA concentration in the area of anterior and posterior cingulate cortex of patients with early-stage schizophrenia using the spectral-edited magnetic resonance spectroscopy.
ObjectivesTo measure the cerebral concentrations of the gamma-aminobutyric acid in schizophrenia patients at early stage.
MethodsThirty-one subject, 18 controls (11m+7f, 29.6±5.7 y.o.) and 13 schizophrenia patients (F20.0, 8m+5f, 27.5±3.1 y.o.). Philips Achieva dStream 3T MRI scanner, standard head coil. The 3D T1w head images and MEGA-PRESS GABA spectra in ACC and PCC areas were acquired with the following parameters: 50x25x25 mm, TR = 2 s, TE = 64 ms, 180-editing pulses applied at 1.9 ppm and 7.6 ppm, NSA = 288 (acq.time ~10 min). GABA spectra were processed in Gannet program. The intensities of the GABA, Glutamate+glutamine (Glx), creatine (Cr) and unsuppressed water signals were acquired. T-test was used in search for between-group differences.
ResultsIn ACC region, significant reduction of the GABA/Water was observed (by ~15%, p=0.02) as well as a trend to a decrease in GABA/Cr (by ~10%, p=0.07) in schizophrenia. In PCC, no significant GABA/Water or GABA/Cr differences were observed. Glx/Water and Glx/Cr in both areas were also unchanged.
Image:
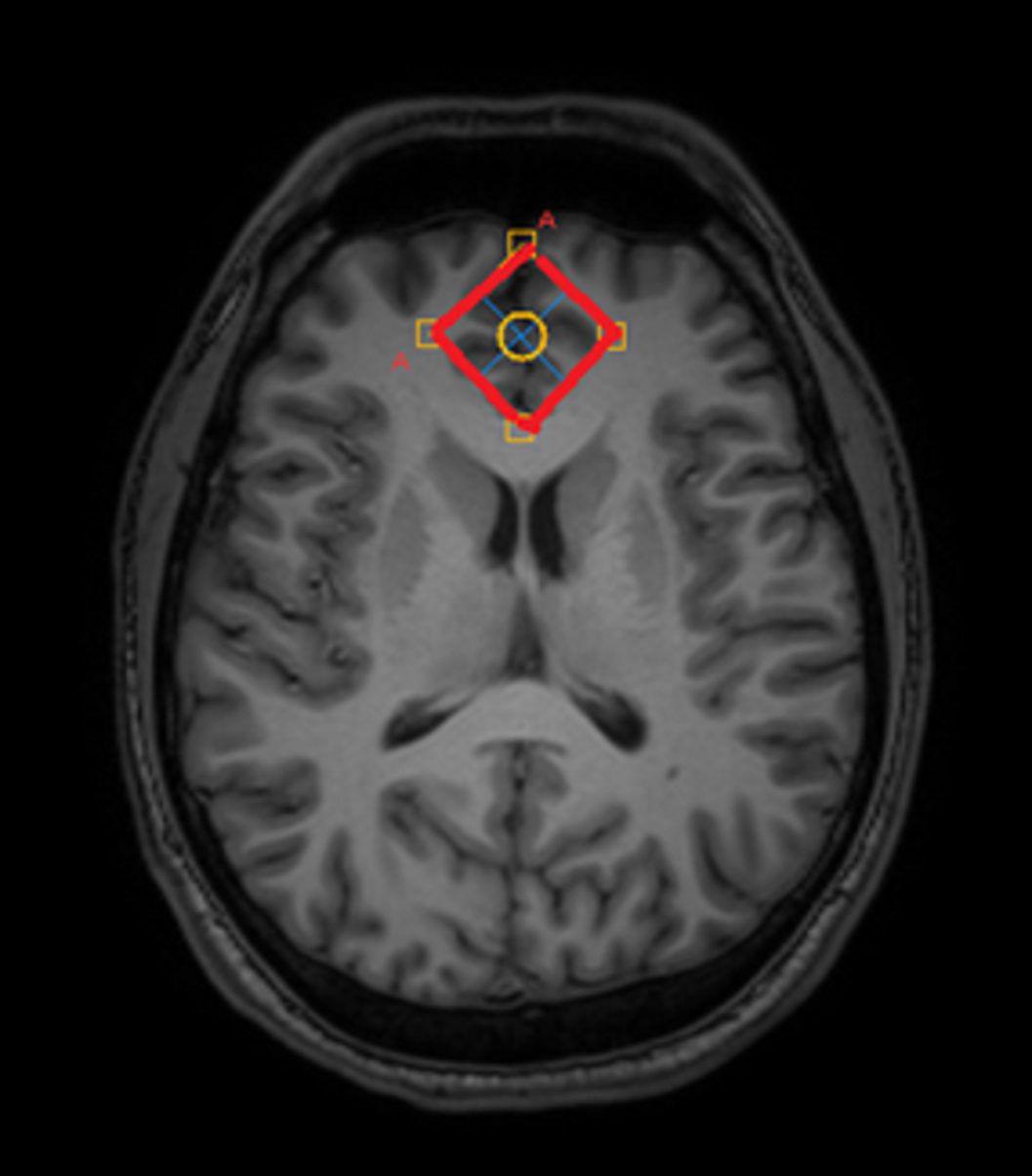
Image 2:
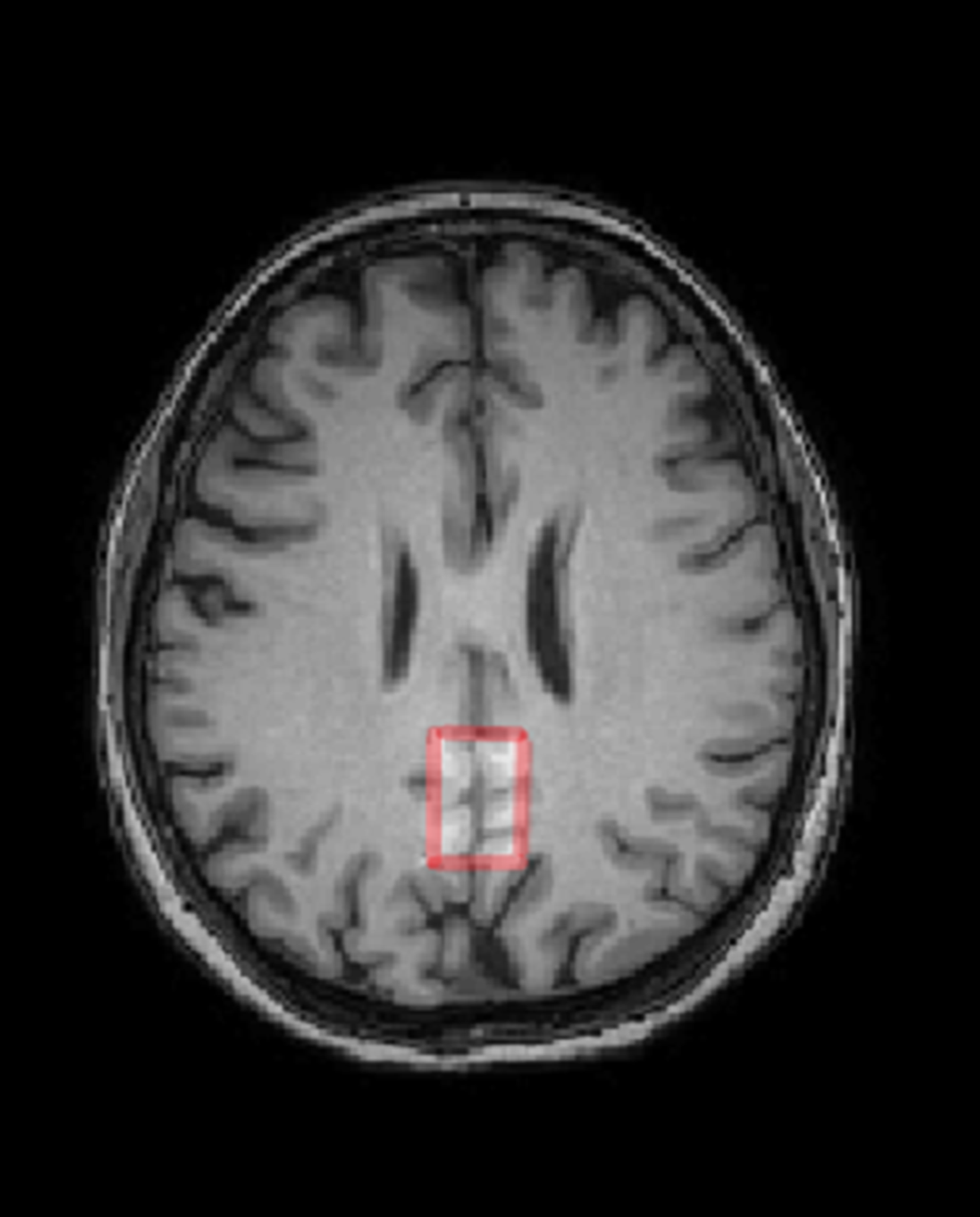 Conclusions
ConclusionsThis study provides insight into neurotransmitter alterations at early-stage schizophrenia. The results demonstrate the region-specific changes in the balance of the main neurotransmitters. Since this balance is crucial for the normal cerebral functioning, the results may facilitate better understanding of the dynamics of the pathological process and provide additional information for understanding the biological mechanisms of the schizophrenia development.
Disclosure of InterestNone Declared
Alterations in brain myelination at early-stage schizophrenia detected by macromolecular proton fraction MRI
- E. Krupina, A. Manzhurtsev, M. Ublinskiy, O. Bozhko, G. Mamedova, V. Ushakov, N. Zakharova, V. Yarnykh, D. Andreyuk, M. Shlyapnikov, G. Kostyuk, T. Akhadov
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S134-S135
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is evidence that cerebral myelination is impaired in schizophrenia. The purpose of this study is to find the myelin content changes in the brain structures of patients with early-stage schizophrenia using the macromolecular proton fraction (MPF) method, and also to evaluate the differences in the myelination of these structures.
ObjectivesTo measure MPF in the brain structures of schizophrenia patients
MethodsForty-five subjects, 22 controls (10m+12f, 31.6±9.7 y.o.) and 23 schizophrenia patients (F20.0, 11m+12f, 31.5±5.1 y.o.). Philips Achieva dStream 3T MRI scanner, standard head coil. The magnetization transfer (TR=20 ms, TE=4.60 ms, FA=10°), T1-weighted (TR=20 ms, TE=4.60 ms, FA=20°) and PD-weighted (TR=20 ms, TE=4.60 ms, FA=4°) were acquired. The MPF maps were reconstructed using home-made software. In FSL, non-brain structures were removed and MPF maps were registered to a standard MNI152 1 mm atlas. Harvard Oxford Cortical and Subcortical atlases were used to select areas of interest. T-test was used in search for between-group differences.
ResultsA 3% decrease in myelination in schizophrenia was observed in whole cerebral cortex p = 0.03) and cerebral white matter (p=0.02). Trends to cortical demyelination were found: paracingular cortex (p=0.06), anterior (p=0.1) and posterior cingulate cortex (p=0.07). No myelination disorders were detected in the cerebellum.
Image:
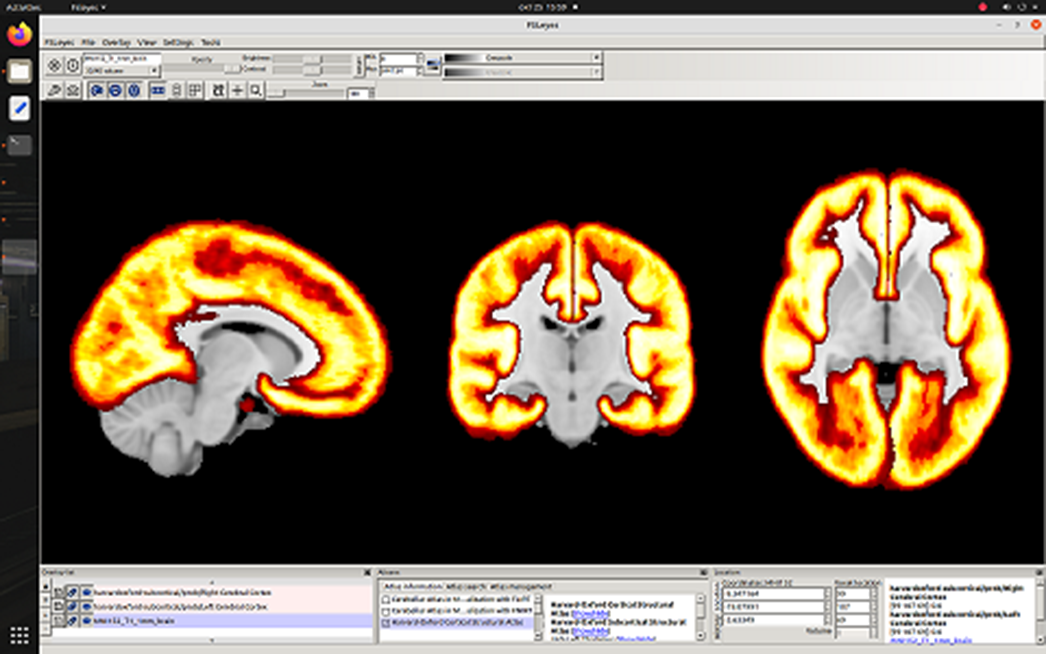
Image 2:
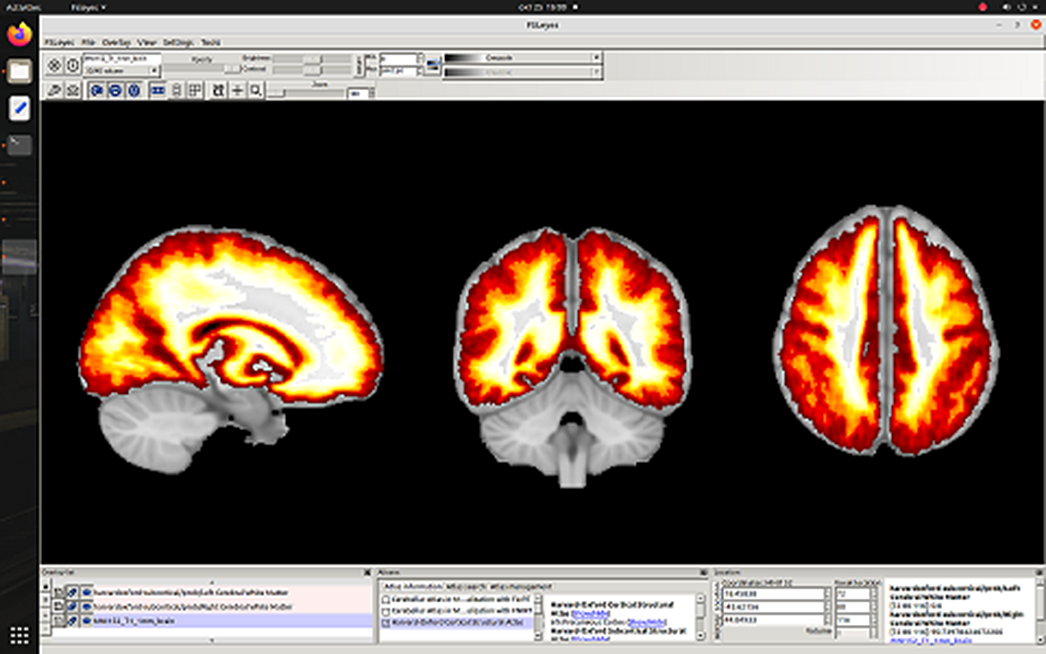
Image 3:
 Conclusions
ConclusionsTo our knowledge, the absence of cerebellar myelination disorders in patients at an early-stage schizophrenia is reported for the first time, while the observed decrease in cerebrum myelination in schizophrenia is consistent with the previous findings. The difference in myelination between cerebellum and cerebrum may help to characterize the dynamics of the pathological process and provide additional information for understanding the biological mechanisms of the development of schizophrenia.
Grant RSF 20-15-00299 (partially).
Disclosure of InterestNone Declared








