312 results
Molecular detection of Histoplasma capsulatum in organ samples from bats randomly captured in urban areas of Araraquara, São Paulo state, Brazil
- Jessica A. Ruiz-Muñoz, Gabriela Rodríguez-Arellanes, José A. Ramírez, Laura E. Carreto-Binaghi, Ana M. Fusco-Almeida, Maria J. S. Mendes-Giannini, Blanca E. García-Pérez, Maria L. Taylor
-
- Journal:
- Epidemiology & Infection / Volume 152 / 2024
- Published online by Cambridge University Press:
- 06 May 2024, e83
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The mycosis histoplasmosis is also considered a zoonosis that affects humans and other mammalian species worldwide. Among the wild mammals predisposed to be infected with the etiologic agent of histoplasmosis, bats are relevant because they are reservoir of Histoplasma species, and they play a fundamental role in maintaining and spreading fungal propagules in the environments since the infective mycelial phase of Histoplasma grows in their accumulated guano. In this study, we detected the fungal presence in organ samples of bats randomly captured in urban areas of Araraquara City, São Paulo, Brazil. Fungal detection was performed using a nested polymerase chain reaction to amplify a molecular marker (Hcp100) unique to H. capsulatum, which revealed the pathogen presence in organ samples from 15 out of 37 captured bats, indicating 40.5% of infection. Out of 22 Hcp100-amplicons generated, 41% corresponded to lung and trachea samples and 59% to spleen, liver, and kidney samples. Data from these last three organs suggest that bats develop disseminated infections. Considering that infected bats create environments with a high risk of infection, it is important to register the percentage of infected bats living in urban areas to avoid risks of infection to humans, domestic animals, and wildlife.
Nematocide activity of 6,7-diarylpteridines in three experimental models
- C. Ochoa, M. Rodríguez, L. Domínguez, J. Saldaña, R. Di Maio, P. Alonso-Villalobos, M.M. Martínez Grueiro
-
- Journal:
- Journal of Helminthology / Volume 73 / Issue 4 / April 1999
- Published online by Cambridge University Press:
- 11 April 2024, pp. 333-336
-
- Article
- Export citation
-
The in vitro nematocide activity of seventeen 6,7-diarylpteridines has been tested using three different experimental models, Caenorhabditis elegans, Nippostrongylus brasiliensis and Heligmosomoides polygyrus. The method of evaluation of inhibition in the secretion of acetylcholinesterase by H. polygyrus seems to be the most indicated to avoid false positives. The in vivo activities, against Trichinella spiralis, of the most in vitro active pteridines have been assayed. All pteridine derivatives bearing 6,7-di-p-bromophenyl substituents have shown in vitronematocide activites in the three experimental models used. Amongst all the pteridines tested in vivo, only 2,4-pteridinedithione derivatives exhibited moderate activity.
Pyrophyllite Determination in Mineral Mixtures
- J. L. Pérez Rodríguez, C. Maqueda, A. Justo
-
- Journal:
- Clays and Clay Minerals / Volume 33 / Issue 6 / December 1985
- Published online by Cambridge University Press:
- 02 April 2024, pp. 563-566
-
- Article
- Export citation
Application of Inverse Gas Chromatography to the Study of the Surface Properties of Slates
- M. A. Rodriguez, J. Rubio, F. Rubio, M. J. Liso, J. L. Oteo
-
- Journal:
- Clays and Clay Minerals / Volume 45 / Issue 5 / October 1997
- Published online by Cambridge University Press:
- 28 February 2024, pp. 670-680
-
- Article
- Export citation
-
Inverse gas chromatography (IGC) at zero surface coverage was used for determining the surface characteristics of a slate sample. Previously this sample had been characterized by means of X-ray diffraction (XRD), chemical analysis, infrared (IR) spectroscopy and nitrogen adsorption. Quartz, muscovite and chlorite were the minerals foming the slate. A well-defined mesoporous structure with pores of 15 Å of interlayer distance was observed. Chemical analysis and IR spectroscopy corroborated the X-ray results. The surface characteristics of the slate were defined in relation to nonspecific and specific interactions with organic molecules. In accordance with the nonspecific interactions, the London component (γSD) of the surface free energy gave an estimation of the surface energy of the slate sample. The obtained values for γSD were 140.0, 124.8, 108.2 and 96.8 mN m-1 at 100, 110, 120 and 130 °C, respectively. These values were characteristic of an inorganic sample of high surface energy. The values of the thermodynamic variables—differential heat of adsorption, free energy and entropy of adsorption—were in accordance with these results. At the same time, specific interactions were characterized by the ηπ parameter and the acid-base (KA, KB) indices. The positive value of ηπ (0.09 kJ mol-1) indicated the presence of Lewis acidic sites on the slate surface. The value of KA (acid index) of 1.17 was higher than the value of KB (base index) of 0.37; this result confirmed the acidic nature of the studied slate's surface.
Interaction of Vermiculite with Aliphatic Amides (Formamide, Acetamide and Propionamide): Formation and Study of Interstratified Phases in the Transformation of Mg- to NH4-Vermiculite
- Antonio Ruiz-Conde, Antonio Ruiz-Amil, Jose L. Perez-Rodriguez, Pedro J. Sanchez-Soto, Francisco Aragon de la Cruz
-
- Journal:
- Clays and Clay Minerals / Volume 45 / Issue 3 / June 1997
- Published online by Cambridge University Press:
- 28 February 2024, pp. 311-326
-
- Article
- Export citation
-
The Mg-vermiculite from Santa Olalla has been treated with aliphatic amides—formamide (FM), acetamide (AM) and propionamide (PM)—in aqueous solution. These treatments produce the transformation towards NH4-vermiculite and interstratified NH4-vermiculite-Mg-vermiculite phases. The NH4-vermiculite, Mg-vermiculite and interstratified (mixed-layer) phases have been identified from basal X-ray diffraction (XRD) interval peaks between 10.3 Å and 14.4 Å, and confirmed by direct Fourier transform method, as well as by atomic absorption spectrometry (AAS), infrared (IR) spectroscopy and thermal analysis.
According to their NH4-vermiculite/Mg-vermiculite probability coefficients ratio (PA/PB), and PAA, these interstratified phases can be divided into 3 categories: 1) If the PA/PB ratio is ≥ 7/3 and PAA ≥ 0.7, there are interstratified phases with a strong tendency toward segregation (case of FM, AM and PM). 2) If the PA/PB ratio is between 5/5 and 6/4, with PAA in the range 0.45–0.6, there are nearly regular alternating and random interstratified phases (case of AM and PM). 3) If the PA/PB ratio is ≤ 5/5 and PAA ≤ 0.45, there are interstratified phases with a strong tendency toward alternation (case of PM).
Experimental evidence reported in the present work indicates that the mechanism of interaction of Mg-vermiculite with FM, AM and PM in an aqueous medium takes place by ion exchange of NH4 between the layers. The hydrolysis of these aliphatic amides leads to the liberation of NH4+ into the medium. It has been found that the NH4+ sorption depends on the physico-chemical characteristics of the particular aliphatic amide, and the transformation of Mg-vermiculite to interstratified and/or NH4-vermiculite phases depends on the amide concentration. These treatments allow one to control the formation of interstratified and NH4-vermiculite phases.
Naturally-Occurring Silicates as Carriers for Copper Catalysts used in Methanol Conversion
- M. R. Sun Kou, S. Mendioroz, J. L. G. Fierro, I. Rodriguez-Ramos, J. M. Palacios, A. Guerrero-Ruiz, A. M. De Andres
-
- Journal:
- Clays and Clay Minerals / Volume 40 / Issue 2 / April 1992
- Published online by Cambridge University Press:
- 28 February 2024, pp. 167-174
-
- Article
- Export citation
-
Bentonite- and sepiolite-supported copper catalysts have been prepared either by adsorption of Cu(II) from aqueous solutions of copper nitrate at pH ~4.5 or by adsorption of a [Cu(NH3)4]2+ complex from an ammonia solution of CuSO4 at pH ~9.5. The structure and composition of the calcined preparations have been studied by X-ray diffraction, chemical analysis, and energy dispersive X-rays. Textural characteristics have derived from the analysis of the adsorption-desorption isotherms of N2. All catalysts have been tested for the dehydrogenation of methanol to methyl formate. For this reaction, bentonite-based catalysts were found to have very little activity, which indicates that copper located in the inter-lamellar spaces is inaccessible to methanol molecules. On the contrary, copper-sepiolite catalysts showed a very high specific activity even for those catalysts with a very low copper content. The chemical state of copper in the catalysts on-stream has been revealed by X-ray photoelectron spectroscopy and X-ray-induced Auger techniques. In most of the catalysts Cu+ is the dominant copper species.
TRANVIA: A program for continuum mental health assistance in transition period
- L. Pérez Gómez, A. González Álvarez, M. A. Reyes Cortina, E. Lanza Quintana, N. Álvarez Alvargonzález, C. Rodríguez Turiel, E. Lago Machado, J. J. Martínez Jambrina
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S728
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Transition between adolescence and adulthood represents the most important challenge for personal development and involves several transformations: physical, psychological and social. It is a complex age bracket, concurring the transition from youth psychiatric units to adult ones, with an increased risk for the appearance of mental disorders and risky behaviours. TRANVIA program, developed in Avilés, provides psychiatric assistance to patients between 15 and 25 years old, diagnosed with a severe psychiatric disorder or with an increased risk of having one.
ObjectivesOur objectives are: ensuring clinical continuity assistance, promoting communication among professionals and the empowerment of our patients to improve their functionality and quality of life.
MethodsDescriptive study including patients involved in TRANVIA program from November 2019 to November 2021.
ResultsDuring this two-years period there have been 44 referrals to the program, 11 of them were rejected for failure to comply with diagnostic criteria. In November 2021 there were 33 patients included in the TRANVIA program with an average age of 17 years old (range: 15-22). 70% of them were men and 30% women. All of them had psychiatric assistance from different sources: youth mental health units, neuropediatrics… About 75% of the patients were diagnosed with autistic spectrum disorder and approximately three-quarters of the sample needed pharmacological treatment. Risperidone was the most prescribed drug. We have also developed other assistance alternatives as home-based care, relaxation sessions, social worker interventions and coordination with schools.
ConclusionsTRANVIA program has allowed us to provide continual attention to vulnerable patients that shift from youth psychiatric units to adult ones. Patients that meet inclusion criteria were enrolled independently the type of assistance they have previously received. Accessibility and flexibility were our priority. During the described period there was only one dropout, three patients required psychiatric hospitalization and two others visited the emergency department. There have been no cases of completed suicide.
Disclosure of InterestNone Declared
Non-convulsive epiletic seizure after electroconvulsive therapy session
- L. Llovera García, L. Veiga Gil, L. Lopez Unzue, A. Corrales Rodriguez, A. Ballesteros Prados, J. Yoldi Murillo, J. M. Lopez Ilundain
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1021-S1022
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Electroconvulsive therapy (ECT) is a procedure performed under general anaesthesia involving triggering an intentional brief seizure through small electrical currents through the brain. The anaesthetic depth should be adequate prior to shock and measured with BIS, a processed electroencephalogram (EEG) monitor. Adjusting the hypnotic dose allows to decrease the ictal threshold and thus improve the response to treatment and decrease side effects.
ObjectivesOur goal is detecting elements such as spontaneous epileptiform activity after ECT without tonic-clonic activity with the spectral density matrix (SDM).
MethodsOur patient: an 87-year-old woman, diagnosed with F20.2 catatonic schizophrenia and under antipsychotic treatment since her youth. She has required multiple hospital admissions due to psychopathological decompensations until starting monthly maintenance ECT sessions in 2014. Since then she no new hospital admissions have been required.
ResultsImages 1D and 1E shows the SDM, a spectrogram of the EEG. The X axis show time (minutes), the Y axis shows the frequency (Hz) and the Z axis shows the energy or intensity of that electrical activity in the frequency bands replaced by colors: warm colors (red) reflecting high intensity electroencephalographic activity and cool colors (yellow, blue and green), low activity. Images 2 and 3’s EDM shows spontaneous epileptiform activity after electroconvulsive therapy without tonic-clonic activity. We observed an initial EDM of an awake patient, with warm colours in practically all frequency bands, including the beta band (13-30 Hz), characteristic of waking states. Around 9:50 anaesthetic induction occurs, activity increases in slow frequencies (red colours in alpha, theta and delta), plus an increase of cold colours in beta, reflecting the disappearance of brain activity in that frequency. The asterisk reflects the EEG response to the electrical discharge, followed by a postcritical state with brain activity exclusively in slow waves and high amplitude (delta and some theta) and absence of activity in other frequencies (blue colour in the beta and alpha bands) around 9:57. At about 10:00 there is an abrupt appearance of high intensity brain activity (warm colours) in beta and alpha and delta, mainly, reflecting spontaneous epileptiform activity after treatment and clinically reflected as a patient absent and disconnected from the environment, but without tonic-clonic activity. New postcritical state in which blue colour predominates, reflecting little brain activity, and warmer colours reappear in all frequency bands, including beta, reflecting the progressive recovery of wakefulness.
Image:
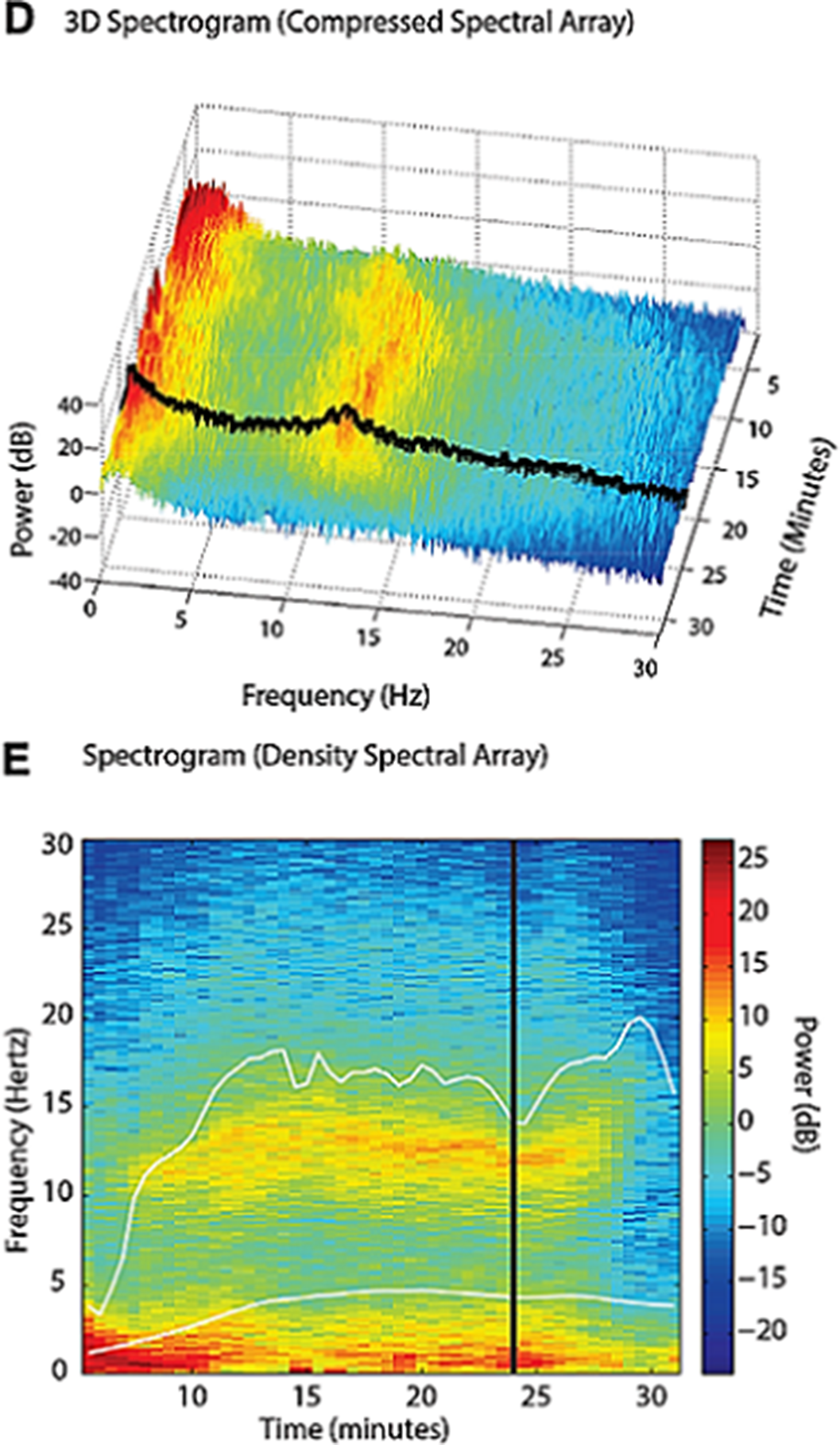
Image 2:
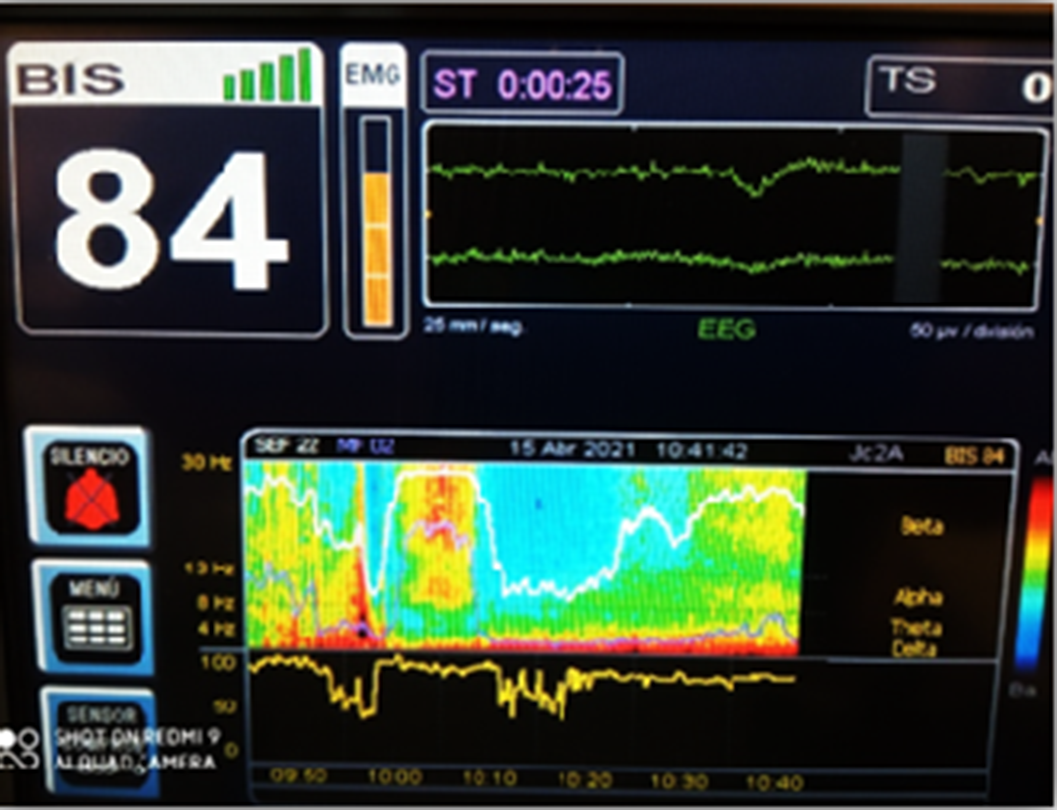
Image 3:
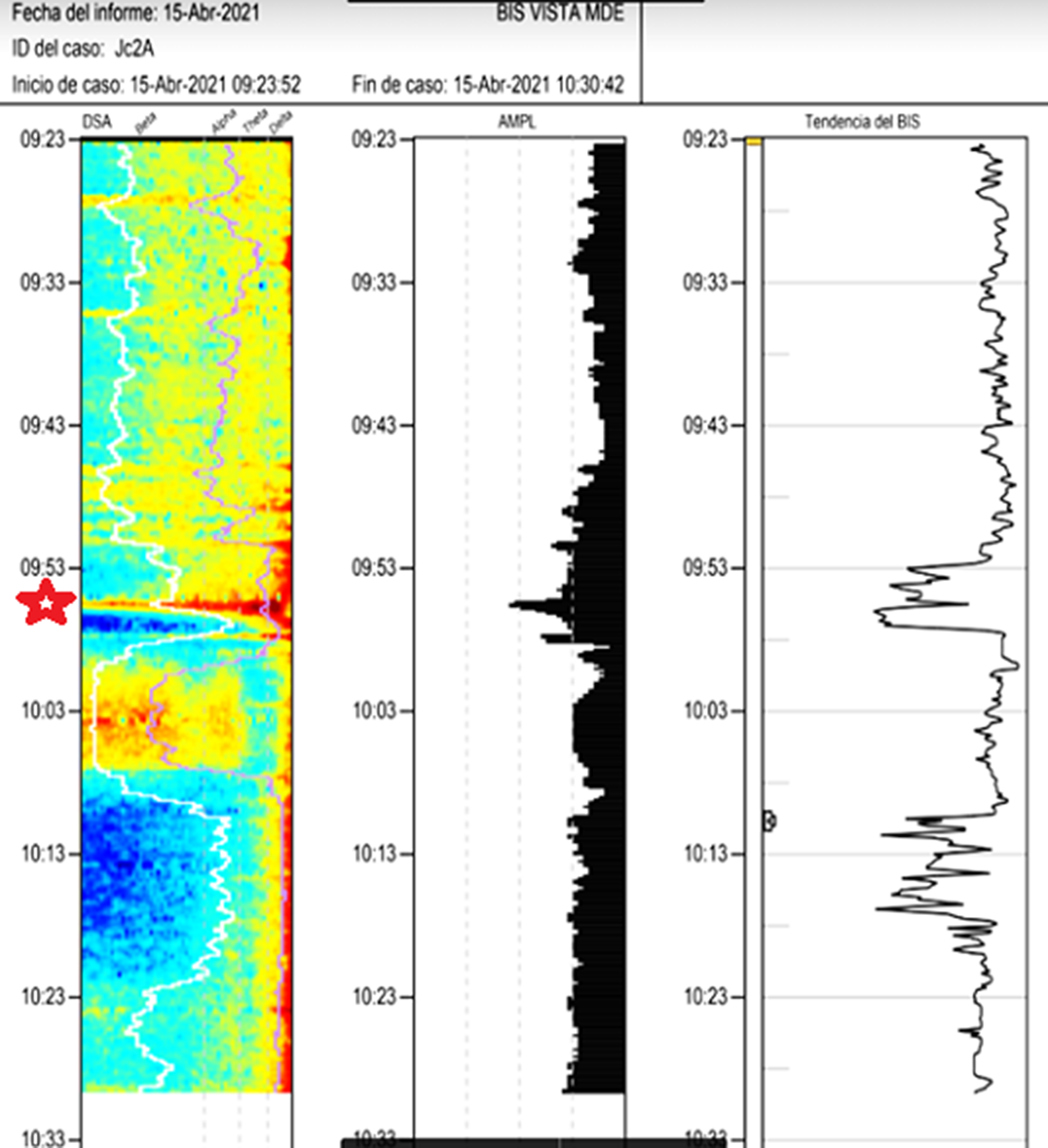 Conclusions
ConclusionsPsychiatric pathology can be reflected in the SDM, which allows to observe changes in the EEG, correcting the electrical stimulus of the shock and the dose of anesthetic appropriate to the patient to trigger an intentional brief seizure under general anesthesia.
Disclosure of InterestNone Declared
Clinical experience with clozapine in patients with severe intellectual disability and behavioral disorders.
- N. Laherrán Cantera, R. Palacios-Garrán, L. Jiménez Suarez, C. Rodriguez Martín, J. Machuca Sicilia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S149
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It is estimated that the prevalence of severe Intellectual Disability (ID) is 6 per 1,000 people. ID is sometimes the cause of Behavioral Disorders (BD) with aggressive and impulsive behaviors that make family and social life difficult. However, despite its high prevalence, the number of studies on it is very scarce.
When BD appears, it should be evaluated if there is a physical or psychiatric cause that causes it and assess non-pharmacological treatments. If they are insufficient, treatments such as risperidone are used to manage BD. When these are ineffective, the use of drugs with greater difficulties in their effects and clinical management, such as clozapine, is required.
ObjectivesThe objective is to describe the use of clozapine in patients with severe ID associated with BD.
MethodsRetrospective descriptive study. Patients older than 18 years with severe ID and BD, treated with clozapine for at least two years were included. Those with medical or psychiatric comorbidity were excluded.
ResultsThe sample consisted of 12 patients, 16.67% women (n=2) and 83.33% men (n=10), aged 47.57±9.27 years. Prior to the introduction of clozapine, a mean of 2.67±1.21 antipsychotics had been tested. The mean dose of clozapine was 264.24±70.50 mg/day. The patients had received treatment for 51.57±25.67 months, following the usual controls. None had hematological adverse effects or other serious adverse effects.
ConclusionsClozapine can be an effective and safe therapeutic alternative in the treatment of BD in intellectual disabled patients which do not respond to other treatments. The clinical benefits of clozapine treatment seem to outweigh the potential risks associated with the treatment. However, more studies are needed to evaluate the effects of clozapine in patients with intellectual disabilities.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
Phenomenology, clinical aspects and therapeutic implications of delusional memories in Delusional Disorders: A Systematic Review
- A. González- Rodríguez, J. A. Monreal, M. Solmi, M. Balestrieri, M. Fornaro, A.-L. Panfil, F. Duval, M. V. Seeman
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S373
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Delusional memories or retrospective delusions have been extensively reported in subjects during or after intensive care stays. In major psychoses, authors have classically observed delusional memories impacting the prognosis and mental well-being.
ObjectivesOur aim was to review the phenomenology, psychological/biological factors contributing to delusional memories in delusional disorder (DD), and potential treatment strategies.
MethodsSystematic review using PubMed, Scopus, SciELO and Web of Science electronic databases (inception-September 2022). Search terms: (“delusional memories” OR “retrospective delusions”) AND (“Schizophrenia, Paranoid”) [MeSH]. Studies were included if they reported psychopathology, clinical characteristics or treatment strategies of “delusional memories” in DD. Team members: AGR, JAM, MS, MB, MF, ACP, FD, MVS.
ResultsA total of 786 records were retrieved, including six studies. Psychogenesis:A novel cognitive neuropsychological research model (based on hypnosis) in erotomania delusions suggest a potential recall and reinterpretation of delusions beliefs in highly hypnotizable subjects. Biological basis: Frontal lobe (or executive) dysfunction does not seem to contribute to delusional memories in De Clérambault syndrome (erotomania). Phenomenology: 1)General knowledge was essentially intact, while the perceptual characteristics of delusional memories were stronger than real memories. 2)Correlations were found between delusional ideation, positive dimension of schizotypy (r=0.18), and false memories (r=0.27). 3)Jumping-to-conclusions and liberal acceptance bias influence delusional memories. Treatment:Efficacy of 1)Cognitive Behavioural Therapy (CBT) (significant reduction delusions), and 2)Metacognitive control over false memories.
ConclusionsThis is the first review exploring the genesis and management of delusional memories in DD. Memory deficits/executive dysfunctions do not seem to be the only cause of this phenomenon.
Disclosure of InterestNone Declared
The role of thyroid function on the occurrence and psychopathological exacerbation of delusional disorders: Two case studies and review of recent works.
- A. Guàrdia, A. González-Rodríguez, L. Lafuente, M. Natividad, E. Izquierdo, E. Roman, J. A. Monreal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1047
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Primary hypothyroidism has been extensively associated with the presence of depressive symptoms in major depressive and bipolar disorders; however, the association between psychosis and hypothyroidism has received less attention.
ObjectivesWe aimed to present two cases of patients with delusional disorder (DD) and hypothyroidism and review studies focused on this association.
Methods(1)Two case studies of DD patients. (2)Narrative review on the association of hypothyroidism and psychosis by using PubMed database (2000-August 2022). Search terms: [Hypothyroidism AND (psychosis or delusional disorder)].
ResultsTwo case-studies. Case A: 58 year-old woman with DD who presented a worsening of psychotic symptoms in association with the occurrence of newly diagnosed hypothyroidism. Risperidone 1mg daily was initiated. A combination of levothyroxine 100 mcg/day and paroxetine 20mg/day was started. Case B: 51 year-old DD women with remission of delusional symptoms, who presented occurrence of depressive symptoms and panic attacks with agoraphobia. Olanzapine 5 mg/day and venlafaxine 225 mg/day were started combined with levothyroxine 75 mcg/day.
Review: From a total of 159 records, 52 studies described an association between psychosis and hypothyroidism. Most of the studies are focused on the Myxedema madness, treatment of psychosis with comorbid hypothyroidism, and the role of thyroid function on emerging psychoses. Others: intellectual disability, epilepsy, psychosis, asthma, diabetes and heart failure. Genetic associations of Xq13 gene, encoding for nuclear receptors of thyroid receptors, with psychosis.
ConclusionsMany questions pertaining to DD and thyroid function remain unanswered. Treatment of hormonal comorbidities may be associated with a clinical improvement of psychotic symptoms.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
Two-year experience of the implementation of a psychiatric home hospitalization care service for acute mental illness
- A. Guàrdia, L. Marin, A. González-Rodríguez, V. Bañon, E. Izquierdo, L. Lafuente, X. Martinez-Bio, D. Llors, M. Natividad, L. Ros, J. A. Monreal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S169
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychiatric home hospitalisation is a service aiming to support people with mental illnesses in their acute stage at their own home. This care model has been recently implemented in our territory with the main objective of avoiding hospital admissions.
ObjectivesOur goal is to describe a cohort of patients followed up over 2-years in the context of a pilot mental health program within a community-based model (Mutua Terrassa University Hospital).
MethodsWe conducted a prospective longitudinal study including 125 patients attended from 01/11/2020 to 09/11/2022 in our reference area of 250,000 inhabitants. The team was formed by 1 psychiatrist and 1 mental health nurse. DSM-5 diagnoses, socio-demographic variables, mean stay and care trajectories were collected.
ResultsOne-hundred twenty-five patients were attended (women: 70). Mean age at consultation: 38.3 years-old. Mean stay: 24 days. The most frequent diagnoses: non-affective psychotic disorders (58%), affective disorders (30%), followed by anxiety and personality disorders. Referrals from Community Mental Health Outpatient Services (CMHS) (72%), Acute Inpatient Unit (25%), and Psychiatric Emergency Service (3%). Referrals after discharge: CMHS (83%), Adult Acute Inpatient Unit (13%), others (4%). Individualized mental health plans were carried out in all cases, in coordination with community mental health services. Follow-up adherence after discharge was about 95%. Patients with first-episode of psychosis showed the highest degree of satisfaction (N=46).
ConclusionsPatients with emerging psychosis were the profile of users who showed the highest benefit of our service. Women showed higher adherence, and loss to follow-up was lower than we expected.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
“Keeping an eye on amylase”. Side effects of antidepressants
- T. Jiménez Aparicio, G. Medina Ojeda, A. Rodríguez Campos, L. Rodríguez Andrés, C. Vallecillo Adame, C. De Andrés Lobo, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. J. Mateos Sexmero, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M. P. Pando Fernández, P. Martínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Both in consultations with the general practitioner and with the psychiatrist, antidepressants are one of the most used drugs (1). These have multiple indications, and there are different groups according to their mechanism of action. In relation to this case, we are going to talk about Venlafaxine, a dual-type antidepressant, that is, it inhibits the reuptake of serotonin and norepinephrine. One of the most common side effects is digestive discomfort, which usually resolves after a few weeks (2). However, we should not ignore these symptoms, since they can hide something more serious.
ObjectivesPresentation of a clinical case on a patient who presented an increase in pancreatic amylase after starting treatment with Venlafaxine.
MethodsBibliographic review including the latest articles in Pubmed on side effects of antidepressant treatment, and more specifically at the gastrointestinal level (in this case we will talk about pancreatitis).
ResultsWe present the case of a 49-year-old woman, who was hospitalized 2 years ago, due to a first depressive episode. During this admission, psychopharmacological treatment was started for the first time, on that occasion with a selective serotonin reuptake inhibitor (SSRI), treatment of first choice (3). The patient had no side effects at that time, but the response was very modest, so it was decided to replace that antidepressant with Venlafaxine (with dual action), up to 150mg. The depressive symptoms improved markedly, however the patient began to feel digestive discomfort (which at first did not seem to be of great importance). A general analysis was performed, in which an increase in lipase (978 U/L) and amylase (528 U/L) was detected. An echoendoscopy, an abdominal scan, and a magnetic resonance cholangiography were performed; Pancreatitis secondary to drugs was suspected (a severe condition). Luckily, no significant lesions were found in the tests, and the levels of amylase and lipase decreased when Venlafaxine treatment was withdrawn (without reaching the normal range). The patient was discharged and continued to attend consultations. In the last control, amylase had dropped to 225 U/L. His abdominal pain disappeared. Treatment with Vortioxetine (a multimodal antidepressant) was started, however the amylase levels continue to be monitored, and the patient continues to see the gastroenterologist.
ConclusionsGastrointestinal side effects are very common when taking antidepressant treatment, and in most cases they do not usually represent a serious problem.
However, it is described in the scientific literature that in some cases, acute pancreatitis secondary to some drugs, including Venlafaxine, can occur (4). In order to detect it, it is necessary to perform a blood test and sometimes also other complementary tests.
For its treatment, the fundamental thing is to withdraw the causing drug, trying to find other alternatives, and carry out a control to monitor possible complications
Disclosure of InterestNone Declared







