7 results
In-depth assessment of critical access hospital stewardship program adherence to the CDC Core elements in Iowa and Nebraska
- Jonathan Ryder, Jeremy Tigh, Andrew Watkins, Jenna Preusker, Daniel Schroeder, Muhammad Salman Ashraf, Trevor Van Schooneveld
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s41
-
- Article
-
- You have access Access
- Open access
- Export citation
-
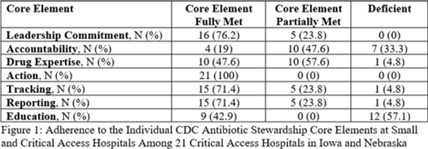
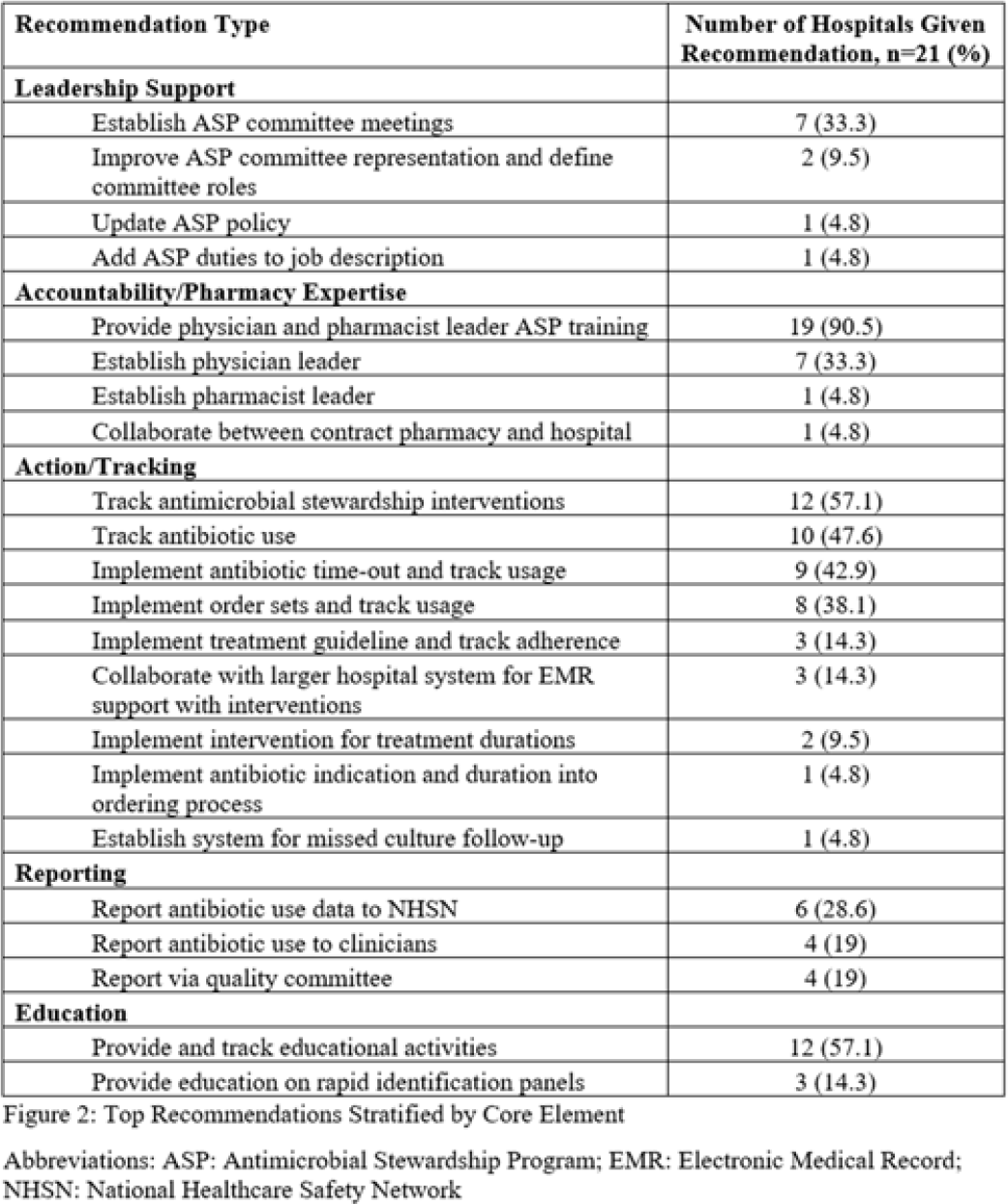
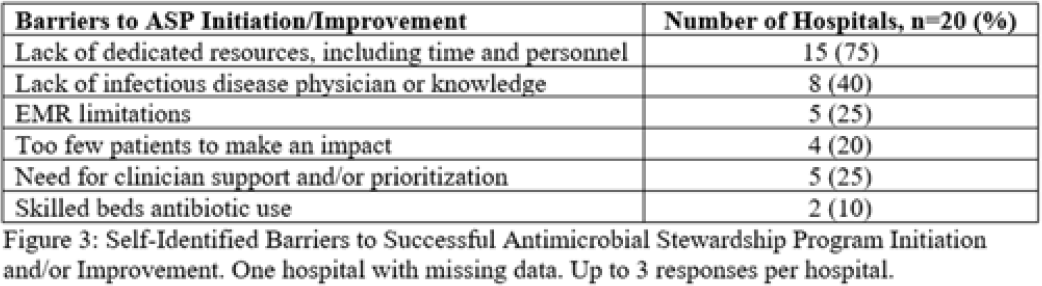
Background: Critical-access hospitals (CAHs) are required to meet the CDC 7 Core Elements of antimicrobial stewardship programs (ASPs). CAHs have lower adherence to the core elements than larger acute-care hospitals, and literature defining which core-element deficiencies exist within CAHs as well as barriers to adherence is lacking. Methods: We evaluated 21 CAH ASPs (5 in Nebraska and 15 in Iowa) that self-identified as potentially deficient in the Core Elements, via self-assessment followed by in-depth interviews with local ASP team members to assess adherence to the CDC Core Elements for ASPs. Core-element compliance was rated as either full (1 point), partial (0.5), or deficient (0), with a maximum score of 7 per ASP. High-priority recommendations to ensure core-element compliance were provided to facilities as written feedback. Self-reported barriers to implementation were thematically categorized. Results: Among the 21 CAH ASPs, none fully met all 7 core elements (range, 2.5–6.5), with a median of 5 full core elements met (Fig. 1). Only 6 ASPs (28.6%) had at least partial adherence to each of the 7 core elements. Action (21 of 21, 100%) and leadership commitment (16 of 21, 76.2%) were the core elements with the highest adherence, and accountability (4 of 21, 19%) and education (9 of 21, 42.9%) were the lowest. The most frequent high-priority recommendations were to provide physician and pharmacist leader ASP training (19 of 21, 90.5%), to track antimicrobial stewardship interventions (12 of 21, 57.1%), and to provide or track educational activities (12 of 21, 57.1%) (Fig. 2). One-third of programs were recommended to establish a physician leader. The most commonly self-identified barriers to establishing and maintaining an ASP were a lack of dedicated resources such as time of personnel (15 of 20, 75%), lack of infectious diseases expertise and training (8 of 20, 40%), and electronic medical record limitations (5 of 20, 25%) (Fig. 3). Conclusions: CAH ASPs demonstrate several critical gaps in achieving adherence to the CDC Core Elements, primarily in training for physician and pharmacist leaders and providing stewardship-focused education. Further resources and training customized to the issues present in CAH ASPs should be developed.
Disclosures: None
In-depth assessment of critical access hospital stewardship program adherence to the CDC Core Elements in Iowa and Nebraska
- Jonathan H. Ryder, Jenna Preusker, Andrew B. Watkins, Jeremy Tigh, Danny Schroeder, Muhammad Salman Ashraf, Trevor C. Van Schooneveld
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 03 August 2023, pp. 123-126
- Print publication:
- January 2024
-
- Article
- Export citation
-
In 21 antimicrobial stewardship programs in critical-access hospitals in Nebraska and Iowa that self-reported nonadherence to a CDC Core Element or Elements, in-depth program assessment and feedback revealed that accountability and education most needed improvement. Recommendations included providing physician and pharmacist training, tracking interventions, and providing education. Program barriers included lack of time and/or personnel and antimicrobial stewardship and/or infectious diseases expertise.
Disinfection of vascular catheter connectors that are protected by antiseptic caps is unnecessary
- Kelsey M. Fillman, Jonathan H. Ryder, Daniel M. Brailita, Mark E. Rupp, R. Jennifer Cavalieri, Paul D. Fey, Elizabeth R. Lyden, Richard J. Hankins
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 19 July 2023, pp. 35-39
- Print publication:
- January 2024
-
- Article
- Export citation
-
Objective:
Determination of whether vascular catheter disinfecting antiseptic-containing caps alone are effective at decreasing microbial colonization of connectors compared to antiseptic-containing caps plus a 5-second alcohol manual disinfection.
Setting:The study was conducted in a 718-bed, tertiary-care, academic hospital.
Patients:A convenience sample of adult patients across intensive care units and acute care wards with peripheral and central venous catheters covered with antiseptic-containing caps.
Methods:Quality improvement study completed over 5 days. The standard-of-care group consisted of catheter connectors with antiseptic-containing caps cleaned with a 5-second alcohol wipe scrub prior to culture. The comparison group consisted of catheter connectors with antiseptic-containing caps without a 5-second alcohol wipe scrub prior to culture. The connectors were pressed directly onto blood agar plates and incubated. Plates were assessed for growth after 48-72 hours.
Results:In total, 356 catheter connectors were cultured: 165 in the standard-of-care group, 165 in the comparison group, and 26 catheters connectors without an antiseptic-containing cap, which were designated as controls. Overall, 18 catheter connectors (5.06%) yielded microbial growth. Of the 18 connectors with microbial growth, 2 (1.21%) were from the comparison group, 1 (0.61%) was from the standard-of-care group, and 15 were controls without an antiseptic-containing cap.
Conclusions:Bacterial colonization rates were similar between the catheter connectors cultured with antiseptic-containing caps alone and catheter connectors with antiseptic-containing caps cultured after a 5-second scrub with alcohol. This finding suggests that the use of antiseptic-containing caps precludes the need for additional disinfection.
Nosocomial outbreak of SARS-CoV-2 delta variant among vaccinated healthcare workers and immunocompromised patients on a solid-organ transplant unit: Complexities of an epidemiologic and genomic investigation
- Jonathan H. Ryder, Trevor C. Van Schooneveld, Baha Abdalhamid, Macy G. Wood, Taylor A. Wahlig, Richard Starlin, Gayle Gillett, Teresa Balfour, Libby Pflueger, Mark E. Rupp
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 8 / August 2023
- Published online by Cambridge University Press:
- 09 September 2022, pp. 1355-1357
- Print publication:
- August 2023
-
- Article
- Export citation
-
In September 2021, a cluster of 6 patients with nosocomial coronavirus disease 2019 (COVID-19) were identified in a transplant unit. A visitor and 11 healthcare workers also tested positive for severe acute respiratory coronavirus virus 2 (SARS-CoV-2). Genomic sequencing identified 3 separate introductions of SARS-CoV-2 with related transmission among the identified patients and healthcare workers.
The interplay of infectious diseases consultation and antimicrobial stewardship in candidemia outcomes: A retrospective cohort study from 2016 to 2019
- Jonathan H. Ryder, Trevor C. Van Schooneveld, Elizabeth Lyden, Razan El Ramahi, Erica J. Stohs
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 7 / July 2023
- Published online by Cambridge University Press:
- 09 September 2022, pp. 1102-1107
- Print publication:
- July 2023
-
- Article
- Export citation
-
Objective:
To evaluate the need for mandatory infectious diseases consultation (IDC) for candidemia in the setting of antimicrobial stewardship guidance.
Design:Retrospective cohort study from January 2016 to December 2019.
Setting:Academic quaternary-care referral center.
Patients:All episodes of candidemia in adults (n = 92), excluding concurrent bacterial infection or death or hospice care within 48 hours.
Methods:Primary outcome was all-cause 30-day mortality. Secondary outcomes included guideline-adherence and treatment choice. Guideline-adherence was assessed with the EQUAL Candida score.
Results:Of 186 episodes of candidemia, 92 episodes in 88 patients were included. Central venous catheters (CVCs) were present in 66 episodes (71.7%) and were the most common infection source (N = 38, 41.3%). The most frequently isolated species was Candida glabrata (40 of 94, 42.6%). IDC was performed in 84 (91.3%) of 92 candidemia episodes. Mortality rates were 20.8% (16 of 77) in the IDC group versus 25% (2 of 8) in the no-IDC group (P = .67). Other comparisons were numerically different but not significant: repeat blood culture (98.8% vs 87.5%; P = .17), echocardiography (70.2% vs 50%; P = .26), CVC removal (91.7% vs 83.3%; P = .45), and initial echinocandin treatment (67.9% vs 50%; P = .44). IDC resulted in more ophthalmology examinations (67.9% vs 12.5%; P = .0035). All patients received antifungal therapy. Antimicrobial stewardship recommendations were performed in 19 episodes (20.7%). The median EQUAL Candida score with CVC was higher with IDC (16 vs 11; P = .001) but not in episodes without CVC (12 vs 11.5; P = .81).
Conclusions:In the setting of an active antimicrobial stewardship program and high consultation rates, mandatory IDC may not be warranted for candidemia.
Nosocomial outbreak of δ (delta) variant SARS-CoV-2 on a liver transplant unit: A complex epidemiologic and genomic investigation
- Jonathan Ryder, Trevor Van Schooneveld, Baha Abdalhamid, Macy Wood, Richard Starlin, Gayle Gillett, Teresa Balfour, Libby Pflueger, Mark Rupp
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s83-s84
-
- Article
-
- You have access Access
- Open access
- Export citation
-
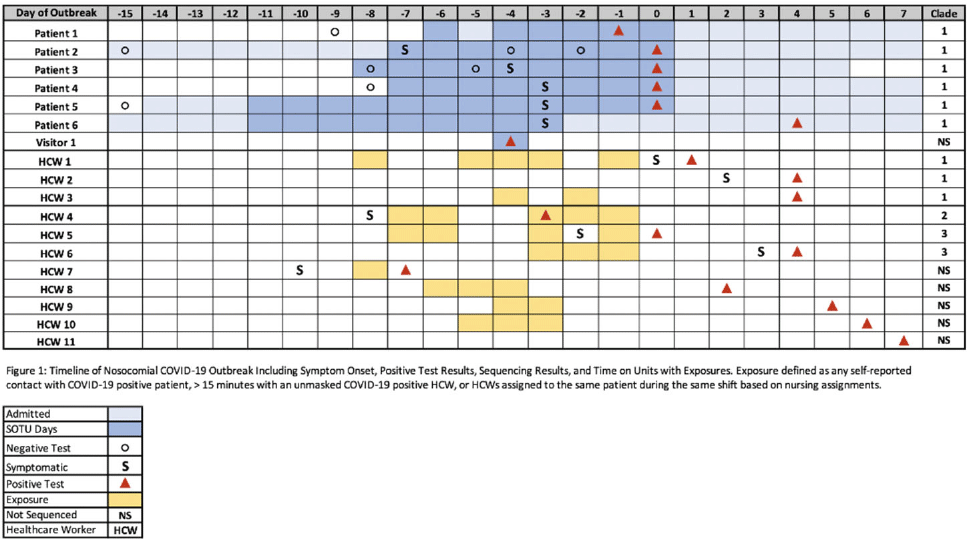
Background: In late September 2021, a cluster of patients with nosocomial COVID-19 was identified on a liver transplant unit at University of Nebraska Medical Center. Methods: The outbreak investigation included contact tracing via patient chart and employee health record reviews and serial prevalence testing for SARS-CoV-2 among potentially exposed patients and healthcare workers (HCWs). Routine admission and preprocedural screening for SARS-CoV-2 was performed, and involved patients had negative admission screening results with positive SARS-CoV-2 tests >5 days from admission. Mitigation strategies involved reinforcement of patient care and visitation procedures. Whole-genome sequencing of positive SARS-CoV-2 specimens was conducted. Results: The potential outbreak cluster included 6 patients in the same quadrant of the liver transplant unit, 1 visitor, and 11 healthcare workers (Fig. 1). Moreover, 4 patients had severe liver disease, including 2 with liver transplants. All HCWs and half of the patients had received 2 doses of mRNA vaccine, albeit >5 months from their second vaccination. Whole-genome sequencing confirmed patients 1–6 and HCWs 1–3 had related transmission of COVID-19. However, infections in HCWs 4–6, who worked in a transplant-related office setting without patient contact, were due to 2 separate introductions of SARS-CoV-2 unrelated to the hospital outbreak. Sequencing could not be performed on HCWs 7–11 due to low viral concentration in the original specimens or unavailable specimen. The SARS-CoV-2 δ (delta) variant (B.1.617.2) was identified in all sequenced samples. HCWs 8–10 were asymptomatic and had had contact with each other and had been involved with an intubation without proper PPE for SARS-CoV-2 on patient 6. HCW 8 had had contact with all 6 patients and HCW 9 had had contact with 5 patients. A clear index case could not be identified; however, we suspect that the index case was either visitor 1, who tested positive during patient 2’s admission, or an asymptomatic healthcare worker (HCWs 8–10). Conclusions: We identified a nosocomial outbreak of the SARS-CoV-2 δ (delta) variant in a solid-organ transplant unit including patients, a visitor, and vaccinated healthcare workers with multiple introductions of the virus. Further transmission was not detected after enhanced infection control measures were introduced, including universal masking and eye protection, closing patient doors, and enforcement of visitor masking policy. We describe the difficulties tracing SARS-CoV-2 transmission in the hospital setting, even with advanced sequencing techniques. This outbreak highlights the importance of booster vaccination and strict infection control practices, especially in the setting of the δ (delta) variant.
Funding: None
Disclosures: None
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation







