3 results
305 - What happens before, during and after crisis for someone with dementia living at home
- Sabarigirivasan Muthukrishnan, Jane Hopkinson, Kate Hydon, Lucy Young, Cristie Howells
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 04 November 2020, pp. 62-63
-
- Article
-
- You have access Access
- Export citation
-
Background:
Best practice in dementia care is support in the home. Yet, crisis is common and can result in hospital admission. Home-treatment of crisis is an alternative to hospital admission that can have better outcomes and is the preference of people living with dementia.
Purpose:To report an investigation of the management of crisis for people with dementia living at home and managed by a Home Treatment Crisis Team.
Objective:To identify critical factors for successful resolution of crisis and avoidance of hospital admission
Methods:The research was mixed-methods case study design. It was an in depth investigation of what happens during crisis in people with dementia and how it is managed by a home treatment crisis team to resolution and outcome at six weeks and six months. Methods were observation of the management of crisis in the home setting for 15 people with dementia (max 3 per person, total 41 observations), interviews with people with dementia (n=5), carers (n=13), and 14 professionals (range 1 to 6 per person, total 29), a focus group with professionals (n=9) and extraction from medical records of demographics and medical history.
The analysis focused on the identification of key treatments, behaviours, education and context important for home treatment to prevent hospital admission.
Findings:The study recruited 15 of the 88 accepted referrals to the service for management of a crisis in a person with dementia.
Factors key for crisis resolution were
a systems approach with embedded respect for personhood,
attention to carer needs independently of the person with dementia,
review and monitoring of the effect of medications,
awareness and promotion of potential benefits with treatment at home,
education of the health and social care workforce in dementia care,
local availability of respite and other social care services.
The Home Treatment Crisis Team created a ‘Safe Dementia Space’ for the person with dementia in crisis. In the first instance, this was immediate but temporary with on-going assessment and intervention until negotiated permanent support was in place coproduced and agreed by stakeholders to be a sustainable dementia space with acceptable risk of harm to the person with dementia or others. The approach enabled avoidance of hospital admission in more than 80% of referrals.
Conclusion:This is the first study to collect data during crisis at home for people with dementia and to investigate process and management. It reveals the Home Treatment Crisis Team created sustainable ‘Safe Dementia Space’ to enable the person with dementia to continue to live in the community during and after crisis, thus avoiding hospital admission. The identified key components of the management approach for crisis resolution are important considerations in the design and delivery of home treatment services for people with dementia in the UK and beyond.
345 - 7 Critical factors for safely supporting dementia patients in mental health crisis in community
- Sabarigirivasan Muthukrishnan, Kate Hydon, Lucy Young, Cristie Howells
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 04 November 2020, pp. 105-106
-
- Article
-
- You have access Access
- Export citation
-
Background:
Best practice in dementia care is support in the home. Yet, crisis is common and can result in hospital admission. Home-treatment of crisis is an alternative to hospital admission that can have better outcomes and is the preference of people living with dementia.
Purpose:To report an investigation of the management of crisis for people with dementia living at home and managed by a Home Treatment Crisis Team.
Objective:To identify critical factors for successful resolution of crisis and avoidance of hospital admission
Methods:The research was mixed-methods case study design. It was an in depth investigation of what happens during crisis in people with dementia and how it is managed by a home treatment crisis team to resolution and outcome at six weeks and six months. Methods were observation of the management of crisis in the home setting for 15 people with dementia (max 3 per person, total 41 observations), interviews with people with dementia (n=5), carers (n=13), and 14 professionals (range 1 to 6 per person, total 29), a focus group with professionals (n=9) and extraction from medical records of demographics and medical history.
The analysis focused on the identification of key treatments, behaviours, education and context important for home treatment to prevent hospital admission.
Findings:The study recruited 15 of the 88 accepted referrals to the service for management of a crisis in a person with dementia.
The seven key factors key for crisis resolution were
a systems approach with embedded respect for personhood,
attention to carer needs independently of the person with dementia,
review and monitoring of the effect of medications,
awareness and promotion of potential benefits with treatment at home,
education of the health and social care workforce in dementia care,
local availability of respite and other social care services.
a dynamic and flexible working ethos and meaningful MDT working with flattened hierarchy
The Home Treatment Crisis Team created a ‘Safe Dementia Space’ for the person with dementia in crisis. In the first instance, this was immediate but temporary with on-going assessment and intervention until negotiated permanent support was in place coproduced and agreed by stakeholders to be a sustainable dementia space with acceptable risk of harm to the person with dementia or others. The approach enabled avoidance of hospital admission in more than 80% of referrals.
Conclusion:This is the first study to collect data during crisis at home for people with dementia and to investigate process and management. It reveals the Home Treatment Crisis Team created sustainable ‘Safe Dementia Space’ to enable the person with dementia to continue to live in the community during and after crisis, thus avoiding hospital admission. The identified key components of the management approach for crisis resolution are important considerations in the design and delivery of home treatment services for people with dementia in the UK and beyond.
446 - Persistent Delusional Disorder (Late Paraphrenia) - An innovative and cost effective clinical model in the community by older adult‘s mental health crisis and home treatment team
- Sabarigirivasan Muthukrishnan, Kate Hydon
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 04 November 2020, pp. 165-166
-
- Article
-
- You have access Access
- Export citation
-
Aims
To review the various available clinical models of care delivery for patients with persistent delusional disorder (PDD) in community and economically evaluate the REACT model of safe care delivery- REACT’s Assertive and Prudent- Model of Safe Care (RAP–MoSC).
MethodsREACT (Response Enhanced Assessment Crisis and Home Treatment Team) is the only bespoke crisis and home treatment team for older adults with mental health problems in the whole of Wales available only for the residents of Cardiff and Vale of Glamorgan through Cardiff and Vale University Health Board..
It was set up on 28 February 2012. The cases of PDD in REACT service since its inception to 31 Dec 2016 were studied in relation to the assertive and prudent health care model. The economic evaluation of this service model for PDD patients was studied in detail.
Results of the studyThe RAP-MoSC model is economically effective in avoiding patients getting admitted to hospital under Mental Health Act by managing them safely in the community.
During the period between 28 February 2012 and 31 December 2016 there were 44 patients with a diagnosis of PDD in REACT’s case load. Only 3 patients got admitted to mental health assessment ward with the average length of stay period of 120 days. 41 patients were safely managed in the community with REACT with an average length of stay period of 21 days in REACT.
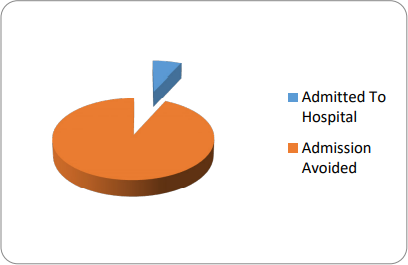
A PDD patient will cost NHS £21,000 if admitted to a mental health bed. If the patient is managed in the community with RAP-MoSC model of care the cost will be £1533.
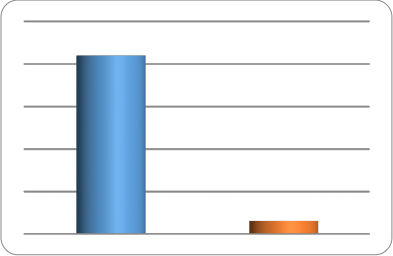
REACT saved £793,548 by avoiding 41 PDD patients being admitted into hospital during an episode of delusional intensification in the period February 2012 to December 2016. PDD patients need under the RAP-MoSC model a bespoke MDT approach with better communication between secondary mental health and primary care services. Assertive and Prudent Clinical leadership is needed to sustain the RAP-MoSC in the community. Clinical reflections of this model of care will be presented in the conference.
ConclusionsOn reflection REACT found that the key points in working with PDD are;
Using a ‘foot in the door approach’
Mental health professionals introducing themselves as Health professionals
Remote prescribing





