5 results
Non-convulsive epiletic seizure after electroconvulsive therapy session
- L. Llovera García, L. Veiga Gil, L. Lopez Unzue, A. Corrales Rodriguez, A. Ballesteros Prados, J. Yoldi Murillo, J. M. Lopez Ilundain
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1021-S1022
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Electroconvulsive therapy (ECT) is a procedure performed under general anaesthesia involving triggering an intentional brief seizure through small electrical currents through the brain. The anaesthetic depth should be adequate prior to shock and measured with BIS, a processed electroencephalogram (EEG) monitor. Adjusting the hypnotic dose allows to decrease the ictal threshold and thus improve the response to treatment and decrease side effects.
ObjectivesOur goal is detecting elements such as spontaneous epileptiform activity after ECT without tonic-clonic activity with the spectral density matrix (SDM).
MethodsOur patient: an 87-year-old woman, diagnosed with F20.2 catatonic schizophrenia and under antipsychotic treatment since her youth. She has required multiple hospital admissions due to psychopathological decompensations until starting monthly maintenance ECT sessions in 2014. Since then she no new hospital admissions have been required.
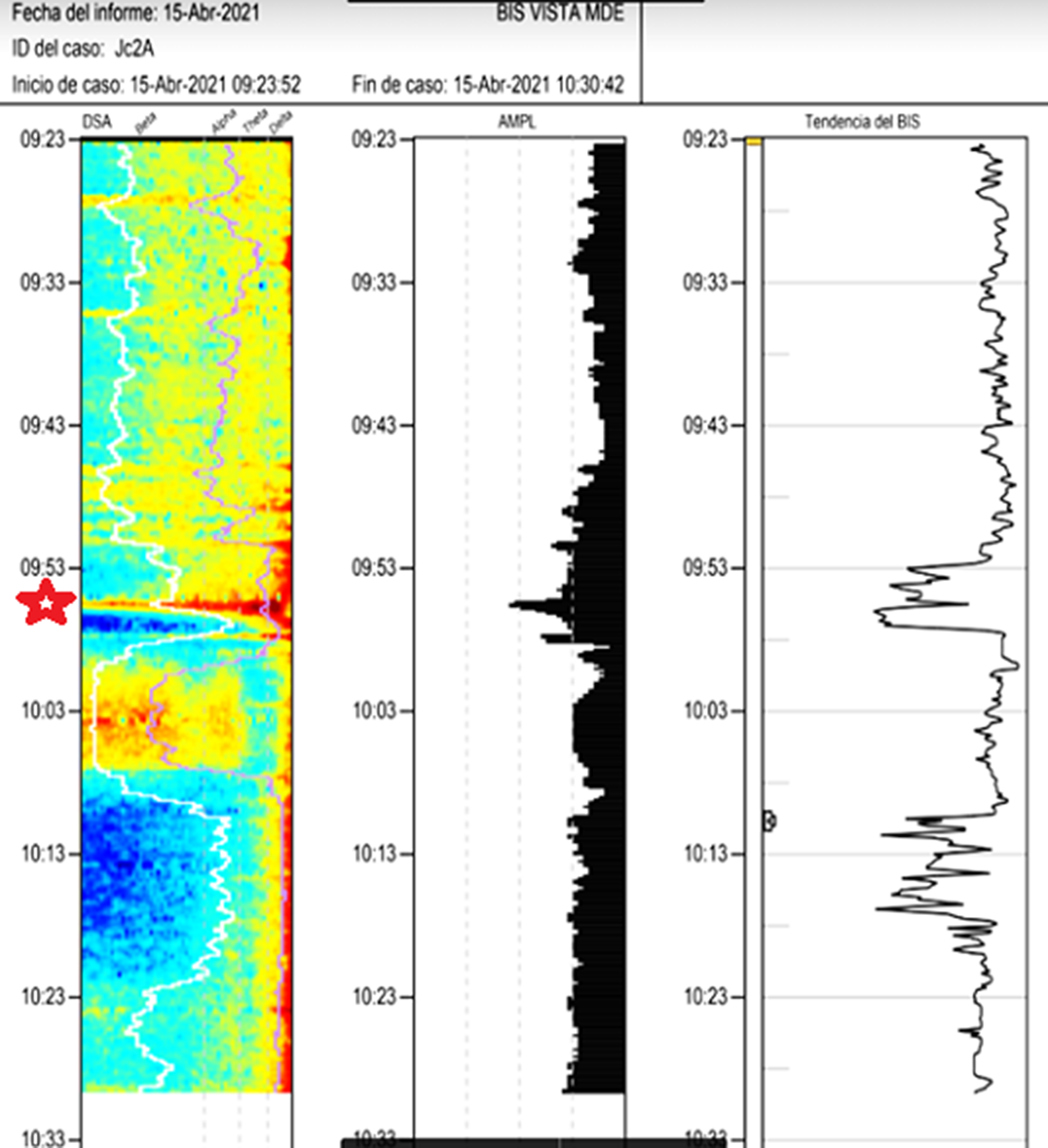
ResultsImages 1D and 1E shows the SDM, a spectrogram of the EEG. The X axis show time (minutes), the Y axis shows the frequency (Hz) and the Z axis shows the energy or intensity of that electrical activity in the frequency bands replaced by colors: warm colors (red) reflecting high intensity electroencephalographic activity and cool colors (yellow, blue and green), low activity. Images 2 and 3’s EDM shows spontaneous epileptiform activity after electroconvulsive therapy without tonic-clonic activity. We observed an initial EDM of an awake patient, with warm colours in practically all frequency bands, including the beta band (13-30 Hz), characteristic of waking states. Around 9:50 anaesthetic induction occurs, activity increases in slow frequencies (red colours in alpha, theta and delta), plus an increase of cold colours in beta, reflecting the disappearance of brain activity in that frequency. The asterisk reflects the EEG response to the electrical discharge, followed by a postcritical state with brain activity exclusively in slow waves and high amplitude (delta and some theta) and absence of activity in other frequencies (blue colour in the beta and alpha bands) around 9:57. At about 10:00 there is an abrupt appearance of high intensity brain activity (warm colours) in beta and alpha and delta, mainly, reflecting spontaneous epileptiform activity after treatment and clinically reflected as a patient absent and disconnected from the environment, but without tonic-clonic activity. New postcritical state in which blue colour predominates, reflecting little brain activity, and warmer colours reappear in all frequency bands, including beta, reflecting the progressive recovery of wakefulness.
Image:
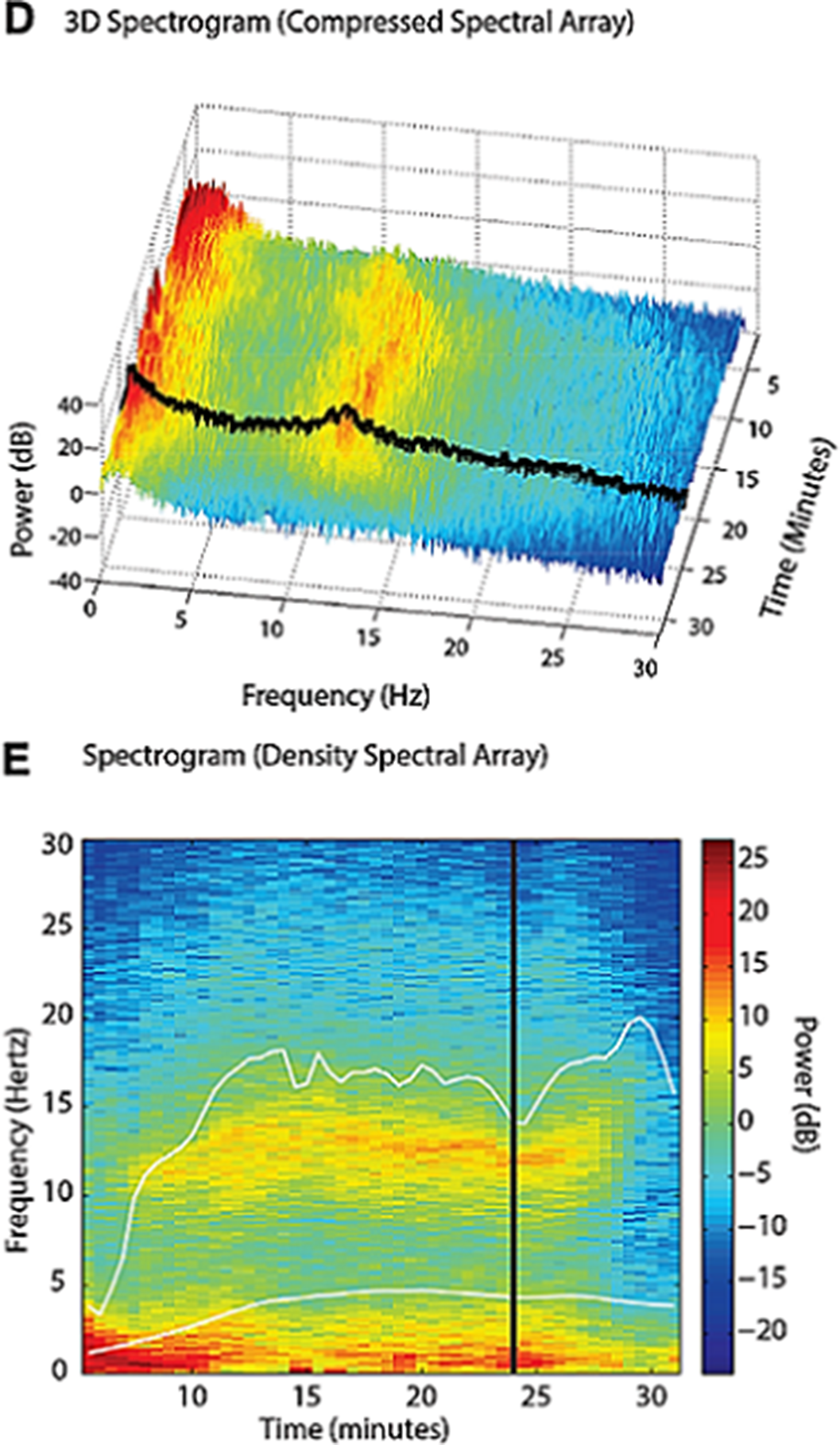
Image 2:
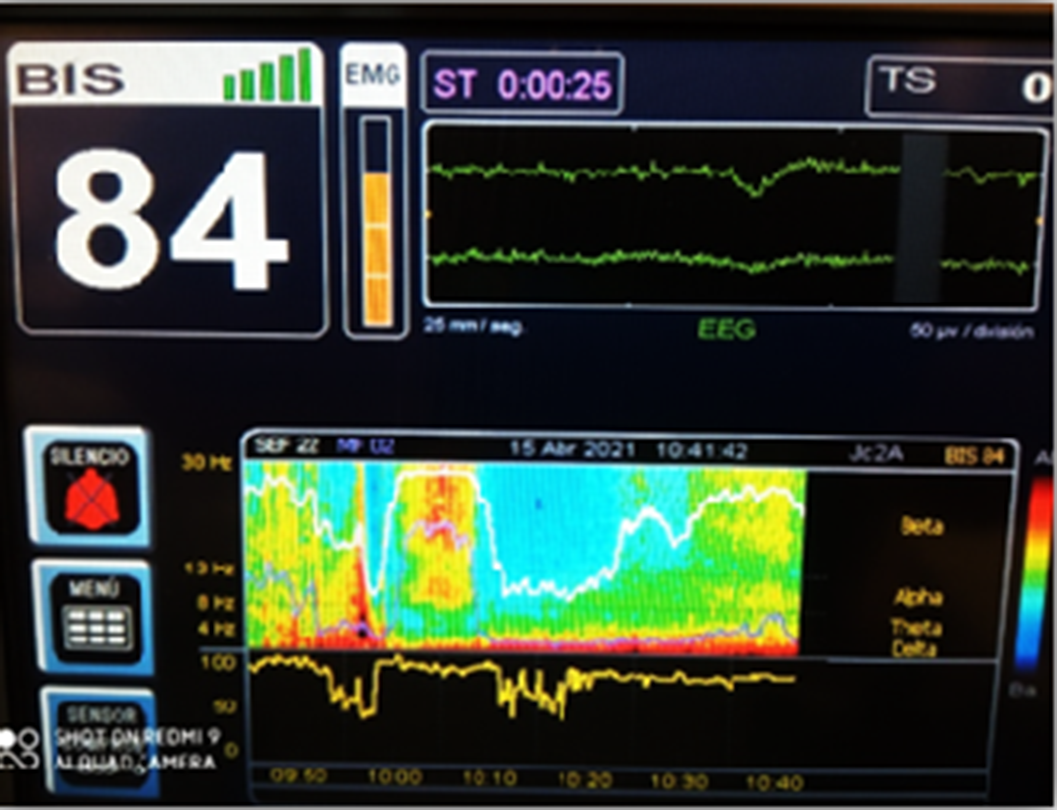
Image 3:
 Conclusions
ConclusionsPsychiatric pathology can be reflected in the SDM, which allows to observe changes in the EEG, correcting the electrical stimulus of the shock and the dose of anesthetic appropriate to the patient to trigger an intentional brief seizure under general anesthesia.
Disclosure of InterestNone Declared
P01-157 - Comorbidity of Generalized Anxiety Disorder with Mayor Depression in Primary Care
- E. Serrano Drozdowskyj, P. García Parajuá, C. Peláez, L. García Murillo
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E362
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Generalized anxiety disorder (GAD) is the second more frequent disorder after mayor depression in primary care. It has great impact in patients functioning and consumption of health services. The clinical presentation in this setting, predominantly somatic, and its frequent comorbidity may lead to underdiagnosed and mistreatment. Features of GAD in this setting are evaluated.
MethodsAn epidemiological and multicenter study was carried out, collecting demographic data and clinical history, on a randomly selected representative sample of 225 patients from three primary care centers of the area of Madrid (Spain). Also Patient Health Questionnaire (PHQ) and Dream Questionnaire of Oviedo were reported.
Chi-square test were used to compare in patients diagnosed of GAD versus other psychiatric patients and non-psychiatric diagnosed.
Results and conclusionsClinic prevalence of GAD was 11,1% in the sample. In GAD cases, mayor depression was found in 68,0% (Chi2, p< 0,001). So, it shows the comorbidity of GAD with mayor depression has a relevant presence in primary care. This suggest a possible relation between both disorders.
On the other hand, the presence of depressive symptoms were significantly higher in GAD patients (U test, p< 0,001). Unexpected non statistical significant differences were found in the number of somatic symptoms, sick leave days and utilization of medical services. Comorbidity with mayor depression disorder may work as a confounding factor masking the differences found in other epidemiological studies.
Better clinical diagnosis tools and longitudinal studies might be proceed to clear this relation and improve its treatment.
P01-181 - Anthropometric Paramethers in Males with Eating Disorder
- R. Calero-Fernández, L. García-Murillo, M.J. Martín, V. Costarelli, C. Peláez, J. Picazo, L. Fernández, L. Caballero-Martínez, M. Graell-Berna
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E387
-
- Article
-
- You have access Access
- Export citation
-
Background
Most of the studies about Eating Disorders in adolescents have been typically focused on females, only to conclude that the approach should be similar in males. It has been stimated that 5-10% of patients with Anorexia Nervosa are males. Later age of onset and higher prevalence of premorbid overweight are considered among the main differences with female patients.
ObjectivesAnalysis of the anthropometric variables of a sample of males with diagnosis of Restrictive Eating Disorder.
MethodsNaturalistic, Descriptive and Retrospective study
- Sample: 22 male adolescents
- Inclusion criteria: males with Restrictive Eating Disorder diagnosis (according to DSM-IV criteria) admitted to an Eating Disorder ward during 2007 and 2008
- “ad hoc” questionnaire (15 items)
- Analysis: PASW statistics 18
ResultsAge range: 7-14years (medium age=14,79±2,50years).11 patients (50%) were older than 16 years-old
- Medium BMI (Body Mass Index) at the beginning of the admission was 17,79kg/m2.
medium weight loss: 13,5±7,02kg/m2 (corresponding to a reduction of 22,24±7,52% of the previous weight)
- Medium speed of weight loss: 0,92±1,1kg/54
- BMI at discharge: 18,69 ±3,43 kg/m2
- 19/22 patients (86%) had a premorbid history of overweight
- Binge eating: 8 patients (36,4%)
- Purgative behaviour: 10 patients (45%)
- Laxatives use: 4 patients (18%)
- Intense physical exercise: 21 patients (95,5%)
- Average duration of current restrictive episode: 13,7 months
ConclusionsIn the studied sample we observed:
- High prevalence of premobid overweight
- Very high frequency of compulsive exercise
- Drastic weight loss and loss of a very high percentage of the previous weight, in short periods of time, reaching very low BMI.
P03-330 Case Report: Serotonin Syndrome vs Neuroleptic Malignant Syndrom
- L. García-Murillo, R. Calero-Fernandez, S. Jimenez Fernandez, M. Rojas Estape, E. Serrano, E. Sanchez, C. Iglesias
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E936
-
- Article
-
- You have access Access
- Export citation
-
Background
Serotonin Syndrome (SS) is an adverse drug reaction that drives mental-status changes, autonomic hyperactivity and neuromuscular abnormalities.
Neuroleptic Malignant Syndrome (NMS) is an idiopathic reaction to dopamine-antagonist that consists of extra-pyramidal symptoms, autonomic dysfunction, hyperthermia, diaphoresis and fluctuating consciousness.
Differential diagnosis is sometimes difficult for their overlapping clinical features. Potentially lethal, both require heightened clinical awareness for prevention, recognition and prompt treatment.
Case reportCaucasian 59 years-old woman with Catatonic profile (Scored: severity-17points/ 5 screening in Bush-Francis Catatonia-Rating-Scale).
Past Medical History- Hypothyroidism
- Bipolar Disorder type-2 (25 years of evolution)
15 days before hospitalization, anafranil and fluoxetine treatment was replaced by Trazodone 200 mg/day and venlafaxine 150mg/day. She was also on valpromida and lorazepam 15 mg/day.
Current historyMutism, negativism. No reaction to painful stimuli, stuporous. Diaphoresis, pallor, tremor, axial rigidity without pyramidalism (>lower limbs), high fever (40°C), tachycardia (>100lpm), rhabdomyolysis (CPK reached 17.000, 48 hours after the admission), leukocytosis, upper transaminasas, hiponatremia with hiperpotasemia.
Differential diagnosis- NMS: Intensity, duration and high CPK are suggestive (Sternbach). This syndrome has been described due to Venlafaxine.
- SS: Combination of Venlafaxine and Trazodone favors but she doesn't have acatisia, hiperreflexia, diarrhea and it wasn't resolved after 96 hours.
Drugs were removed and Lorazepam on high doses (5mg/day) was prescribed. One month later the patient was totally recovered of the episode.
ConclusionsIf unsure diagnoses it's priority to remove the causing drugs and supportive care. Afterwards, it can be used benzodiacepines, also dantroleno in SNM.
Hospitalized psychoses after liver transplantation
- M. Rojas-Estapé, C. Iglesias Rodriguez, L. Garcia Murillo
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 395
-
- Article
-
- You have access Access
- Export citation
-
Calcineurin inhibitors can cause neurological and psychiatric side effects. Mild symptoms to severe complications can be found.
Case presentationWe report a 49 year old man who received an orthotopic liver transplantation in May 2010. He received tacrolimus. Ten days later, while he was still in Hospital, he suffered behavioural disorders, being psychotic with delusions of persecution; he called the police thinking that he was being poisened by the staff of the Hospital. Although his Tacrolimus blood concentration had been kept in the normal range, his symptoms improved dramatically when the Tacrolimus was changed into Cyclosporine and Haloperidol was introduced at high doses (7 mg/day) for 10 days when the dose was reduced to 4 mg/day.
Medical historyChronic hepatitis VHC 1a in 1994. Received treatment with Interferon alfa in 1997 with no antiviral answer. In 2001 new treatment with pegylated Interferon and Ribavirine with positive virological answer but had to be stopped because of psychoses secondary to treatment. New treatment in March 2006 to March 2007 with Pegasys+Ribavirine with rapid virologycal answer with prophylactic Olanzapine 5 mg during a year with no psychotic symptons. In May 2009, Child Pugh C10, in list for liver transplantation.
We discuss the implications of these findings and the relevance for future clinical care in these patients.






