16 results
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
- Konstantinos N. Fountoulakis, Grigorios N. Karakatsoulis, Seri Abraham, Kristina Adorjan, Helal Uddin Ahmed, Renato D. Alarcón, Kiyomi Arai, Sani Salihu Auwal, Michael Berk, Sarah Bjedov, Julio Bobes, Teresa Bobes-Bascaran, Julie Bourgin-Duchesnay, Cristina Ana Bredicean, Laurynas Bukelskis, Akaki Burkadze, Indira Indiana Cabrera Abud, Ruby Castilla-Puentes, Marcelo Cetkovich, Hector Colon-Rivera, Ricardo Corral, Carla Cortez-Vergara, Piirika Crepin, Domenico De Berardis, Sergio Zamora Delgado, David De Lucena, Avinash De Sousa, Ramona Di Stefano, Seetal Dodd, Livia Priyanka Elek, Anna Elissa, Berta Erdelyi-Hamza, Gamze Erzin, Martin J. Etchevers, Peter Falkai, Adriana Farcas, Ilya Fedotov, Viktoriia Filatova, Nikolaos K. Fountoulakis, Iryna Frankova, Francesco Franza, Pedro Frias, Tatiana Galako, Cristian J. Garay, Leticia Garcia-Álvarez, Maria Paz García-Portilla, Xenia Gonda, Tomasz M. Gondek, Daniela Morera González, Hilary Gould, Paolo Grandinetti, Arturo Grau, Violeta Groudeva, Michal Hagin, Takayuki Harada, Tasdik M. Hasan, Nurul Azreen Hashim, Jan Hilbig, Sahadat Hossain, Rossitza Iakimova, Mona Ibrahim, Felicia Iftene, Yulia Ignatenko, Matias Irarrazaval, Zaliha Ismail, Jamila Ismayilova, Asaf Jakobs, Miro Jakovljević, Nenad Jakšić, Afzal Javed, Helin Yilmaz Kafali, Sagar Karia, Olga Kazakova, Doaa Khalifa, Olena Khaustova, Steve Koh, Svetlana Kopishinskaia, Korneliia Kosenko, Sotirios A. Koupidis, Illes Kovacs, Barbara Kulig, Alisha Lalljee, Justine Liewig, Abdul Majid, Evgeniia Malashonkova, Khamelia Malik, Najma Iqbal Malik, Gulay Mammadzada, Bilvesh Mandalia, Donatella Marazziti, Darko Marčinko, Stephanie Martinez, Eimantas Matiekus, Gabriela Mejia, Roha Saeed Memon, Xarah Elenne Meza Martínez, Dalia Mickevičiūtė, Roumen Milev, Muftau Mohammed, Alejandro Molina-López, Petr Morozov, Nuru Suleiman Muhammad, Filip Mustač, Mika S. Naor, Amira Nassieb, Alvydas Navickas, Tarek Okasha, Milena Pandova, Anca-Livia Panfil, Liliya Panteleeva, Ion Papava, Mikaella E. Patsali, Alexey Pavlichenko, Bojana Pejuskovic, Mariana Pinto Da Costa, Mikhail Popkov, Dina Popovic, Nor Jannah Nasution Raduan, Francisca Vargas Ramírez, Elmars Rancans, Salmi Razali, Federico Rebok, Anna Rewekant, Elena Ninoska Reyes Flores, María Teresa Rivera-Encinas, Pilar Saiz, Manuel Sánchez de Carmona, David Saucedo Martínez, Jo Anne Saw, Görkem Saygili, Patricia Schneidereit, Bhumika Shah, Tomohiro Shirasaka, Ketevan Silagadze, Satti Sitanggang, Oleg Skugarevsky, Anna Spikina, Sridevi Sira Mahalingappa, Maria Stoyanova, Anna Szczegielniak, Simona Claudia Tamasan, Giuseppe Tavormina, Maurilio Giuseppe Maria Tavormina, Pavlos N. Theodorakis, Mauricio Tohen, Eva Maria Tsapakis, Dina Tukhvatullina, Irfan Ullah, Ratnaraj Vaidya, Johann M. Vega-Dienstmaier, Jelena Vrublevska, Olivera Vukovic, Olga Vysotska, Natalia Widiasih, Anna Yashikhina, Panagiotis E. Prezerakos, Daria Smirnova
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
The prevalence of medical illnesses is high among patients with psychiatric disorders. The current study aimed to investigate multi-comorbidity in patients with psychiatric disorders in comparison to the general population. Secondary aims were to investigate factors associated with metabolic syndrome and treatment appropriateness of mental disorders.
MethodsThe sample included 54,826 subjects (64.73% females; 34.15% males; 1.11% nonbinary gender) from 40 countries (COMET-G study). The analysis was based on the registration of previous history that could serve as a fair approximation for the lifetime prevalence of various medical conditions.
ResultsAbout 24.5% reported a history of somatic and 26.14% of mental disorders. Mental disorders were by far the most prevalent group of medical conditions. Comorbidity of any somatic with any mental disorder was reported by 8.21%. One-third to almost two-thirds of somatic patients were also suffering from a mental disorder depending on the severity and multicomorbidity. Bipolar and psychotic patients and to a lesser extent depressives, manifested an earlier (15–20 years) manifestation of somatic multicomorbidity, severe disability, and probably earlier death. The overwhelming majority of patients with mental disorders were not receiving treatment or were being treated in a way that was not recommended. Antipsychotics and antidepressants were not related to the development of metabolic syndrome.
ConclusionsThe finding that one-third to almost two-thirds of somatic patients also suffered from a mental disorder strongly suggests that psychiatry is the field with the most trans-specialty and interdisciplinary value and application points to the importance of teaching psychiatry and mental health in medical schools and also to the need for more technocratically oriented training of psychiatric residents.
Are there any differences in clinical and biochemical variables between bipolar patients with or without lifetime psychotic symptoms?
- C. M. Esposito, A. Ceresa, M. Di Paolo, T. Surace, L. Moioli, F. Legnani, G. Nosari, V. Ciappolino, A. M. Auxilia, M. Cappellazzi, I. Tagliabue, L. Cirella, E. Capuzzi, A. Caldiroli, A. Dekanalis, M. Clerici, M. Buoli
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S505-S506
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar Disorder (BD) is a frequent psychiatric disorder, which can be associated with high disability. Psychotic symptoms occur in more than half of bipolar patients and are associated with an unfavorable course of the disorder (Chakrabarti et al. World J Psychiatry 2022; 12(9) 1204-1232).
ObjectivesThe aim of this study is therefore to identify clinical and biological markers able to discriminate between BD patients with (BD-PS) and without lifetime psychotic symptoms (BD-NPS) to facilitate early diagnosis and to implement a target clinical management of these patients.
MethodsWe recruited 665 patients consecutively hospitalized for BD at Fondazione IRCCS Policlinico (Milan) and at San Gerardo Hospital (Monza). Data were obtained through a screening of the clinical charts and blood analyses conducted during the hospitalization. Patients were assessed by psychometric scales. The two groups (BD-PS and BD-NPS) were compared by t tests for quantitative variables and χ2 tests for qualitative ones. Variables that resulted to be significant in univariate analyses were inserted in binary logistic models with the presence of psychotic symptoms as dependent variable.
ResultsAmong the total sample, 64.5% of patients were affected by BD-PS while 35.5% by BD-NPS. The final binary logistic regression model showed that, compared to patients with BD-NPS, those with BD-PS had a longer duration of hospitalization (p=0.007) and were more frequently hospitalized for a manic episode (p=0.001). In addition, subjects with BD-PS had a lower score on the current Global Assessment of Functioning (GAF) (t = 3.157; p = 0.002) and were more frequently males (χ² = 4.061; p = 0.044; OR = 1.399). With regard to biological variables, patients with BD-PS, compared to the counterpart, had a higher Neutrophile to Lymphocyte Ratio (NLR) (t = 2.776; p = 0.006), lower levels of Gamma-Glutamyl Transferase (γGT) (t = 2.249; p = 0.026), higher total bilirubin (t = 2.348; p = 0.019) and creatine phosphokinase (CPK) (t=2.807; p = 0.005), lower total cholesterol (t = 2.369; p = 0.018) and triglycerides (t = 2.554; p = 0.013).
ConclusionsOur data appear to be in line with the literature, especially with respect to the occurrence of psychotic symptoms mainly in manic episodes and their association with greater clinical severity, longer hospitalization and worse outcome (Altamura et al. Aust N Z J Psychiatry 2019; 53(8) 772-781). From a biological point of view, it seems important to emphasize that patients with lifetime psychotic symptoms presented a higher NLR, revealing more prominent low-grade inflammation in these patients than the counterpart. These data confirm the possibility of using NLR as biomarker of severity in bipolar patients, as proposed previously by other authors (Kulacaoglu et al. Nord J Psychiatry 2022). Future multi-center study have to confirm the results of the present study.
Disclosure of InterestNone Declared
Clinical and biochemical parameters associated with substance-induced psychotic disorder: which differences between alcohol, cannabis and psychostimulants
- G. Nosari, A. Ceresa, M. Di Paolo, C. M. Esposito, V. Ciappolino, A. Calabrese, F. Legnani, A. M. Auxilia, M. Capellazzi, I. Tagliabue, L. Cirella, E. Capuzzi, A. Caldiroli, A. Dakanalis, M. Clerici, M. Buoli
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S514-S515
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
According to DSM V, substance-induced psychotic disorder is a mental health condition in which the onset of psychotic symptoms can be traced to the use of a psychotropic substance. The pathogenesis of this disease is still poorly understood; current literature traces its causes back to genetic predisposition and early traumatic events (i.e. child abuse).
ObjectivesThe present study aims to identify specific clinical features and biochemical markers which could be addressed as predictors for the long-term prognosis of this disease. Moreover, we aim to identify specific correlations between the clinical phenotype and the underlying substance abuse, in order to allow the early start of a tailored treatment.
MethodsBetween 2020 and 2022 we recruited 218 patients referring to the Policlinico Hospital in Milan and the San Gerardo Hospital in Monza, Italy. All the patients were diagnosed with substance induced psychotic disorder: 31 reported alcohol abuse (14,2%), 71 psichostimulants (32,6%), 116 cannabis, (53,2%). For each patients, we collected demographic data, medical records and a comprehensive psychometric assessment (GAF, PANSS, BPRS, Modified Sad Person Scale-MOAS). Furthermore, we collected a blood sample for dosing Na+, K+, Na+/K+, hemogram with formula and platelets, glucose , urea, creatinine, uric acid, transaminases, γGT, bilirubin, plasma proteins, albumin, LDH, CPK, PCHE, cholesterol, HDL, LDL, Tg, TSH.
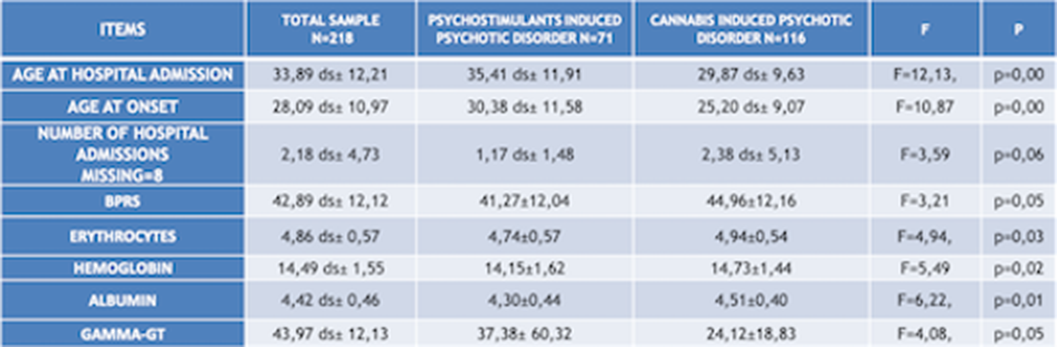
ResultsChi squared test (χ²) has been used to compare qualitative variables between the 3 subgrous (alcohol-, psychostimulants- and cannabis-induced psychotic syndromes) (fig.1). One way ANOVA test has been used to compare quantitative variables between the same 3 subgroups (fig.2). After removing one of the subgropus (alcohol-induced psychotic symptoms), the same analysis have been repeated. Significant variables have been included in a binary logistic regression model in order to confirm their validity as predictors for cannabis- and psychostimulants-induced psychotic disorders (fig 3). Finally we performed Omnibus test and Hosmer-Lemeshow test in order to verify the validity of these regression models.
Image:
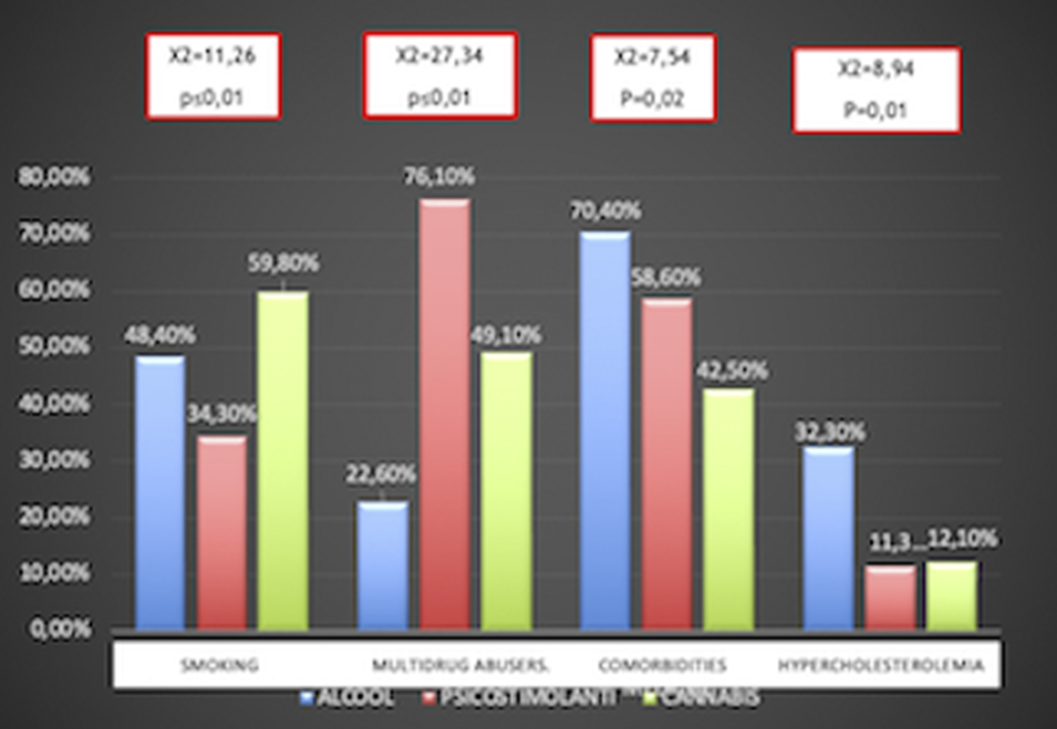
Image 2:
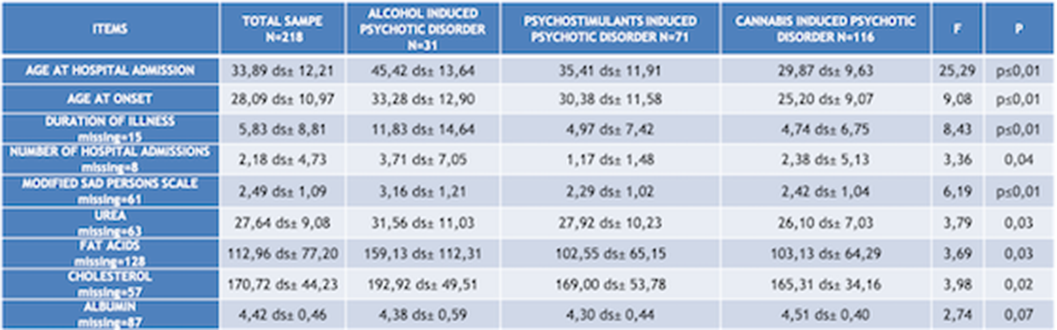
Image 3:
 Conclusions
ConclusionsFor each considered subgroups, we indentified the following features. Alcohol induced psychotic syndrome: higher age of onset and age of hospital admission, higher cholesterol and hurea levels, , high comorbidity with medical conditions anxiety/depression, low social functioning, higher suicidal risk;, higher hospitalization rate. Cannabis induced psychotic syndrome: higher hemoglobin and albumin levels, more severe psychiatric symtoms (BPRS), higher smoking rates. Psychostimulants induced psychotic syndrome: higher multi-drug abuse risk. We could assume that according to this consideration the treatment protocols for each of these subgroups should be tailored according to their specific features.
Disclosure of InterestNone Declared
Burden of infectious disease studies in Europe and the United Kingdom: a review of methodological design choices
- Periklis Charalampous, Juanita A. Haagsma, Lea S. Jakobsen, Vanessa Gorasso, Isabel Noguer, Alicia Padron-Monedero, Rodrigo Sarmiento, João Vasco Santos, Scott A. McDonald, Dietrich Plass, Grant M. A. Wyper, Ricardo Assunção, Elena von der Lippe, Balázs Ádám, Ala'a AlKerwi, Jalal Arabloo, Ana Lúcia Baltazar, Boris Bikbov, Maria Borrell-Pages, Iris Brus, Genc Burazeri, Serafeim C. Chaintoutis, José Chen-Xu, Nino Chkhaberidze, Seila Cilovic-Lagarija, Barbara Corso, Sarah Cuschieri, Carlotta Di Bari, Keren Dopelt, Mary Economou, Theophilus I. Emeto, Peter Fantke, Florian Fischer, Alberto Freitas, Juan Manuel García-González, Federica Gazzelloni, Mika Gissler, Artemis Gkitakou, Hakan Gulmez, Sezgin Gunes, Sebastian Haller, Romana Haneef, Cesar A. Hincapié, Paul Hynds, Jane Idavain, Milena Ilic, Irena Ilic, Gaetano Isola, Zubair Kabir, Maria Kamusheva, Pavel Kolkhir, Naime Meriç Konar, Polychronis Kostoulas, Mukhtar Kulimbet, Carlo La Vecchia, Paolo Lauriola, Miriam Levi, Marjeta Majer, Enkeleint A. Mechili, Lorenzo Monasta, Stefania Mondello, Javier Muñoz Laguna, Evangelia Nena, Edmond S. W. Ng, Paul Nguewa, Vikram Niranjan, Iskra Alexandra Nola, Rónán O'Caoimh, Marija Obradović, Elena Pallari, Mariana Peyroteo, Vera Pinheiro, Nurka Pranjic, Miguel Reina Ortiz, Silvia Riva, Cornelia Melinda Adi Santoso, Milena Santric Milicevic, Tugce Schmitt, Niko Speybroeck, Maximilian Sprügel, Paschalis Steiropoulos, Aleksandar Stevanovic, Lau Caspar Thygesen, Fimka Tozija, Brigid Unim, Hilal Bektaş Uysal, Orsolya Varga, Milena Vasic, Rafael José Vieira, Vahit Yigit, Brecht Devleesschauwer, Sara M. Pires
-
- Journal:
- Epidemiology & Infection / Volume 151 / 2023
- Published online by Cambridge University Press:
- 09 January 2023, e19
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
This systematic literature review aimed to provide an overview of the characteristics and methods used in studies applying the disability-adjusted life years (DALY) concept for infectious diseases within European Union (EU)/European Economic Area (EEA)/European Free Trade Association (EFTA) countries and the United Kingdom. Electronic databases and grey literature were searched for articles reporting the assessment of DALY and its components. We considered studies in which researchers performed DALY calculations using primary epidemiological data input sources. We screened 3053 studies of which 2948 were excluded and 105 studies met our inclusion criteria. Of these studies, 22 were multi-country and 83 were single-country studies, of which 46 were from the Netherlands. Food- and water-borne diseases were the most frequently studied infectious diseases. Between 2015 and 2022, the number of burden of infectious disease studies was 1.6 times higher compared to that published between 2000 and 2014. Almost all studies (97%) estimated DALYs based on the incidence- and pathogen-based approach and without social weighting functions; however, there was less methodological consensus with regards to the disability weights and life tables that were applied. The number of burden of infectious disease studies undertaken across Europe has increased over time. Development and use of guidelines will promote performing burden of infectious disease studies and facilitate comparability of the results.
A systematic review on mediators between adversity and psychosis: potential targets for treatment
- Luis Alameda, Victoria Rodriguez, Ewan Carr, Monica Aas, Giulia Trotta, Paolo Marino, Natasha Vorontsova, Andrés Herane-Vives, Romayne Gadelrab, Edoardo Spinazzola, Marta Di Forti, Craig Morgan, Robin M Murray
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 12 / September 2020
- Published online by Cambridge University Press:
- 03 August 2020, pp. 1966-1976
-
- Article
- Export citation
-
Various psychological and biological pathways have been proposed as mediators between childhood adversity (CA) and psychosis. A systematic review of the evidence in this domain is needed. Our aim is to systematically review the evidence on psychological and biological mediators between CA and psychosis across the psychosis spectrum. This review followed PRISMA guidelines. Articles published between 1979 and July 2019 were identified through a literature search in OVID (PsychINFO, Medline and Embase) and Cochrane Libraries. The evidence by each analysis and each study is presented by group of mediator categories found. The percentage of total effect mediated was calculated. Forty-eight studies were included, 21 in clinical samples and 27 in the general population (GP) with a total of 82 352 subjects from GP and 3189 from clinical studies. The quality of studies was judged as ‘fair’. Our results showed (i) solid evidence of mediation between CA and psychosis by negative cognitive schemas about the self, the world and others (NS); by dissociation and other post-traumatic stress disorder symptoms; and through an affective pathway in GP but not in subjects with disorder; (iii) lack of studies exploring biological mediators. We found evidence suggesting that various overlapping and not competing pathways involving post-traumatic and mood symptoms, as well as negative cognitions contribute partially to the link between CA and psychosis. Experiences of CA, along with relevant mediators should be routinely assessed in patients with psychosis. Evidence testing efficacy of interventions targeting such mediators through cognitive behavioural approaches and/or pharmacological means is needed in future.
Specific rehabilitative and psychotherapeutic groups for cocaine addicted patients: A new model of treatment
- G. Conte, L. Angelicola Nizza, B. Cassiani, M. Di Paolo, F. Focà, E. Rigino, C. Villella, P. Bria
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, pp. S184-S185
-
- Article
-
- You have access Access
- Export citation
-
The need for a specific therapeutic-rehabilitative group for cocaine addicted patients rises up both from the progressive increase of cocaine use in the general population and from peculiar personality traits and associated psychopathology of these clients. Moreover, it is difficult to mantain a compliance to therapy, because there are no specific anticraving or antidothic drugs for cocaine addiction.
Therefore our equipe developed a short integrated treatment (ten weeks), of “group concelling” and “psychodinamic group therapy” in association. The group is open and composed by a maximum of eight participants.
The novelties of this model are: (1) hospital setting, (2) a short duration and (3) synergy between two different approaches: Minnesota 12 steps model (one sessions weekly, held by a councellor on addiction), and a psychodinamic group therapy (one session weekly).
Main success is the retention of patinets in therapy for a long time. In twenty months (March 2005- October 2006), fourty cocaine-addicted patients started this program: only 30% of them dropped out, while 70% of patients completed the treatment. 64% of the latter where completely abstinent, while 36% relapsed during the therapy. All of them are still continuing some therapy at the moment: 46% individual psychotherapy, 25% individual psychotherapy and pharmacological therapy, 14% narcotics anonymous attendance, 11% N.A. groups and pharmacological therapy, 4% is in a T. C.
Changes of the populations of patients in an addictive disorders service in Rome: 2001-2006
- G. Conte, E. Righino, E. Maniccia, L. Angelicola Nizza, M. Di Paolo, M. Pomponi, C. Villella, P. Bria
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, p. S185
-
- Article
-
- You have access Access
- Export citation
-
In the last six years an increasing number of patients seeking care for cocaine dependence entered the Day Hospital program at Catholic University medical school, with a milder variation in the number of opioid dependent patients. The number of cocaine dependent patients doubled year by year from 15 pts in 2003, through 32 in 2004, to 60 in 2005; preliminary data from 2006 seem to follow this trend. A minority of patients are addicted to other drugs. This outgrowth in cocaine addicted patients could be related both to a wider diffusion of cocaine related problems in the general population in Italy1 and to the institution of a specific program for cocaine related disorders in our service. The mean age of opioid dependent patients remained quite stable through years, with a slight increase from 32,1 years, with a standard deviation of 6,9 in 2001 to 33,5 with a SD of 7,0 in 2005. In the same years we observed a slight decrease in the mean age of cocaine patients, frome 36,2 years with a SD of 11,2 in 2001 to 32,8 with a SD of 6,8 in 2005. Both substances are most commonly abused by men: 83,1% of cocaine dependent and 79,2% of opioid dependent patients are male, while only 16,1% of cocaine and 20,1% of opioid dependent patients are female.
Age in Pathological Gambling: Correlations with Personality and Psychiatric Comorbidity
- M. Pascucci, M. Pettorruso, C. Villella, E. Righino, C. Ciciarelli, S. Chiappini, A. Di Cesare, R. Testa, M. Di Paolo, L. Janiri, G. Conte
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Aims
over the past few years Gambling has significantly increased in Italy, being considered as an acceptable form of entertainment and leisure activity. Our aim is to study personality traits and the psychiatric comorbidity of gamblers in relation to the different age and the onset of gambling.
Methods71 patients affected by Pathological Gambling (PG), who accessed in our service (A. Gemelli Hospital, Rome- Italy), underwent the following assessment tests:
-Addiction Severity Index (ASI);
-Temperament and Character Inventory-Revised (TCI-R) to study personality traits;
-MINI-International Neuropsychiatric Interview for psychiatric comorbidity.
Resultswe found that younger gamblers have higher TCI-R scores in the subscales NS1 (exploratory excitability)(p<0,001) and NS3 (extravagance)(p=0,024) and lower scores in HA2 (fear of uncertainty) and ST3 (spiritual acceptance)(p=0,005). An earlier age of onset of PG correlates with higher scores in NS1 (p=0,003), NS3 (p=0,047), Novelty Seeking (p=0,016) and lower HA2 (p=0,034). Patients with gambling onset before age 20 have more probabilities of playing multiple kinds of games (p=0,004), while lower probabilities of playing passive games (p=0026); furthermore they exhibit antisocial personality disorder (p=0,033) and addiction familiarity (p=0,006). Late-onset gamblers (age > 45 years) prefer passive games (p=0,007) and usually don't play online games (p=0,02).
Conclusionsgamblers are a heterogeneous population with regard to personality traits, psychiatric comorbidity, familiarity and type of games played. Paying attention to the gamblers' age and the age of onset of PG could be useful to a greater understanding of the individual differences of patients, and to a deeper knowledge of their disorder.
Frequency and clinical correlates of bipolar features in acute coronary syndrome patients
- S. Pini, M. Abelli, C. Gesi, L. Lari, A. Cardini, L. Di Paolo, F. Felice, R. Di Stefano, G. Mazzotta, C. Oligeri, F.M. Bovenzi, L. Borelli, D. Bertoli, P. Michi, A. Muccignat, J. Micchi, A. Balbarini
-
- Journal:
- European Psychiatry / Volume 29 / Issue 4 / May 2014
- Published online by Cambridge University Press:
- 15 April 2020, pp. 253-258
-
- Article
- Export citation
-
Background:
Depression and acute coronary syndrome (ACS) are both extremely prevalent diseases. Studies aimed at evaluating whether depression is an independent risk factor for cardiac events provided no definitive results. In most of these studies, depression has been broadly defined with no differentiation between unipolar (MDD) versus bipolar forms (BD). The aim of this study was to evaluate the frequency of DSM-IV BD (bipolar I and bipolar II subtypes, cyclothymia), as well as temperamental or isolated bipolar features in a sample of 171 patients hospitalized for ACS. We also explored whether these psychopathological conditions were associated with some clinical characteristics of ACS.
Methods:Patients with ACS admitted to three neighboring Cardiac Intensive Care Units (CICUs) in a 12-month continuative period of time were eligible for inclusion if they met the criteria for either acute myocardial infarct with or without ST-segment elevation or unstable angina, verified by standard ACS criteria. All patients underwent standardized cardiological and psychopathological evaluations.
Results:Of the 171 ACS patients enrolled, 37 patients (21.7%) were found to have a DSM-IV mood disorder. Of these, 20 (11.7%) had bipolar type I or type II or cyclothymia, while 17 (10%) were the cases of MDD. Rapid mood switches ranged from 11% of ACS patients with no mood disorders, to 47% of those with MDD to 55% of those with BD. Linear regression analysis showed that a diagnosis of BD (p = .023), but not that of MDD (p = .721), was associated with a significant younger age at the index episode of ACS. A history of previous coronary events was more frequent in ACS patients with BD than in those with MDD.
Conclusions:Our data indicate that bipolar features and diagnosis are frequent in ACS patients. Bipolar disorder has a negative impact on cardiac symptomatology. Further research in this area is warranted.
P-199 - Panic-Agoraphobic Spectrum Symptoms are Associated With Impulsivity in Bipolar Disorder
- M. Preve, M. Mula, S. Calugi, L. Lari, A. Cardini, L. Di Paolo, M. Abelli, C. Gesi, M. Muti, S. Pini, M. Mauri
-
- Journal:
- European Psychiatry / Volume 27 / Issue S1 / 2012
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Impulsivity is a core feature of bipolar disorder (BD). The best definition of impulsivity is the predisposition to have rapid and unplanned reactions to internal and external stimuli without regard to the negative consequences of these actions to the impulsive individual or others. Thus, the aim of our study is to investigate the relationship between impulsivity, panic disorder (PD) comorbidity and panic spectrum symptoms in patients with BD.
Method:247 eutimic patients were assessed with SCID-P, MOOD-SR, PAS-SR. Impulsivity dimension was defined on the basis BIS Scale score (version 11).
Results:A backward stepwise logistic regression in bipolar patients with PAS explained score statistically much higher for impulsivity (pas +6.09 vs pas - 3.88 p < 001) and the difference is statistically significant stratifing for BD. A stepwise linear regression, corrected by age and gender, displayed significantly statistical correlation with impulsivity score and PAS-SR by cut-off 35 (OR = 1.210).
Conclusions:In our sample BD eutimic patients explained score statistically much higher for impulsivity. This data confirm the presence of the trait impulsivity in BD eutimic patients. BD patients with a comorbid anxiety disorder seem to display significant higher levels of impulsivity when compared to patients without an anxiety disorder. Impulsivity was linked with atypical panic like symptoms more with PD diagnosis. Results suggest the presence of specific bipolar disorder endophenotipe. Further neurobiologies studies are needed to elucidate the implications and reasons of this association.
Online Gambling, Impulsivity and Personality Traits: an Italian Sample
- M. Pascucci, S. Chiappini, C. Villella, E. Righino, M. Pettorruso, C. Ciciarelli, A. Di Cesare, R. Testa, M. Di Paolo, L. Janiri, G. Conte
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Background and Aims
Internet Gambling has become one of the most popular and lucrative internet business. The recent improvements in technology have changed betting habits with online poker, casinos, sport betting, bingo and lotteries. Liberalization of the Italian online gambling market gradually started in 2006, but only in 2010 foreign gambling operators have been able to launch online real money games.
Our aim is to study the impulsivity and personality traits of an Italian sample of Pathological Gamblers (PG), showing the peculiarities of Online Gambling (OG).
Methods69 patients affected by PG, who accessed to our clinical center, were asked to fill the following questionnaires:
- Temperament and Character Inventory-Revised (TCI-R)
- Europ-ASI (Addiction Severity Index)
- Barratt Impulsiveness Scale (BIS-11)
Resultswe found significant statistical correlations between OG and: younger age (p<0,01), early onset of gambling (p=0,012), male gender (p=0,015), gambling exclusively with active games (p<0,001), gambling that involves different games (p=0,04) and PG familiarity (p=0,03). Considering gamblers'personality traits, OG significantly correlates with higher scores in TCI-R subscales NS1(exploratory excitability) and Persistence, while lower scores in HA2 (fear of uncertain) and ST3 (spiritual acceptance). There is no correlation between OG and impulsivity.
Conclusionsinternet gamblers’ young age could explain the correlations between OG and higher scores in NS1, HA2 and ST3, and consequently risky behaviours and less spiritual believes/acceptance. Higher scores in Persistence indicate perseverance in spite of fatigue or frustration. Cloninger's research found that Persistence, like the other temperament traits, is highly heritable.
2650 – Validation of a Diagnostic Questionnaire Based on DSM-IV Criteria for Gambling
- L. Sabetta, M. Di Paolo, R. Testa, S. Chiappini, M. Pettorruso, A. Di Cesare, C. Villella, G. Conte
-
- Journal:
- European Psychiatry / Volume 28 / Issue S1 / 2013
- Published online by Cambridge University Press:
- 15 April 2020, 28-E1567
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Different questionnaires were formulated in order to assess the severity of gambling. The most used questionnaire is the South Oaks Gambling Screen (SOGS), based on DSM-III criteria for gambling, even though it has poor specificity, because overestimates the prevalence of the disorder when used in general population.
Objectives:Try to overcome SOGS limits using a questionnaire based on DSM-IV criteria for gambling.
Aims:Validate the questionnaire based on DSM-IV criteria, using as gold standard the clinical interview developed through the SOGS.
Methods:The sample used is formed by 71 subjects, 58 men (81.7%) and 13 women (18.3%), recruited from the Psychiatric Department of Gemelli General Hospital in Rome, who were asked to fill out both questionnaires.
Results:The sensitivity of our questionnaire was 93% (compared to 100% in the SOGS); the specificity was 100% (97.1% in the SOGS). False negatives were 7%, while they were absent in the SOGS ; false positives were absent in the DSM-IV questionnaire, while they were 2.9% in the SOGS.
We also determined the prevalence of each item of DSM-IV questionnaire in all gamblers identified (66 subjects): the most relevant item was “chasing one's losses”(item6), instead the least one was “committing illegal acts such as forgery, fraud, theft, or embezzlement to finance gambling”(item8).
Conclusions:Our data confirm the greater specificity of the questionnaire of DSM-IV criteria for gambling compared to the SOGS. We suggest its use for the identification of gamblers in a sample formed by general population.
P-144 - Duloxetine in Somatic Gastric Pain
- M. Preve, C. Nisita, M. Bellini, L. Di Paolo, S. Pini, L. Dell’osso
-
- Journal:
- European Psychiatry / Volume 27 / Issue S1 / 2012
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Panic disorder is the most common anxiety disorder and panic attacks are the most common expression of panic disorder. Panic attacks are characterized with sudden attacks of anxiety with numerous somatic symptoms, such as palpitations, tachycardia, tachypnea, nausea, vertigo (cardiovascular, gastro-enterological, respiratory and neurootological symptoms). Sometimes in clinical practice panic disorder show itself with isolated gastroenteric or cardiovascular symptoms, that request other clinical visit and after psychiatric intervention. The SSRIs are preferred treatment for anxiety disorders and in particular panic disorder. However these drugs may cause some adverse effects such as sexual disfunction (Serretti A et al., 2011), increased bodyweight (Serretti A et al., 2010), abnormal bleending (Andrade C et al., 2010) and others, that may be problematic for some patients.We hereby describe the case of G.V., a 29-year-old Caucasican young woman affected by panic disorder with agoraphobia, referred to our clinic for of the re-occurrence of panic gastroenteric symptoms. With SSRIs the patients feelt an improvement in every anxiety symptoms and panic attacks, but not in the gastric somatic concern, then we decided to enter duloxetine. After six months treatment the patient presented complete remission of gastric sypmtoms and panic related symptoms, and suspended every tree different gastric treatment. Others author like Simon NM et al., hypothesized and confirm the duloxetine a serotonin-norepinephrine inhibitor (SNRI) that has greater initial noradrenergic effects than venlafaxine, would have broad efficacy for individuals with panic disorder.
Our case report underlines the possibility of tailored therapeutic strategies for gastroenteric expression of panic disorder.
2651 – Behavioural Changes in Cocaine Dependent Patients after Group-Therapy
- M. Di Paolo, S. Chiappini, R. Testa, M. Pettorruso, A. Di Cesare, L. Sabetta, G. Conte
-
- Journal:
- European Psychiatry / Volume 28 / Issue S1 / 2013
- Published online by Cambridge University Press:
- 15 April 2020, 28-E1568
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Frequent and increasing relations among psychiatric and substance dependence disorders, have made, to date, more complex the treatment of this dependence, especially when the patient is facing the difficult task of maintaining abstinence, which requires a work of self-awareness, motivation to change and active modification of dysfunctional lifestyles.
Objectives:Our study has the aim to detect patients’ changes in personality between the beginning of the rehabilitative therapy and its end, trying to get information on aspects of addiction on which the treatment affects the most.
Methods:Our sample was formed by 153 patients, recruited at the Department of Psychiatry of Gemelli General Hospital, who were subjected to an integrated approach of treatment, both pharmacological and rehabilitative group-therapy, according to Minnesota rehabilitation model, that considers addiction as a bio-psycho-social problem.
Patients, after a first psychiatric evaluation, were asked to fill out two psychometric tests, the SymptomCheckList-90 R and the Structural Clinical Interview for DSM-IV, in two times, at the first meeting and at the last one, after 20 meetings of group therapy.
Results:At the end of the group therapy 39 patients dropped-out, 114 patients had a significant improvement in depressive symptoms (DEP item), greater responsibility perseverance and attention in their activities and habitual contexts (GSI, DIS, W/S items), as well as better management of compulsion and impulsivity (OC item) and a lower sense of inferiority, inadequacy and discomfort in interpersonal relationships (PAR, ANX, IS, SOC. A., PSY. A. items).
Compulsiveness dimension in a case of pathological gambling
- S. Chiappini, R. Testa, F. Maisto, B. Leone, M. Di Paolo, M. Pascucci, P. Polidori, P. Grandinetti, G. Conte
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, p. S294
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Pathological gambling (PG) is currently included among Addictive Disorders (DSM-5). However, its phenomenology resembles features of Obsessive Compulsive Disorder. Several models of addiction conceptualize a progression from impulsivity to compulsivity transitioning from initial positive reinforcement motivations to later negative reinforcement and less pleasurable and automaticity mechanisms.
Clinical presentationA 34-year-old male, since diagnosed with PG in 2013 and prescribed a group rehabilitation therapy, presented in 2015 complaining of intrusive thoughts and depression symptoms. During the psychiatric examination emerged: low mental concentration; dysphoria; hyporexia; irritability; insomnia; persistent ideas and excessive preoccupations to be betrayed by his girlfriend; and behaviours of hyper control on her life. He has been evaluated using MMPI-2 (obsessivity Tscore 70, depression Tscore 67) and BIS-11 (high score of non-planning impulsiveness).
TreatmentIt appeared there was a shift from ego-syntonic novelty driven/impulsive behaviours focused primarily on gambling to ego-dystonic habit driven/compulsive behaviours focused on her girlfriend. He started an individual psychodynamic psychotherapy centred on dysfunctional beliefs and behavioural strategies for treating the compulsive features. As thought content was the most relevant aspect, he was prescribed olanzapine, not a SSRI (normally indicated for OCD), up to 10 mg/die. After a month obsessions and compulsions reduced, and he seemed to reach a good level of personal functioning, despite a rigid anankastic personality trait.
ConclusionsAs the management of compulsive behaviours is complex, physician should better assess and recognize psychological personality aspect, collecting patients’ complete history, also testing them psychometrically, and paying more attention to an eventual treatment (both psychological and pharmacological).
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Contributors
-
- By Jane E. Adcock, Yahya Aghakhani, A. Anand, Eva Andermann, Frederick Andermann, Alexis Arzimanoglou, Sandrine Aubert, Nadia Bahi-Buisson, Carman Barba, Agatino Battaglia, Geneviève Bernard, Nadir E. Bharucha, Laurence A. Bindoff, William Bingaman, Francesca Bisulli, Thomas P. Bleck, Stewart G. Boyd, Andreas Brunklaus, Harry Bulstrode, Jorge G. Burneo, Laura Canafoglia, Laura Cantonetti, Roberto H. Caraballo, Fernando Cendes, Kevin E. Chapman, Patrick Chauvel, Richard F. M. Chin, H. T. Chong, Fahmida A. Chowdhury, Catherine J. Chu-Shore, Rolando Cimaz, Andrew J. Cole, Bernard Dan, Geoffrey Dean, Alessio De Ciantis, Fernando De Paolis, Rolando F. Del Maestro, Irissa M. Devine, Carlo Di Bonaventura, Concezio Di Rocco, Henry B. Dinsdale, Maria Alice Donati, François Dubeau, Michael Duchowny, Olivier Dulac, Monika Eisermann, Brent Elliott, Bernt A. Engelsen, Kevin Farrell, Natalio Fejerman, Rosalie E. Ferner, Silvana Franceschetti, Robert Friedlander, Antonio Gambardella, Hector H. Garcia, Serena Gasperini, Lorenzo Genitori, Gioia Gioi, Flavio Giordano, Leif Gjerstad, Daniel G. Glaze, Howard P. Goodkin, Sidney M. Gospe, Andrea Grassi, William P. Gray, Renzo Guerrini, Marie-Christine Guiot, William Harkness, Andrew G. Herzog, Linda Huh, Margaret J. Jackson, Thomas S. Jacques, Anna C. Jansen, Sigmund Jenssen, Michael R. Johnson, Dorothy Jones-Davis, Reetta Kälviäinen, Peter W. Kaplan, John F. Kerrigan, Autumn Marie Klein, Matthias Koepp, Edwin H. Kolodny, Kandan Kulandaivel, Ruben I. Kuzniecky, Ahmed Lary, Yolanda Lau, Anna-Elina Lehesjoki, Maria K. Lehtinen, Holger Lerche, Michael P. T. Lunn, Snezana Maljevic, Mark R. Manford, Carla Marini, Bindu Menon, Giulia Milioli, Eli M. Mizrahi, Manish Modi, Márcia Elisabete Morita, Manuel Murie-Fernandez, Vivek Nambiar, Lina Nashef, Vincent Navarro, Aidan Neligan, Ruth E. Nemire, Charles R. J. C. Newton, John O'Donavan, Hirokazu Oguni, Teiichi Onuma, Andre Palmini, Eleni Panagiotakaki, Pasquale Parisi, Elena Parrini, Liborio Parrino, Ignacio Pascual-Castroviejo, M. Scott Perry, Perrine Plouin, Charles E. Polkey, Suresh S. Pujar, Karthik Rajasekaran, R. Eugene Ramsey, Rahul Rathakrishnan, Roberta H. Raven, Guy M. Rémillard, David Rosenblatt, M. Elizabeth Ross, Abdulrahman Sabbagh, P. Satishchandra, Swati Sathe, Ingrid E. Scheffer, Philip A. Schwartzkroin, Rod C. Scott, Frédéric Sedel, Michelle J. Shapiro, Elliott H. Sherr, Michael Shevell, Simon D. Shorvon, Adrian M. Siegel, Gagandeep Singh, S. Sinha, Barbara Spacca, Waney Squier, Carl E. Stafstrom, Bernhard J. Steinhoff, Andrea Taddio, Gianpiero Tamburrini, C. T. Tan, Raymond Y. L. Tan, Erik Taubøll, Robert W. Teasell, Mario Giovanni Terzano, Federica Teutonico, Suzanne A. Tharin, Elizabeth A. Thiele, Pierre Thomas, Paolo Tinuper, Dorothée Kasteleijn-Nolst Trenité, Sumeet Vadera, Pierangelo Veggiotti, Jean-Pierre Vignal, J. M. Walshe, Elizabeth J. Waterhouse, David Watkins, Ruth E. Williams, Yue-Hua Zhang, Benjamin Zifkin, Sameer M. Zuberi
- Edited by Simon D. Shorvon, Frederick Andermann, Renzo Guerrini
-
- Book:
- The Causes of Epilepsy
- Published online:
- 05 March 2012
- Print publication:
- 14 April 2011, pp ix-xvi
-
- Chapter
- Export citation






