10 results
Evaluating indwelling devices and other risk factors for mortality in invasive Carbapenem-resistant Enterobacterales infections in Georgia, 2012–2019
- Lucy S. Witt, Mary Elizabeth Sexton, Gillian Smith, Monica Farley, Jesse T. Jacob
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 02 January 2024, e254
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Carbapenem-resistant Enterobacterales (CRE) infections are a public health threat due to the risk of transmission between patients and high associated mortality. We sought to identify risk factors for mortality in patients with invasive CRE infections and to specifically evaluate whether there was an association between indwelling medical devices and 90-day mortality.
Design:Retrospective observational cohort study of patients infected with CRE in the eight-county metropolitan Atlanta area between 2012 and 2019.
Methods:Patients with invasive CRE infections were identified via the Georgia Emerging Infections Program’s active, population- and laboratory-based surveillance system and linked with the Georgia Vital Statistics database. We used bivariate analysis to identify risk factors for mortality and completed log binomial multivariable regression to estimate risk ratios (RR) for the association between indwelling devices and mortality.
Results:In total, 154 invasive CRE infections were identified, with indwelling devices present in most patients (87.7%) around the time of infection. Admission to an intensive care unit was found to be associated with 90-day mortality (adjusted RR [aRR] 1.55, 95% CI 1.07, 2.24); however, the presence of any indwelling device was not associated with increased risk of 90-day mortality in multivariable analysis (aRR 1.22, 95% CI 0.55, 2.73). Having at least two indwelling devices was associated with increased mortality (aRR 1.79, 95% CI 1.05, 3.05).
Conclusions:Indwelling devices were prevalent in our cohort but were not consistently associated with an increased risk of mortality. Further studies are needed to examine this relationship and the role of device removal.
20 Examining the Recovery Course of Pediatric Concussion Patients with Protracted Recovery Referred to a Specialty Concussion Clinic
- Abel S. Mathew, Alison Datoc, Scott O. Burkhart, August M. Price, Christine Ellis, Jacob Sexton, John P. Abt
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 896-897
-
- Article
-
- You have access Access
- Export citation
-
Objective:
The purpose of this study was to explore overall recovery time and post-concussive symptoms (PCSS) of pediatric concussion patients who were referred to a specialty concussion clinic after enduring a protracted recovery (>28 days). This included patients who self-deferred care or received management from another provider until recovery became complicated. It was hypothesized that protracted recovery patients, who initiated care within a specialty concussion clinic, would have similar recovery outcomes as typical acute injury concussion patients (i.e., within 3 weeks).
Participants and Methods:Retrospective data were gathered from electronic medical records of concussion patients aged 6-19 years. Demographic data were examined based on age, gender, race, concussion history, and comorbid psychiatric diagnosis. Concussion injury data included days from injury to initial clinic visit, total visits, PCSS scores, days from injury to recovery, and days from initiating care with a specialty clinic to recovery. All participants were provided standard return-to-learn and return-to-play protocols, aerobic exercise recommendations, behavioral health recommendations, personalized vestibular/ocular motor rehabilitation exercises, and psychoeducation on the expected recovery trajectory of concussion.
Results:52 patients were included in this exploratory analysis (Mean age 14.6, SD ±2.7; 57.7% female; 55.7% White, 21.2% Black or African American, 21.2% Hispanic). Two percent of our sample did not disclose their race or ethnicity. Prior concussion history was present in 36.5% of patients and 23.1% had a comorbid psychiatric diagnosis. The patient referral distribution included emergency departments (36%), local pediatricians (26%), neurologists (10%), other concussion clinics (4%), and self-referrals (24%).
Given the nature of our specialty concussion clinic sample, the data was not normally distributed and more likely to be skewed by outliers. As such, the median value and interquartile range were used to describe the results. Regarding recovery variables, the median days to clinic from initial injury was 50.0 (IQR=33.5-75.5) days, the median PCSS score at initial visit was 26.0 (IQR=10.0-53.0), and the median overall recovery time was 81.0 (IQR=57.0-143.3) days.
After initiating care within our specialty concussion clinic, the median recovery time was 21.0 (IQR=14.0-58.0) additional days, the median total visits were 2.0 (IQR=2.0-3.0), and the median PCSS score at follow-up visit was 7.0 (IQR=1-17.3).
Conclusions:Research has shown that early referral to specialty concussion clinics may reduce recovery time and the risk of protracted recovery. Our results extend these findings to suggest that patients with protracted recovery returned to baseline similarly to those with an acute concussion injury after initiating specialty clinic care. This may be due to the vast number of resources within specialty concussion clinics including tailored return-to-learn and return-to-play protocols, rehabilitation recommendations consistent with research, and home exercises that supplement recovery. Future studies should compare outcomes of protracted recovery patients receiving care from a specialty concussion clinic against those who sought other forms of treatment. Further, evaluating the influence of comorbid factors (e.g., psychiatric and/or concussion history) on pediatric concussion recovery trajectories may be useful for future research.
Carbapenemase genes and mortality in patients with carbapenem-resistant Enterobacterales, Atlanta, Georgia, 2011–2020
- Lucy Witt, Ahmed Babike, Gillian Smith, Sarah Satola, Mary Elizabeth Sexton, Jesse Jacob
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s12-s13
-
- Article
-
- You have access Access
- Open access
- Export citation
-
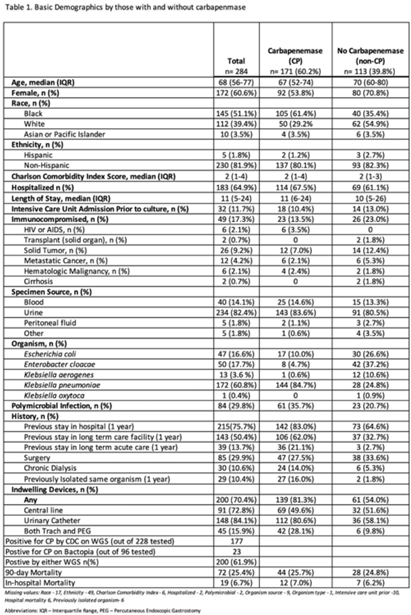
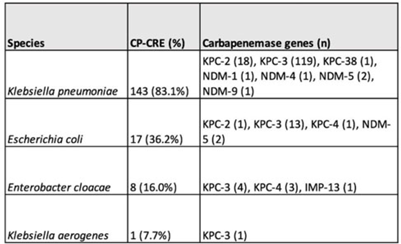
Background: Carbapenemase genes in carbapenem-resistant Enterobacterales (CP-CRE) may be transmitted between patients and bacteria. Reported rates of carbapenemase genes vary widely, and it is unclear whether having a carbapenemase gene portends worse outcomes given that all patients with CRE infections have limited treatment options. Methods: Using active population- and laboratory-based active surveillance data collected by the US CDC-funded Georgia Emerging Infections Program from 2011 to 2020, we assessed the frequency of carbapenemase genes in a convenience sample of CRE isolates using whole-genome sequencing (WGS), and we investigated risk factors for carbapenemase positivity. Only the first isolate per patient in a 30-day period was included. We compared characteristics of patients with CP-CRE and non–CP-CRE. Using multivariable log binomial regression, we assessed the association of carbapenemase gene positivity and 90-day mortality. Results: Of 284 CRE isolates, 171 isolates (60.2%) possessed a carbapenemase gene (Table 1), and KPC-3 was the most common carbapenemase gene (80.7%), with only 7 isolates possessing NDM (Table 2). No isolates possessed >1 carbapenemase gene, and most isolates were from urine (82.4%) (Table 1). Carbapenemase gene positivity was associated with lower age, male sex, black race, infection with Klebsiella pneumoniae, polymicrobial infection, having an indwelling medical device, receiving chronic dialysis, and prior stay in a long-term acute-care hospital, long-term care facility, and/or prior hospitalization in the last year. The 90-day mortality rates were similar in patients with non–CP-CRE and CP-CRE: 24.8% versus 25.7% (P = .86). In multivariable analysis, carbapenemase gene presence was not associated with 90-day mortality (adjusted risk ratio, 0.82; 95% CI, 0.50–1.35) when adjusting for CCI, infection with Klebsiella pneumoniae, and chronic dialysis use. Conclusions: The frequency of CP-CRE among CRE was high in this study, but unlike prior studies, the 90-day mortality rates wer similar in patients with CP-CRE compared to non–CP-CRE. Our results provide novel associations (eg, lower age, male sex, infection with Klebsiella pneumoniae, and indwelling medical devices) that infection preventionists could use to target high-risk patients for screening or isolation prior to CP-CRE detection.
Disclosure: None
Do hospitalists who prescribe high (risk-adjusted) rates of antibiotics do so repeatedly?
- Udodirim Onwubiko, Christina Mehta, Zanthia Wiley, Jesse Jacob, Ashley Jones, Shabir Hassan, Marybeth Sexton, Sujit Suchindran, Scott Fridkin
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
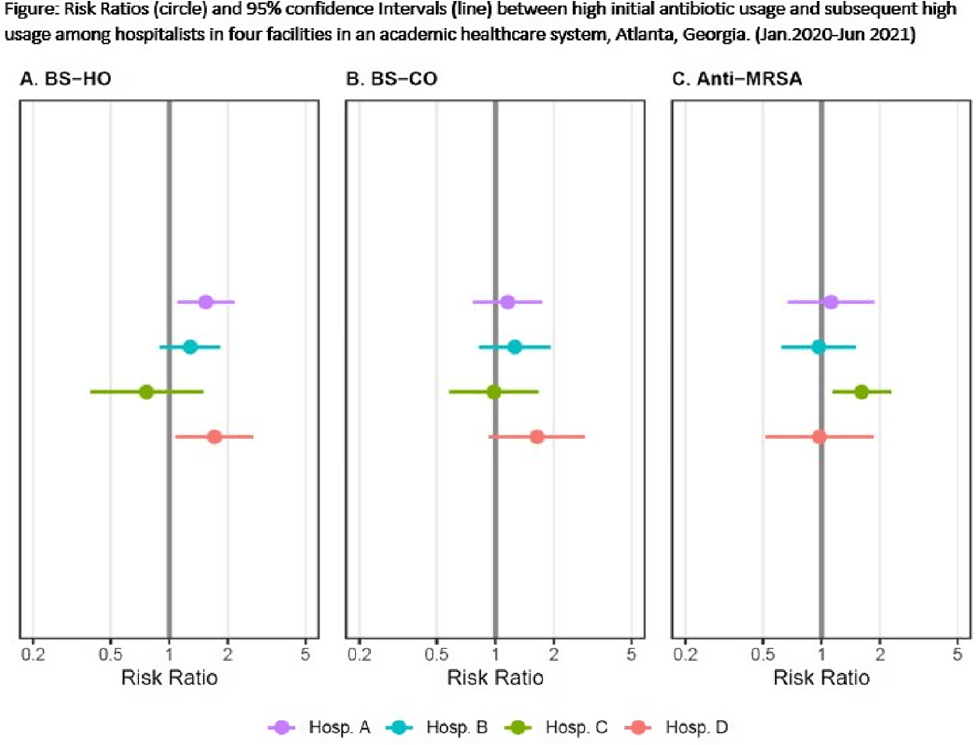
Background: Provider-specific prescribing metrics can be used for benchmarking and feedback to reduce unnecessary antibiotic use; however, metrics must be credible. To improve credibility of a recently described risk-adjusted antibiotic prescribing metric for hospital medicine service (HMS) providers, we assessed whether providers who initially prescribed excess antibiotics continued to prescribe antibiotics excessively. Methods: We linked administration and billing data among patients at 4 acute-care hospitals (1,571 beds) to calculate days of therapy (DOT) ordered by individual hospitalists for each of 3 NHSN antibiotic groupings: broad-spectrum hospital onset (BS-HO), broad-spectrum community-onset (BS-CO), or anti-MRSA for each patient day billed from January 2020 to June 2021. To incorporate repeated measures by provider, mixed models adjusted for patient-mix characteristics (eg, % encounters with urinary tract infection, etc) were used to calculate serial, bimonthly, provider-specific, observed-to-expected ratios (OERs). An OER of 1.25 indicates that the prescribing rate observed was 25% higher than predicted, adjusting for patient mix. We then used log binomial generalized estimating equations to assess whether a high prescribing rate (defined as an OER ≥ 1.25) for an individual provider in an earlier bimonthly period was associated with a persistent high rate for that provider in the following period. Results: Overall, 975 bimonthly periods were evaluated from 136 hospitalists. Most (58%) contributed data the entire 18-month study period. Median OERs were similar between hospitals: 0.94 (IQR, 0.65–1.28) for BS-HO antibiotic use, 0.99 (IQR, 0.73–1.24) for BS-CO antibiotic use, and 0.95 (IQR, 0.65–1.28) for anti-MRSA antibiotic use. At the individual prescriber level, roughly one-quarter of bimonthly OERs (range varied by group and hospital from 21% to 31%) were categorized as high. At 3 of the 4 hospitals, a provider with a high OER for either BS-HO or BS-CO antibiotic use in any bimonthly period was more likely to have a high OER in the subsequent period (Fig. 1). These observed risk ratios were statistically significant for BS-HO antibiotic use at only 2 hospitals: hospital A risk ratio (RR) was 1.54 (95% CI, 1.10–2.16); hospital B RR was 1.28 (95% CI, 0.90–1.82); hospital C RR was 0.76 (95% CI, 0.39–1.48); and ospital D RR was 1.71 (95% CI, 1.09–2.68). Conclusions: Our findings suggest that hospitalists with a higher than expected 2-month period of antibiotic prescribing are likely to continue to have elevated prescribing rates in the following period, particularly for BS-HO antibiotics. These findings increase the credibility of using a 2-month prescribing metric for BS-HO antibiotic stewardship efforts; further work is needed to evaluate utility for other antibiotic groupings.
Funding: None
Disclosures: None
Reductions in inpatient fluoroquinolone use and postdischarge Clostridioides difficile infection (CDI) from a systemwide antimicrobial stewardship intervention
- Part of
- K. Ashley Jones, Udodirim N. Onwubiko, Julianne Kubes, Benjamin Albrecht, Kristen Paciullo, Jessica Howard-Anderson, Sujit Suchindran, Ronald Trible, Jesse T. Jacob, Sarah H. Yi, Dana Goodenough, Scott K. Fridkin, Mary Elizabeth Sexton, Zanthia Wiley
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 22 October 2021, e32
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To determine the impact of an inpatient stewardship intervention targeting fluoroquinolone use on inpatient and postdischarge Clostridioides difficile infection (CDI).
Design:We used an interrupted time series study design to evaluate the rate of hospital-onset CDI (HO-CDI), postdischarge CDI (PD-CDI) within 12 weeks, and inpatient fluoroquinolone use from 2 years prior to 1 year after a stewardship intervention.
Setting:An academic healthcare system with 4 hospitals.
Patients:All inpatients hospitalized between January 2017 and September 2020, excluding those discharged from locations caring for oncology, bone marrow transplant, or solid-organ transplant patients.
Intervention:Introduction of electronic order sets designed to reduce inpatient fluoroquinolone prescribing.
Results:Among 163,117 admissions, there were 683 cases of HO-CDI and 1,104 cases of PD-CDI. In the context of a 2% month-to-month decline starting in the preintervention period (P < .01), we observed a reduction in fluoroquinolone days of therapy per 1,000 patient days of 21% after the intervention (level change, P < .05). HO-CDI rates were stable throughout the study period. In contrast, we also detected a change in the trend of PD-CDI rates from a stable monthly rate in the preintervention period to a monthly decrease of 2.5% in the postintervention period (P < .01).
Conclusions:Our systemwide intervention reduced inpatient fluoroquinolone use immediately, but not HO-CDI. However, a downward trend in PD-CDI occurred. Relying on outcome measures limited to the inpatient setting may not reflect the full impact of inpatient stewardship efforts.
Reductions in Postdischarge Clostridioides difficile Infection after an Inpatient Health System Fluoroquinolone Stewardship
- K. Ashley Jones, Zanthia Wiley, Julianne Kubes, Mary Elizabeth Sexton, Benjamin Albrecht, Jesse Jacob, Jessica Howard-Anderson, Scott Fridkin, Udodirim Onwubiko
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s4
-
- Article
-
- You have access Access
- Open access
- Export citation
-
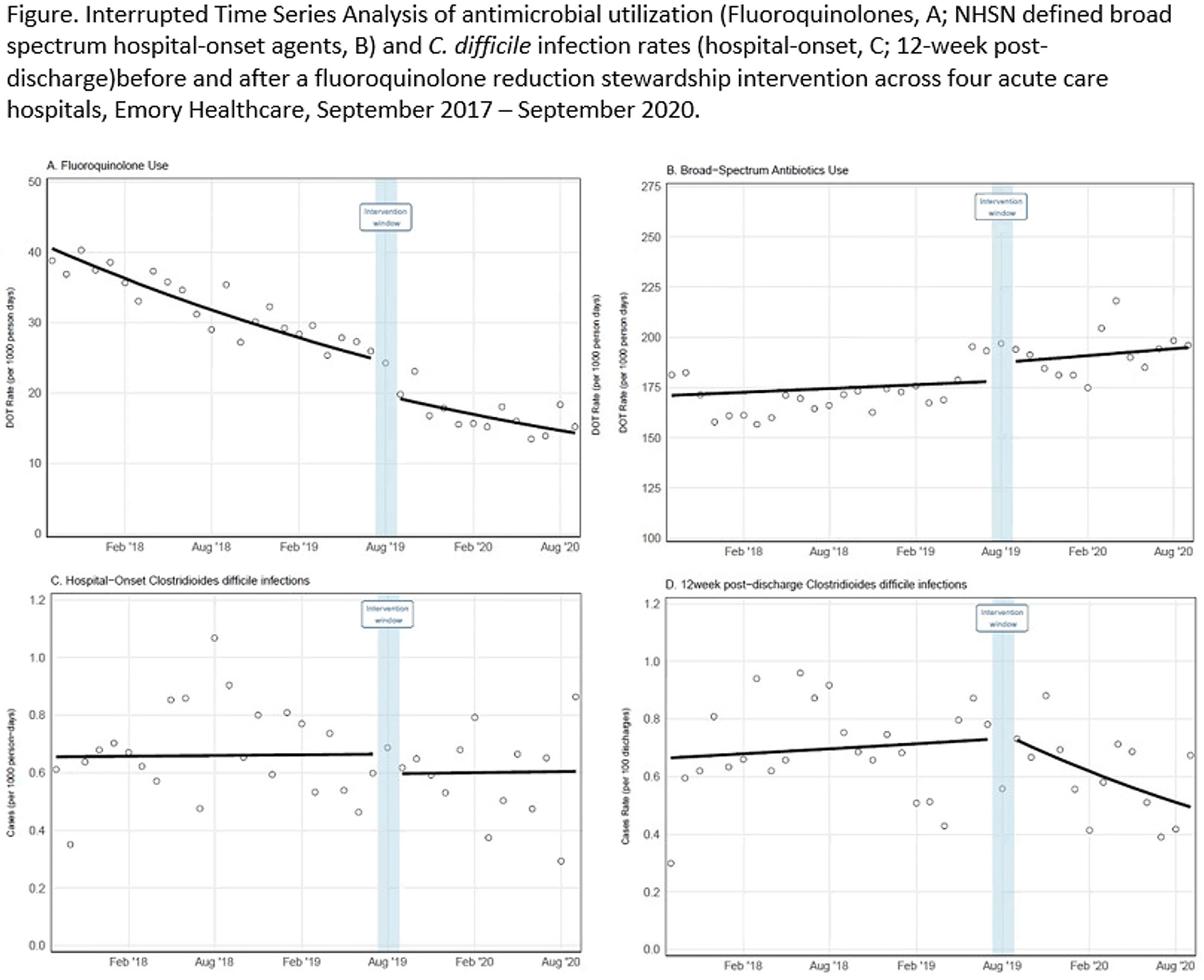
Background: Effective inpatient stewardship initiatives can improve antibiotic prescribing, but impact on outcomes like Clostridioides difficile infections (CDIs) is less apparent. However, the effect of inpatient stewardship efforts may extend to the postdischarge setting. We evaluated whether an intervention targeting inpatient fluoroquinolone (FQ) use in a large healthcare system reduced incidence of postdischarge CDI. Methods: In August 2019, 4 acute-care hospitals in a large healthcare system replaced standalone FQ orders with order sets containing decision support. Order sets redirected prescribers to syndrome order sets that prioritize alternative antibiotics. Monthly patient days (PDs) and antibiotic days of therapy (DOT) administered for FQs and NHSN-defined broad-spectrum hospital-onset (BS-HO) antibiotics were calculated using patient encounter data for the 23 months before and 13 months after the intervention (COVID-19 admissions in the previous 7 months). We evaluated hospital-onset CDI (HO-CDI) per 1,000 PD (defined as any positive test after hospital day 3) and 12-week postdischarge (PDC- CDI) per 100 discharges (any positive test within healthcare system <12 weeks after discharge). Interrupted time-series analysis using generalized estimating equation models with negative binomial link function was conducted; a sensitivity analysis with Medicare case-mix index (CMI) adjustment was also performed to control for differences after start of the COVID-19 pandemic. Results: Among 163,117 admissions, there were 683 HO-CDIs and 1,009 PDC-CDIs. Overall, FQ DOT per 1,000 PD decreased by 21% immediately after the intervention (level change; P < .05) and decreased at a consistent rate throughout the entire study period (−2% per month; P < .01) (Fig. 1). There was a nonsignificant 5% increase in BS-HO antibiotic use immediately after intervention and a continued increase in use after the intervention (0.3% per month; P = .37). HO-CDI rates were stable throughout the study period, with a nonsignificant level change decrease of 10% after the intervention. In contrast, there was a reversal in the trend in PDC-CDI rates from a 0.4% per month increase in the preintervention period to a 3% per month decrease in the postintervention period (P < .01). Sensitivity analysis with adjustment for facility-specific CMI produced similar results but with wider confidence intervals, as did an analysis with a distinct COVID-19 time point. Conclusion: Our systemwide intervention using order sets with decision support reduced inpatient FQ use by 21%. The intervention did not significantly reduce HO-CDI but significantly decreased the incidence of CDI within 12 weeks after discharge. Relying on outcome measures limited to inpatient setting may not reflect the full impact of inpatient stewardship efforts and incorporating postdischarge outcomes, such as CDI, should increasingly be considered.
Funding: No
Disclosures: None
Figure 1.
Carbapenem-resistant Enterobacterales bacteriuria and subsequent bacteremia: A population-based study
- Jessica R. Howard-Anderson, Chris W. Bower, Gillian Smith, Mary Elizabeth Sexton, Monica M. Farley, Sarah W. Satola, Jesse T. Jacob
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 8 / August 2021
- Published online by Cambridge University Press:
- 10 December 2020, pp. 962-967
- Print publication:
- August 2021
-
- Article
- Export citation
-
Objective:
To describe the epidemiology of carbapenem-resistant Enterobacterales (CRE) bacteriuria and to determine whether urinary catheters increase the risk of subsequent CRE bacteremia.
Design:Using active population- and laboratory-based surveillance we described a cohort of patients with incident CRE bacteriuria and identified risk factors for developing CRE bacteremia within 1 year.
Setting:The study was conducted among the 8 counties of Georgia Health District 3 (HD3) in Atlanta, Georgia.
Patients:Residents of HD3 with CRE first identified in urine between 2012 and 2017.
Results:We identified 464 patients with CRE bacteriuria (mean yearly incidence, 1.96 cases per 100,000 population). Of 425 with chart review, most had a urinary catheter (56%), and many resided in long-term care facilities (48%), had a Charlson comorbidity index >3 (38%) or a decubitus ulcer (37%). 21 patients (5%) developed CRE bacteremia with the same organism within 1 year. Risk factors for subsequent bacteremia included presence of a urinary catheter (odds ratio [OR], 8.0; 95% confidence interval [CI], 1.8–34.9), central venous catheter (OR, 4.3; 95% CI, 1.7–10.6) or another indwelling device (OR, 4.3; 95% CI, 1.6–11.4), urine culture obtained as an inpatient (OR, 5.7; 95% CI, 1.3–25.9), and being in the ICU in the week prior to urine culture (OR, 2.9; 95% CI, 1.1–7.8). In a multivariable analysis, urinary catheter increased the risk of CRE bacteremia (OR, 5.3; 95% CI, 1.2–23.6).
Conclusions:In patients with CRE bacteriuria, urinary catheters increase the risk of CRE bacteremia. Future interventions should aim to reduce inappropriate insertion and early removal of urinary catheters.
Variation in Hospitalist-Specific Antibiotic Prescribing at Four Hospitals: A Novel Tool for Antibiotic Stewardship
- Julianne Kubes, Jesse Jacob, Scott Fridkin, Raymund Dantes, K. Ashley Jones, Sujit Suchindran, Mary Elizabeth Sexton, Zanthia Wiley
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s56-s57
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Hospitalists play a critical role in antimicrobial stewardship as the primary antibiotic prescriber for many inpatients. We sought to describe antibiotic prescribing variation among hospitalists within a healthcare system. Methods: We created a novel metric of hospitalist-specific antibiotic prescribing by linking hospitalist billing data to hospital medication administration records in 4 hospitals (two 500-bed academic (AMC1 and AMC2), one 400-bed community (CH1), and one 100-bed community (CH2)) from January 2016 to December 2018. We attributed dates that a hospitalist electronically billed for a given patient as billed patient days (bPD) and mapped an antibiotic day of therapy (DOT) to a bPD. Each DOT was classified according to National Healthcare Safety Network antibiotic categories: broad-spectrum hospital-onset (BS-HO), broad-spectrum community-onset (BS-CO), anti-MRSA, and highest risk for Clostridioides difficile infection (CDI). DOT and bPD were pooled to calculate hospitalist-specific DOT per 1,000 bPD. Best subsets regression was performed to assess model fit and generate hospital and antibiotic category-specific models adjusting for patient-level factors (eg, age ≥65, ICD-10 codes for comorbidities and infections). The models were used to calculate predicted hospitalist-specific DOT and observed-to-expected ratios (O:E) for each antibiotic category. Kruskal-Wallis tests and pairwise Wilcoxon rank-sum tests were used to determine significant differences between median DOT per 1,000 bPD and O:E between hospitals for each antibiotic category. Results: During the study period, 116 hospitalists across 4 hospitals contributed a total of 437,303 bPD. Median DOT per 1,000 bPD varied between hospitals (BS-HO range, 46.7–84.2; BS-CO range, 63.3–100; anti-MRSA range, 48.4–65.4; CDI range, 82.0–129.4). CH2 had a significantly higher median DOT per 1,000 bPD compared to the academic hospitals (all antibiotic categories P < .001) and CH1 (BS-HO, P = .01; anti-MRSA, P = .02) (Fig. 1A). The 4 antibiotic groups at 4 hospitals resulted in 16 models, with good model fit for CH2 (R2 > 0.55 for all models), modest model fit for AMC2 (R2 = 0.46–0.55), fair model fit for CH1 (R2 = 0.19–0.35), and poor model fit for AMC1 (R2 < 0.12 for all models). Variation in hospitalist-specific O:E was moderate (IQR, 0.9–1.1). AMC1 showed greater variation than other hospitals, but we detected no significant differences in median O:E between hospitals (all antibiotic categories P > .10) (Fig. 1B). Conclusions: Adjusting for patient-level factors significantly reduced much of the variation in hospitalist-specific DOT per 1,000 bPD in some but not all hospitals, suggesting that unmeasured factors may drive antibiotic prescribing. This metric may represent a target for stewardship intervention, such as hospitalist-specific feedback of antibiotic prescribing practices.
Funding: None
Disclosures: Scott Fridkin, consulting fee - vaccine industry (various) (spouse)
The impact of an electronic medical record nudge on reducing testing for hospital-onset Clostridioides difficile infection
- Jessica R. Howard-Anderson, Mary Elizabeth Sexton, Chad Robichaux, Zanthia Wiley, Jay B. Varkey, Sujit Suchindran, Benjamin Albrecht, K. Ashley Jones, Scott K. Fridkin, Jesse T. Jacob
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 4 / April 2020
- Published online by Cambridge University Press:
- 10 February 2020, pp. 411-417
- Print publication:
- April 2020
-
- Article
- Export citation
-
Objective:
To determine the effect of an electronic medical record (EMR) nudge at reducing total and inappropriate orders testing for hospital-onset Clostridioides difficile infection (HO-CDI).
Design:An interrupted time series analysis of HO-CDI orders 2 years before and 2 years after the implementation of an EMR intervention designed to reduce inappropriate HO-CDI testing. Orders for C. difficile testing were considered inappropriate if the patient had received a laxative or stool softener in the previous 24 hours.
Setting:Four hospitals in an academic healthcare network.
Patients:All patients with a C. difficile order after hospital day 3.
Intervention:Orders for C. difficile testing in patients administered a laxative or stool softener in <24 hours triggered an EMR alert defaulting to cancellation of the order (“nudge”).
Results:Of the 17,694 HO-CDI orders, 7% were inappropriate (8% prentervention vs 6% postintervention; P < .001). Monthly HO-CDI orders decreased by 21% postintervention (level-change rate ratio [RR], 0.79; 95% confidence interval [CI], 0.73–0.86), and the rate continued to decrease (postintervention trend change RR, 0.99; 95% CI, 0.98–1.00). The intervention was not associated with a level change in inappropriate HO-CDI orders (RR, 0.80; 95% CI, 0.61–1.05), but the postintervention inappropriate order rate decreased over time (RR, 0.95; 95% CI, 0.93–0.97).
Conclusion:An EMR nudge to minimize inappropriate ordering for C. difficile was effective at reducing HO-CDI orders, and likely contributed to decreasing the inappropriate HO-CDI order rate after the intervention.
3167 Evaluation of risk factors for progression from carbapenem-resistant Enterobacteriaceae bacteriuria to an invasive infection
- Jessica Howard-Anderson, Rebekah Blakney, Christopher Bower, Mary Elizabeth Sexton, Sarah W. Satola, Monica M. Farley, Jesse T. Jacob
-
- Journal:
- Journal of Clinical and Translational Science / Volume 3 / Issue s1 / March 2019
- Published online by Cambridge University Press:
- 26 March 2019, pp. 43-44
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: To describe the epidemiology of patients with carbapenem-resistant Enterobacteriaceae (CRE) bacteriuria in metropolitan Atlanta, GA and to identify risk factors associated with progression to an invasive CRE infection. We hypothesize that having an indwelling urinary catheter increases the risk of progression. METHODS/STUDY POPULATION: The Georgia Emerging Infections Program (EIP) performs active population- and laboratory-based surveillance to identify CRE isolated from a sterile site (e.g. blood) or urine among patients who reside in the 8-county metropolitan Atlanta area (population ~4 million). The Georgia EIP performs a chart review of each case to extract data on demographics, culture location, resistance patterns, healthcare exposures, and other underlying risk factors. We used a retrospective cohort study design to include all Georgia EIP cases with Escherichia coli, Klebsiella pneumoniae, Klebsiella oxytoca, Enterobacter cloacae, or Klebsiella (formerly Enterobacter) aerogenes, adapting the current EIP definition of resistance to only include isolates resistant to meropenem, imipenem or doripenem (minimum inhibitory concentration ≥ 4) first identified in a urine culture from 8/1/2011 to 7/31/2017. Patients with CRE identified in a sterile site culture prior to a urine culture will be excluded. Within this cohort, we will identify which patients had a subsequent similar CRE isolate identified from a sterile site between one day and one year after the original urine culture was identified (termed “progression”). CRE isolates will be defined as similar if they are the same species and have the same carbapenem susceptibility pattern. Univariable analyses using T-tests or other nonparametric tests for continuous variables, and Chi-square tests (or Fisher’s exact tests as appropriate) for categorical variables will compare patient demographics, comorbidities and presence of invasive devices including urinary catheters between patients who had progression to an invasive infection and those who did not have progression. Covariates with a p-value of < 0.2 will be eligible for inclusion in the multivariable logistic regression model with progression to invasive infection as the primary outcome. All statistical analyses will be done in SAS 9.4. RESULTS/ANTICIPATED RESULTS: From 8/1/2011 to 7/31/2017 we have preliminarily identified 546 patients with CRE first identified in urine, representing an annual incidence rate of 1.1 cases per 100,000 population. Most cases were K. pneumoniae (352, 64%), followed by E. coli (117, 21%), E. cloacae (48, 9%), K. aerogenes (18, 3%), and K. oxytoca (11, 2%). The mean patient age was 64 +/− 18 years and the majority (308, 56%) were female. Clinical characterization through chart review was available for 507 patients. The majority of the patients were black (301, 59%), followed by white (166, 33%), Asian (12, 2%), and other or unknown race (28, 6%). 466 (92%) patients had at least one underlying comorbid condition with a median Charlson Comorbidity Index of 3 (IQR 1-5). 460 (91%) infections were considered healthcare-associated (366 community-onset and 94 hospital-onset), while 44 (9%) were community-associated. 279 (55%) patients had a urinary catheter within the two days prior to the CRE culture. The analysis of patients who progress to an invasive CRE infection, including the results of the univariable and multivariable analyses assessing risk factors for progression is in progress and will be reported in the future. DISCUSSION/SIGNIFICANCE OF IMPACT: In metropolitan Atlanta, the annual incidence of CRE first isolated in urine was estimated to be 1.1 cases per 100,000 population between 2011 and 2017, with the majority of the cases being K. pneumoniae. Most patients had prior healthcare exposure and more than 50% of the patients had a urinary catheter. Our anticipated results will identify risk factors associated with progression from CRE bacteriuria to an invasive infection with a specific focus on having a urinary catheter, as this is a potentially modifiable characteristic that could be a target of future interventions.







